Objective: To investigate the pulmonary function and pain in adult patients undergoing heart surgery via sternotomy and to verify possible correlations of these variables with the characteristics of the surgical procedure and hospital stay. Methods: A cross-sectional study was carried out of 70 individuals undergoing heart surgery. The lung function was assessed before and after surgery by spirometry and incentive spirometry. Details of the surgical procedure were studied and patients were followed up postoperatively using a visual analogue scale and design of the human body to evaluate pain. Results: The pulmonary function was significantly impaired in the postoperative compared to preoperative period (P <0.01). The pain was centered in the region of the sternotomy and persisted until at least the 5th postoperative day. There was a correlation between pain and the parameters of pulmonary function (forced expiratory volume in 1 second - percentage: r = -0.271, P <0.047; peak expiratory flow: r = -0.357, P <0.008; and maximum inspiratory volume: r = -0.293, P <0.032). There was no significant correlation between pain and other variables. Conclusion: There was significant impairment of lung function which had not recovered completely on the 5th postoperative day. Pain was a complaint that persisted throughout the study period. The parameters of pulmonary function showed a significant relationship with pain. There was no correlation between pain and the characteristics of individuals, the surgical procedure or the length of hospital stay.
OBJETIVO: Avaliar o comportamento da função pulmonar e da dor em pacientes adultos submetidos à cirurgia cardíaca por esternotomia. Além de verificar possíveis correlações e comparações dessas variáveis com as características do procedimento cirúrgico e o tempo de internação hospitalar. MÉTODOS: Foi realizado estudo de coorte composto de 70 indivíduos, nos quais foi avaliada a função pulmonar préoperatória por espirometria e inspirometria de incentivo. Os pacientes foram acompanhados no pós-operatório, por meio de protocolo com informações da cirurgia, função pulmonar e um protocolo de avaliação álgica (escala análoga visual e desenho do corpo humano). RESULTADOS: Os valores de função pulmonar do período pós-operatório apresentaram diminuição significativa em relação ao pré-operatório (P<0,01). A dor localizou-se na região da esternotomia, persistindo até o 5º dia de pósoperatório. Houve correlação da dor com os parâmetros de função pulmonar (volume expiratório forçado no 1º segundo - percentual r=-0,271 e P<0,047; pico de fluxo expiratório r=-0,357 e P<0,008; volume inspiratório máximo r=-0,293 e P<0,032). Não se observou correlação significativa da dor com outras variáveis. CONCLUSÃO: Observou-se prejuízo significativo da função pulmonar, não se restabelecendo completamente até o 5º dia de pós-operatório. A dor foi uma queixa que persistiu durante todo o período do estudo. Os parâmetros de função pulmonar apresentaram relação significativa com a dor. Não houve correlação entre dor e as características dos indivíduos, do procedimento cirúrgico e tempo de internação hospitalar.
INTRODUCTION
Pain, the main manifestation reported by patients who undergo heart surgery, has a multifactorial character. The factors that influence pain may be the surgical incision, retraction and dissection of tissue during the surgical procedure, multiple intravenous cannulations, chest drains and the invasive procedures to which these patients are submitted during treatment [1].
Median sternotomy is the most commonly used approach in heart surgeries due to the easy access to the region. However this approach may significantly affect the pulmonary function due to the consequent instability of the chest. According to publications, pain caused by the surgical procedures associated to sternotomy is an important cause of morbidity and mortality, and thus affects the postoperative evolution. The surgical technique can alter gas exchange by modifying ventilatory mechanics and cause restrictive alterations to the pulmonary function [2-5].
Westerdahl et al. [6] reported that individuals can present with atelectasis, a significant reduction in pulmonary volumes and hypoxemia in the immediate postoperative period of coronary artery bypass surgery (CABG). These complications may be related to the effects of anesthesia, to events in the transoperative period, to diaphragmatic dysfunction, to medications and to the hemodynamic status of patients [7].
In the literature, postoperative pain is described as being one condition responsible for respiratory dysfunction associated with the aforementioned factors [8,9]. The intensity of pain increases mainly when the parietal pleura is maneuvered to perform left internal thoracic artery (LITA) grafts, causing additional surgical injury and a reduction in the inspiratory muscle force [10]. Hence, postoperative pain is considered normal and expected. Because of the lack of understanding about the physiology of pain and the pharmacology of analgesics, the surgical team is more concerned about the most common postoperative complications rather than the symptom that most concerns the patient, pain [11]. Perhaps strategies to improve pain control may begin to be developed when more is understood out the characteristics of postoperative pain and its influence on pulmonary function during this period.
