Alexandre Visconti BrickI; Domingo Marcolino BraileII
DOI: 10.5935/1678-9741.20150078
AF = Atrial fibrillation
ISMICS = International Society of Minimally Invasive Cardiothoracic Surgery
LILACS = Latin American and Caribbean Health Sciences
Medline = Medical Literature Analysis and Retrieval System Online
SciELO = Scientific Electronic Library Online
SICTRA = Saline-Irrigated Cooled-tip Radiofrequency Ablation
INTRODUCTION
Atrial fibrillation (AF) is the most common and complex supraventricular arrhythmia with loss of atrial contraction, occurring in about 0.4% of the population and with 10% of the patients being over 60 years old. It is frequently associated with mitral valve disease and it is a constant cause of thromboembolic events, especially cerebrovascular[1].
There are several studies demonstrating that pharmacological means of controlling the rhythm does not reduce morbidity and mortality rate nor does it protect against thromboembolism. The AF that does not respond to medicines has several consequences such as maintaining the irregular rhythm (palpitations and discomfort), loss of atrioventricular synchrony, heart failure, and atrial thrombosis with thromboembolic episodes, being the cause of stroke and pulmonary embolism in 33% of the cases[2-4]. Catheter ablation has an outstanding position in the treatment of AF, but surgery is an effective therapeutic method for treating chronic AF in patients who require heart surgery for other reasons.
The most accepted theory to explain the electrophysiological mechanism for maintenance of AF is multiple waves, described by Moe[5] and confirmed by the studies of Alessie et al.[6] and Cox et al.[7]. Subsequently, it was shown that AF is initiated by automatic foci with high triggering frequency[8,9]. The endocardial mapping revealed that these foci are located in the pulmonary veins and the creation of multi-shaped lesions with radiofrequency energy where foci originate interrupts AF[10]. While the cardiac electrical stimulation does not propagate where there is lesion with scarring, requiring normal myocardium to progress, the injury caused by ablation with energy sources interrupts the reentry circuit[8-10].
The International Consensus on Catheter Ablation for Atrial Fibrillation Surgery defined the following indications for surgical ablation of AF[11]: 1) symptomatic patients undergoing surgical procedures; 2) selected asymptomatic patients undergoing another surgical procedure in which ablation can be performed with minimal risk; and 3) surgery for primary AF, to be considered for symptomatic patients who opt for surgery in which one or more attempts of catheter ablation have failed or who are not candidates for catheter ablation.
In addition, the Brazilian Guidelines for Treatment of AF indicate the following[12]: Class I: patients with symptomatic AF undergoing mitral valve surgery; Class II B: surgery for treatment of AF in patients with symptomatic AF in which catheter ablation cannot be performed or has failed.
The first non-pharmacological treatment of AF includes: 1) electrical cardioversion with a high recurrence rate[13]; 2) techniques using intraoperative cryoablation of the bundle of His and the atrioventricular junction[14]; 3) isolation of the left atrium[15]; 4) catheter ablation of the atrioventricular junction and permanent pacemaker implantation[9]; 5) catheter ablation of the bundle of His and definitive pacemaker implant; and 6) "Corridor Operation[16]".
Although they regularize heart rate, these procedures maintain the atria, or part of them, fibrillating, thereby not eliminating the risk of complications such as hemodynamic compromise and the occurrence of thromboembolic events.
Based on the electrophysiological mechanisms of AF analyzed in experimental studies, the "Cox operation" has been described, which consists of making incisions and sutures on the atrial wall, enabling the spread of electrical stimulation in the atria within a labyrinth, ordering atrial contraction[17]. Changes have been performed to the "Cox Operation", making it simpler and also propitiating the return of sinusal rhythm[18]. Studies reporting the success of this technique were published, and it is considered the reference standard for the surgical treatment of AF[19,20], mainly in patients with mitral valve disease[21].
The wide dissection of cardiac structures and the extensive lines of section and suturing of the atrial wall, however, significantly increased operative time as well as cardiopulmonary bypass and aortic clamping time, resulting in higher postoperative morbidity and making the widespread application of the procedure difficult.
In order to increase the applicability and reduce the complexity of the "Cox operation", several technical modifications were introduced, such as the change in the location of the atrial incisions[22]; the reduction of section lines and suturing of the atrial wall, known as "Mini Cox[23]"; and the unilateral procedure, performed only in the left atrium, called "Cox at Left"[24].
The use of catheter ablation for the treatment of supraventricular arrhythmias stimulated the use of energy sources (cryoablation, radiofrequency, microwave, ultrasound, and laser) to cause linear ablative lesions for endocardial and epicardial applications or to replace the cutting and suturing of the atrial wall[25-28], especially when associated with valvular disease.
The Maze I procedure developed by Cox employed section, suture, and cryoablation[19]. Changes in techniques, including the dismissal of cryoablation, have been introduced, such as described by Jazbik et al.[29], Gregori Jr. et al.[30], and Batista et al.[31].
Kalil et al.[32] performing a simplified surgical technique with a single incision around all four pulmonary vein ostia in patients with mitral valve disease, found that this technique was effective in treating AF secondary to mitral valve disease.
Several authors have developed and improved techniques to eliminate chronic AF and return to sinus rhythm in patients undergoing cardiac surgery, especially in patients with mitral valve disease, using various sources of energy capable of causing permanent blocking lines such as microwaves[33], ultrasound[34], cryoablation[23], radiofrequency[35], and laser[27].
