INTRODUCTION
Pulmonary ischemia/reperfusion (IR) presents intense inflammatory response, with the infiltration of neutrophils in the lungs, endothelial injure of the micro-vases and pulmonary edema. Furthermore, IR results in excessive production of reactive species of oxygen and decrease in production or availability of nitric oxide, causing harmful effects to tissues. Moderate exercise training promotes benefic effects either in the prevention as in the treatment of several diseases, such as high blood pressure, diabetes mellitus and atherosclerosis. Despite the role of exercise as prevention against inflammatory diseases, and more specifically, against pulmonary diseases related to the process of IR, it still requires more studies. Recent researches in our laboratories using experimental models of pulmonary IR showed that moderate physical preconditioning, promotes significant beneficial effects [1-3]. Therefore, physical preconditioning can be of great relevance either to reduce comorbidities or to prevent postsurgical complications associated to the process of pulmonary IR.
This review was based on a bibliographic research of scientific articles in English and Portuguese found in the SciELO and MEDLINE database (from 1987 to 2008) and also classical texts related to the topic. The primary search strategy involved the combination of the following keywords: ischemia, reperfusion, pulmonary ischemia/reperfusion, inflammatory response, reactive species of oxygen, oxidative stress, antioxidant defense and physical conditioning. In addition, it was performed a secondary search including the list of references of the articles found in the primary search.
ISCHEMIA/REPERFUSION AND PULMONARY COMPLICATIONS
One of the situations that causes major complications after cardiothoracic surgeries is the IR process that causes intense inflammatory response, causing serious complications and pulmonary dysfunction. The reperfusion acute lesion has become an important factor of morbidity in cardiothoracic surgeries, with significant impacts in expenses and health care. Furthermore, the International Heart and Lung Transplantation Society showed that the most significant risk factors for the development of postsurgical complications or death for transplanted patients are: donor's age and time of organ's ischemia [4]. Although there are considerable advances in the transplantation immunology area, the reperfusion acute lesion or the reimplantation response remain as considerable source of morbidity, reckoning, diagnostic and the management of postsurgical complications still need further advances [5].
The integrity of the endothelial cells and the vascular smooth muscles is of crucial importance in the maintenance of alveolar perfusion for the pulmonary physiology, regarding gas exchange and homeostasis of the system. The blood vessels, usually, have three layers: the inner layer, which is in contact with the blood elements and basically consists of endothelial cells; the middle layer, consisted by smooth muscle cells; and the adventitial layer, consisted by fibrous conjunctive tissue which overlays the external part of the vessel. The endothelial cells are responsible for the synthesis, metabolism and release of a large variety of mediating agents that regulate the vascular tonus, vascular permeability, metabolism of endogenous and exogenous substances, and platelet and leukocyte activity. The substances produced by the endothelium can be divided in vasodilating agents, such as prostacicline (PGI2), nitric oxide (NO) and endothelium-derived hyperpolarizing factor (EDHF), and vasoconstrictor agents, such as endothelines, prostaglandin H
2 (PGH
2), tromboxane A
2 (TXA
2) and the reactive species of oxygen (RSOs) [6]. Amongst this variety of substances, the NO deserves special attention due to its role in the mechanism of vasodilation and neutralizer of EROS. Enzymes known as NO synthesis (NOS), which are divided in two large groups of constitutive isoforms (cNOS: eNOS-endothelial and nNOS-neuronal), and undividable isoform (iNOS) are capable of catalyzing the oxidation of terminal nitrogen of the guanidine group of L-arginin, forming NO and L-citrulin. Once released, NO promotes several actions in the cardiovascular system, among them, platelet aggregation inhibition, vasodilation, inhibition of cellular growth and inflammatory response and neutralization of RSOS [7]. In addition, the endothelial cells present in the lung vessels play important role in the synthesis and degradation of substances present in the blood, such as angiotensin and bradicinin [6].
Vascular functional alterations associated to the process of IR may be involved in pulmonary complications related to the development of several diseases, such as pulmonary high blood pressure (PHBP) and acute respiratory anguish syndrome (ARAS). The PHBP is defined as an increase in the mean pressure of the pulmonary artery higher than 25 mmHg (rest) or higher than 30 mmHg (exercise), with occlusion pressure of the pulmonary artery lower than 15 mmHg [8] and it is considered a serious clinical situation. It is known that the lesion and/or dysfunction of the endothelial cells is related to the development of PHBP, to the unbalance between the vasodilating and vasoconstrictors mediators, including the decrease in production of PGI2 and NO and increase in the production of endotheline (ET-1) and TXA2 [9]. The initial endothelial lesion results in restoring local vasoactive mediators, promoting a pro-clotting state, leading to the consequent vascular obstruction. Moreover, defects in the potassium channels of the smooth muscles of the pulmonary circulation seem to be involved in the beginning and/or progression of PHBP [10].
