Marcos Antonio CanteroI; Rui M. S. AlmeidaII; Roberto GalhardoI
DOI: 10.5935/1678-9741.20120007
ABSTRACT
OBJECTIVE: The objective of this study is to compare the immediate results of patients undergoing on-pump versus off-pump coronary artery bypass graft (CABG) surgery.
METHODS: From January 2007 to January 2009, 177 patients underwent CABG. Of these, 92 underwent off-pump CABG and 85 on-pump CABG. We evaluated the demographics, preoperative risk factors, preoperative functional class, and risk assessment by the EuroSCORE. A comparison between both groups regarding the postoperative evolution was carried out as well.
RESULTS: The mean number of grafts per patient was 2.48 ± 0.43 in the off-pump group versus 2.90 ± 0.59 in the on pump group. In the off-pump group, 97.8% of patients received an internal thoracic artery graft, while in the onpump group, the percentage was 94.1% (P = 0.03). The rate of complete revascularization was similar in both groups. In the off-pump group, the circumflex artery (circumflex branch of the left coronary artery) was revascularized in 48.9% of the patients versus 68.2% of the patients in the onpump group (P = 0.01). Hospital mortality was 4.3% for offpump CABG and 4.7% for on-pump CABG (P = 0.92). The off-pump group had fewer complications in relation to perioperative myocardial infarction (P = 0.02) and use of intra-aortic balloon pump (P = 0.01).
CONCLUSION: The off-pump CABG is a safe procedure with hospital mortality similar to that observed in on-pump CABG, with lower rates of complications and less need for intra-aortic balloon.
RESUMO
ans-serif">OBJETIVO: Comparar os resultados imediatos da cirurgia de revascularização do miocárdio com e sem circulação extracorpórea (CEC).MR: Myocardial revascularization
ECC: Extracorporeal Circulation
FC: Functional class
EuroSCORE: European System for Cardiac Operative Risk Evaluation
NYHA: New York Heart Association
MAP: Mean arterial pressure
CVP: Central venous pressure
STS: Society of Thoracic Surgeons
ACT: Activating clotting time
INTRODUCTION
During the past decades, coronary artery by-pass graft surgery (CABG) has allowed patients with coronary atherosclerotic disease to improve survival, symptoms, and quality of life [1]. From the mid-1990s, efforts focused on ways to reduce complications and make CABG less invasive. Cardiopulmonary bypass (CPB) induces the systemic inflammatory response through activation of the complement system, mainly via the alternative pathway induced by blood contact with the surface of the extracorporeal circuit, which triggers the release of inflammatory mediators such as the interleukin 1, interleukin 6, and tumor necrosis factor responsible for the systemic inflammatory response. In an attempt to reduce the systemic inflammatory response, the off-pump CABG has been rediscovered and refined. In 1964, Kolesov performed the first off-pump CABG in Leningrad [2].
This technique, after the initial experiments [3] has been revived by Buffolo et al. [4] and Benetti et al. [5]. Since then, it has been recommended as a primary treatment option for high-risk patients [6].
Since 1990, the experience with off-pump CABG has increased. In 1999, data from the Society of Thoracic Surgeons (STS) reveal that it represented about 10% of the total CABG surgeries performed in the United States [7]. Since 2001, the number of all surgical revascularization procedures in the United States increased up to 25%. According to STS, this proportion was about 20% until 2007 [9].
In an attempt to evaluate and demonstrate that the offpump CABG is feasible in our country, with results similar to those found in the literature, even in a service located in the countryside of Brazil, the objective of this study was to evaluate the immediate results of patients undergoing onpump and off-pump CABG. We analyzed the demographics of the population and the differences in morbidity and mortality rates at the Cardiovascular Surgery Service of the Hospital do Coração de Dourados, Mato Grosso do Sul, Brazil.
METHODS
According to current guidelines, we screened 177 patients with multiarterial coronary artery disease (insufficiency), who had surgical indication to CABG from January 2007 to January 2009 at the Hospital do Coração de Dourados (Dourados, MS, Brazil). Of these, 92 patients underwent off-pump CABG surgery (Group 1) and 85 patients underwent on-pump CABG (Group 2).