Currently, the most widely used energy source is radiofrequency, an alternating current released in the form of an unmodulated, continuous sine wave capable of promoting ablation of the entire tissue. The wave can be either unipolar or bipolar, irrigated or not. The driving of the energy can be measured, demonstrating the transmural lesion, an important factor to eliminate arrhythmia[36]. After the use of radiofrequency as the form of energy most commonly applied in catheter ablation, results of experimental studies have been published[37,38] with new sources of energy being used in surgical ablation. Radiofrequency ablation for treatment of AF was described by Hindricks et al.[35].
Regarding cryoablation, there are two energy sources available: nitrogen oxides and argon, the difference being the ability to freeze the tissue. The size and depth of the lesion will depend on factors such as temperature of the ablation catheter, tissue temperature, size of the catheter, duration and number of ablation lines, and the type of source[20]. The disadvantage lies in the length of application and its limited use in minimally invasive techniques.
In an experimental study, Manasse et al.[39] used radiofrequency and cryoablation for endocardial and epicardial routes and/or video-assisted thoracoscopy, demonstrating the importance of the pulmonary veins and the presence of transmural lesions created quickly.
Microwave energy uses an electromagnetic field generated by oscillation of the tissue molecules, producing heat with uniform penetration and without burning the surrounding tissues[28]. There is also a limitation on its use in minimally invasive surgery, and complications and concerns about possible esophageal perforation.
The laser, despite being a promising form of energy, has been tested only in experimental studies[27].
The effects of ultrasound to treat AF are produced by tissue damage derived from hyperthermia in tissue necrosis, resulting in a transmural lesion that can be used in both endocardial and epicardial applications, in a minimally invasive manner. Considering the experience with the ultrasound scalpel (UltraCision®), often used in videolaparoscopic procedures[40] for treating refractory ventricular tachycardia, Brick et al.[26,41] devised a new approach to form lines of lesions, which would determine the partitioning of the left and right atria under shorter surgical and cardiopulmonary bypass time, reflecting positively in postoperative complications.
The aim of this study is to present a literature review on surgical ablation of AF in patients undergoing cardiac surgery considering energy sources and return to sinus rhythm.
METHODS
This study was based on a review of the literature on chronic AF surgery using energy sources, available in the following databases: Latin American and Caribbean Health Sciences (LILACS), Medical Literature Analysis and Retrieval System Online (Medline), and Scientific Electronic Library Online (SciELO), in Portuguese and English, in the last 20 years. The keywords used included: atrial fibrillation, ablation techniques, energy sources, and results of surgical treatment.
The analysis of the studies was performed descriptively in order to present current knowledge about surgical ablation of AF in patients undergoing cardiac surgery[42].
Experimental, randomized and non-randomized studies were analyzed on the development of surgical ablation of AF with energy sources associated with cardiac surgery.
Catheter ablation studies and surgical treatment of AF alone were excluded.
RESULTS
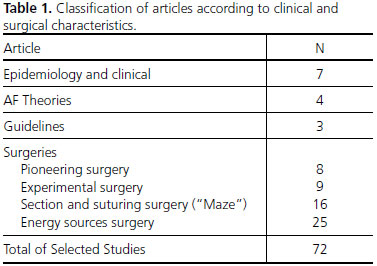
In this literature review, we identified 72 studies on evolution and improvement of surgery of arrhythmias, divided into: epidemiology and clinics (n=7), AF theories (n=4), guidelines (n=3), experimental surgery (n=9), pioneering surgery (n=8), section and suturing surgery ("Maze") (n=16), and energy sources surgery (n=25) (Table 1).
Nineteen articles were identified from the first surgery to eliminate fibrillation, known as the Maze procedure pioneered by Cox, until the early use of energy sources for ablation of arrhythmia.
Regarding the use of energy sources, Table 2 presents 25 articles focusing on sample size, type of study, results (early and late), and completion (percentage of return to sinus rhythm). Of those, six are randomized trials (484 patients), 17 are non-randomized (1,551 patients), and two are meta-analyzes (74 studies). A total of 19 studies were prospective; 4, retrospective.
Analyzing studies with immediate results (n=5), the percentage of return to sinus rhythm ranged from 73% to 96%, whereas in the long-term results (n=20) (from 12 months) the range was from 62% to 97.7%. In both, there was subsequent clinical improvement of patients who underwent ablation, regardless of the energy source used.
DISCUSSION
With research on the origin of AF and with the experience of electrophysiologists and surgeons, new approaches have emerged from the classic Maze surgery (Cox-Maze)[7,17,18], making the extensive manipulation of the atria inconvenient, with peri- and postoperative repercussions. Consequently, there has been a demand for less invasive procedures, such as manipulation only in the pulmonary veins and intraoperative ablation of atrial walls with alternative energy sources (cryoablation, microwave, radiofrequency, laser, and ultrasound), and thoracoscopy procedures using radiofrequency and ultrasound catheters from the epicardium in on-pump surgeries.
Atrial ablation can be performed using the traditional cut and suture technique as well as the simplified technique for pulmonary vein isolation, as demonstrated by Albrecht et al.[43] in a controlled, prospective randomized study.
In a prospective randomized study of patients with rheumatic mitral valve disease with chronic AF, Vasconcelos et al.[44] studied 29 patients (n=13, control group; n=14, treated group) for 11.5 months. The authors concluded that surgical isolation of the posterior wall of the left atrium involving the pulmonary vein ostia is an effective way of treating rheumatic mitral valvular disease in chronic AF.