The acute respiratory anguish syndrome (ARAS) is considered the most serious respiratory dysfunction [5,11]. ARAS is described as an event of acute pulmonary lesion, associated to an acute pulmonary edema, non-hydrostatic or non-cardiogenic, followed by a serious hypoxemia, responsible for high rates of mortality. It is characterized by damage to the endothelium and pulmonary epithelium, with consequent lesion to the capillary alveolus membrane. There are many mediators that are ascribed as cause and perpetuators of the syndrome, but, in general, its pathogenesis consists of two aspects: the direct effects of the lesion on the pulmonary cells and an acute systemic inflammatory response that may include cellular and humoral components. Despite the fact of ARAS having been first described more than 30 years ago, many doubts still persist regarding its definition, physiology, physiopathology and treatment [12-14].
The IR pulmonary lesion consists in an important common physiopathologic event to several situations in clinical practice. Its local and systemic effects can be studied in conditions that involve lung transplantation, cardiothoracic surgery, occlusion of the pulmonary artery, pulmonary thromboembolism, total pneumothorax and important pleural suffusion [15]. Ischemia is characterized by the interruption of oxygen and nutrients supply to a certain area, it leads to tissue dysfunction and, depending on the degree of ischemia, it can cause necrosis of the tissues. The damages to the tissues depend on the characteristics of the tissue involved, ability of capillary restoration in microcirculation, metabolic demand, available oxygen supply, and the ability of producing energy by anaerobic metabolism. The IR lesion can be defined as the damage that occurs in a tissue with the restoration of blood flow, after the period of ischemia [16-18].
Evidences show that the lesion of tissues is not only limited to ischemia, but during or after reperfusion, tissue compromising is also of great clinical relevance. Reperfusion can damage individually an organ severed by ischemia, as it occurs in organ transplantations or it can extent to other organs, due to a systemic inflammatory response, in which inflammatory mediators are produced and released in the blood flow, reaching deferent organs [19-21].
The pulmonary ischemia occurred as result of the pulmonary artery occlusion followed by reperfusion is associated to the infiltration of neutrophils in the lungs, endothelial lesion of the microvases and pulmonary edema [22,23]. The RSOs derived from the neutrophils can cause tissue and vessel damage by the adherence of polimorfonuclear neutrophils in the endothelial cells [20,24]. Furthermore, the cellular response involves neutrophils, macrophages/monocytes and lymphocytes, which have an important role in the process that includes bonding, chemotaxis and the activation of these leukocytes [14,16]. This intercellular interaction is done by bonding molecules (adesines, integrines and selectines), present in the endothelial cells and inflammatory [25]. The events involved in the systemic inflammatory response include plasmatic alterations, such as activation of the complementary system, coagulation/fibrinolysis and cynines, increase of the pro-inflammatory mediators; cytokines as a factor of tumoral necrosis a (TNF-a), interleukin 1ß (IL-1ß), interleukin 6 (IL-6), interleukin 8 (IL-8), oxidant lipid mediators, proteases, nitric oxide and neuropeptide and induction of protein synthesis. These factors are considered responsible for cellular damage and alterations in the surface-active agent (an important substance that acts reducing the superficial tension of the liquids that overlay the interior of the alveoli and other respiratory means), disturbing the ventilation/perfusion relation, resulting in hypoxemia [26]. Commonly, the IR corresponds to the anoxia-reoxygenation in the transplanted organs, however, the lungs are considered different, for they contain oxygen in the alveoli during ischemia. Thus, in the lungs, the oxidative stress resulting from ischemia must be distinguished from that resulting from other organs [18,27,28].
INFLAMMATORY RESPONSE IN THE ISCHEMIA/REPERFUSION PROCESS
The cytokines consist of a large number of glycoproteins of low molecular weight that act in the cellular intercommunication. The most important aspects of these proteins are their vast specter and action potential. They can be produced by any cell of the body, but the erythrocytes and they are related to stimulation and suppression of the events of immune response, triggering and coordinating the inflammatory response [29].
The inflammatory response that can lead to dysfunction and failure of an organ is one of the most serious problems after the occurrence of lesions under different conditions, such as in sepses, serious burning, acute pancreatitis, hemorrhagic shock, trauma and transplants [30,31]. It is known that pro-inflammatory cytokines have an important role in the IR lesion of the heart, kidneys, small intestine, skin and liver, but little is known about their role in pulmonary IR lesion [32].
An important cytokine is released during the IR process is TNF-a. This cytokine, besides of having a direct cytotoxic effect on the endothelium, stimulates the production of other cytokines, such as the interleukins. These substances interact with the endothelial cells, increasing the pro-coagulating activity and the production of the plasminogen inhibitor, facilitating coagulation and promoting the activation of neutrophils, monocytes and lymphocytes that on their turn, release superoxide anions (O
2-) and other RSOs that participate in the process of endothelial tissue lesion [31]. Studies evidence that the TNF-a alters the selectivity of the endothelial barrier and produces pulmonary edema in experimental models, the TNF-a increases the pulmonary vascular resistance, which results in alveolar edema, being a result of the release of tromboxane A
2 (TXA
2) in response to the activation of polimorfonuclear leucocytes [33,34].