The objective of this study was to evaluate pulmonary function in respect to pain in adult patients submitted to heart surgery via sternotomy and to investigate possible correlations and comparisons of these variables with the characteristics of the surgical procedure and the length of hospital stay.
METHODS
This was a prospective cross-sectional cohort study with a non-probabilistic, intentional sample performed in the period from March 2005 to September 2007 in the Santa Casa Hospital Complex. The study was approved by the Research Ethics Committees of the institutions involved (Centro Universitário Metodista do Sul IPA # 1142/04 and Santa Casa Hospital Complex # 930/04).
The men and women enrolled in this study fulfilled the following inclusion criteria: age greater than 18 years old and no history of thoracic surgeries including heart surgery via sternotomy. The patients were selected from the hospitalization list of the government healthcare system (SUS) of the Cardiology Unit of Santa Clara Polyclinic. The objectives of the study were explained to all participants who signed consent forms before being enrolled.
The following conditions were considered exclusion criteria: unstable angina (Class III - classification of Braunwald), urgent or emergency surgeries and mediastinal tumors. Initially 125 patients were selected for this study. Of these, 27 were excluded with 33.3% of these patients refusing to participate in the study.
A total of 98 individuals participated in the study, however 28 did not complete all the stages and are considered lost. The main reasons for these losses were: the surgery was moved to an earlier date or cancelled, dates of surgical procedures after the data collection period, all the tests were not completed as the patient complained of tiredness and intubation time greater than 24 hours (Figure 1).
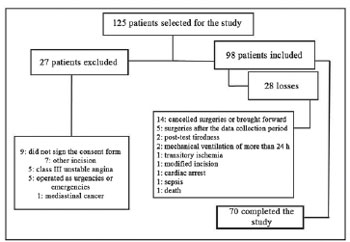
Fig.1 - Dados dos pacientes relacionados para o estudo
The study was completed with 70 patients who had been electively submitted to CABG and/or valve replacement surgery (metallic or biological) via sternotomy, with cardiopulmonary bypass (CPB) or not and who were extubated according to the norms of the service.
During the preoperative period, an evaluation was performed that consisted in collecting the patient's data, including detailed information about risk factors and associated diseases. Additionally, the pulmonary function was tested by means of lung function trests and incentive spirometry (to obtain an estimate of the maximum inspiratory volume) [12,13].
The pulmonary function, tested using the MicroPlus model (Micro Medical Limited®, Kent, England) and Vitalograph micro (Vitalograph®, Ennis, Ireland) spirometers provided measurements of the forced vital capacity (FVC), the forced expiratory volume in the first second (FEV
1), the forced expiratory coefficient in the first second (FEV
1/FVC%) and the peak expiratory flow (PEF). The patient, 15 minutes after the spirometric maneuver, performed incentive spirometry using a Sherwood device (Voldyne®) chosen due to its low cost and the easy reproducibility of the method to obtain the maximum inspiratory volume (Vimax) [12,13]. Three measurements were taken for all the parameters of both tests with a rest of one minute between each set of measurements. Spirometry followed the criteria established by the guidelines for pulmonary function tests [14]. The best of the three maneuvers was used as long as the difference between the first and second best was less than 10%.
All patients left the surgical center with a nº 36 drain (Braile®, São Paulo, Brazil); located in the pleura in 13 (18.57%) patients, mediastinum in 19 (27.14%) and in both for 38 (54.28%) patients. The patients underwent pulmonary function tests on the 1
st, 2
nd, 3
rd and 5
th postoperative days. During this period, a follow-up protocol was utilized that included information on the surgical procedure and data of the pulmonary function. To evaluate the pain, a specific protocol was utilized that consisted in front and back views of the human body divided into 37 anatomical areas on which the patients were instructed to mark the most painful area. This was applied together with a visual analogous subjective scale (VAS) of 0 (no pain) to 10 (the most intense pain) for each painful area (pain scale utilized by Mueller et al.) [1]. The length of hospital stay of the patients was recorded.
