To evaluate incidence, mortality, and risk factors related to the development of acute renal failure (ARF) after on-pump coronary artery bypass grafting (CABG), between January 2002 and November 2004.
Seventy four patients who underwent on-pump CABG were analyzed retrospectively and distributed into two groups according to the development of ARF. Bivariate and multivariate analyses were performed to analyze. P £ 0.05 was considered statistically significant.
During the period analyzed, 18 patients (24.32%) developed acute renal failure (ARF); 1 patient (1.35%), who required dialysis, died. Associated risk factors identified in-between the development of ARF was: the postoperative use of inotropic or vasoconstrictor drugs (p=0.048) and body mass index greater than 25 (p=0.004). The CPB time did not determine the ARF increase (p=0.0668).
The CPB time was not associated with an increased of ARF following on-pump CABG.
Avaliar a incidência, a mortalidade e os fatores de risco no desenvolvimento de insuficiência renal aguda (IRA) após cirurgia de revascularização miocárdica com o emprego de circulação extracorpórea (CEC), no serviço de Cirurgia Cardiovascular do Hospital Universitário da Universidade Federal de Mato Grosso do Sul, de janeiro de 2002 a novembro de 2004.
Estudo retrospectivo de 74 pacientes submetidos à revascularização miocárdica com circulação extracorpórea, distribuídos em dois grupos segundo o desenvolvimento ou não de insuficiência renal aguda, diagnosticada por critérios laboratoriais. Foram realizadas análises estatísticas bivariada e multivariada, com significância de 5%.
A incidência de IRA foi de 24,32%, sendo que 5,56% necessitaram de diálise, correspondendo a 1,35% do total de pacientes avaliados. A mortalidade por IRA foi de 5,56%. O uso de drogas inotrópicas ou vasoconstritoras no pós-operatório (p=0,048) e o IMC maior que 25 kg/m2 (p=0,004) foram fatores determinantes para o desenvolvimento de IRA. O tempo de circulação extracorpórea foi baixo, não influenciando um aumento significativo de IRA pós-operatória neste estudo.
O tempo de CEC não esteve associado a um aumento estatisticamente significativo da incidência de IRA pós-operatória na cirurgia de revascularização do miocárdio.
INTRODUCTION
Usually, myocardial revascularizations are performed with the aid of cardiopulmonary bypass (CPB) and light-to-moderate hypothermia. However, the most recognized complication following cardiac surgery is acute renal failure (ARF), which has been the cause of high mortality and morbidity [1-22]. The increase of renal dysfunction has been related to a number of factors, with the most important being the use and the time of CPB, age, preoperative renal function, use of inotropic drugs, use of intraoperative furosemide, and associated comorbidities, such as diabetes, heart failure, and peripheral vascular disease, among others [2-14].
The nature of heart surgery impact on renal function is not completed clarified and one of the most common risk factors is the use of CPB. Among the consequences of this method probably involved in the pathophysiology of ARF, we can list the following: nonpulsatile renal blood flow, increases in levels of circulating catecholamines and inflammatory mediators (IL-1, IL-6, IL-8), macroembolic and microembolic insults to the kidney, electrolytic disorders (hypomagnesemia), and the increase of free hemoglobin resulting from hemolysis [5,18,20]. Nevertheless, some authors do not take into consideration the CPB adverse effects, ascribing renal dysfunction to reduce blood flow, increase of renal vascular resistance, and to hemodynamic changes from the surgery itself [2].
As a result of the aging of Brazilian population and the increasingly patients' requirements to undergo myocardial revascularizations surgeries, it is of vital concernment to identify the risk factors related to one of the most important postoperative complications resulting from such a therapeutic procedure - the acute renal failure.
After reviewing the available literature, it was observed an incidence of 0.7% to 31% [2-14] of ARF after on-pump coronary artery bypass grafting and requirements of dialitic therapy of 0.9% to 4.9% [5,11,12].
Currently, there is no consensus about the most prevalent factors associated to postoperative ARF, making it difficult to stratify the risk for the development renal dysfunction. It is worth mentioning that the comparison among the studies is, in a way, difficult as a consequence of the several classification criteria between normal renal function and ARF used.