Files were retrieved from hospital registry and reviewed retrospectively through review of the medical records and evaluation of medical examination performed preoperatively. The study was approved by the Local Ethical Committee (committee report nº 004/2009).
Patients were included in the study by an agreement between the surgeons provided that the revascularization might be performed reliably and in a similar manner for both operative techniques. Randomization assignment was not provided. After a detailed explanation of the investigative purpose of the study and the results already obtained in other services, written informed consent was obtained from all participants. Exclusion criteria were the presence of cardiogenic shock or mechanical complications of infarction, ejection fraction changes (<55%), and non-acceptance of the method by the patient.
The following variables were included in the study:
1. Age, type of operation (first operation or reoperation);
2. Clinical stratification of the heart functional class (FC) according to the New York Heart Association (NYHA);
3. The presence of risk factors, such as systemic hypertension, smoking, dyslipidemia, diabetes mellitus, chronic obstructive pulmonary disease, and peripheral arterial insufficiency;
4. Occurrence of complications, such as stroke, perioperative acute myocardial infarction, presence of ventricular and atrial arrhythmias, need for mechanical ventilation > 24 hours, use of intra-aortic balloon pump, surgical bleeding indicating exploratory mediastinotomy and death.
The study data were set with the risk index developed by the European Association for Cardiothoracic Surgery, the European System for Cardiac Operative Risk Evaluation (EuroSCORE) [8]. The model database used by STS [9] was not used due to the lack of some data on all medical records. After the initial trial period of service that began the offpump CABG in mid-2004, all patients were operated on by the same surgeon and surgical team.
Trans- and postoperative monitoring included continuous electrocardiogram with electrodes placed on the posterior (dorsal) surface, mean arterial pressure (MAP) through peripheral artery catheterization, central venous pressure (CVP) by placing a double lumen catheter into the vena cava, pulse oximetry by placing a digital sensor, temperature by using an esophageal thermometer, and urinary output. Anesthesia was induced with fentanyl (5 mcg/kg) and etomidate (0.3 mg/kg) followed by neuromuscular blocking agents to facilitate tracheal intubation, or pancuronium (0.1 mg/kg intravenous bolus, and 0.03 mg/kg in maintenance doses). Maintenance was performed with sufentanil (0.02 mg/kg/min), midazolam bolus dose depending on requirements, and pancuronium (0.03 mg/kg/h). Both inhalation anesthetics and halogens in combination with nitrous oxide (N2O) have also been used. Vasopressors and inotropic support was administered after the onset of mobilization of the heart aiming at appropriate organic and tissue perfusion.
Patients who underwent on-pump CABG received heparin (3 mg/kg) after induction of anesthesia and harvesting of grafts. Patients underwent a median sternotomy, cardiopulmonary bypass established by cannulation of the ascending aorta and right atrium, cannulation of the right superior pulmonary vein with introduction of a catheter for aspiration and decompression of the left ventricle, hypothermia at 28ºC, isothermic blood cardioplegia delivered in an antegrade manner at a ratio of 1:4, followed by distal anastomoses. The proximal anastomoses were performed with partial clamping of the aorta and on a beating heart.
Patients who underwent off-pump CABG received heparin (2 mg/kg) after induction of anesthesia and harvesting of grafts. In both techniques, heparinization was controlled by the activated clotting time (ACT). We have placed a point with Ethibond 2-0 attached to a cotton strip with 3 cm in the pericardial deflection between the inferior vena cava and right inferior pulmonary vein in order to expose completely the heart. Distal anastomoses were performed, and the artery occluded proximally to the anastomosis with a 5-0 polypropylene thread point anchored in Teflon pledge. The area in which the anastomosis was being performed was exposed and stabilized with a suction stabilizer (The Medtronic Octopus® System). At the completion of the distal anastomoses, the systolic blood pressure was maintained at 100 mmHg. The aorta was partially clamped, and the proximal anastomoses performed. Upon completion of the anastomoses, heparin was reversed with protamine sulfate in both groups, and the operation was completed.
Statistical Analysis
In this study, mean age and number of vessels treated were compared by the Student's t test. Other variables were analyzed using the Chi-square test. A p-value of less than 0.05 was considered statistically significant.