Gomes et al.[45], using electrocautery in mitral valve surgery, found that this source of energy reversed arrhythmia in a significant number of patients. In the absence of ultrasound equipment, Brick (personal communication) had the opportunity to use electrocautery in a small number of patients, not recommending its routine use due to charring with the release of small emboli inside the atrium.
In the following paragraphs, the energy sources are reviewed with data from the literature.
In regard to cryoablation, Gallagher et al.[46] described its initial use in the treatment of accessory bundles as a method for correcting pre-excitation syndrome. Fukada et al.[47] investigated the indication of "Cox operation" in patients with mitral valve disease and AF using cryoablation to replace some of the atrial incisions. They observed that the ideal cases were patients with disease of non-rheumatic origin, especially those undergoing valve repair.
Lee et al.[48] used cryoablation to replace the section and suture lines, dividing the patients into two groups: in the first one, the lines described in the "Cox operation" were used; in the second, the left and right pulmonary veins were isolated separately. Thus, they studied the improvement of atrial contraction in 83 patients undergoing surgical treatment of AF and other heart diseases. During early evolution and the six-month follow-up, it was demonstrated that the restoration of sinus rhythm and recovery of atrial contraction were significantly more evident in the second group. Later, Lee et al.[49] compared 86 patients with mitral valve disease of rheumatic origin to 43 patients with mitral disease of degenerative etiology and found similar results in both groups after six months, with conversion to sinus rhythm in 95.3% and 97.7% and recovery of atrial contraction in 90.4% and 91.9%, respectively.
Cox et al.[50] described a minimally invasive technique for performing the "Cox operation III", with access through right inframammary thoracotomy of about 7 cm, cannulation of artery, right femoral vein and superior vena cava for installation of cardiopulmonary bypass system and endocardial application of cryoablation to replace the section and suture lines.
In 2007, Blomström-Lundqvist et al.[51] stated the benefit of cryoablation in reversion and maintenance of sinus rhythm in patients undergoing mitral valve surgery. In a prospective multicenter randomized study, they analyzed 69 patients who underwent mitral valve surgery with or without cryoablation in order to assess the efficacy of cryoablation applied to the epicardium of the left atrium in patients undergoing this type of surgery. During follow-up, heart rate was measured at 6 and 12 months, sinus rhythm was regained in 73.3% of the patients who underwent ablation (in both periods) and in 45.7% (6 months) and 42.9% (12 months) of patients who underwent mitral valve surgery alone. There was a significant difference between the groups in the two follow-up periods.
Johansson et al.[52] used epicardial cryoablation in a randomized study with 65 patients undergoing mitral valve surgery, concluding that the ablation group had better results.
This source of energy, originally used by Cox et al.[50], represents an effective and safe therapeutic option. However, the main drawback in minimally invasive surgery (off-pump) is that freezing the blood produces coagulation, resulting in the risk of thromboembolism[51].
Another source of energy, radiofrequency was the first alternative energy source applied in the surgical treatment of AF and it has been widely used. In point-by-point radiofrequency ablation, the irrigated unipolar device produces linear tissue lesions. A bipolar catheter is able to promote ablation of all tissue involved by the electrodes quickly (usually less than 10 seconds). Breda et al.[53] reported the initial assessment of surgical biatrial ablation by radiofrequency. Energy output can be measured during ablation and this can be correlated with proven transmural lesions[54].
In 2008, Beukema et al.[55] published the results of medium- and long-term follow-up after radiofrequency ablation associated with other cardiac surgeries and demonstrated maintenance of sinus rhythm in 69% of the cases treated in the 1-year follow-up, 56% in 3 years, 52% in five years, and 57% in later periods. Treatment with antiarrhythmic drugs was maintained in 64% of the patients who were free of AF; only 1% was under oral anticoagulation regimen.
Williams et al.[56] described the experience of three centers with the use of flexible catheter for applying radiofrequency in pulmonary vein isolation using the endocardial application, similar to the "Cox operation", or separately in the right and left sides, with lesions communicating between the two blocs. The procedure was performed in 48 patients undergoing other associated procedures and, in eight cases, lesions were performed in the right atrium. Results showed survival rates of 87.5% and restoration of sinus rhythm in 81% of the cases at an average follow-up of four months.
Kottkamp et al.[57], through access with anterolateral right mini-thoracotomy and video-assisted cardiopulmonary bypass, performed continuous linear lesions with endocardial application of radiofrequency in the left atrium, involving the mitral annulus and the pulmonary veins after anatomical definition of reentrant circuits with electrophysiological mapping. The procedure was performed in 70 patients with persistent or paroxysmal AF. After six months, 93% of patients were in sinus rhythm; after 12 months, 95% of patients had persistent AF and 97% of patients with paroxysmal AF were in sinus rhythm. Complications from the procedure are a case of esophageal perforation and a case of development of circumflex coronary artery stenosis.
Benussi et al.[58] described the epicardial application of radiofrequency with multipolar catheter for performing lesions in 40 patients with mitral valve disease. The procedure was performed around the right and left pulmonary veins, connecting them to the left atrial appendage. After the left atriotomy, endocardial application joined the lesions of the pulmonary veins with the mitral valve, with the exclusion, in the end, of the left atrial appendage. In the mean follow-up of 11.6 months, 76.9% of the patients had reverted to sinus rhythm, with a significant reduction in the diameter of the left atrium and recovery of right and left atrial contraction. In the medium-term, the results of the experience with radiofrequency ablation for AF in 132 patients were presented, being performed through epicardial application in 107 patients. The lesions in the left atrium were performed prior to cardiopulmonary bypass and used for correction of associated heart diseases. Operative mortality was 0.8%. After three years of development, 77% of the patients were free of AF and 98% were free of stroke, with a survival rate of 94%.