In the immediate postoperative period, the analgesia employed by the service consisted of morphine (2 to 10 mg) diluted in 9 mL of distilled water with extra 1 mL of morphine added to the solution at 3 to 4-hour intervals. This solution was slowly but continuously infused at 2 mg to 5 mg per hour (when necessary). During the hospital stay, 750mg or 500mg paracetamol was prescribed every 6 hours when necessary. Standard evaluations were carried out before and after the surgery by the authors with controlled use of analgesics.
The Statistical Package for Social Sciences (SPSS) version 17.0 was employed to analyze the data. Initially, the Kolmogorov-Smirnov normality test was performed to check that the continuous variables had parametric distributions. In the descriptive analysis, the continuous variables were expressed as means, medians, 25% and 75% interquartile intervals and standard deviations and the categorical variables as frequencies and percentages. The analysis of variance test (ANOVA) together with the Bonferroni adjustment was utilized to compare the results of the pre- and post-operative pulmonary function tests. The Friedman test followed by the Wilcoxon test with Finner adjustment was used to compare the intensity of pain on the postoperative days. The Mann-Whitney non-parametric test was utilized in the comparison of the type of surgery with the pulmonary function variables and pain. The Spearman correlation coefficient was used to identify correlations between two continuous variables. The level of significance was set for a
P-value < 0.05.
RESULTS
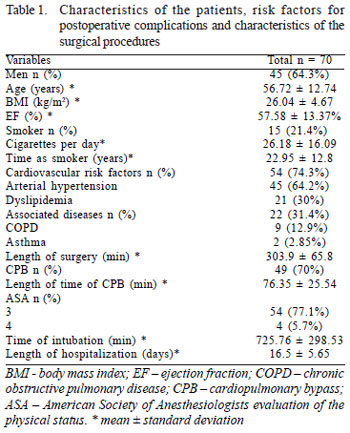
The characteristics of the patients and the surgical procedures, as well as the main risk factors for postoperative complications and length of hospital stay are shown in Table 1.
The surgical procedures carried out were valve replacement in 34 (48.57%) patients, CABG in 27 (38.57%) and combined valve replacement and CABG in 9 (12.85%) patients. Saphenous vein grafts were utilized in 14 (20%) patients and saphenous vein and LITA grafts were performed in 13 (18.57%). For 13 (18.57%) patients the aortic valve was replaced by a metallic prosthesis and for 11 (15.71%) the aortic valve was replaced by a biological prosthesis. The most common combined surgery, in three (4.28%) patients, was CABG utilizing the saphenous vein and valve replacement using a biological prosthesis.
The pulmonary function in the postoperative period compared to the pre-operative period is demonstrated in Table 2. On the 1st postoperative day, the function diminished considerably compared to the preoperative period for FEV
1, FVC, EFP and Vimax. Even on the 5
th postoperative day these values had not returned to the levels seen before the surgery.
The percentages of the FEV
1 and FVC had similar patterns to the absolute values (Table 3). There were significant differences for both the FEV1 and FVC between the preoperative period and the postoperative days (
P<0.01). The difference in the FEV
1 on the 1
st postoperative day compared to the 2
nd, 3
rd and 5
th postoperative days was also significant (
P<0.01). Statistically significant differences were seen for the FEV
1 comparing the 2nd and 3rd postoperative days (
P<0.05), the 2
nd and 5
th postoperative days (
P<0.01) and the 3
rd and 5
th postoperative days (p<0.02).
There were significant differences in the FVC between the 1
st and 3rd postoperative days (
P<0.04), between the 1
st and 5
th postoperative days (
P<0.01) and between the 2
nd and 5
th postoperative days (
P<0.01). However, there were no significant differences between the 1
st and 2
nd postoperative days (P=0.928) or between the 2
nd and 3
rd postoperative days (
P=0.196).
Thirty-three patients did not present with pain during the postoperative period. The painful region most commonly identified was that of the sternum, with the spinal column (T10) being the second most cited area.