RESULTS
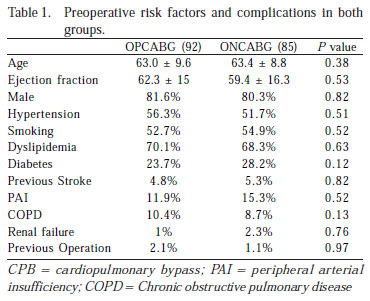
The mean age of the patients was 63.4 ± 8.8 years in the on-pump CABG group versus 63.0 ± 9.6 years in the offpump CABG group, with a range of 29-87 years. There were 75 men (81.6%) in the off-pump CABG and 50 men (59.4%) in the on-pump CABG. Regarding other demographic data, there were no statistically significant risk factors (Table 1).
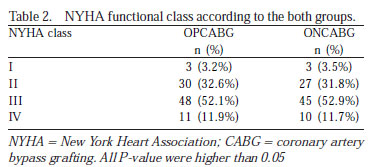
Both groups showed no differences in preoperative NYHA FC (NYHA FC I: Group 1 (3.2%) vs. Group 2 (3.5%); NYHA FC II: off-pump CABG (32.6%) vs. on-pump CABG (31.8%); NYHA FC III: off-pump CABG (52.1%) vs. on-pump CABG (52.9%); NYHA FC IV: off-pump CABG (11.9%) vs. on-pump CABG (11.7%). Elective surgery was required in 56.5% of patients in the off-pump CABG group (52 cases) vs. 60% in the on-pump CABG group (P = 0.70). Considering the mortality rate logistic EuroSCORE, seven patients in the off-pump CABG group were considered low-risk patients (score 0-2), 27 medium-risk (score 3-5), and 57 highrisk (score >6). Six patients in the on-pump CABG group were considered low-risk patients (score 0-2), 25 mediumrisk (score 3-5), and 54 high-risk (score >6).
The extent of coronary artery disease also showed no significant differences between both groups (11 patients (11.9%) with one impaired vessel in the off-pump CABG group vs. two patients (2.3%) in the on-pump CABG group (P = 0.11)). Twenty-five patients (27.1%) had two-vessel coronary artery disease in the off-pump CABG group vs. 22 patients (25.8%) in the on-pump CABG group (P = 0.98). Triple-vessel disease was present in 56 patients (60.8%) in the off-pump CABG group vs. 61 patients (71.7%) in the on-pump CABG group (P = 0.37).
The analysis of the type of coronary lesions showed no differences between the two groups. Thus, 97.8% of the patients in the off-pump CABG group had critical injuries in the anterior interventricular branch of the left coronary artery vs 98.8% in the on-pump CABG group (P = 0.84). Obstructions in the circumflex branch of the left coronary artery were significant (> 50%) on a lesser ratio in the offpump CABG group (P = 0.06). The right coronary artery was affected in 85.8% of patients in the off-pump CABG group and in 80% of the patients in the on-pump CABG group (P = 0.61).
The mean number of grafts per patient was 2.48 ± 0.43 in the off-pump CABG group versus 2.90 ± 0.59 in the onpump CABG group (P = 0.02). The number of grafts performed (Table 3) ranged from 1 to 6 with a higher proportion of patients with one graft (14.1% vs. 2.3%, P = 0.001) and two grafts (35.8% vs. 24.7%, P = 0.03) in the offpump CABG group. However, the on-pump CABG group had more patients with three grafts (58.8% vs. 40.2%, P = 0.004). In off-pump CABG group, 97.8% of patients received internal thoracic artery bypass-graft versus 94.1% in the on-pump CABG group (P = 0.03). The rate of complete revascularization was similar in both groups (69.5% in the off-pump CABG group vs. 67.0% in the on-pump CABG group, P = 0.68). The anterior interventricular branch of left coronary artery was revascularized in 92.3% of patients in the off-pump CABG group, the right coronary artery in 54.3% and the circumflex branch in 48.9%; in the on-pump CABG group, these proportions were 90.5%, 67.0%, and 68.2% respectively. There was a statistically significant difference in the amount of grafts using the circumflex branch of left coronary artery in 48.9% of the patients in the offpump CABG group versus 68.2% of the patients in the onpump CABG group (P = 0.02).