Taking into account the current data available in the pertinent literature and the lack of Brazilian studies concerning the addressed theme, and in the attempt to acknowledge the risk factors of the predisposing patients to this complication, this study was designed to provide a better medical care during pre-, intra-, and postoperative periods.
OBJECTIVE
To assess incidence, mortality, and risk factors associated with ARF in the postoperative on-pump coronary artery bypass grafting in patients attending the Cardiovascular Surgery service at the Hospital Universitário da Universidade Federal de Mato Grosso do Sul from January 2002 to November 2004.
METHODS
Medical records of 102 patients were retrospectively analyzed. Of these, 74 met the inclusion criteria, which were as follows: patients undergoing myocardial revascularization surgery with cardiopulmonary bypass. These patients were consecutively operated by the same medical staff (surgeons, perfusionists, and anesthesiologists) during the above mentioned period.
Exclusion criteria were death in the first 24 hrs postoperatively, reoperation from possible surgical complications, preoperative serum creatinine > 3.0 mg/dL, and uncompleted tests making it difficult to define acute renal failure. Patients were followed-up over five days or during the admission period in the ICU.
The surveyed data corresponding to preoperative period included age, gender, body mass index (BMI), number of coronary arteries impaired, serum creatinine levels, and comorbidities such as diabetes mellitus, chronic arterial hypertension, congestive heart failure, peripheral arterial insufficiency, and previous episodes of stroke, angina, and acute myocardial infarction. Length of CPB time was evaluated postoperatively.
Following the pattern longitudinal median sternotomy, cardiopulmonary bypass was instituted using ascending aortic cannulation and a two-stage venous cannulation in all patients after systemic heparinization with 4 mg/kg repeated according to activated clotting time (ACT), aiming at keeping it over 450 seconds. Perfusions were performed with light hypothermia (32°C) with intermittent aortic clamping. All disposable artificial material used in CBP was not covered with heparin (nonheparinized circuit). Heparin neutralization was performed in all cases with protamine sulfate infusion in a dose of 1:1 diluted in D5W. Roller pump in arterial line and a hollow fiber membrane oxygenator with arterial line filter (Braile Biomédica - São José do Rio Preto - SP) and an approximately 1500 mL of perfusate solution.
Regarding the postoperative period, the following parameters were recorded: serum creatinine levels, central venous pressure, urinary output, need for dialysis, length of stay in the ICU and hospital length of stay.
As an ARF diagnosis criterion, the following were taken into consideration: for patients with preoperative serum creatinine concentrations d" 1.2 mg/dL, increased serum creatinine values; rise in serum creatinine concentrations > 0.5 mg/dL for those with serum creatinine concentrations e" 1.8 mg/dL; rise in preoperative serum creatinine > 1.2 mg/dL and d" 2.0 mg/dL; or increased serum creatinine concentrations of 10 mg/dL in patients with preoperative serum creatinine > 2.0 mg/dL [11].
Our study has limitations. It is a retrospective study, the number of patients studied was significant, but relatively small compared to the studies surveyed, and we used plasma creatinine as a predictor of renal dysfunction, with the most sensitive predictor for such a diagnosis being creatinine clearance [21].
Patients were divided into two groups based on ARF: Group I - patients who evolved with ARF, and Group II - patients who evolved without ARF.
The Chi-square test with Yates' continuity correction (Tables 2x2) or Fisher's exact test was used to compare categorical variables between patients who developed ARF and those who did not. Student's t test, Mann-Whitney test, or Krushal-Wallis test was used to analyze the quantitative variables by comparing the difference between the means of the two groups (normal distribution of the data was previously checked). A multiple logistic regression was used to identify the variables for p < 0.15 (BMI, hospitalization time, postoperative inotropic or vasoconstrictor drug usage, and CPB time). A simple linear regression model was used to analyze the relationship between CBP time and postoperative serum creatinine. Analysis was performed with Epi Info version 3.3.2 and Bio Estat version 4.0.