Another important interleucine in the inflammatory response linked to the IR is IL-1ß, characterized also as pro-inflammatory, is connected to the activation of neutrophils and induces the connection of molecules linked to the leucocytes and endothelium. The IL-1ß induces the action of the cicloxigenase (COX) and the expression of the inductive nitric oxide syntax (iNOS). It also increases the expression of other cytokines such as the TNF-a, IL-6 and the linking molecules [35]. The COX is an important enzyme present in the cellular membranes, that produces prostanoids from the arachnoidal acid, it can be divided into two subtypes, COX-1 and COX-2; more specifically, the COX-2 is associated to the inflammatory response and production of important mediators, such as the cytokines [36].
The IL-6 possesses an important role in the acute inflammatory response and it is produced by different types of cells, such as monocytes, fibroblasts and endothelial cells, being the main source for the production of the IL-6, lipopolysaccharides, IL-1 and TNF-a. Initially, it was believed that the IL-6 played only a pro-inflammatory role, but recent studies suggest that it plays an anti-inflammatory role as well, being very important for the return of homeostasis after the inflammatory process. High plasmatic concentrations of IL-6 have been confirmed in several conditions in which the homeostasis of the system is compromised or jeopardized such as sepsis or multiple traumas [37,38]. The role of the IL-6 in the lung transplantation is still not well established and there are conflicting results. Although, high levels of IL-6 were observed in the lesion of respiratory means and pulmonary tissue after inflammatory stimuli, but the functional relevance of these findings still remains unclear[39,40].
OXIDATIVE STRESS AND REACTIVE SPECIES OF OXYGEN
Several authors have shown direct association between the increase in the production of reactive species of oxygen (RSOs) and several human pathologies, among them brain stroke, myocardial infarction , atherosclerosis, IR lesion, rheumatoid arthritis and aging [41-43]. Furthermore, the RSOs play an important role in ARAS and in pulmonary and vascular lesion after the process of pulmonary IR [44]. Especially, the neutrophils linked to the pulmonary vascular endothelium during pulmonary IR are responsible for the tissue damage through the production of the RSOs [26,45].
The oxidative stress involves the production of RSOs by different cells of the body, such as the endothelial cells, the smooth muscle cell, cells from the adventitial layer, cells from the immunologic system, among others. The RSOs are formed by intracellular and extracellular enzymatic activity, being the oxidase xantine, the cytochrome P450, by the cycloxigenase, the endothelial nitric oxide sintetase (eNOS) disconnected and the NADPH oxidase, the main enzymes involved in this process. The NADPH oxidase is the main forming enzyme of superoxide anion (O2-) that possesses high cytotoxicity and is involved in the genesis of the pulmonary IR lesion [46-48].
The NADPH oxidase is an enzyme consisted of several subunits, such as the p22
phox and gp91
phox (Nox2), p47
phox, p67
phox, p40
phox, and the small guanosine-triphosphate (GTP)-linked to the Rac protein [48,49]. This complex is involved in the production of O
2-. The enzyme eNOS disconnected may also be an important source of O
2- and the aforementioned production occurs when the bioavailability of L-arginine or of (6R)-5,6,7,8-tetraidrobiopterine (BH
4), substrates for the formation of nitric oxide (NO), are in short concentrations [50]. The reaction of the O2-with the NO produced by the endothelial cell reduces its bioavailability, generating a highly unstable molecule, the peroxinitrite (OONO
-), capable of oxidizing proteins, lipids and nucleic acids, causing cellular damage through the activation of the nuclear factor kappa B (NF-kB), growth factors, and cytokines, that on their turn trigger structural and functional alterations, such as the vascular remodeling, increase of extracellular matrix proteins deposition, increase in the inflammatory process and endothelial permeability in the tissues involved [51].
The antioxidant enzymes consist in the main line of defense to the oxidant components of the system. Amongst the antioxidant enzymes present in the vascular tissue, there is the catalase (CAT), glutatione peroxidade (GSH-Px) and more three types of superoxide dismutase (SOD), being the SOD-1 dependent of the Cu/Zn, present in the nucleus and in the citosol, the SOD-2 dependent of the Mn, present in the mitochondria and the SOD-3 dependent of the Cu/Zn, present in the extracellular matrix. In the SOD enzyme, its system seems to be specific for the dismutation of O
2-, thus, forming hydrogen peroxide (H2O2). The CAT and the GSH-Px play an important role in the elimination of H
2O
2, thus, promoting water formation. The perfect balance among the antioxidant enzymes is important for maintaining cellular integrity, for SOD, CAT and GSH-Px prevent the accumulation of O
2- and H
2O
2, preventing cellular damage [52] (Figure 1).