The proportion of grafts in the anterior interventricular branch of left coronary artery and in the right coronary artery was similar in both groups. The conversion rate to on-pump CABG was 5.4% (five cases). Hospital mortality in the off-pump CABG was 4.3% versus 4.7% in the onpump CABG group (P = 0.92).
The most common complication was atrial fibrillation, which occurred in 12.9% of the patients in the on-pump CABG group versus 12% of the patients in the off-pump CABG group.
Among other complications (Table 4), the least frequent in the off-pump CABG group was the perioperative infarction rate (7.6% versus 16.4% in the on-pump group (Group 2) (P = 0.04)). The need for intra-aortic balloon pump was 3.2% in Group 1 vs. 11.7% in Group 2 (P = 0.01). It is noteworthy that the groups were similar in risk score, ventricular function and NYHA FC. Therefore, the groups were homogeneous, although there was no randomization.

DISCUSSION
The literature worldwide shows that off-pump CABG has been a viable option for the treatment of severe coronary insufficiency [10,11].
A systemic inflammatory response can be caused by platelet degranulation, activation of neutrophils and monocytes, and release of cytokines, thus contributing to cardiac dysfunction after CPB. The inflammatory response impairs lung function; CPB adds lung injury and delays the recovery of respiratory function [12]. Several studies [13] compared the inflammatory response with and without cardiopulmonary bypass by measuring serum concentrations of cytokines and acute-phase proteins before and after surgery. There was a significant attenuation of the inflammatory response during cardiopulmonary bypass. With the reduction of inflammatory response, the pathophysiological analysis may reduce organ dysfunction, which makes off-pump surgery less harmful.
The risks of CABG have increased in recent years due to patients' older age, the greater number of patients undergoing prior angioplasty and also by the expansion of indications for certain groups of patients, especially those with severe ischemic cardiomyopathy and comorbidities. Such conditions confirmed the distribution of patients in EuroSCORE, in which most of them are in the range of high risk.
A randomized meta-analysis (ROOBY Trial) showed that off-pump CABG surgery was associated with worse outcomes and lower graft patency [14]. Observational studies have already suggested similar results to conventional CABG [15]. The effectiveness of off-pump CABG surgery has been demonstrated in patients with multivessel disease [22], or in those with disease in the left coronary artery [16], and in high-risk patients preoperatively as well [17].
The lack of a clear benefit in clinical trials that compared patients who underwent off-pump versus on-pump CABG, led to the meta-analysis of 22 observational studies and 37 randomized clinical trials [18].
In observational studies, off-pump CABG surgery was associated with significant reductions in all points, such as 30-day mortality, myocardial infarction, stroke, atrial fibrillation, and acute renal failure
In randomized clinical trials, off-pump CABG surgery was not associated with any significant reduction in 30day mortality and myocardial infarction. It showed a relevant reduction in the incidence of stroke and atrial fibrillation. There was no significant reduction in acute renal failure.
The benefits of the off-pump CABG surgery in the elderly [19], in patients undergoing hemodialysis [20] and, lately, in females [21] were shown in several subgroups of patients. In Brazil, other services have recorded their experiences demonstrating that myocardial revascularization without cardiopulmonary bypass is a procedure that can be performed with low surgical risk and with excellent results [22]. It is considered as an independent protective factor for some complications such as mediastinitis [23] and the need for blood transfusion [24].
There was no difference between groups in the rate of complications. Analyzing the incidence of perioperative infarction in our sample, we found a higher incidence in onpump (12.9%) versus off-pump (7.6%) CABG surgery. These data are similar to those found by Demers et al. [25], who reported 5.1% of acute myocardial infarction post-CPB versus 2.0% without CPB. Lima et al. [26] also reported 8.0% and 4.3%, respectively.
The need for intra-aortic balloon pump shows a statistically significant reduction in the off-pump CABG group (3.2%) compared to patients undergoing on-pump CABG surgery (14.1%) (P = 0.01). There was no difference between groups in the NYHA FC, in left ventricular function, and risk score, making them homogeneous, although they were not randomized.
The off-pump CABG surgery allows a complete revascularization rate similar to that of patients undergoing on-pump CABG, as well as a percentage of use of left internal thoracic artery superior in Group 1, which may be due to the need to avoid manipulation of the ascending aorta. The number of grafts per patient, however, was lower in the offpump CABG group. The statistically significant decrease of the grafts performed (Table 3) using the circumflex branch of the left coronary artery in the off-pump CABG group should be hold responsible for this result.