Of those who felt pain on the 1
st postoperative day, the median level of pain was 5 (range: 2.75 - 8.0), on the 2
nd postoperative day it was 5 (range: 2.0 - 7.0) and on the 3
rd and 5
th postoperative days the scores were 3 (range: 0.5 - 6.0) and 3 (range: 0 - 6.0), respectively. In respect to pain, there was no significant difference between the first two postoperative days (
P=0.726) however statistically significant differences were observed comparing the 1st postoperative day with the 3
rd and 5
th postoperative days (
P<0.01).
A statistically significant difference was found for pain on comparing the 2
nd and 3
rd postoperative days (
P<0.003), however no significant difference was observed comparing the 2
nd and 5
th postoperative days (
P=0.192). Additionally no significant difference was observed on comparing the 3
rd and 5
th postoperative days (
P=0.827).
When the pulmonary function is correlated with pain, there was a significant negative relationship for FEV
1, EFP and Vimax on the 1
st postoperative day. This correlation is shown in Table 4.
On analyzing the length of hospital stay with pulmonary function and pain, a significant correlation was observed for the preoperative values of FEV
1 and Vimax and the values of EFP and Vimax on the 5
th postoperative day (Figure 2). The pain did not present any association with the length of hospital stay. The results of this correlation are shown in Table 5.
The intubation time was associated with the changes in the pulmonary function variables. Of the preoperative measurements, only the absolute value of FEV
1 had a significant negative correlation (r = -0.237 and
P < 0.049). On the 1
st postoperative day, a significant negative correlation was found for FEV
1, EFP and Vimax (r = -0.365 and P<0.005; r = -0.366 and
P<0.004; r= -0.310 and
P<0.017, respectively), and on the 5
th postoperative day significant negative correlations were found for the same variables as the 1st postoperative day (r = -0.326 and
P<0.009; r= -0.364 and
P<0.03; r= -0.331 and
P<0.007, respectively).
On comparing the preoperative values of the variables with the same variables on the 5th postoperative day no significant correlation was observed between the pulmonary function and the time of intubation. Pain was also not correlated with the time of mechanical ventilation (1st postoperative day - r=0.146 and P=0.245; 5th postoperative day - r=0.272 and P=0.067) and the variation between the 1st and 5th postoperative days (r=0.066 and P=0.667).
Despite of the low number of patients who performed combined surgery, a significant correlation was found between the pulmonary function variables and pain. For the 1
st postoperative day, a statistically significant difference was only observed for the EFP (
P< 0.05) but for the 5th postoperative day a statistically significant difference was found with pain (
P < 0.008), FEV
1 (
P < 0.005), FVC (
P < 0.001), FVC percent (
P < 0.014), EFP (
P < 0.044) and the Vimax (
P < 0.005) and for the variation of the pulmonary function variables from the percentage value of FEV
1 (
P < 0.013) and of FVC (
P < 0.039).
When pain is considered in respect to the characteristics of the participants and to the characteristics of the surgeries, no statistical significance was noted. On comparing the different postoperative days, the time of analgesia was not associated with pain.
DISCUSSION
In this study, major impairment of the pulmonary function is observed in the postoperative period as identified by a significant reduction (
P<0.01) in the pulmonary function variables compared to the preoperative period. These changes in the pulmonary function are a common finding in studies about heart surgery [15,16]; thus this is a well known complication although the causes are still being investigated.
CPB is considered one of the factors responsible for pulmonary injuries due to the increase in airways resistance and respiratory dysfunction caused by this procedure [17,18]. Chest drains also cause significant changes in the FEV
1 and FVC. Guizilini et al. [19] reported that intercostal drains are worse than mediastinal drains due to friction caused by the respiratory movement.
The incision itself was also questioned by Lichtenberg et al. [4], who demonstrated that a mini-incision results in less impairment of the pulmonary function than median sternotomy, and less pain thereby making early mobilization possible due to sternal stability. However this relationship can not be confirmed in the current study as the objectives did not consider this question.
As was demonstrated in this study, there is still a significant reduction in the pulmonary volumes and capacities on the 5
th postoperative day. Morsch et al. [15] and Renault et al. [16] also observed that the significant impairment to the pulmonary function is not completely recovered on the 7
th postoperative day.
In this study, pain was evaluated using a VAS which is a subjective scale with scores between 0 and 10. To analyze the pattern of pain in the postoperative period, the scores were expressed as medians and 25 and 75 percentiles. In the immediate postoperative period (1
st postoperative day) the pain was significantly more intense (p<0.01) compared to the 5
th postoperative day. These findings are similar to the results of other publications [20] however few studies evaluate pain in the postoperative period of heart surgery.
