Objective: To compare the observed incidence of mediastinitis and strokes versus the expected incidence according to the NNECDSG score (Northern New England Cardiovascular Disease Study Group) in a population submitted to coronary artery bypass graft surgery.
Methods: A retrospective consultation was made of medical records of all patients submitted to isolated CABG from January 1st, 2000 to December 31st, 2004, at the Cardiac Surgery Service of the Triângulo Mineiro Federal University (UFTM). Data regarding the incidences of observed mediastinitis and strokes and those estimated by the NNECDSG score were submitted to the Kolmogorov-Smirnov normality test. A comparison was achieved using the paired Student t test, with the level of significance determined as p=0.05.
Results: A group of 230 patients were analyzed, including 144 (62.60%) men and 86 (37.39%) women. Sixty-one (26.52%) presented with diabetes, 30 (13.04%) with chronic obstructive pulmonary disease (COPD) and 23 (10%) had peripheral vascular disease (PVD). Emergency surgery occurred in 34 (14.78 %) cases. In 37 (16.08%) patients an ejection fraction (EF) of less than 40% was identified. Mediastinitis occurred in 12 (5.21%) patients and despite the greater general incidence in the sample studied, no statistical significance was found. Strokes occurred in 12 patients (5.21%) and in spite of the higher mean percentage incidence of observed strokes for all scores, a level of statistical significance was not found.
Conclusions: Although the incidences of mediastinitis and strokes were greater in the population studied, these values showed no statistical significance, confirming the score recommended by the NNECDSG as a safe and efficient method for predicting postoperative mediastinitis and strokes in patients submitted to myocardial revascularization surgery in the UFTM.
Objetivo: Comparar as incidências observadas de mediastinite e acidente vascular cerebral (AVC) versus as incidências esperadas pelo escore NNECDSG (Northern New England Cardiovascular Disease Study Group), em população submetida à cirurgia de revascularização do miocárdio.
Método: Foram analisados, retrospectivamente, os prontuários de todos os pacientes submetidos à CRVM isolada, no período de 1/1/2000 a 31/12/2004, no Serviço de Cirurgia Cardíaca da Universidade Federal do Triângulo Mineiro (UFTM). Foi aplicado o escore proposto pelo NNECDSG e calculadas as incidências esperadas de mediastinite e AVC para cada paciente. Os dados de incidência observados e a incidência estimada pelo escore do NNECDSG foram submetidos ao teste de normalidade de Kolmogorov-Smirnov. A comparação foi realizada pelo teste t-Student pareado. O nível de significância foi de á=0,05.
Resultados: Foram analisados 230 pacientes, sendo 144 (62,60%) homens e 86 (37,39%) mulheres. Sessenta e um (26,52%) doentes apresentavam diabetes, 30 (13,04%), doença pulmonar obstrutiva crônica (DPOC) e 23 (10%), doença vascular periférica (DVP). Cirurgia de urgência aconteceu em 34 (14,78%) casos. Trinta e sete (16,08%) pacientes tinham uma fração de ejeção (FE) menor que 40%. Mediastinite ocorreu em 12 (5,21%) pacientes. Apesar da incidência geral de mediastinite ter sido maior nesta amostra, não houve significância estatística. AVC ocorreu em 12 (5,21%) pacientes. Apesar da incidência percentual média de AVC observada ter sido maior, não atingiu nível de significância estatística.
Conclusão: Apesar das incidências de mediastinite e AVC terem sido maiores na população estudada, estes valores não atingiram significância estatística, sendo o escore preconizado pela NNECDSG um método seguro e eficaz na predição de mediastinite e AVC pós-operatórios nos pacientes submetidos à CRVM na UFTM.
INTRODUCTION
In light of all the advances achieved in cardiology, whether clinical or interventionist, cardiac surgeons have seen a progressive change in the profile of patients submitted to coronary artery bypass grafting surgery (CABG) [1]. In Brazil, Sant'Anna et al. [2] demonstrated that current CABG patients are older and in worse clinical conditions (cardiac and systemic) than the ones operated 10 years ago.