RESULTS
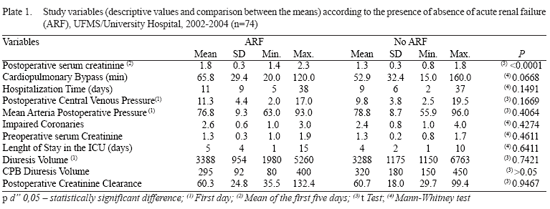
The studied sample was composed of 51 men (68.9%) and 23 women (31.1%). Their mean age was 61.82 years (SD±9.86). The mean age of the patients who presented ARF was 63±11 years and that of those who did not present ARF was 61±9 years. There was statistically significant difference (p=0.4591). Patients' mean BMI in both groups (I and II) was 27±5; 25 kg/m2, and 25±4 kg/m2, respectively. There was a statistically significant difference (p=0.0191). ARF incidence was 24.32% (n=18) among whom 5.56% (n=1) required dialysis, what corresponded to 1.35% of the sample. Mortality associated with ARF was 5.56% (n=1). This death was related to the patient who was submitted to dialitic therapy. Patients' baseline features are expressed in Table 1. The mean length of stay in the ICU of patients with ARF was 5 days (SD±4), while that of those without ARF was 4 days (SD±2). There was no statistically significant difference between these patients (p=0.6411).

Among the categorical variables compared among groups presenting ARF or not, there was a significant difference in the following parameters: BMI > 25 kg/m2 (p=0.004) and use of postoperative vasoconstrictor or inotropic drugs (p=0.048) (Table 2). The quantitative variables were statistically compared and expressed in Figure 1. No statistically significant difference was observed for CPB time (p=0.0668) between both groups.
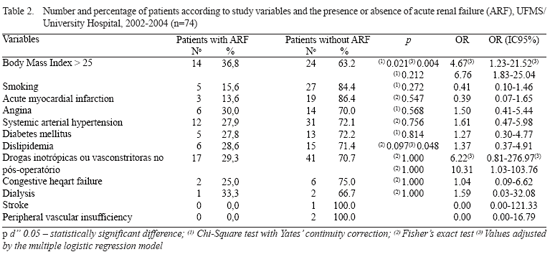
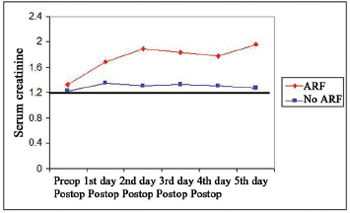
Fig. 1 - Mean preoperative (Preop) and postoperative (Postop) serum creatinine from Day 1 to 5, according to presence or absence of acute renal failure (ARF), UFMS / University Hospital, 2002-2004 (n=74)
There was no statistically significant difference in preoperative creatinine when comparing patients with and without ARF (p=0.4611), however, there was a statistically significant difference ranging from day 1 to 5 postoperatively (p ranging from <0.001 to 0.0002). Taking into consideration only the postoperative serum creatinine in each group separately, there was no statistically significant difference from day 1 to 5 in patients with and without ARF (p=0.6709 vs p=0.7230), respectively (Figure 1).
When comparing postoperative serum creatinine and CBP time by means of a simple linear regression model (b=0.0037; t=3.1797; p=0.0022; R2 (adjusted) = 11.10%), only 11% of the dependent variable (creatinine) is explained by the independent variable (CPB). This means that other variables are involved in the increase of serum creatinine after surgery (Figure 2).
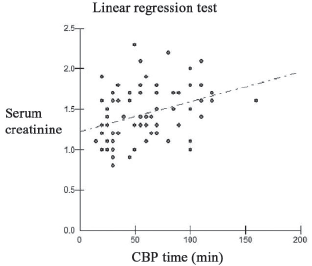
Fig. 2 - Postoperative serum creatinine in relation to the CPB time of patients with presence or absence of acute renal failure, UFMS / University Hospital, 2002-2004 (n=74)
ARF has been widely documented as an important postoperative complication for myocardial revascularization, once considerable increase of morbimortality is associated to this event.
In the present study, it was evidenced an incidence of both ARF and mortality (24.32% and 5.56%, respectively) for those who developed ARF. In the literature values ranging from 0.7% to 31%, and 1.3% to 90%, respectively, were found [2-14]. It is worth mentioning that the disagreeing incidence values are often due to the different criteria of ARF used. Attempting not to underestimate the several stages of renal dysfunction, we used more accurate criteria than some of the studies analyzed did. Because serum creatinine is an easy test to be performed and due to its use as a routine text in UFMS Cardiovascular Surgery Service, it was chosen as an assessment parameter of renal dysfunction.
