Solange GuiziliniI; Marcela ViceconteII; Gabriel Tavares da M. EsperançaII; Douglas W. BolzanIII; Milena VidottoI; Rita Simone L MoreiraIII; Andréia Azevedo CâncioIV; Walter J GomesIII
DOI: 10.5935/1678-9741.20140047
ABSTRACT
OBJECTIVE: To evaluate the lung function and clinical outcome in severe chronic obstructive pulmonary disease in patients undergoing off-pump coronary artery bypass grafting with left internal thoracic artery graft, comparing the pleural drain insertion in the intercostal versus subxyphoid region.
METHODS: A randomized controlled trial. Chronic obstructive pulmonary disease patients were randomized into two groups according pleural drain site: II group (n=27) - pleural drain in intercostal space; SI group (n=29) - pleural drain in the subxyphoid region. Spirometry values (Forced Vital Capacity - and Forced expiratory volume in 1 second) were obtained on preoperative and 1, 3 and 5 postoperative days. Chest x-ray from preoperative until postoperative day 5 (POD5) was performed for monitoring respiratory events, such as atelectasis and pleural effusion. Pulmonary shunt fraction and pain score was evaluate preoperatively and on postoperative day 1.
RESULTS: In both groups there was a significant decrease of the spirometry values (Forced Vital Capacity and Forced expiratory volume in 1 second) until POD5 (P<0.05). However, when compared, SI group presented less decrease in these parameters (P<0.05). Pulmonary shunt fraction was significantly lower in SI group (P<0.05). Respiratory events, pain score, orotracheal intubation time and postoperative length of hospital stay were lower in the SI group (P<0.05).
CONCLUSION: Subxyphoid pleural drainage in severe Chronic obstructive pulmonary disease patients determined better preservation and recovery of pulmonary capacity and volumes with lower pulmonary shunt fraction and better clinical outcomes on early postoperative off-pump coronary artery bypass grafting.
RESUMO
OBJETIVO: Avaliar a função pulmonar e os resultados clínicos em pacientes com doença pulmonar obstrutiva crônica grave submetidos à cirurgia de revascularização do miocárdio sem circulação extracorpórea, com enxerto da artéria torácica interna esquerda, comparando a inserção do dreno pleural intercostal versus subxifoide.
MÉTODOS: Estudo clínico, controlado e randomizado. Pacientes com doença pulmonar obstrutiva crônica foram randomizados em dois grupos de acordo com a posição do dreno pleural: grupo II (n=27) - dreno pleural intercostal; grupo IS (n=29) - dreno pleural na região subxifóide. Os valores espirométricos (Capacidade Vital Forçada e Volume expiratório forçado no 1 segundo) foram obtidos no pré-operatório, e no 1º, 3º e 5º dias de pós-operatório. Foi realizada radiografia de tórax no pré-operatório até o 5º dia pós-operatório (5PO) para monitoração de eventos respiratórios, como atelectasia e derrame pleural. A fração de shunt pulmonar e a escala de dor foram avaliadas no 1º dia pós-operatório.
RESULTADOS: Em ambos os grupos houve queda significativa dos valores espirométricos (Capacidade Vital Forçada e Volume expiratório forçado no 1 segundo) até o 5PO (P<0.05), porém, quando comparados, o grupo IS apresentou menor queda destes parâmetros (P<0.05). A fração de shunt pulmonar foi significativamente menor no grupo IS (P<0.05). Os eventos respiratórios, escala da dor, tempo de intubação orotraqueal e dias internação hospitalar no pós-operatório foram menores no grupo IS (P<0.05).
CONCLUSÃO: Drenagem pleural subxifoide em pacientes com doença pulmonar obstrutiva crônica grave determinou melhor preservação e recuperação dos volumes e capacidades pulmonares, com menor fração de shunt pulmonar e melhores resultados clínicos no pós-operatório precoce de cirurgia de revascularização do miocárdio sem circulação extracorpórea.