Thus, it is expected that patients operated nowadays have a higher risk of complications. It is important to try to preoperatively predict the chance of each patient developing complications. Among these morbidities, strokes and mediastinitis are important as they increase mortality, hospitalization times and costs [3,4]. In Brazilian publications, data on predicting the morbidity of patients submitted to CABG is scarce.
The objective of the current study is to compare the incidences of mediastinitis and strokes versus the expected incidences according to the score proposed by the NNECDSG study (Northern New England Cardiovascular Disease Study Group) [3], in a population submitted to CABG in isolation in a general hospital in the interior of Brazil.
METHOD
The project was approved by the Research Ethics Commission of the Federal University of the Triângulo Mineiro.
were collected retrospectively from an investigation of the records of all patients submitted to CABG in isolation in the period from January 1st, 2000 to December 31st, 2004 in the Heart Surgery Service of the Teaching Hospital of the Federal University of the Triângulo Mineiro. In total, 230 patients were included in the study. All the patients were submitted to CABG in isolation using cardiopulmonary bypass and anterograde cold crystalloid cardioplegia.
The study sample consisted of 144 (62.6%) male and 86 (37.39%) female patients.
Sixty-one (26.52%) patients had diabetes, 30 (13.04%) had COPD and 23 (10%) were diagnosed with peripheral vascular disease (PVD).
Urgent surgery was necessary in 34 (14.7%) patients.
Myocardial infraction with less than 7 days of evolution was observed in 6 (2.6%) patients.
In 37 (16.08%) patients, the ejection fraction was less that 40%. Mediastinitis was defined as a culture and/or gram-positive infection in the deep mediastinal tissue and/or radiographic findings indicating mediastinal infection that required re-operation. Strokes were defined as a new focal neurological event that persisted for at least twenty-four hours.
The score proposed by NNECDSG was applied to the collected data and the expected incidence of mediastinitis and strokes were calculated for each patient.
The observed incidences of mediastinitis and strokes and incidences estimated using the NNECDSG score were submitted to the Kolmogorov-Smirnov normality test. A comparison was achieved using the paired Student t-test. The level of significance was set at a p-value = 0.05.
RESULTS
The results relative to the occurrence of mediastinitis are shown in Table 1. We saw that, for scores 5 and 11, the model proposed by NNECDSG overestimated the percentage of mediastinitis and for the other scores the model underestimated the incidence (Figure 1). We stress that the mean percentage incidence of mediastinitis observed among all the scores, although without statistical significance, was higher than the mean percentage incidence of mediastinitis estimated by the NNECDSG model (Figure 1 and Table 1).


Fig. 1 - Mean pattern of the observed incidence of mediastinitis compared to the incidence estimated according to the NNECDS score
It is worthwhile mentioning that it is important to consider a larger sample of patients to verify whether this pattern persists as the variations in data were very high (variation coefficient > 100%) - Figure 2.

Fig. 2 - Spread of differences between the observed incidence of mediastinitis and that estimated according to the NNECDS score
The results related to the occurrence of strokes are reported in Table 2.
We verified that for scores 8 and 9 the model proposed by NNECDSG overestimated the percentage incidence of strokes and for the other scores the model underestimated the occurrence of strokes (Figure 3). We stress that the mean percentage incidence of strokes observed was higher for the total of patients, however without being statistically significant (Figure 3 and Table 2).
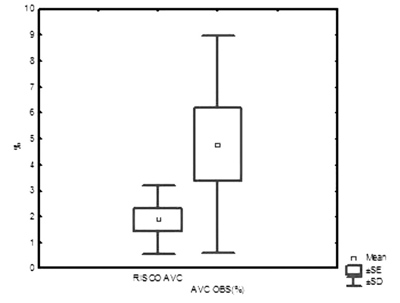
Fig. 3 - Mean pattern of the observed percentage of strokes and the percentage estimated according to the NNECDS score
It is worthwhile pointing out that it is important to consider a larger sample of patients to verify whether this pattern persists as the variations in data were very high (variation coefficient next to 100%) - Figure 4.