In 2011, Canale et al.[59,60] performed retrospective studies demonstrating that the use of bipolar radiofrequency led to the reversal of arrhythmia in 68% of the patients after 14 months in one of the studies and in 73% of the patients in the period of 7 months according to the other one. The author's experience with the use of bipolar radiofrequency was more efficient than with unipolar. In 2014, Huang et al.[61], after comparing the use of monopolar and bipolar radiofrequency, concluded that both are effective for the treatment of chronic AF, however, ablation with bipolar radiofrequency is more convenient.
Dong et al.[62], in 2013, analyzed concomitant valve replacement and radiofrequency ablation in 191 patients with rheumatic disease; 158 patients were followed-up for a year and sinus rhythm was maintained in 79.11%.
In 2014, Phan et al.[63], after performing cumulative metaanalysis of randomized clinical trials of surgeries with and without AF ablation in six databases, identified sixteen randomized trials and concluded that surgical ablation concomitant with cardiac surgery was effective and safe to restore sinus rhythm, after 12 months of follow-up.
Colafranceschi et al.[64] performed video-assisted thoracoscopic surgery in 2009, concluding that it is safe and reproducible, especially in patients with paroxysmal fibrillation refractory to drug therapy who did not require concomitant surgery. This technique opens new paths for patients who have not responded adequately to catheter treatment.
In Brazil, Brick et al.[26] started to experience with a unipolar radiofrequency catheter while performing point-by-point ablation of the left atrium. The development of bipolar ablation devices with irrigated catheter contributed to the technical improvement of the procedure, leading to shorter operative time and postoperative results showing a satisfactory success rate of 96% of sinus rhythm reversal[53].
Abreu Filho et al.[65] evaluated 70 patients with permanent AF and rheumatic mitral valve disease. These patients were randomly assigned to undergo either a modified Maze III procedure using Saline-Irrigated Cooled-tip Radiofrequency Ablation (SICTRA) associated with mitral valve surgery (group A) or mitral valve surgery alone (group B). The cumulative rates of sinus rhythm were 79.4% in group A and 26.9% in group B (P=0.001). They concluded that SICTRA is effective for treating permanent AF associated with rheumatic mitral valve disease.
Using microwave as an energy source, Gillinov et al.[28] described their experience with ablation in 10 patients undergoing surgery for mitral valve and pulmonary vein isolation for epicardial application. After opening the left atrium, the lesions were observed from the endocardial surface, proving to be transmural.
In 2012, MacDonald et al.[66] concluded that microwave energy concomitant with surgery was not as effective when compared to radiofrequency ablation in long-term outcome assessment.
Lin et al.[67], in 2011, compared the use of microwave in 94 patients to the use of bipolar radiofrequency in 93 patients undergoing valve surgery, for three months, concluding that radiofrequency ablation is superior to ablation with microwave.
The use of ultrasound in the treatment of AF promotes tissue damage by hyperthermia. This technology is attracting interest because it allows for ablation in a less invasive manner, without damaging adjacent structures. Brick et al.[68] began their experience with ultrasound using the unipolar endocardial catheter ablation and three patients underwent surgery with reversion to sinus rhythm.
Execution of intraoperative ablation using this technique, in addition to facilitating and reducing the operative time, allowed for greater understanding of the role of the left atrium and pulmonary veins in chronic fibrillation[26,37].
Additional procedures were performed, such as exclusion of the right and left atrial appendages; reduction of the left atrium, where necessary; and ablation of the right atrium to eliminate the possibility of atrial flutter.
Ninet et al.[69], in a multicenter study, prospectively analyzed 103 patients between September 2002 and February 2004, using ultrasound for epicardial ablation of AF. Ablation was performed through epicardial application using a high-frequency ultrasound, EpiCor® (St Jude Medical Inc). Analysis showed that, after six months, 85% of patients were in sinus rhythm. They demonstrated the advantage of using the energy of ultrasound, creating a transmural lesion around the left atrium without the use of cardiopulmonary bypass.
Lins et al.[70] showed an improvement in functional class in the treated group versus the control group in a comparative study of patients with mitral valve disease, using ultrasound scalpel (UltraCision®). The groups presented homogeneous preoperative characteristics and no significant difference considering cardiopulmonary bypass times, anoxia and postoperative intensive care unit stay, which leads to the conclusion that the use of ultrasonic scalpel for AF ablation does not act to worsen patient outcomes. Comparing patients who underwent ultrasound ablation with those who received no recent ultrasound ablation, no more complications or deaths in recent or late postoperative were found. The results observed in this study show that the ultrasound ablation technique can be applied to patients who have surgical indication for mitral valve disease correction.
In addition to the endocardial application, ultrasound with other devices such as the EpiCor® can be used in off-pump surgery, through epicardial application in patients with isolated fibrillation, as well as in patients with ischemic heart disease undergoing coronary artery bypass graft surgery[71].