CABG: Coronary artery bypass graft
COPD: Chronic obstructive pulmonary disease
FEV1: Forced expiratory volume in 1 second
FVC: Forced Vital Capacity
ITA: Internal thoracic artery
OPCAB: Off-pump coronary artery bypass grafting
POD: Postoperative day
INTRODUCTION
Chronic obstructive pulmonary disease (COPD) has been associated with increased morbidity and mortality in patients undergoing coronary artery bypass graft (CABG)[1]. Many studies showed that as higher severity degree of COPD is associated to longer mechanical ventilation time and length of stay in the hospital and, consequently, increased hospital costs[2]. Furthermore, severe COPD patients undergoing CABG have a worse prognosis and increased mortality rate at long-term, when compared to patients without COPD[3,4].
Several factors may influence pulmonary function and clinical results in patients undergoing CABG, such as: general anesthesia, sternotomy, cardiopulmonary bypass, internal thoracic artery (ITA) graft with pleurotomy and pleural drain[5]. Pleural drain insertion through intercostal space promotes higher thoracic trauma, increased pain and discomfort for the patient, leading to increased vulnerability to lung complications. In patients without COPD undergoing off-pump CABG (OPCAB), the shift of pleural drain insertion to subxyphoid region reduces postoperative pulmonary dysfunction[6,7]. Our hypothesis is that reducing thoracic trauma in COPD patients underwent OPCAB could determine lower impairment to the lung function and better clinical results.
Therefore, the aim of this study was to evaluate the pulmonary function and clinical outcomes in severe COPD patients, comparing pleural drain insertion site in intercostal space versus subxyphoid region after OPCAB using left ITA (LITA).
METHODS
This prospective randomized study was performed between December 2007 and March 2012 at the Cardiovascular Surgery Discipline, Sao Paulo and Pirajussara Hospitals of the Federal University of Sao Paulo, Sao Paulo, Brazil. The Institutional Human Ethics Committee approved the protocol and written informed consent was obtained from all patients.
Patients study group
Patients of both sexes, age between 35 and 75 years old, coronary disease confirmed by coronary angiography, undergoing elective OPCAB using LITA, with an ejection fraction > 50%, and severe COPD were included in this study. We excluded patients unable to perform spirometry, with hemodynamic instability, intraoperative death, renal failure (creatinine >1.3 mg/dL), intact pleura, intraoperative complications requiring on-pump CABG conversion and patients who required additional analgesia.
The subjects were randomized into two groups by computerized system according to pleural drain position and the secrecy was maintained by sealed, numbered and opaque envelopes: II group (n=27), pleural drain was inserted in the sixth intercostals space; and SI group (n=29), pleural drain in the subxyphoid position.
Lung function assessment
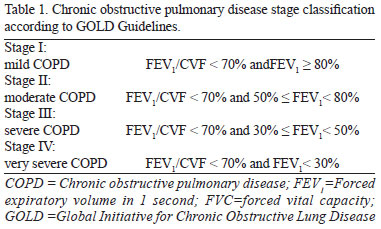
Spirometry records were obtained to evaluate the forced vital capacity (FVC) and the forced expiratory volume in 1 second (FEV1) on preoperative and postoperative days 1, 3, and 5 (POD1, POD3, POD5) by the same respiratory physiotherapist, using a portable espirometer (Spirobank G, MIR, Rome, Italy) according to the standards of the American Thoracic Society[8]. Chronic obstructive pulmonary disease was defined according to the criteria of the Global Initiative for Chronic Obstructive Lung Disease - GOLD, with presence of dyspnea (progressive and/or persistent), chronic cough or sputum production, and/or a history of exposure to risk factors for the disease (tobacco smoking, occupational dusts and chemical), and by spirometry with FEV1/FVC < 0.70. Furthermore, the severity of COPD was defined as described on Table 1[9].
Pulmonary shunt fraction was evaluated preoperatively and on POD1 using the software Oxygen Status Algorithm, (version 2.0; Mads & Ole Siggaard; Radiometer). This software needs the arterial blood gas and the fraction of inspired oxygen to calculate the percentage of blood that is not supplied by oxygen.
Anesthesia and ventilation management
All patients received a standard anesthetic technique, induction with etomidate and midazolam, maintenance with sufentanil and isofluorane (0.5% to 1%) and were mechanically ventilated to maintain normocapnia, with a 50% inspired oxygen fraction without positive end-expiratory pressure. Intraoperative fluids were given according to the anesthetist discretion.
