Objective: To evaluate the use of the right common carotid artery to establish cardiopulmonary bypass (CPB) and the use of anterograde cerebral perfusion as cerebral protection in patients scheduled for ascending aortic repair surgery.
Methods: Twenty-three patients were submitted to aortic repair because of different aortic diseases. In all of them a Gore-tex tube was anastomosed to the right common carotid artery to establish CPB and anterograde cerebral perfusion during distal anastomosis. Average CPB time was 195 minutes; average temperature was 24 degrees Celsius; average anterograde cerebral hypoperfusion time was 29 minutes; average hospital stay was 18 days.
Results: None of the 23 patients had any neurological dysfunction within the first 48 postoperative hours. Prior to discharge, all of them were submitted to the "Mini Mental State Examination (MMSE)" which did not identify any cognitive dysfunction or neurological injury. Two patients developed pulmonary infection, two patients needed dialysis and two patients died due to the high complexity of the cases. There were no perioperative deaths.
Conclusion: This is a practical, fast, efficient and reproducible way to establish CPB and anterograde cerebral protection, reducing the risk of cerebral ischemia and improving the natural postoperative outcome of these procedures.
Objetivo: Analisar os resultados da utilização da artéria carótida comum direita no estabelecimento da circulação extracorpórea (CEC) para perfusão sistêmica (PS), bem como na utilização como via anterógrada para proteção cerebral (PC), nos pacientes submetidos à correção das doenças que envolveram a aorta ascendente (AA).
Método: Foram operados 23 pacientes portadores de várias afecções da AA, nos quais a abordagem foi possível por meio do estabelecimento da CEC pela anastomose de um tubo de PTFE (politetrafluoretileno) à artéria carótida comum direita e manutenção de fluxo cerebral anterógrado durante a confecção da anastomose distal. O tempo médio de CEC foi de 195 minutos (152 a 253 minutos), a temperatura média sistêmica foi de 24°C (18°C a 25°C), hipofluxo cerebral anterógrado, com média de 29 minutos (27 a 51 minutos) e o tempo de internação média foi de 18 dias (8 a 30 dias).
Resultados: Todos os pacientes despertaram nas primeiras 48 horas sem dano neurológico. Por ocasião da pré-alta, foram submetidos ao teste MINI MENTAL STATE EXAMINATION (MMSE), que demonstrou não haver desordens cognitivas com dano neurológico. Ocorreram dois casos de infecção pulmonar, dois pacientes necessitaram de diálise e ocorreram dois óbitos relacionados à gravidade dos casos. Não houve óbito per-operatório.
Conclusão: Este é um método prático, rápido, seguro, eficaz e reprodutível, tanto no estabelecimento da CEC como da proteção cerebral anterógrada, reduzindo o risco de isquemia cerebral, alterando a história natural da evolução pós-operatória destas correções.
INTRODUCTION
The femoral artery has been, over the few last years, the favorite access for surgeons to establishment cardiopulmonary bypass (CPB) to repair aortic aneurysms and dissections. However, it has been reported that perfusion via the femoral artery is associated with higher morbidly, as well as bad cerebral perfusion [1-3]. Additionally, this technique is contraindicated in cases of aorto-iliac and femoral artery disease and in cases of acute aortic dissections in which there is involvement of the femoral arteries. Another factor which must be taken into account when establishing CPB via the femoral artery is the inversion of flow, which favors the release of 'debris', thereby increasing the risk of strokes [3]. Aiming at finding alternatives, Neri et al. [4] in 1999 demonstrated that with cannulation of the auxiliary artery it is possible to repair dissecting type-A aneurysms, without causing complications due to cannulation, thus representing a safer manner to use CPB. Kazui et al. [5] demonstrated, in a long observation work (from 1990 to 1999) an analysis of 220 patients, that anterograde cerebral perfusion, as a method of cerebral protection, is possible with cannulation of the brachiocephalic trunk and left carotid artery, after the incision of the aneurysm. Souza et al. [6] utilized CPB for systemic perfusion, as well as for selective anterograde cerebral perfusion with hypoflow through the right common carotid artery (RCCA) during aortic arch repair procedures.