The objective of the 2009 Consensus Conference of the International Society of Minimally Invasive Cardiothoracic Surgery (ISMICS)[72] was to determine whether surgical ablation of AF during associated cardiac procedures improved postoperative clinical outcomes. The group involved in the study analyzed the best available evidence, with systematic data review, including randomized and non-randomized controlled studies, always in descending order of importance. A systematic review and meta-analysis identified 10 randomized trials (650 patients) and 23 non-randomized (3997 patients); the great majority was published in English and performed in the United States.
The authors of the consensus defined the following recommendation: in patients with persistent and permanent AF, surgical ablation is recommended to increase the incidence of sinus rhythm in the short- and long-term (Class 1, Level A); reduce the risk of stroke and thromboembolic events (Class 2a, level A); increase exercise tolerance and improve ventricular function (Class 2a, level A); and increase survival (Class 2a, level B)[72].
CONCLUSION
Evolving from the classical labyrinth surgery (Cox-Maze), changes in demand for less invasive procedures have occurred with the use of alternative sources of energy.
The results of the surgical ablation of AF in patients undergoing cardiac surgery depend on the energy source used; the lesion produced is transmural and applied in both atria.
We conclude that surgical ablation of AF is essential in the treatment of this arrhythmia. With current technology, it may be minimally invasive, making it mandatory to perform a procedure in an attempt to revert to sinus rhythm in patients requiring heart surgery.
Situations involving primary fibrillation surgery indication should include a multidisciplinary team approach involving cardiologists, electrophysiologists and surgeons to make the correct choice of patients and the most appropriate procedure.
REFERENCES
1. Go AS, Hylek EM, Phillips KA, Chag Y, Henault LE, Selby JV, et al. Prevalence of diagnosed atrial fibrillation in adults: national implications for rhythm management and stroke prevention: the Anticoagulation and Risk Factors In Atrial Fibrillation (ATRIA) Study. JAMA. 2001;285(18):2370-5. [MedLine]
2. Kannel WB, Abbott RD, Savage DD, McNamara PM. Epidemiological features of chronic atrial fibrillation: the Framingham study. N Engl J Med. 1982;306(17):1018-22. [MedLine]
3. Wolf PA, Abbott RD, Kannel WB. Atrial fibrillation: a major contributor to stroke in the elderly: the Framinghan study. Arch Intern Med. 1987;147(9):1561-4. [MedLine]
4. Hart RG, Halperin JL, Pearce LA, Anderson DC, Kronmal RA, McBride R, et al.; Stroke Prevention in Atrial Fibrillation Investigators. Lessons from the Stroke Prevention in Atrial Fibrillation trials. Ann Intern Med. 2003;138(10):831-8. [MedLine]
5. Moe FK. On the multiple wavelet hypothesis of atrial fibrillation. Arch Int Pharmacodyn Ther. 1962;140:183-8.
6. Allessie MA, Bonke FI, Schopman FJ. Circus movement in rabbit atrial muscle as a mechanism of tachycardia. III. The "Leading Circle"concept: a new model of circus movement in cardiac tissue without the involvement of an anatomical obstacle. Circ Res. 1977;41(1):9-18. [MedLine]
7. Cox JL, Schuessler RB, Boineau JP. The surgical treatment of atrial fibrillation: I.Summary of the current concepts of the mechanisms of atrial flutter and atrial fibrillation. J Thorac Cardiovasc Surg. 1991;101(3):402-5. [MedLine]
8. Haïssaguerre M, Jaïs P, Shah DC, Takahashi A, Hocini M, Quiniou G, et al. Spontaneous initiation of atrial fibrillation by ectopic beats originating in the pulmonary veins. N Engl J Med. 1998;339(10):659-66. [MedLine]
9. Scheinman M, Morady F, Hess DS, Gonzalez R. Catheter-induced ablation of the atrioventricular junction to control refractory supraventricular arrhythmias. JAMA 1982;248(7):851-5. [MedLine]
10. Gallagher JJ, Svenson RH, Kasell JH, German LD, Bardy GH, Broughton A, et al. Catheter technique for closed-chest ablation of the atrioventricular conduction system: a therapeutic alternative for the treatment of refractory supraventricular tachycardia. N Engl J Med. 1982;306(4):194-200. [MedLine]
11. European Heart Rhythm Association (EHRA); European Cardiac Arrhythmia Scoiety (ECAS); American College of Cardiology (ACC); American Heart Association (AHA); Society of Thoracic Surgeons (STS), Calkins H, Brugada J, Packer DL, Cappato R, Chen SA, Crijins HJ, et al. HRS/EHRA/ECAS expert Consensus Statement on catheter and surgical ablation of atrial fibrillation: recommendations for personnel, policy, procedures and follow-up. A report of the Heart Rhythm Society (HRS) Task Force on catheter and surgical ablation of atrial fibrillation. Heart Rhythm. 2007;4(6):816-61. [MedLine]
12. Zimerman LI, Fenelon G, Martinelli Filho M, Grupi C, Atié J, Lorga Filho A, et al. Diretrizes Brasileiras de Fibrilação Atrial. Arq Bras Cardiol. 2009;92(supl.1):1-39.
13. Van Noord T, Van Gelder IC, Schoonderwoord BA, Crijns HJ. Immediate reinitiation of atrial fibrillation after electrical cardioversion predicts subsequent pharmacologic and electrical conversion to sinus rhythm on amiodarone. Am J Cardiol. 2000;86(12):1384-5.