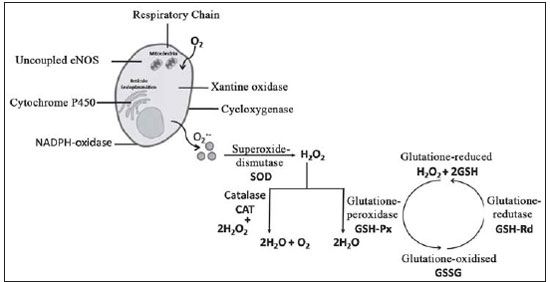
Fig. 1 - Oxidant and antioxidant enzymatic system. eNOS = endothelial nitric oxide synthesis; O2+- = super-oxide anion; H2O2 = hydrogen peroxide). Adapted from Fortuño et al. [48] and Ray & Shah [49]
Exercise training is an activity performed with a systematic repetition of oriented movements, with consequent increase in the consumption of oxygen due to muscular requirement. Exercise training provokes a series of physiological responses in the body systems and, especially, in the cardiovascular system, aiming to maintain the cellular balance due to the increase of metabolic demands and consumption of energy [53,54]. It is known that moderate exercise training, performed on a regular basis, promotes positive effects either in preventing as in the treatment of cardiovascular diseases, and its regular practice has been recommended by different health associations throughout the world. Its benefits have also been shown in the prevention and treatment of high blood pressure, diabetes mellitus, dislipidemia, obesity and osteoporosis. Thus, the low levels of physical activity or exercise training are considered risk factors for the development of these diseases [55-57].
These benefits are related to the increase in production of vasoactive substances, such as NO, and/or to the increase of its availability in the endothelial cells [58-60]. It is known that exercise training increases the flow of pulsating blood and the pressure that the blood exerts over the vascular wall and the shearing force over the endothelial cells are powerful stimuli for generating NO in the vascular system. Therefore, one of the beneficial effects of regular exercise training is closely related to its ability of stimulating the synthesis of NO by the endothelial cells [61,62]. Another vascular change caused by exercise training is related to the expression and activity of antioxidant enzymes. Amongst these enzymes, the SOD-1 Cu/Zn is the most sensitive to the shearing force caused by exercise training [63].
Nevertheless, there are few studies relating the chronic role of exercise training as protector against inflammatory diseases, and more specifically against pulmonary diseases associated to the pulmonary IR lesion. The response of cytokines to acute exercise differs from that seen in the IR lesion IR. It is noticed that classical pro-inflammatory cytokines, TNF-a and IL-1ß, generally do not increase with exercise training, indicating that the cascade of cytokines induced by exercise training differs from the cascade induced by the IR [64,65]. Recent studies performed in our laboratory using experimental models showed that moderate physical training previous to the process of IR pulmonary IR promotes a decrease in the overfilling of proteins in the lungs, diminishing vascular permeability and, consequently, pulmonary edema permeability. Physical training also promoted decrease in the plasmatic levels of the TNF-a and IL-1ß, increase in the plasmatic activity of the antioxidant enzyme SOD in this experimental model [2]. More recently, it could be observed that physical training promotes reduction in the super-expression of the cytosolic subunit of the NADPH oxidase p47
phox triggered by pulmonary IR in the mesenteric artery of rats [3]. All these data evidence the beneficial effects of physical training in preventing inflammatory responses before the process of pulmonary IR, as well as increase in the antioxidant defense, crucial for the control of RSOs. It was also shown that pulmonary IR causes local and systemic vascular and inflammatory alterations in the body, and physical training helped controlling these alterations on a systemic level [1-3] (Figure 2).
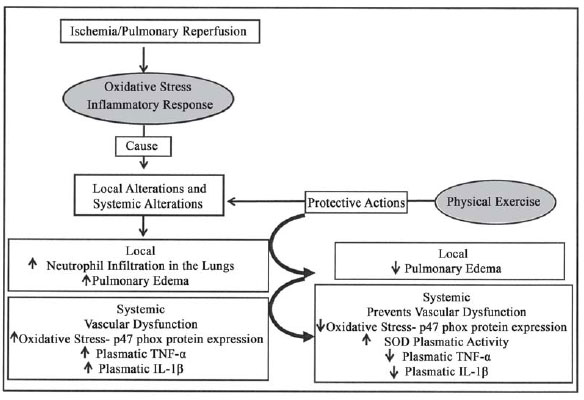
Fig. 2 - Effects of moderate exercise training previous to the process of pulmonary IR. TNF-á = tumoral necrosis factor á ; IL-1â = interleukine 1â; SOD = super-oxide dismutase;, p47phox = cytolosic sub-unit of NADPH oxidase p47phox
The protocol of exercise training known for improving cardio-respiratory ability is the moderate type (running, swimming, bicycle-riding are the most common), with intensity between 50 to 75% of maximum oxygen consumption (VO
2max), with 3 to 5 weekly sessions and duration between 30 and 60 minutes of continual activity [66,67]. Considering the great individual variability in response to exercise training prescription regarding the amount of training (involving intensity, frequency and duration) it is necessary to evaluate the physical and clinical conditions of each individual in order to attain the most beneficial effects.