METHOD
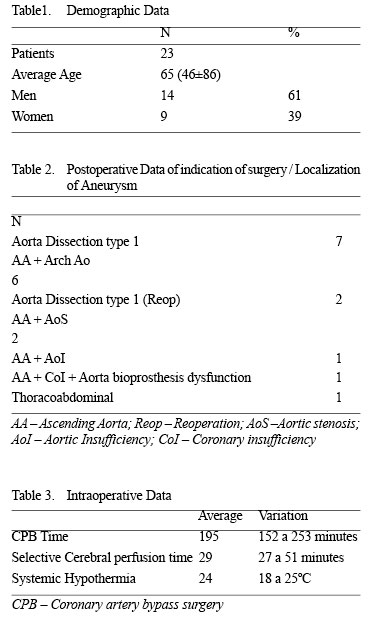
From July 2002 to February 2005, 23 patients were submitted to surgeries involving the ascending aorta. The mean age was 65 years old (varying from 43 to 86 years). Of the 23 patients, 14 (61%) were men and nine (39%) were women (Table 1). Diagnoses included aorta type-I dissection (seven); ascending aorta and aortic arch aneurysms (six); reoperation of dissecting type-I aneurysm (two); ascending aorta aneurysm associated with severe aortic stenosis (two); ascending aortic aneurysm associated with severe aortic insufficiency (one); ascending aorta aneurysm associated with dysfunction of an aortic bioprosthesis and coronary insufficiency (one); thoracoabdominal aneurysm (one); re-operation of an infected ascending aorta pseudo-aneurysm (one); aneurysm of the sinus of Valsalva and ascending aorta (one) and ascending aorta aneurysm associated with aortic and coronary insufficiency (one) - Table 2.
The mean CPB and cerebral hypoflow times were 195 minutes (range 152 - 253 minutes) and 29 minutes (range 27 - 51 minutes) respectively and the average hypothermia was 24ºC (ranging from 18ºC to 25ºC) - Table 3.
Technique
The technique consists in the dissection and repair of the RCCA, in which, by longitudinal arteriotomy, an 8-mm polytetrafluoroethylene tube is anastomosed, sectioned in a bevel shape, to the RCCA, with 6-0 prolene sutures, making arterial cannulation through the graft possible.
The venous cannulation is achieved in the normal way by means of a two-section cannula inserted in the right atrium (Figures 1 and 2).
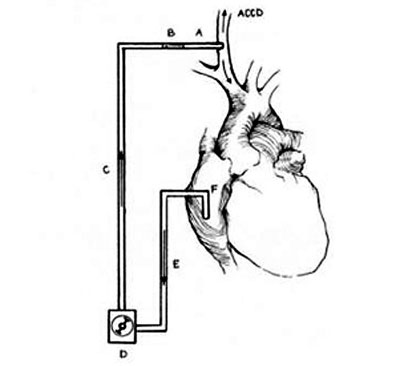
Fig. 1 - Design of CPB: A) PTFE tube. B) 3/8 connector - ¼ inch. C) Arterial line. D) roller. E)Venous line. F) Two-stage venous cannula
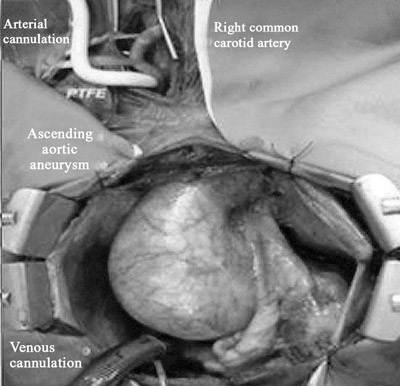
Fig. 2 - Surgical aspect of perfusion by the right common carotid artery through the PTFE tube connected to the arterial line of the CPB
For three patients, we opted for CPB through the femoral vein, because they were being re-operated and there was a risk of rupture of the aneurysm during the median sternotomy. In these three cases, during reheating, the venous cannula was repositioned in the right atrium in the normal manner. Systemic hypothermia varied between moderate and deep and was associated to cardiocirculatory arrest. During the procedure on the aortic arch and great vessels, the aortic clamp was repositioned on the RCCA, close to the anastomosis of the PTFE tube (Figure 3).
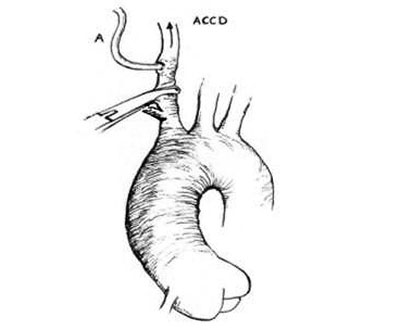
Fig. 3 - Detail of right common carotid artery (RCCA) clamping site during selective cerebral perfusion. A = PTFE tube
The clamp was positioned on the brachiocephalic trunk (BCT) when there was a high risk of medullary ischemia. An anterograde cerebral flow was maintained at around 10 mL/kg/minute associated with topical hypothermia (ice helmet). During this series, a left common carotid artery approach was used for just one patient with acute aortic dissection involving the RCCA.
RESULTS
In the group of 23 patients operated on using this technique with CPB via the RCCA and anterograde cerebral perfusion, there were no intraoperative deaths. Two patients died due to the severity of the disease; one suffered from an acute aortic dissection with severe entero-mesenteric ischemia and the other had an infected pseudo-aneurysm that evolved to untreatable sepsis in the postoperative period. All the other 21 patients recovered in the postoperative period without neurological sequels. Before discharge, the patients was submitted to the Mini Mental State Examination test (MMSE) [7,8], where orientation, memory, attention, calculation and language were evaluated to assess postoperative cognitive alterations related to transitory ischemia, as well as alterations of the cerebral cortex. In the analysis of this test, patients that present a score of almost thirty are not suffering from cognitive alterations (Figure 4).