14. Harrison L, Gallagher JJ, Kasell J, Anderson RH, Mikat E, Hackel DB, et al. Cryosurgical ablation of the A-V node-His bundle: a new method for producing A-V block. Circulation. 1977;55(3):463-70. [MedLine]
15. Williams JM, Ungerleider RM, Lofland GK, Cox JL. Left atrial isolation: new technique for the treatment of supraventricular arrhythmias. J Thorac Cardiovasc Surg. 1980;80(3):373-80. [MedLine]
16. Guiraudon GM, Klein GL, Yee R, Leitch JW, Kaushik RR, McLellan DG. Surgery for atrial tachycardia. Pacing Clin Electrophysiol. 1990;13(12 Pt 2):1996-9. [MedLine]
17. Cox JL, Schuessler RB, D'Agostinho Jr HJ, Stone CM, Chang BC, Cain ME, et al. The surgical treatment of atrial fibrillation. III. Development of a definitive surgical procedure. J Thorac Cardiovasc Surg. 1991;101(4):569-83. [MedLine]
18. Cox JL, Jaquiss RD, Schuessler RB, Boineau JP. Modification of the Maze procedure for atrial flutter and atrial fibrillation. II. Surgical technique of the maze III procedure. J Thorac Cardiovasc Surg. 1995;110(2):485-95. [MedLine]
19. Jatene AD, Sosa E, Tarasoutchi F, Jatene MB, Pomerantzeff PMA. Tratamento cirúrgico da fibrilação atrial. Procedimento do "labirinto": experiência inicial. Rev Bras Cir Cardiovasc. 1992;7(2):107-11. View article
20. Cox JL, Boineau JP, Schuessler RB, Kater KM, Lappas DG. Five-year experience with the maze procedure for atrial fibrillation. Ann Thorac Surg. 1993;56(4):814-24.
21. Jatene MB, Sosa E, Jatene FB, Tarasoutchi F, Monteiro AC, Salerno PR, et al. Evolução tardia da operação de Cox para fibrilação atrial em valvopatia mitral. Rev Bras Cir Cardiovasc. 1995;10(1):18-24. View article
22. Kim KB, Huh JH, Kang CH, Ahn H, Sohn DW. Modifications of the Cox-Maze III procedure. Ann Thorac Surg. 2001;71(3):816-22. [MedLine]
23. Szalay ZA, Skwara W, Pitschner HF, Faude I, Klövekorn WP, Bauer EP. Midterm results after the mini-maze procedure. Eur J Cardiothorac Surg. 1999;16(3):306-11. [MedLine]
24. Sueda T, Nagata H, Shikata H, Orihashi K, Morita S, Sueshiro M, et al. Simple left atrial procedure for chronic atrial fibrillation associated with mitral valve disease. Ann Thorac Surg. 1996;62(6):1796-800. [MedLine]
25. Haïssaguerre M, Marcus FI, Fischer B, Clémenty J. Radiofrequency catheter ablation in unusual mechanisms of atrial fibrillation: report of three cases. J Cardiovasc Electrophysiol. 1994;5(9):743-51. [MedLine]
26. Brick AV, Seixas T, Peres A, Vieira Jr JJ, Mattos JV, Mesquita A, et al. Reversão da fibrilação atrial crônica pela técnica do labirinto com aplicação de radiofreqüência e ultra-som transoperatórios. Rev Bras Cir Cardiovasc. 1999;14(4):290-7. View article
27. Williams M, Argenziano M, Oz M. Linear atrial ablation using laser energy. Columbia University College of Physicians and Surgeons; 2002.
28. Gillinov AM, Smedira NG, Cosgrove DM 3rd. Microwave ablation of atrial fibrillation during mitral valve operations. Ann Thorac Surg. 2002;74(4):1259-61. [MedLine]
29. Jazbik JC, Coutinho JH, Amar MR, Silva SL, Jazbik J, Jazbik AT, et al. Tratamento cirúrgico da fibrilação atrial em pacientes com insuficiência mitral: proposta inicial de uma nova abordagem cirúrgica. Rev SOCERJ. 1993;6(3):142-5.
30. Gregori Jr F, Cordeiro C, Goulart M, Couto N, Rosa V, Silva SS, et al. Técnica de Cox sem crioablação para tratamento cirúrgico da fibrilação atrial. Rev Bras Cir Cardiovasc. 1993;8(3):220-4. View article
31. Batista RJV, Franzoni M, Precoma D, Bochino L, Nery P, Oliveira E, et al. Autotransplante cardíaco: um novo método no tratamento de problemas cardíacos complexos. Rev Bras Cir Cardiovasc. 1995;10(2):90-100. View article
32. Kalil RAK, Lima GG, Abrahão R, Stürmer ML, Albrecht A, Moreno P, et al. Técnica cirúrgica simplificada pode ser eficaz no tratamento da fibrilação atrial crônica secundária a lesão valvar mitral? Rev Bras Cir Cardiovasc. 2000;15(2):129-35. View article
33. Krum D, Shetty S, Mare J, Silverstein E, Ishii T, Khan M, et al. Characteristics of myocardial lesions created using microwave energy: optimization of antenna design. Circulation. 1994;90(4 Part 2):I271.
34. He DS, Simmons WN, Zimmer JE, Marcus FI, Hynynen K, Lampe LF, et al. Comparison of several ultrasonic frequencies for cardiac ablation. Circulation. 1994;90(4 Part 2):I271.