Thus, the intensity of exercise training can be measured by the maximum cardiac frequency (maxCF) using the formula: maxCF = 220 - age. From that formula is possible calculate the desired maxCF rate, and then determine the different intensities, considering moderate exercise between 55 and 80% of maxCF. It is also possible to determine the intensity of exercise training from the reserve cardiac frequency (reserveCF), in which is considered the cardiac frequency at rest (restCF) and it is applied the following equation [68]: reserveCF = CF rest + I. (maxCF - CFrest); where I is considered the intensity of exercise to be performed in decimal, moderate between 50 to 75% of the CFreserve. The Borg scale of subjective perception of effort must be also used in the training follow-up, considering as reference a moderate level from 12 to 14 in the scale [69,70].
Specifically, the physical exercise program in preparation of patients for cardiothoracic surgeries must involve exercise training (gym bicycle or running on a treadmill) 3 to 5 times a week, from 10 to 30 minutes, that must be done at the same intensity (continuous), between 40 to 60% of the CFreserve, during a period of at least 8 weeks previous to the surgery. Many patients presented limitations due to the decrease in respiratory functions, the moderate exercises produce the best results and must be encouraged; however, the low intensity exercises are also benefic for those patients that are unable to reach that intensity. Breaks during the training can be useful and efficient in promoting tolerance in the practice of exercises of low and moderate intensity. The exercise prescription must involve careful clinical evaluation, making sure that the training sessions as well as the prescription of exercise training must be done by a physical education professional, and be under his supervision. Therefore, the preoperative preparation of patients must involve a multidiscipline health crew. Furthermore, the inclusion of exercise training as a preoperative preparation might be able to reduce the complications resulting from cardiothoracic surgery, reduce the period of hospital internment and, consequently, improve the patient's recovery, which will cause the Health System expenses to be cut down.
The benefits of regular practice of exercise training have also been shown in pulmonary rehabilitation, with increase in the pulmonary function and quality of life in individuals submitted to pulmonary transplantation. These studies involved exercise training (gym bicycle and walking on a treadmill), 3 to 5 times a week, for 30 to 60 minutes, intensity 30 to 60% CFreserve and subjective perception of effort 13 to 14. The minimum time after the transplantation to start the training protocol in these studies varied between 1 and 6 months [71-73]. Thus, the physical training must also be done after the surgery in order to improving the quality of life of the patient and providing independence in his daily and professional activities.
CONCLUSION
The process of pulmonary IR is associated to the infiltration of neutrophils in the lungs, pulmonary edema, intense inflammatory response and local and systemic vascular alterations with a high rate of morbidity and mortality. Moderate exercise training has been employed as an important tool in preventing and/or treating several cardiovascular and endocrine-metabolic diseases. Studies in healthy animal models showed that the regular practice of previous physical exercise improves and/or prevents local and systemic lesions caused by the process of pulmonary IR. Therefore, the regular practice of supervised physical exercise would be of great relevance either in reducing co-morbidities or in preventing postoperative complications associated to the process of pulmonary IR. Consequently, the inclusion of low and moderate exercise training as preoperative preparation and as auxiliary in the postoperative recovery process is of great relevance in the cardiovascular surgery area, for it will result in reduction of the complications caused by the surgical procedure, reduction of the hospital internment period and, consequently, improve in the patient's recovery, resulting in a significant reduction in the costs for the Health System.
ACKNOWLEDGEMENT
We would like to thank FAPESP (Fundação de Amparo à Pesquisa do Estado de São Paulo) for its financial support.
REFERENCES
1. Delbin MA, Moraes C, Camargo E, Mussi RK, Antunes E, de Nucci G, et al. Influence of physical preconditioning on the responsiveness of rat pulmonary artery after pulmonary ischemia/reperfusion. Comp Biochem Physiol A Mol Integr Physiol. 2007;147(3):793-8. [
MedLine]
2. Mussi RK, Camargo EA, Ferreira T, De Moraes C, Delbin MA, Toro IF, et al. Exercise training reduces pulmonary ischemia-reperfusion-induced inflammatory response. Eur Respir J. 2008;31(3):645-9. [
MedLine]
3. Delbin MA, Davel AP, Bau FR, Priviero FBM, Rossoni LV, Antunes E, et al. Reduction in vascular oxidative stress and improvement of NO/cGMP pathway in trained rats after lung ischemia/reperfusion. In: Inter-American Society of Hypertension 18th Scientific Sessions. 17º Congresso da Sociedade Brasileira de Hipertensão, 2009;Belo Horizonte. Hipertensão. 2009;12(supl 1):8.