Some studies [3,5,11,14] demonstrated a higher length of hospital stay for patients who developed ARF, exposing these patients to in-hospital morbidities, besides the hospital admission costs. Notwithstanding, in the present study, the mean length of stay in the ICU for those patients who developed ARF was 5 days, and for those who did not was 4 days. There was no significant statistical difference (p=0.6411).
In scientific literature, many factors have been related to the increase of renal injury incidence and the most important ones are the CPB use and time [3-5,7,11,13]; age [3,5,7,11]; preoperative renal function [3-5,7-11,22]; use of inotropic drugs [11]; use of intraoperative furosemide [10], and comorbidities associated such as diabetes [5,7], heart failure [5.7,8], and peripheral vascular disease [8].
In the present study, the statistical analysis of all probable risk factors showed a correlation between patients' overweight or obesity and the use of vasoconstrictor or inotropic drugs postoperatively, thus evidencing the severity of some patients as a consequence of complications such as ventricle dysfunction with postoperative ARF incidence. Besides, it was not observed any relation between previous comorbidities and the development of ARF.
The relationship between the reduction of daily mean pressures - MAP and CVP - on the first postoperative day and the increase in serum creatinine in these patients reflected the importance of prerenal mechanism, thus contributing to the deterioration in postoperative renal function. According to Mangano et al. [5] the major risk factor for the development of renal dysfunction in the postoperative period was the low cardiac output syndrome and the hemodynamic instability, indicators of which were hemorrhage, and use of inotropic drugs and intraaortic balloon pump. Such a study showed that among patients with cardiac index < 1.5 L/min/m2, at the day of surgery, 20% developed ARF and among those who presented such an index on the first day postoperatively, 61% evolved to renal dysfunction.
In the present study, the CPB time was not the most important factor in the development of ARF, what is corroborated by other studies [3-5,7,11,13]. Attempts to explain such a phenomenon have been controversial in the literature by holding ARF responsible for the blood flow reduction during CPB. Boldt et al. [13] concluded that a CPB time > 90 minutes was the most important risk factor for ARF with the hypoxic effects being account for the reduced blood perfusion, which leads to distress and death of proximal convoluted tubule cells. Other authors further highlighted the homeostasis changes due to plasma inflammatory cytokines with an enhanced filtration being more likely to be responsible for tubular damage [5,14-17].
Ascione et al. [6] observed that during CPB there has been a significant increase of creatinine clearance in the group of patients undergoing CPB as a consequence of renal autoregulation mechanism, thus increasing the glomerular filtration capacity. In the meantime, in this same group there has been a clearance reduction in the following days followed by an increase of the N-acetyl glucosaminidase (NAG) activity - an important renal tubular damage marker, thus corroborating the influence of CPB use in the pathophysiology of ARF postoperatively.
It must be emphasized that the mean CBP time in the present study was low (56.08 minutes) comparing to other studies, even though some studies have included other heart surgery modalities besides myocardial revascularization. Only one of the surveyed studies [6] evaluated myocardial revascularization surgeries alone and provided data regarding the duration of CPB time, which was of 70.3 minutes.
In the present study, due to its limitations, because it is a clinical trial analyzing multiple factors, one can conclude that CPB did not determine the impact on ARF occurrence in myocardial revascularization postoperative period, probably due to the low CPB mean time in the studied group, what also yielded a low morbimortality and a better course of renal function of these patients postoperatively. Increased BMI has been shown to be a risk factor for the development of ARF besides the use of inotropic or vasoconstrictor drugs in more severe patients who presented ventricular dysfunction. Al the other variables studied were not presented as a risk factor in the occurrence of ARF for this group.
Although there is not a specific guidance as for the prophylaxis of ARF development in heart surgeries postoperative period with the use of CPB, in the available literature, in the present survey we could observe a better prognosis of the renal function when both CPB time is not prolonged and adequate optimization of postoperative cardiac output have been reached.




 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license