35. Hindricks F, Mohr W, Autschbach R, Kottkamp H. Antiarrhytmic surgery for treatment of atrial fibrillation - new concepts. Thorac Cardiovasc Surg. 1999; 47 (supply) 365-369. [MedLine]
36. Taylor GW, Kay GN, Zheng X, Bishop S, Ideker RE. Pathological effects of extensive radiofrequency energy applications in the pulmonary veins in dogs. Circulation. 2000;101(14):1736-42. [MedLine]
37. Santos MA. Estudo experimental comparativo entre ultra-som e radiofreqüência na realização de linhas de ablação atriais por via epicárdica [Tese de doutorado]. São Paulo: Universidade Federal de São Paulo; 2003. 106p.
38. Caccitolo JA, Stulak JM, Schaff HV, Francischelli D, Jensen DN, Mehra R. Open-heart endocardial radiofrequency ablation: an alternative to incisions in Maze surgery. J Surg Res. 2001;97(1):27-33. [MedLine]
39. Manasse E, Infante M, Ghiselli S, Cariboni U, Alloisio M, Barbone A, et al. A video-assisted thoracoscopic technique to encircle the four pulmonary veins: a new surgical intervention for atrial fibrillation ablation. Heart Surg Forum. 2002;5(4):337-9. [MedLine]
40. Amaral JF. Laparoscopic application of an ultrasonically activated scalpel. Gastrointest Clin North Am. 1993;3:381-91.
41. Brick AV, Seixas TN, Portilho CF, Vieira Jr JJ, Mattos JV, Peres AK. Tratamento cirúrgico da taquicardia ventricular refratária: nova proposta técnica. Rev Bras Cir Cardiovasc. 1997;12(3):269-73. View article
42. Souza MT, Silva MD, Carvalho R. Revisão integrativa: o que é e como fazer. Einstein. 2010;8(1 pt 1):102-6.
43. Albrecht A, Kalil RA, Schuch L, Abrahão R, Sant'Anna JR, Lima G, et al. Randomized study of surgical isolation of the pulmonary veins for correction of permanent atrial fibrillation associated with mitral valve disease. J Thorac Cardiovasc Surg. 2009;138(2):454-9. [MedLine]
44. Vasconcelos JT, Scanavacca MI, Sampaio RO, Grinberg M, Sosa EA, Oliveira SA. Surgical treatment of atrial fibrillation through isolation of the left atrial posterior wall in patients with chronic rheumatic mitral valve disease: a randomized study with control group. Arq Bras Cardiol. 2004;83(3):203-10.
45. Gomes Jr JF, Pontes JCDV, Gomes OM, Duarte JJ, Gardenal N, Dias AMSAS, et al. Tratamento cirúrgico da fibrilação atrial crônica com eletrocautério convencional em cirurgia valvar mitral. Rev Bras Cir Cardiovasc. 2008;23(3):365-71. [MedLine] View article
46. Gallagher JJ, Sealy WC, Anderson RW, Kasell J, Millar R, Campbell RW, et al. Cryosurgical ablation of accessory atrioventricular connections: a method for correction of the pre-excitation syndrome. Circulation. 1977;55(3):471-9. [MedLine]
47. Fukada J, Morishita K, Komatsu K, Sato H, Shiiku C, Muraki S, et al. Is atrial fibrillation resulting from rheumatic mitral valve disease a proper indication for the maze procedure? Ann Thorac Surg. 1998;65(6):1566-9.
48. Lee JW, Choo SJ, Kim KI, Song JK, Kang DH, Song JM, et al. Atrial fibrillation surgery simplified with cryoablation to improve left atrial function. Ann Thorac Surg. 2001;72(5):1479-83. [MedLine]
49. Lee JW, Park NH, Choo SJ, Jo MS, Song H, Song MG. Surgical outcome of the maze procedure for atrial fibrillation in mitral valve disease: rheumatic versus degenerative. Ann Thorac Surg. 2003;75(1):57-61. [MedLine]
50. Cox JL, Ad N, Palazzo T, Fitzpatrick S, Suyderhoud JP, DeGroot KW, et al. Current status of the Maze procedure for the treatment of atrial fibrillation. Semin Thorac Cardiovasc Surg. 2000;12(1):15-9. [MedLine]
51. Blomström-Lundqvist C, Johansson B, Berglin E, Nilsson L, Jensen SM, Thelin S, et al. A randomized double-blind study of epicardial left atrial cryoablation for permanent atrial fibrillation in patients undergoing mitral valve surgery: the SWEDish Multicentre Atrial Fibrillation study (SWEDMAF). Eur Heart J. 2007;28(23):2902-8. [MedLine]
52. Johansson B, Bech-Hanssen O, Berglin E, Blomström P, Holmgren A, Jensen SM, et al. Atrial function after left atrial epicardial cryoablation for atrial fibrillation in patients undergoing mitral valve surgery. J Interv Card Electrophysiol. 2012;33(1):85-91. [MedLine]
53. Breda JR, Ragognette RG, Breda ASCR, Gurian DB, Horiuti L, Machado LN, et al. Avaliação inicial da ablação operatória biatrial por radiofrequência de fibrilação atrial. Rev Bras Cir Cardiovasc. 2010;25(1):45-50. [MedLine] View article
54. Viola N, Williams MR, Oz MC, Ad N. The technology in use for the surgical ablation of atrial fibrillation. Semin Thorac Cardiovasc Surg. 2002;14(3):198-205. [MedLine]
55. Beukema WP, Sie HT, Misier AR, Delnoy PP, Wellens HJ, Elvan A. Intermediate to long-term results of radiofrequency modified Maze procedure as an adjunct to open-heart surgery. Ann Thorac Surg. 2008;86(5):1409-14. [MedLine]
56. Williams MR, Stewart JR, Bolling SF, Freeman S, Anderson JT, Argenziano M, et al. Surgical treatment of atrial fibrillation using radiofrequency energy. Ann Thorac Surg. 2001;71(6):1939-44.