4. Hosenpud JD, Bennett LE, Keck BM, Boucek MM, Novick RJ. The Registry of the International Society for Heart and Lung Transplantation: seventeenth official report-2000. J Heart Lung Transplant. 2000;19(10):909-31. [
MedLine]
5. Ng CS, Wan S, Yim AP, Arifi AA. Pulmonary dysfunction after cardiac surgery. Chest. 2002;121(4):1269-77. [
MedLine]
6. Zanesco A. Células endoteliais. In: Células: uma abordagem multidisciplinar. 1ª ed. São Paulo:Manole;2005. p.184-91.
7. Ignarro LJ. Nitric oxide: a unique endogenous signaling molecule in vascular biology. Biosci Rep. 1999;19(2):51-71. [
MedLine]
8. Barst RJ, McGoon M, Torbicki A, Sitbon O, Krowka MJ, Olschewski H, et al. Diagnosis and differential assessment of pulmonary arterial hypertension. J Am Coll Cardiol. 2004;43(12 Suppl S):40S-7S.
9. Yildiz P. Molecular mechanisms of pulmonary hypertension. Clin Chim Acta. 2009;403(1-2):9-16. [
MedLine]
10. Ricachinevsky CP, Amantéa SL. Treatment of pulmonary arterial hypertension. J Pediatr (Rio J). 2006;82(5 Suppl):S153-65. [
MedLine]
11. Andrejaitiene J, Sirvinskas E, Bazeliene R. Prevention of pulmonary alterations after cardiopulmonary bypass. Medicina (Kaunas). 2004;40(6):517-21. [
MedLine]
12. Zapol WM, Snider MT. Pulmonary hypertension in severe acute respiratory failure. N Engl J Med. 1977;296(9):476-80. [
MedLine]
13. Cremona G, Dinh Xuan AT, Higenbottam TW. Endotheliumderived relaxing factor and the pulmonary circulation. Lung. 1991;169(4):185-202. [
MedLine]
14. Antoniazzi P, Pereira Jr GA, Marson F, Abeid M, Baldisserotto S, Basile-Filho A. Síndrome da angústia respiratória aguda (SARA). Medicina. 1998:31:493-506.
15. Esme H, Fidan H, Koken T, Solak O. Effect of lung ischemiareperfusion on oxidative stress parameters of remote tissues. Eur J Cardiothorac Surg. 2006;29(3):294-8. [
MedLine]
16. Scannell G. Leukocyte responses to hypoxic/ischemic conditions. New Horiz. 1996;4(2):179-83. [
MedLine]
17. Reilly PM, Schiller HJ, Bulkley GB. Pharmacologic approach to tissue injury mediated by free radicals and other reactive oxygen metabolites. Am J Surg. 1991;161(4):488-503. [
MedLine]
18. de Perrot M, Liu M, Waddell TK, Keshavjee S. Ischemia-reperfusion-induced lung injury. Am J Respir Crit Care Med. 2003:167(4):490-511. [
MedLine]
19. Horiguchi T, Harada Y. The effect of protease inhibitor on reperfusion injury after unilateral pulmonary ischemia. Transplantation. 1993;55(2):254-8. [
MedLine]
20. Carden DL, Granger DN. Pathophysiology of ischaemiareperfusion injury. J Pathol. 2000;190(3):255-66. [
MedLine]
21. Seal JB, Gewertz BL. Vascular dysfunction in ischemia/reperfusion injury. Ann Vasc Surg. 2005;19(4):572-84. [
MedLine]
22. Overand PT, Bishop MJ, Eisenstein BL, Chi EY, Su M, Cheney FW. Lack of alveolar O2 during lung reperfusion does not decrease edema formation. J Appl Physiol. 1989;67(2):528-33. [
MedLine]
23. Chan RK, Ibrahim SI, Verna N, Carroll M, Moore FD Jr, Hechtman HB. Ischaemia-reperfusion is an event triggered by immune complexes and complement. Br J Surg. 2003;90(12):1470-8. [
MedLine]
24. Horgan MJ, Wright SD, Malik AB. Antibody against leukocyte integrin (CD18) prevents reperfusion-induced lung vascular injury. Am J Physiol. 1990;259(4Pt[part]1[/part]):L315-9. [
MedLine]
25. Albelda SM, Buck CA. Integrins and other cell adhesion molecules. FASEB J. 1990;4(11):2868-80. [
MedLine]
26. Novick RJ, Gehman KE, Ali IS, Lee J. Lung preservation: the importance of endothelial and alveolar type II cell integrity. Ann Thorac Surg. 1996;62(1):302-14. [
MedLine]
27. Eckenhoff RG, Dodia C, Tan Z, Fisher AB. Oxygen-dependent reperfusion injury in the isolated rat lung. J Appl Physiol. 1992;72(4):1454-60. [
MedLine]
28. Date H, Matsumura A, Manchester JK, Obo H, Lima O, Cooper JM, et al. Evaluation of lung metabolism during successful twenty-four-hour canine lung preservation. J Thorac Cardiovasc Surg. 1993;105(3):480-91. [
MedLine]
29. Hamblin AS. Cytokines and cytokine receptors. 2nd ed. New York:Oxford University Press;1993.
30. Bhatia M, Moochhala S. Role of inflammatory mediators in the pathophysiology of acute respiratory distress syndrome. J Pathol. 2004;202(2):145-56. [
MedLine]
31. Ertel W, Morrison MH, Wang P, Ba ZF, Ayala A, Chaudry IH. The complex pattern of cytokines in sepsis. Association between prostaglandins, cachectin, and interleukins. Ann Surg. 1991;214(2):141-8. [
MedLine]
32. Krishnadasan B, Naidu BV, Byrne K, Fraga C, Verrier ED, Mulligan MS. The role of proinflammatory cytokines in lung ischemia-reperfusion injury. J Thorac Cardiovas Surg. 2003;125(2):261-72.