Fig. 4 - Spread of differences between the observed incidence of strokes and that estimated according to the NNECDS score
The current study demonstrates that the utilization of an American score approved by the ACC/AHA Guideline Update for Coronary Artery Bypass Graft Surgery, to estimate morbidity, may be applicable in Brazil.
In light of all the advances achieved in cardiology, whether clinical or interventionist, cardiac surgeons had seen a progressive change in the profile of patients submitted to CABG [1]. In Brazil, Sant'Anna et al. [2] demonstrated that the patients submitted to CABG nowadays are older and in worse clinical conditions (cardiac and systemic) than those operated 10 years ago.
There are numerous works in the international literature that try to predict the risk of operative mortality [1,5-8]. It is believed that systematization of variables may assist to compare results among institutions and among surgeons, working as a control of quality of cardiovascular surgery services [1,8-10].
The validation of these mortality scores has happened in some countries, with very varied study populations in respect to the population where the scores were originally designed [11-13].
In respect to morbidity, studies are scarcer [5,15]. The CABDEAL study [5] was designed to predict morbidity in patients submitted to their first CABG. The mortality rate of the cohort from which this system was derived was extremely low at 1.6%. Thus, the CABDEAL model was originally validated to predict morbidity and not mortality.
The incidence of mediastinitis varies from 0.4% to 5% in different series [16-18]. Once established, mediastinitis causes high mortality rates varying between 10% and 47% [17,18]. The proportion of patients that undergo CABG, that are at high risk for infection, has increased substantially with the aging of the population, increasing the number of coronary re-operations. These patients are frequently associated to conditions that increase both the cardiovascular risk and the risk of infection, such as obesity and diabetes mellitus [17,18].
The incidence of strokes after CABG varies greatly in the literature: from 0.8% to 5.2% [19]. Moreover, it is already well established that this feared complication is associated to increases in the hospitalization time, costs and the mortality rate [19,20]. We can list the known risk factors of strokes after CABG: chronic renal failure, recent myocardial infarction, previous strokes, known carotid artery disease, systemic arterial hypertension, diabetes, age greater than 75 years, moderate to serious left ventricular dysfunction, low cardiac output syndrome and atrial fibrillation [19].
It is essential that we manage to estimate which patients are more prone to these complications, especially as the surgical procedure can be modified, aiming at reducing these events.
In truth, we found population and epidemiological samples very distinct when we compared the North American and Brazilian studies. These populational and epidemiological differences are also observed in other scores, as, for example, the Euroscore, that even demonstrated epidemiological differences between the counties that comprised the trial [14].
After statistical analysis of the sample, we concluded that the model proposed by NNECDSG is adequate to estimate the occurrence of mediastinitis and strokes of patients studied in this sample.
In the current study, we identified the sample size to be a limiting factor. Nevertheless, we saw the possibility of applying a North American score to patients submitted to CABG in the Federal University of the Triângulo Mineiro, with the tool being easy to use in cardiovascular surgery. We stress that, even though the incidences of mediastinitis and strokes are higher in the studied population, these differences were not statistically significant.
With the small sample size of the current study and due to previously identified epidemiological and populational differences, as well as the lack of studies in Brazil on this subject, we believe that the attempt to create a Brazilian model, involving different institutions from the diverse regions of country, to predict postoperative morbidity is valid and desirable.
REFERENCES
1. Roques F, Nashef SA, Michel P, Gauducheau E, de Vincentiis C, Baudet E, et al. Risk factors and outcome in European cardiac surgery: analysis of the EuroSCORE multinational database of 19030 patients. Eur J Cardiothorac Surg. 1999;15(6):816-22.
2. Feier FH, Sant'anna RT, Garcia E, De Bacco FW, Pereira E, Santos MF, et al. Modificações no perfil do paciente submetido à operação de revascularização do miocárdio. Rev Bras Cir Cardiovasc. 2005;20(3):317-22.