57. Kottkamp H, Hindricks G, Autschbach R, Krauss B, Strasser B, Schirdewahn P, et al. Specific linear left atrial lesions in atrial fibrillation: intraoperative radiofrequency ablation using minimally invasive surgical techniques. J Am Coll Cardiol. 2002;40(3):475-80. [MedLine]
58. Benussi S, Nascimbene S, Agricola E, Calori G, Calvi S, Caldarola A, et al. Surgical ablation of atrial fibrillation using the epicardial radiofrequency approach: mid-term results and risk analysis. Ann Thorac Surg. 2002;74(4):1050-6.
59. Canale LS, Colafranceschi AS, Monteiro AJO, Marques BM, Canale CS, Koehler EC, et al. Tratamento cirúrgico de fibrilação atrial utilizando ablação com radiofrequência bipolar em doença mitral reumática. Rev Bras Cir Cardiovasc. 2011;26(4):565-72. [MedLine] View article
60. Canale LS, Colafranceschi AS, Monteiro AJ, Coimbra M, Weksler C, Koehler E, et al. Uso da radiofrequência bipolar para o tratamento da fibrilação atrial durante cirurgia cardíaca. Arq Bras Cardiol. 2011;96(6):456-64. [MedLine]
61. Huang WZ, Wu YM, Ye HY, Jiang HM. Comparison of the outcomes of monopolar and bipolar radiofrequency ablation in surgical treatment of atrial fibrillation. Chin Med Sci J. 2014;29(1):28-32. [MedLine]
62. Dong L, Fu B, Teng X, Yuan HS, Zhao SL, Ren L. Clinical analysis of concomitant valve replacement and bipolar radiofrequency ablation in 191 patients. J Thorac Cardiovasc Surg. 2013;145(4):1013-7. [MedLine]
63. Phan K, Xie A, Tian DH, Shaikhrezai K, Yan TD. Systematic review and meta-analysis of surgical ablation for atrial fibrillation during mitral valve surgery. Ann Cardiothorac Surg. 2014;3(1):3-14. [MedLine]
64. Colafranceschi AS, Monteiro AJO, Botelho, ESL, Canale LS, Rabischoffsky A, Costa IP, et al. Cirurgia vídeo-assistida para a ablação da fibrilação atrial isolada por radiofrequência bipolar. Arq Bras Cardiol. 2009;93(4):334-42.
65. Abreu Filho CA, Lisboa LA, Dallan LA, Spina GS, Grinberg M, Scanavacca M, et al. Effectiveness of the Maze procedure using cooled-tip radiofrequency ablation in patients with permanent atrial fibrillation and rheumatic mitral valve disease. Circulation. 2005;112(9 suppl):I20-5. [MedLine]
66. MacDonald DR, Maruthappu M, Nagendran M. How effective is microwave ablation for atrial fibrillation during concomitant cardiac surgery? Interact Cardiovasc Thorac Surg. 2012;15(1):122-7. [MedLine]
67. Lin Z, Shan ZG, Liao CX, Chen LW. The effect of microwave and bipolar radio-frequency ablation in the surgical treatment of permanent atrial fibrillation during valve surgery. Thorac Cardiovasc Surg. 2011;59(8):460-4. [MedLine]
68. Brick AV, Seixas T, Portilho C, Peres AK, Vieira Jr JJ, Melo Neto R, et al. Tratamento intra-operatório da fibrilação atrial crônica com ultrasom. Rev Bras Cir Cardiovasc. 2001;16(4):337-49.
69. Ninet J, Roques X, Seitelberger R, Deville C, Pomar JL, Robin J, et al. Surgical ablation of atrial fibrillation with off pump, epicardial, high-intensity focused ultrasound: results of a multicenter trial. J Thorac Cardiovasc Surg. 2005;130(3):803-9. [MedLine]
70. Lins RMM, Lima RC, Silva FPV, Menezes AM, Salerno PR, Thé EC, et al. Tratamento da fibrilação atrial com ablação por ultrassom, durante correção cirúrgica de doença valvar cardíaca. Rev Bras Cir Cardiovasc. 2010;25(3):326-32. [MedLine] View article
71. Groh MA, Binns OA, Burton HG 3rd, Champsaur GL, Ely SW, Johnson AM. Epicardial ultrasonic ablation of atrial fibrillation during concomitant cardiac surgery is a valid option in patients with ischemic heart disease. Circulation. 2008;118(14 Suppl):S78-82. [MedLine]
72. Ad N, Cheng DC, Martin J, Berglin EE, Chang BC, Doukas G. Surgical ablation for atrial fibrillation in cardiac surgery: a consensus statement of the International Society of Minimally Invasive Cardiothoracic Surgery (ISMICS) 2009. Innovations. 2010;5(2):74-83.
No financial support.
Authors' roles & responsibilities
AVB Study design; writing of the manuscript or critical review of its content; final approval of the manuscript
DMB Study design; writing of the manuscript or critical review of its content; final approval of the manuscript
Article receive on Tuesday, September 8, 2015
 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license