33. Hocking DC, Phillips PG, Ferro TJ, Johnson A. Mechanisms of pulmonary edema induced by tumor necrosis factor-alpha. Circ Res. 1990;67(1):68-77. [
MedLine]
34. Koga S, Morris S, Ogawa S, Liao H, Bilezikian JP, Chen G, et al. TNF modulates endothelial properties by decreasing cAMP. Am J Physiol. 1995;268(5 Pt [part]1[/part]):C1104-13. [
MedLine]
35. Putensen C, Wrigge H. Ventilator-associated systemic inflammation in acute lung injury. Intensive Care Med. 2000;26(10):1411-3. [
MedLine]
36. Vane JR, Bakhle YS, Botting RM. Cyclooxigenases 1 and 2. Annu Rev Pharmacol Toxicol. 1998;38:97-120. [
MedLine]
37. Hack CE, Aarden LA, Thijs LG. Role of cytokines in sepsis. Adv Immunol. 1997;66:101-95. [
MedLine]
38. Giannoudis PV, Smith RM, Banks RE, Windsor AC, Dickson RA, Guillou PJ. Stimulation of inflammatory markers after blunt trauma. Br J Surg. 1998;85(7):986-90. [
MedLine]
39. Rizzo M, SivaSai KS, Smith MA, Trulock EP, Lynch JP, Patterson GA, et al. Increased expression of inflammatory cytokines and adhesion molecules by alveolar macrophages of human lung allograft recipients with acute rejection: decline with resolution of rejection. J Heart Lung Transplant. 2000;19(9):858-65. [
MedLine]
40. Teng S, Kurata S, Katoh I, Georgieva GS, Nosaka T, Mitaka C, et al. Cytokine mRNA expression in unilateral ischemicreperfused rat lung with salt solution supplemented with lowendotoxin or standard bovine serum albumin. Am J Physiol Lung Cell Mol Physiol. 2004;286(1):L137-42. [
MedLine]
41. Frederiks WM, Kooji A, Bosch KS. Role of xanthine oxidase activity in tissue damage of rat liver after ischemia. Transplant Proc. 1995;27(5):2855-6. [
MedLine]
42. García-Valdecasas JC, Rull R, Grande L, Fuster J, Rimola A, Lacy AM, et al. Prostacyclin, thromboxane, and oxygen free radicals and postoperative liver function in human liver transplantation. Transplantation. 1995;60(7):662-7. [
MedLine]
43. Halliwell B, Gutteridge JM, Cross CE. Free radicals, antioxidants, and human disease: where are we now? J Lab Clin Med. 1992;119(6):598-620. [
MedLine]
44. Jurmann MJ, Dammenhayn L, Schaefers HJ, Haverich A. Pulmonary reperfusion injury: evidence for oxygen-derived free radical mediated damage and effects of different free radical scavengers. Eur J Cardiothorac Surg. 1990;4(12):665-70. [
MedLine]
45. Russell WJ, Jackson RM. Hydrogen peroxide release by mitochondria from normal and hypoxic lungs. Am J Med Sci. 1994;308(4):239-43. [
MedLine]
46. Lassègue B, Clempus RE. Vascular NAD(P)H oxidases: specific features, expression, and regulation. Am J Physiol Regul Integr Comp Physiol. 2003:285(2):R277-97. [
MedLine]
47. Fortuño A, San José G, Moreno MU, Díez J, Zalba G. Oxidative stress and vascular remodelling. Exp Physiol. 2005;90(4):457-62. [
MedLine]
48. Ray R, Shah AM. NADPH oxidase and endothelial cell function. Clin Sci (Lond). 2005:109(3):217-26. [
MedLine]
49. Bayraktutan U, Blayney L, Shah AM. Molecular characterization and localization of the NAD(P)H oxidase components gp91-phox and p22-phox in endothelial cells. Arterioscler Thromb Vasc Biol. 2000;20(8):1903-11. [
MedLine]
50. Shinozaki K, Kashiwagi A, Nishio Y, Okamura T, Yoshida Y, Masada M, et al. Abnormal biopterin metabolism is a major cause of impaired endothelium-dependent relaxation through nitric oxide/O2- imbalance in insulin-resistant rat aorta. Diabetes. 1999;48(12):2437-45. [
MedLine]
51. Beckman JS, Koppenol WH. Nitric oxide, superoxide, and peroxynitrite: the good, the bad, and ugly. Am J Physiol. 1996;271(5 Pt [part]1[/part]):C1424-37. [
MedLine]
52. Schneider CD, Oliveira AR. Radicais livres de oxigênio e exercício: mecanismos de formação e adaptação ao treinamento físico. Rev Bras Med Esporte. 2004;10(4):308-13.