Operative technique
The OPCAB surgery was performed through a median sternotomy, using LITA complemented with additional saphenous vein grafts. The LITA was harvested in a skeletonized fashion. A heated water mattress was used to keep all patients normothermic throughout the operation. OPCAB has followed the pattern at our service. Briefly, with systemic heparinization to achieve an activated clotting time exceeding 250 seconds, occlusion of the coronary artery was accomplished by using a proximal soft silicone snare. The distal anastomosis was accomplished with a 7-0 running polypropylene suture. The vein top ends were then attached to the ascending aorta using side-bite clamping. An Octopus 3 (Medtronic, Inc, Minneapolis, MN) suction stabilizer was used in all cases. Before chest closure, and in the presence of left pleura opening, the site of pleural drain insertion was randomized. A soft tubular straight PVC drain (¼ inch) was inserted and exteriorized at the intersection of the sixth left intercostal space (Group II) or a curved one at the subxyphoid region and positioned in the left costophrenic sinus (Group SI). In all patients, a straight mediastinal drain was also placed via a subxyphoid approach.
Postoperative Management
All patients were transferred to the intensive care unit (ICU) with orotracheal intubation, inspired oxygen fraction to keep arterial oxygen saturation above 90%, predicted tidal volume of 8 ml/kg, PEEP of 5 cmH2O and extubated according to ICU protocol. The drains (mediastinal and/or pleural) were routinely removed on POD2.
During postoperative days, the patients were evaluated by the same physiotherapist and all patients were undergone to the same physical therapy program until hospital discharge (breathing exercises and early deambulation).
Clinical Outcomes
All patients underwent to the same analgesic protocol administered during the postoperative period (100mg of tramadol chlorhydrate 4 times a day). Pain was evaluated and quantified by Visual Analogical Scale (VAS)[10] (0 = no pain to 10 = unbearable pain) on POD1 and before spirometry. Total orotracheal intubation time and length of hospital stay after surgery were also recorded.
The patients were undergoing chest radiography on preoperative, POD1, POD3 and POD5 for monitoring respiratory events, like pleural effusion and atelectasis. The radiological evaluation was performed by the same radiologist, blinded to the study. The pleural effusion was deemed significant when exceeding the costophrenic angle. Atelectasis was acknowledged when a clear atelectasis radiologic shadow exceeded 15 mm in width, with linear atelectasis being disregarded in this study.
Statistical analysis
Data were expressed as mean ± standard deviation. The FVC, FEV1 were analyzed, and values are expressed as a percentage of the preoperative value considered as 100% the preoperative baseline value. Intragroup variables comparing pre versus postoperative values were evaluated by paired Student t tests and analysis of variance for repeated measures with the Newman-Keuls posttest. Differences between groups were analyzed by unpaired Student t test or the Mann-Whitney test, when necessary. The categoric data were analyzed by the Pearson chi-square test. Statistical analysis was performed with GraphPad Prism 3.0 software (Graph-Pad Software Inc, San Diego, CA). A value of P<0.05 was considered statistically significant.
RESULTS
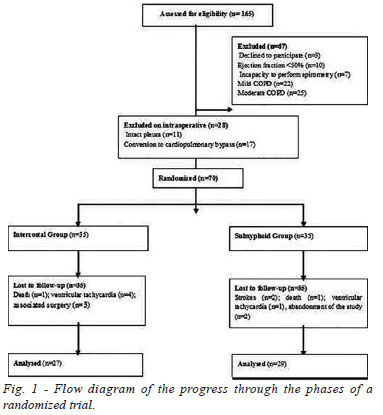
Initially, 165 subjects were selected for this study, however, 95 were excluded in the pre- and intraoperative, 14 were lost to follow-up and 56 were actually analyzed according to Figure 1. Groups were homogeneous preoperatively in terms of age, gender, body mass index (BMI), preoperative pulmonary function, operative time, number of grafts per patients with no significant statistically differences, as shown in Table 2.

No signs of preoperative myocardial infarction were detected in either group, as assessed by electrocardiographic changes or enzyme elevation.