As in the ROOBY study [14], our study did not show significant difference in mortality. Data were confirmed by three large meta-analyses [27]. It was reported a mortality rate after off-pump CABG similar to the on-pump CABG.
THE LIMITATIONS OF THE STUDY
This study has several limitations requiring caution in their interpretation:
1) There are no adjustments for specific risk attributed to clinical characteristics. It may have biased the choice of a particular patient to the surgical procedure;
2) The groups are not randomised, nor are the prospective analysis. This compromises the conclusion, to a certain extent;
3) The primary endpoints could not be outlined in advance, once the analysis is based only on the database.
CONCLUSIONortality rate similar to that of the on-pump CABG surgery, with a lower incidence of complications and perioperative infarction, and less need of the intra-aortic balloon pump. The technique is feasible, with similar results even in small service facilities. However, this study lacks statistical power, and it has some biases that hamper this statement from being consistent.
REFERENCES
1. Yusuf S, Zucker D, Peduzzi P, Fisher LD, Takaro T, Kennedy JW, et al. Effect of coronary artery bypass graft surgery on survival: overview of 10-year results from randomised trials by the Coronary Artery Bypass Graft Surgery Trialist Collaboration. Lancet. 1994;344(8922):563-70. [MedLine]
2. Kolessov VI. Mammary artery-coronary artery anastomosis as method of treatment for angina pectoris. J Thorac Cardiovasc Surg. 1967;54(4):535-44. [MedLine]
3. Favaloro RG. Saphenous vein autograft replacement of severe segmental coronary artery occlusion: operative technique. Ann Thorac Surg. 1968;5(4):334-9. [MedLine]
4. Buffolo E, Andrade JC, Branco JN, Aguiar LR, Ribeiro EE, Jatene AD. Myocardial revascularization without extracorporeal circulation. Seven-year experience in 593 cases. Eur J Cardiothorac Surg. 1990;4(9):504-7.
5. Benetti FJ, Naselli G, Wood M, Geffner L. Direct myocardial revascularization without extracorporeal circulation. Experience in 700 patients. Chest. 1991;100(2):312-6. [MedLine]
6. Al-Ruzzeh S, Nakamura K, Athanasiou T, Modine T, George S, Yacoub M, et al. Does off-pump coronary artery bypass (OPCAB) surgery improve the outcome in high-risk patients? A comparative study of 1398 high-risk patients. Eur J Cardiothorac Surg. 2003;23(1):50-5. [MedLine]
7. Aldea GS, Mokadam NA, Melford R Jr, Stewart D, Maynard C, Reisman M, et al. Changing volumes, risk profiles, and outcomes of coronary artery bypass grafting and percutaneous coronary interventions. Ann Thorac Surg. 2009;87(6):1828-38. [MedLine]
8. Nashef SA, Roques F, Michel P, Gauducheau E, Lemeshow S, Salamon R. European system for cardiac operative risk evaluation (EuroSCORE). Eur J Cardiothorac Surg. 1999;16(1):9-13. [MedLine]