53. Ferreira ALA, Matsubara LS. Radicais livres: conceitos, doenças relacionadas, sistema de defesa e estresse oxidativo. Rev Assoc Med Bras. 1997;43(1):61-8. [
MedLine]
54. McArdle W, Katch F, Katch V. Fisiologia do exercício; energia, nutrição e desempenho humano. 4ª ed. Rio de Janeiro:Guanabara Koogan;1998.
55. Hull SS Jr, Vanoli E, Adamson PB, Verrier RL, Foreman RD, Schwartz PJ. Exercise training confers anticipatory protection from sudden death during acute myocardial ischemia. Circulation. 1994;89(2):548-52. [
MedLine]
56. Brown DA, Jew KN, Sparagna GC, Musch TI, Moore RL. Exercise training preserves coronary flow and reduces infarct size after ischemia-reperfusion in rat heart. J Appl Physiol. 2003;95(6):2510-8. [
MedLine]
57. Ciolac EG, Guimarães GV. Exercício físico e síndrome metabólica. Rev Bras Med Esporte. 2004;10(6):319-24.
58. Claudino MA, Priviero FB, Teixeira CE, de Nucci G, Antunes E, Zanesco A. Improvement in relaxation response in corpus cavernosum from trained rats. Urology. 2004;63(5):1004-8. [
MedLine]
59. Woodman CR, Thompson MA, Turk JR, Laughlin MH. Endurance exercise training improves endothelium-dependent relaxation in brachial arteries from hypercholesterolemic male pigs. J Appl Physiol. 2005;99(4):1412-21. [
MedLine]
60. Zanesco A, Antunes E. Effects of exercise training on the cardiovascular system: pharmacological approaches. Pharmacol Ther. 2007;114(3):307-17. [
MedLine]
61. Woodman CR, Muller JM, Laughlin MH, Price EM. Induction of nitric oxide synthase mRNA in coronary resistance arteries isolated from exercise-trained pigs. Am J Physiol. 1997;273(6 pt [part]2[/part]):H2575-9. [
MedLine]
62. Kingwell BA. Nitric oxide-mediated metabolic regulation during exercise: effects of training in health and cardiovascular disease. FASEB J. 2000;14(12):1685-96. [
MedLine]
63. Rush JW, Turk JR, Laughlin MH. Exercise training regulates SOD-1 and oxidative stress in porcine aortic endothelium. Am J Physiol Heart Circ Physiol. 2003;284(4):H1378-87. [
MedLine]
64. Munro PE, Holland AE, Bailey M, Button BM, Snell GI. Pulmonary rehabilitation following lung transplantation. Transplant Proc. 2009;41(1):292-5. [
MedLine]
65. Febbraio MA, Pedersen BK. Muscle-derived interleukin-6: mechanisms for activation and possible biological roles. FASEB J. 2002;16(11):1335-47. [
MedLine]
66. Howley ET, Franks BD. Health fitness instructor's handbook. 2nd ed.Champaign:Human Kinetics;1992.
67. American College of Sports Medicine. Manual do ACSM para teste de esforço e prescrição de exercício. Tradução: Paula Chermont P. Estima. 5ª ed. Rio de Janeiro:Revinter;2000.
68. Karvonen MJ, Kentala E, Mustala O. The effects of training on heart rate: a longitudinal study. Ann Med Exp Biol Fenn. 1957;35(3):307-15. [
MedLine]
69. Borg GA. Psychophysical bases of perceived exertion. Med Sci Sports Exerc. 1982;14(5):377-81. [
MedLine]
70. American College of Sports Medicine Position Stand. The recommended quantity and quality of exercise for developing and maintaining cardiorespiratory and muscular fitness, and flexibility in healthy adults. Med Sci Sports Exerc. 1998;30(6):975-91. [
MedLine]
71. Ambrosino N, Bruschi C, Callegari G, Baiocchi S, Felicetti G, Fracchia C, et al. Time course of exercise capacity, skeletal and respiratory muscle performance after heart-lung transplantation. Eur Respir J. 1996;9(7):1508-14. [
MedLine]
72. Stiebellehner L, Quittan M, End A, Wieselthaler G, Klepetko W, Haber P, et al. Aerobic endurance training program improves exercise performance in lung transplant recipients. Chest. 1998;113(4):906-12. [
MedLine]
73. Suzuki K, Nakaji S, Yamada M, Totsuka M, Sato K, Sugawara . K. Systemic inflammatory response to exhaustive exercise. Cytokine kinetics. Exerc Immunol Rev. 2002;8:6-48. [
MedLine]


 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license