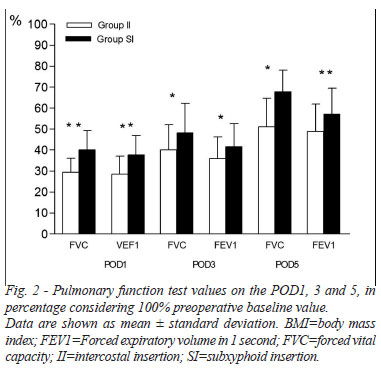
In the postoperative period, the both groups presented significant reduction in spirometric parameters (FVC and FEV1) until POD5 (P<0.05). However, when compared the values, the SI group presented lower impairment (Figure 2).
The pulmonary shunt fraction increase in both groups, but was significantly lesser in SI group (0.24±0.03% versus 0.28±0.04%; P<0.001).
In relation to respiratory events, lower incidence of atelectasis and pleural effusion was observed in SI group (atelectasis: 21±3.4% versus 25±0.1%; P=0.001 e pleural effusion: 22±2.4% versus 26±1.7%; P=0.003).
The chest pain sensation was lesser in group SI than II group (4.6±3.4 versus 7.9±2.1, P=0.001). Moreover, the time of mechanical ventilation and the length of hospital stay was lower in SI group when compared to II group (13.98±1.4 hours versus 16.25±2.1 hours; P=0.001; 9.51±1.6 days versus 12.1±1.4 days; P<0.001).
DISCUSSION
The results demonstrated that both groups presented impairment in pulmonary function in the early postoperative. However, the patients of SI group presented better pulmonary function and clinical outcomes when compared to II group. This data corroborate with findings by other studies with patients without COPD[5,11].
The lung dysfunction in postoperative period after CABG is associated with intraoperative procedures. The use of general anesthesia[12], the sternotomy[13], cardiopulmonary bypass[5], ITA graft with consequent pleurotomy and necessity of pleural drain insertion make the pulmonary dysfunction unavoidable[14].
The use of ITA graft for coronary revascularization is associated with higher survival and less incidence of cardiovascular events when compared to saphenous vein graft[15]. The technique of skeletonized ITA dissection has been proved beneficial to reduce sternal complications or infections, due to better preservation of arterial branches supplying sternal and intercostal muscles[16]. Beyond reduction of blood supply, the manipulation of ITA may lead the opening of parietal pleura[17]. Consequently to pleurotomy, pleural drainage becomes mandatory. In the majority of the operations, the chest tube is inserted and exteriorized in the intercostal space, coming into contact with the periosteum and the parietal pleura, which are highly sensitive. Therefore, the use of intercostal chest tube can promote ventilatory-dependent pain, limiting deep inspiration, which leads to the adoption of an antalgic posture, immobilization and reduced lung volumes and capacities[18].
Recent studies have evaluated the postoperative clinical follow-up of patients undergoing CABG, with exteriorization of the drain in the subxyphoid region, and concluded that this strategy minimizes the pulmonary dysfunction in postoperative period, with better spirometric parameters, lower rate of atelectasis and pleural effusion, and lower pain intensity[6,7,11]. Furthermore, Guizilini et al.[19] observed that the insertion of a chest tube in the subxyphoid region resulted in similar findings to CABG with intact pleura.
COPD can also be considered a risk factor for development of pulmonary dysfunction in postoperative period of CABG. Fuster et al.[2] and Lizak et al.[20] compared postoperative outcomes of patients with and without COPD and observed that patients with COPD had a higher incidence of pulmonary complications and hospital stay, more pronounced in patients with severe COPD.
Taking into account evidence that shifting the site of drain insertion to the subxyphoid region may be beneficial for the postoperative clinical outcomes, and the fact that patients with severe COPD have a higher risk of pulmonary complications in this period, this study aimed to answer the following question: Do patients with clinically severe COPD would benefit by shifting the drain position in the postoperative period of OPCAB using the LITA graft? For our knowledge, no randomized controlled trial has evaluated the impact of drain shifting in severe COPD patients undergoing OPCAB, which makes our proposal innovative and original.
Previous studies compared the effectiveness of shifting the drain insertion site to the subxyphoid region and reported lesser lung function impairment[6,11,19]. These findings corroborate the results found in this study, reiterating the hypothesis that subxyphoid drain minimizes the dysfunction in postoperative period of OPCAB surgery, even in patients with severe COPD.
