George Ronald Soncini da RosaI; Francisco Diniz Affonso da CostaII; Ricardo Guilherme D'Otaviano de Castro VILANIIII; Felipe Phol de SOUZAIII; Lorena REICHERTIV; Iseu de Santo Elias Affonso da COSTAV
DOI: 10.1590/S0102-76382006000300010
ABSTRACT
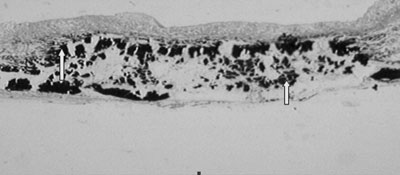
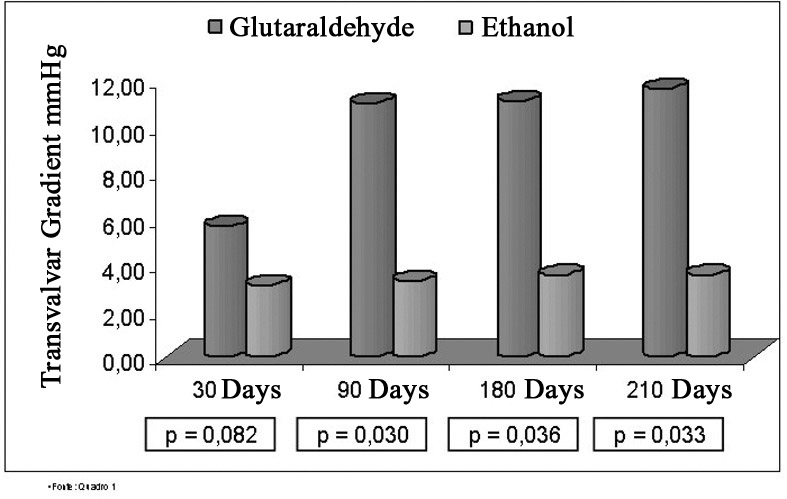
Objective: The objective of this work was to comparatively evaluate the use of ethanol (E) with glutaraldehyde (GDA) to inhibit the calcification of the porcine pulmonary valvar heterografts (PPVH) implanted in the right ventricle outflow tract of young sheep. Method: Ten young sheep were used, divided into two similar groups: the GDA (control) Group and the Ethanol Group (in which the PPVH were pre-treated with ethanol-80). The surgery consisted of implanting the PPVH in the right ventricle outflow tract using a cardiopulmonary bypass. Echocardiography was performed to measure the transvalvar gradient and macroscopic analyses of the PPVH wall and microscopic analysis for calcification were performed. The amount of calcium was measured in the valve cusp at 210 days. Results: The quantity of calcium in the PPVH of the GDA Group was 7.98 ± 6.82µg calcium/mg tissue and of the E Group it was 0.31± 0.33µg calcium/mg tissue. In respect to the maximum transvalvar gradient at 30 days, there was no significant difference between the groups. At 90, 180 and 210 days however, the GDA Group showed a greater transvalvar gradient than the E Group. The macroscopic analyses of the heterograft wall evidenced calcification in both groups but it was more pronounced in the GDA Group. The microscopic analysis of the cusp valve revealed the presence of calcification in all animals of the GDA Group, while in the E Group no calcification was seen. Conclusion: In conclusion ethanol-80 inhibits calcification on the cusps during the period of the analysis but does not inhibit the calcification of the PPVH.RESUMO
bjetivo: Analisar comparativamente o uso do etanol (E) com o glutaraldeído (GDA), como método de inibição da calcificação dos heteroenxertos valvares pulmonares porcinos (HVPP) implantados na via de saída do ventrículo direito (VD) de ovinos jovens. Método: Foram utilizados dez ovinos jovens, em dois grupos contendo cinco animais cada. A operação consistiu na implantação do HVPP na via de saída do VD com circulação extracorpórea, divididos em dois grupos; o grupo do GDA (controle) e o grupo E (grupo em que os HVPP foram pré-tratados com etanol a 80%). Realizou-se estudo ecocardiográfico para medida do gradiente transvalvar pulmonar, análise macroscópica da parede do HVPP e microscópica quanto à presença de calcificação; e mensuração do cálcio na cúspide valvar após 210 dias. Resultados: Na mensuração do cálcio do HVPP encontrou-se no grupo GDA (7,98 ± 6,82µg cálcio/mg tecido), no grupo E (0,31± 0,33µg cálcio/mg tecido). Em relação ao gradiente transvalvar máximo em 30 dias, não houve diferença significativa entre os grupos, já aos 90, 180 e 210 dias, o grupo GDA apresentou maior gradiente transvalvar do que o grupo do etanol. Na análise macroscópica da parede do HVPP, observou-se calcificação em ambos os grupos, sendo mais intensa no grupo do GDA. Na avaliação microscópica das cúspides do HVPP em relação à presença de calcificação, observou-se que no grupo GDA esteve presente em todos os animais, enquanto no grupo E, esteve ausente em todos. Conclusão: Conclui-se que etanol a 80% inibe a calcificação das cúspides no período analisado, mas não inibe a calcificação da parede do HVPP.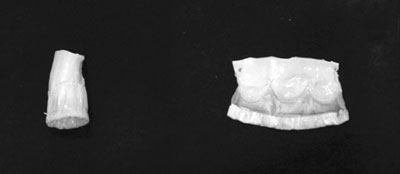



Article receive on Sunday, January 1, 2006
 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license