3. O'Connor GT, Plume SK, Olmstead EM, Coffin LH, Morton JR, Maloney CT, et al. A regional prospective study of in-hospital mortality associated with coronary artery bypass grafting. The Northern New England Cardiovascular Disease Study Group. JAMA. 1991;266(6):803-9. [
MedLine]
4. Kurki TS, Kataja M. Preoperative prediction of postoperative morbidity in coronary artery bypass grafting. Ann Thorac Surg. 1996;61(6):1740-5. [
MedLine]
5. Parsonnet V, Dean D, Bernstein AD. A method of uniform stratification of risk for evaluating the results of surgery in acquired adult heart disease. Circulation. 1989;79(6 Pt 2):I3 [
MedLine]
6. Edwards FH, Grover FL, Shroyer AL, Schwartz M, Bero J. The Society of Thoracic Surgeons National Cardiac Surgery Database: current risk assessment. Ann Thorac Surg. 1997;63(3):903-8. [
MedLine]
7. ShroyerAL, Plomodon ME, Grover FL, Edwards FH. The 1996 coronary artery bypass risk model: the Society of Thoracic Surgeons Adult Cardiac National Database. Ann Thorac Surg. 1999;67(4):1205-8. [
MedLine]
8. Higgins TL, Estafanous FG, Loop FD, Beck GJ, Blum JM, Paranandi L. Stratification of morbidity and mortality outcome by preoperative risk factors in coronary artery bypass patients. A clinical severity score. JAMA. 1992;267(17):2344-8. [
MedLine]
9. Parsonnet V, Bernstein AD, Gera M. Clinical usefulness of risk-stratified outcome analysis in cardiac surgery in New Jersey. Ann Thorac Surg. 1996;61(2 Suppl):S8-S11. [
MedLine]
10. Roques F, Gabrielle F, Michel P, De Vincentiis C, David M, Baudet E. Quality of care in adult heart surgery: proposal for a self-assessment approach based on a French multicenter study. Eur J Cardiothorac Surg. 1995;9(8):433-9.
11. Syed AU, Fawzy H, Farag A, Nemlander A. Predictive value of EuroSCORE and Parsonnet scoring in Saudi population. Heart Lung Circ. 2004;13(4):384-8. [
MedLine]
12. Nashef SA, Carey F, Silcock MM, Oommen PK, Levy RD, Jones MT. Risk stratification for open heart surgery: trial of the Parsonnet system in a British hospital. BMJ. 1992;305(6861):1066-7. [
MedLine]
13. Pons JM, Granados A, Espinas JA, Borras JM, Martin I, Moreno V.Assessing open heart surgery mortality in Catalonia (Spain) through a predictive risk model. Eur J Cardiothorac Surg. 1997;11(3):415-23. [
MedLine]
14. Roques F, Nashef SA, Michel P, Pinna Pintor P, David M, Baudet E. Does EuroSCORE work in individual European countries? Eur J Cardiothorac Surg. 2000;18(1):27-30. [
MedLine]
15. Kurki TS, Kataja M. Preoperative prediction of postoperative morbidity in coronary artery bypass grafting. Ann Thorac Surg. 1996;61(6):1740-5. [
MedLine]
16. Abboud CS, Wey SB, Baltar VT. Risk factors for mediastinitis after cardiac surgery. Ann Thorac Surg. 2004;77(2):676-83. [
MedLine]
17. Fowler VG, O'Brien SM, Muhlbaier LH, Corey RG, Ferguson TB, Peterson ED. Clinical predictors of major infections after cardiac surgery. Circulation. 2005;112(9 Suppl):I358-65. [
MedLine]
18. Guaragna JC, Facchi LM, Baião CG, Cruz IBM, Bodanese LC, Albuquerque L, et al. Preditores de mediastinite em cirurgia cardíaca. Rev Bras Cir Cardiovasc. 2004;19(2):165-70.
19. Stamou SC. Stroke and encephalopathy after cardiac surgery: the search for the holy grail. Stroke. 2006;37(2):284-5. [
MedLine]
20. McKhann GM, Grega MA, Borowicz LM, Baumgartner WA, Selnes OA. Stroke and encephalopathy after cardiac surgery: an update. Stroke. 2006;37(2):562-71. [
MedLine]






 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license