9. Clarke RE. The STS Cardiac Surgery National Database: an update. Ann Thorac Surg. 1995;59(6):1376-80.
10. Tang AT, Knott J, Nanson J, Hsu J, Haw MP, Ohri SK. A prospective randomized study to evaluate the renoprotective action of beating heart coronary surgery in low risk patients. Eur J Cardiothorac Surg. 2002;22(1):118-23. [MedLine]
11. Patel NC, Graysson AD, Jackson M, Au J, Yonan N, Hasan R, et al; North West Quality Improvement Program in Cardiac Interventions. The effect off-pump coronary artery bypass surgery on in-hospital mortality and morbidity. Eur J Cardiothorac Surg. 2002;22(2):255-60. [MedLine]
12. Taggart DP, el-Fiky M, Carter R, Bowman A, Wheatley DJ. Respiratory dysfunction after uncomplicated cardiopulmonary bypass. Ann Thorac Surg. 1993;56(5):1123-8. [MedLine]
13. Diegeler A, Doll N, Rauch T, Haberer D, Walther T, Falk V, et al. Humoral immune response during coronary artery bypass grafting: a comparison of limited approach, "off-pump" technique, and conventional cardiopulmonary bypass. Circulation. 2000;102(19 Suppl 3):III95-100. [MedLine]
14. Shroyer AL, Grover FL, Hattler B, Collins JF, McDonald GO, Kozora E, et al; Veterans Affairs Randomized On/Off Bypass (ROOBY) Study Group. On-pump versus off-pump coronaryartery bypass surgery. N Engl J Med. 2009;361(19):1827-37. [MedLine]
15. Cartier R, Brann S, Dagenais F, Martineau R, Couturier AJ. Systematic off-pump coronary artery revascularization in multivessel disease: experience of three hundred cases. J Thorac Cardiovasc Surg. 2000;119(2):221-9. [MedLine]
16. Dewey TM, Magee MJ, Edgerton JR, Mathison M, Tennison D, Mack MJ. Off-pump bypass grafting is safe in patients with left main coronary disease. Ann Thorac Surg. 2001;72(3):788-91.
17. Arom KV, Flavin TF, Emery RW, Kshettry VR, Janey PA, Petersen RJ. Safety and efficacy of off-pump coronary artery bypass grafting. Ann Thorac Surg. 2000;69(3):704-10. [MedLine]
18. Wijeysundera DN, Beattie WS, Djaiani G, Rao V, Borger MA, Karkouti K, et al. Off-pump coronary artery surgery for reducing mortality and morbidity: meta-analysis of randomized and observational studies. J Am Coll Cardiol. 2005;46(5):872-82. [MedLine]
19. Silva AMRP, Campagnucci VP, Pereira WL, Rosa RF, Franken RA, Gandra SMA, et al. Revascularização do miocárdio sem circulação extracorpórea em idosos: análise da morbidade e mortalidade. Rev Bras Cir Cardiovasc. 2008;23(1):40-5. [MedLine] View article
20. Milani R, Brofman PRS, Souza JAM, Barboza L, Guimarães MR, Barbosa A, et al. Revascularização do miocárdio sem circulação extracorpórea em pacientes submetidos à hemodiálise. Rev Bras Cir Cardiovasc. 2007;22(1):104-10. View article
21. Sá MPBO, Lima LP, Rueda FG, Escobar RR, Cavalcanti PEF, Thé ECS, et al. Estudo comparativo entre cirurgia de revascularização miocárdica com e sem circulação extracorpórea em mulheres. Rev Bras Cir Cardiovasc. 2010;25(2):238-44. [MedLine] View article
22. Lima RC, Escobar M, Wanderley Neto J, Torres LD, Elias DO, Mendonça JT, et al. Revascularização do miocárdio sem circulação extracorpórea: resultados imediatos. Rev Bras Cir Cardiovasc. 1993;8(3):171-6. View article
23. Sá MP, Soares EF, Santos CA, Figueiredo OJ, Lima RO, Escobar RR, et al. Risk factors for mediastinitis after coronary artery bypass grafting surgery. Rev Bras Cir Cardiovasc. 2011;26(1):27-35. [MedLine] View article
24. Sá MP, Soares EF, Santos CA, Figueiredo OJ, Lima RO, Rueda FG, et al. Predictors of transfusion of packed red blood cells in coronary artery bypass grafting surgery. Rev Bras Cir Cardiovasc. 2011;26(4):552-8. [MedLine] View article
25. Demers P, Cartier R. Multivessel off-pump coronary artery bypass surgery in the elderly. Eur J Cardiothorac Surg. 2001;20(5):908-12. [MedLine]
26. Lima RC, Diniz R, Césio A, Vasconcelos F, Gesteira M, Menezes AM, et al. Revascularização miocárdica em pacientes octogenários: estudo retrospectivo e comparativo entre pacientes operados com e sem circulação extracorpórea. Rev Bras Cir Cardiovasc. 2005;20(1):8-13. View article
27. van der Heijden GJ, Nathoe HM, Jansen EW, Grobbee DE. Meta-analysis on the effect of off-pump coronary bypass surgery. Eur J Cardiothorac Surg. 2004;26(1):81-4. [MedLine]
Article receive on Monday, July 18, 2011
 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license