Regarding the chest pain, patients with subxyphoid drain reported less intensity on VAS. The same result was reported in other studies with patients without COPD, which showed less pain when the chest tube was inserted in the subxyphoid region[6,11,21]. Similar outcomes were found in this study.
Sensoz et al.[11] evaluated patients with COPD undergoing on-pump CABG by means of computed tomography. Patients who belonged to the group with pleural drain in subxyphoid region evolved with a lower incidence of atelectasis in postoperative period, corroborating the results found in this study.
Hypoxemia is also an unavoidable consequence in CABG postoperative, regardless of surgical technique[5,6]. There are many causes of hypoxemia, abnormal diffusion, hypoventilation and shunt. In this study, the pulmonary shunt fraction was assessed on the first postoperative day, which was significantly lower in the subxyphoid group.
These findings could be explained due to better preservation and recovery of FVC and consequently decrease of pulmonary fraction shunt, reflects the chest wall lesser degree of trauma in patients with pleural subxyphoid drain.
Fuster et al.[2] associated severe COPD with higher incidence of pneumonia, sepsis and respiratory distress syndrome, longer ICU stay, and greater number of hospitalization days in the postoperative period of coronary revascularization. Saleh et al.[1] found that COPD severity is a significant prognostic marker in clinical outcomes after CABG. In this study, we found similar results; however the SI group presented shorter mechanical ventilation time and length of hospital stay, which may be reflected in reduced hospital costs, although this finding was not evaluated.
This study has some limitations. The assessment of patients after surgery was not blind because of the possibility to visualize the drain position in the rib cage, with exception of radiological analyses; however the spirometry was performed according to ATS standardization to confirm the airflow limitation, by the same evaluator, reducing the evaluation bias. Furthermore, the sample size was limited by the tight inclusion criteria restricted to severe COPD.
Considering the results of this study and others, it is clear that CABG elicits postoperatively pulmonary dysfunction and may exacerbate in the existence of comorbidities such as COPD. Drain shifting to the subxyphoid region is recommended for further decreasing trauma to the chest and can be an alternative to minimize the postoperative pulmonary dysfunction in this group of patients.
CONCLUSION
Subxyphoid pleural drainage in severe COPD patients determined better preservation and recovery of pulmonary capacity and volumes with lower pulmonary shunt fraction and better clinical outcomes on early postoperative OPCAB.
REFERENCES
1. Saleh HZ, Mohan K, Shaw M, Al-Rawi O, Elsayed H, Walshaw M, et al. Impact of chronic obstructive pulmonary disease severity on surgical outcomes in patients undergoing non-emergent coronary artery bypass grafting. Eur J Cardiothorac Surg. 2012;42(1):108-13.
2. Fuster RG, Argudo JAM, Albarova OG, Sos FH, López SC, Codoñer MB, et al. Prognostic value of chronic obstructive pulmonary disease in coronary artery bypass grafting. Eur J Cardiothorac Surg. 2006;29(2):202-9. [MedLine]
3. Nishiyama K, Morimoto T, Furukawa Y, Nakagawa Y, Ehara N, Taniguchi R, et al. Chronic obstructive pulmonary disease-an independent risk factor for long-term cardiac and cardiovascular mortality in patients with ischemic heart disease. Int J Cardiol. 2010;143(2):178-83. [MedLine]
4. Leavitt BJ, Ross CS, Spence B, Surgenor SD, Olmstead EM, Clough RA, et al.; Northern New England Cardiovascular Disease Study Group. Long-term survival of patients with chronic obstructive pulmonary disease undergoing coronary artery bypass surgery. Circulation. 2006;114(1 Suppl):I430-4 [MedLine]
5. Guizilini S, Gomes WJ, Faresin SM, Bolzan DW, Alves FA, Catani R, et al. Evaluation of pulmonary function in patients following on- and off-pump coronary artery bypass grafting. Rev Bras Cir Cardiovasc 2005;20(3):310-6. View article