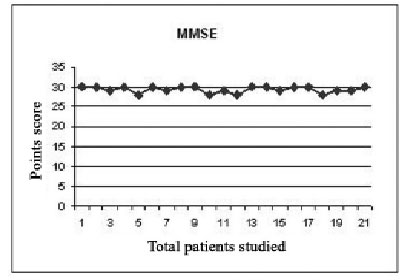
Fig. 4 - In the Mini Mental State Examination test (MMSE), patients that present a score of almost thirty are not suffering from cognitive alterations
Cannulation of the femoral artery continues to be one option for CPB in surgeries involving aortic diseases. Cardiocirculatory arrest, as proposal by Grieep et al. [9] in 1975, with deep hypothermia, improved greatly the repair of aortic arch diseases, however time is limited to approximately 40 minutes, restricting its use in more complex diseases. In 1990 Uedad et al. [10], proposed cerebral retrograde protection. In 2001, Okita et al. [11] presented a study comparing deep hypothermia associated to selective anterograde cerebral perfusion and retrograde cerebral perfusion, observing a higher incidence of cognitive alterations associated to the latter. In 2001, Frist et al. [12] operated eight patients using moderate hypothermia and anterograde cerebral perfusion. In 2003, Souza et al. [6] presented their initial results of nine patients for whom CPB via the right carotid artery and anterograde cerebral perfusion was used, giving excellent results that encouraged us to start this study.
CONCLUSION
Analysis of this work concludes that the right common carotid artery is an approach that enables both CPB with systemic perfusion and maintenance of adequate anterograde cerebral flow, reducing the possibility of cerebral ischemia. It is an efficient, practical, reliable and safe method that is easy to reproduce and as it does not lead to significant neurological damage it changes the natural history of the postoperative period of patients submitted to surgeries involving the ascending aorta.
ACKNOWLEDGEMENT
The authors would like to thank Prof. Dr. Eduardo S. Bastos for the valuable guidance received during the production of this work.
REFERENCES
1. Salerno TA, Lince DP, White DN, Lynn RB, Charrette EJ. Arch versus femoral artery perfusion during cardiopulmonary bypass. J Thorac Cardiovasc Surg. 1978;76(5):681-4.
2. Borst HG. In: Borst HG, Heinemann MK, Stone CD, eds. Surgical treatment of aortic dissection. New York:Churchill Livingstone;1996. p.255-68.
3. Price DL, Harris J. Cholesterol emboli in cerebral arteries as a complication of retrograde aortic perfusion during cardiac surgery. Neurology. 1970;20(12):1209-14.
4. Néri E, Massetti M, Capannini G, Carone E, Tucci E, Diciolla F et al. Axillary artery cannulation in type A aortic dissection operations. J Thorac Cardiovasc Surg. 1999;118(2):324-9.
5. Kazui T, Washiyama N, Muhammad BA, Terada H, Yamashita K, Takinami M et al. Total arch replacement using aortic arch branched grafts with the of aid anterograde selective cerebral perfusion. Ann Thorac Surg. 2000;70(1):3-9.
6. Souza JM, Rojas SO, Berlinck MF, Mazzieri R, Oliveira PAF, Martins JRM et al. Circulação extracorpórea pela artéria carótida comum direita na correção de doenças da aorta ascendente, arco aórtico e aorta descendente. Rev Bras Cir Cardiovasc. 2003;18(2):137-41.
7. Dick JP, Guiloff RJ, Stewart A, Blackstock J, Bielawaska C, Paul EA et al. Mini-mental state examination in neurological patients. J Neurol Neurosurg Psychiatry. 1984;47(5):496-9.
8. Tsai L, Tsuang MT. The mini-mental state test and computerized tomography. Am J Psychiatry. 1979;136(4A):436-8.
9. Griepp RB, Stinson EB, Hollingsworth JF, Buehler D. Prosthetic replacement of the aortic arch. J Thorac Cardiovasc Surg. 1975;70(6):1051-63.
10. Ueda Y, Miki S, Kusuhara K, Okita Y, Tahata T, Yamanaka K. Surgical treatment of aneurysm or dissection involving the ascending aorta and aortic arch, utilizing circulatory arrest and retrograde cerebral perfusion. J Cardiovasc Surg. 1990;31(5):553-8.
11. Okita Y, Minatoya K, Tagusari O, Ando M, Nagatsuka K, Kitamura S. Prospective comparative study of brain protection in total aortic arch replacement:deep hypothermic circulatory arrest with retrograde cerebral perfusion or selective antegrade cerebral perfusion. Ann Thorac Surg. 2001;72(1):72-9.
12. Frist WH, Baldwin JC, Starnes VA, Stinson EB, Oyer PE, Miller DC et al. A reconsideration of cerebral perfusion in aortic arch replacement. Ann Thorac Surg. 1986;42(3):273-81.




 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license