6. Guizilini S, Gomes WJ, Faresin SM, Carvalho ACC, Jaramillo JI, Alves FA, et al. Effects of the pleural drain site on the pulmonary function after coronary artery bypass grafting. Rev Bras Cir Cardiovasc. 2004;19(1):47-54. View article
7. Cancio AS, Guizilini S, Bolzan DW, Dauar RB, Succi JE, de Paola AA, et al. Subxyphoid pleural drain confers lesser impairment in respiratory muscle strength, oxygenation and lower chest pain after off-pump coronary artery bypass grafting: a randomized controlled trial. Rev Bras Cir Cardiovasc. 2012;27(1):103-9. [MedLine] View article
8. American Thoracic Society. Standardization of spirometry. 1994 Update. Am J Respir Crit Care Med.1995;152(3):1107-36. [MedLine]
9. Vestbo J, Hurd SS, Agustí AG, Jones PW, Vogelmeier C, Anzueto A, et al. Global strategy for the diagnosis, management, and prevention of chronic obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care Med. 2013;187(4):347-65. [MedLine]
10. Symreng T, Gomez MN, Rossi N. Intrapleural bupivacaine v saline after thoracotomy--effects on pain and lung function--a double-blind study. J Cardiothorac Anesth. 1989;3(2):144-9. [MedLine]
11. Sensoz Y, Gunay R, Tuygun AK, Balci AY, Sahin S, Kayacioglu I, et al. Computed tomography evaluation of different chest tube sites for residual pleural volumes after coronary artery bypass surgery. Ann Saudi Med. 2011;31(4):383-6. [MedLine]
12. Hedenstierna G, Edmark L. The effects of anesthesia and muscle paralysis on the respiratory system. Intensive Care Med. 2005;31(10):1327-35. [MedLine]
13. Guizilini S, Bolzan DW, Faresin SM, Alves FA, Gomes WJ. Ministernotomy in myocardial revascularization preserves postoperative pulmonary function. Arq Bras Cardiol. 2010;95(5):587-93. [MedLine]
14. Wynne R, Botti M. Postoperative pulmonary dysfunction in adults after cardiac surgery with cardiopulmonary bypass: clinical significance and implications for practice. Am J Crit Care. 2004;13(5):384-93 [MedLine]
15. Rolla G, Fogliati P, Bucca C, Brussino L, Di Rosa E, Di Summa M, et al. Effect of pleurotomy on pulmonary function after coronary artery bypass grafting with internal mammary artery. Respir Med. 1994;88(6):417-20. [MedLine]
16. Berdajs D, Zünd G, Turina MI, Genoni M. Blood supply of the sternum and its importance in internal thoracic artery harvesting. Ann Thorac Surg. 2006;81(6):2155-9. [MedLine]
17. Guizilini S, Gomes WJ, Faresin SM, Bolzan DW, Buffolo E, Carvalho AC, et al. Influence of pleurotomy on pulmonary function after off-pump coronary artery bypass grafting. Ann Thorac Surg. 2007;84(3):817-22. [MedLine]
18. Jakob H, Kamler M, Hagl S. Doubly angled pleural drain circumventing the transcostal route relieves pain after cardiac surgery. Thorac Cardiovasc Surg. 1997;45(5):263-4. [MedLine]
19. Guizilini S, Bolzan DW, Faresin SM, Ferraz RF, Tavolaro K, Cancio AA, et al. Pleurotomy with subxyphoid pleural drain affords similar effects to pleural integrity in pulmonary function after off-pump coronary artery bypass graft. J Cardiothorac Surg. 2012;7:11. [MedLine]
20. Lizak MK, Nash E, Zakliczynski M, Sliwka J, Knapik P, Zembala M. Additional spirometry criteria predict postoperative complications after coronary artery bypass grafting (CABG) independently of concomitant chronic obstructive pulmonary disease: when is off-pump CABG more beneficial? Pol Arch Med Wewn. 2009;119(9):550-7. [MedLine]
21. Hagl C, Harringer W, Gohrbandt B, Haverich A. Site of pleural drain insertion and early postoperative pulmonary function following coronary artery bypass grafting with internal mammary artery. Chest. 1999;115(3):757-61. [MedLine]
No financial support.
Authors' roles & responsibilities
SG: Data collection and manuscript preparation
MV: Data collection and manuscript preparation
GTME: Data collection
DWB: Data collection
MV: Statistical analysis and data collection
RSLM: Manuscript preparation
AAC: Data collection
WJG: Review of the manuscript
Article receive on Thursday, October 24, 2013
 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license