The descriptive form of this variable is still controversial as works that use this tool report it using means and standard deviations. However in biostatistics this variable is classified as a qualitative variable and so the correct way to compare levels of pain is by medians and 25 and 75 percentiles. This makes a discussion of this finding difficult.
The finding that the pain was located in the region of the sternotomy up to the 5
th postoperative day is different to the work of Giacomazzi et al. [20], who reported that the pain is located in the region of the sternotomy until the 3
rd postoperative day after which it moves to the lower extremity associated to the saphenectomy. These variations in the location and in the intensity of the pain occur because the initial painful stimuli diminish with time (the time from the surgical procedure, sternal instability and the use of drains, for example) [11].
The pain had a significant negative correlation with the variables of the pulmonary function (FEV
1, EFP and Vimax), confirming other published results about impairment of pulmonary function after heart surgery [20]. Chest drains, in particular intercostal drains, that perforate the intercostal pleura and intercostal muscles [19] and that limit inspiration are one cause.
Moreover the use of the LITA may influence the pulmonary function, as this is an additional surgical trauma that diminishes the blood supply to the intercostal muscles, thus reducing the ventilatory muscle force [21]. However in our study the ventilatory muscle force was not evaluated as this is contra-indicated in the immediate postoperative period by the guidelines of pulmonary function tests [13].
As was demonstrated in the current study, a significant negative correlation was found between the length of hospitalization and the pulmonary function parameters, proving that heart surgery via sternotomy causes greater respiratory impairment due to the friction of the sternum related to upper chest instability, thereby prolonging the hospital stay of these patients and increasing hospital costs [21].
The time of mechanical ventilation was negatively associated to the pulmonary function parameters. The use of mechanical ventilation has been identified as one of the main factors of pulmonary injury in adults submitted to heart surgery. Studies performed with mechanically ventilated patients demonstrated alterations in the pulmonary extravascular fluid, capillary permeability, in the production of inflammatory mediators and in the development of cellular necrosis [22,23].
Thus as the time of mechanical ventilation proved to be a factor that caused pulmonary function impairment, the type of surgery was also responsible for this injury. According to Renault et al. [18], surgical trauma may alter the contractile properties of the diaphragm and result in incoordination of the rib cage thus causing fatigue of the respiratory muscles.
In our study, a significant difference was observed when the results of the pulmonary function tests were compared in combined surgeries. Publications have provided evidence that the use of the LITA may be a factor responsible for reduced pulmonary function. Mueller et al. [21] reported that the impact of the LITA is moderated in the postoperative period by the greater surgical trauma that this graft causes, however their study did not test the pulmonary function.
On comparing pain with the type of surgery, a significant statistical difference was found for combined surgeries. This result was different to that reported by Mueller et al. [1], who did not find any statistical difference in the characteristics of pain when the different types of surgery were compared, even in procedures with greater painful stimulation such as in valve surgeries. However these authors did not mention if patients submitted to LITA grafts were included in their sample. Yet, in the current study, no relationship between the use of the LITA and the level of pain was found, as of the 70 patients studied, only 13 received LITA grafts and none of the combined surgeries used this graft for CABG.
In the current study, no significant relationships between the characteristics of the participants (age, gender, BMI, etc.) and the surgical procedure were observed. It has been reported that individuals with BMIs greater than 30 kg/m
2 suffer more pain, possibly due to the difficulty of administering adequate analgesia [1]. The findings of this study can not confirm this hypothesis, as only six patients had BMIs greater than 30 kg/m
2.
This study presented some limitations including the high loss of patients with surgeries frequently being cancelled or brought forward (Fig. 1). This may have occurred because the surgical center was closed for a period as the institution was analyzing how to improve the care for government healthcare patients. Additionally, a radiological evaluation was not performed which might have shown pulmonary complications affecting the pulmonary function parameters. The pulmonary function tests presented a limitation in that the results depend on the patients' comprehension of the maneuvers and the patients desire to perform the tests. The resource to evaluate the maximum inspiratory volume is not specific but it is easy to reproduce and of low cost.
Previous works suggest that better prepared and collaborative patients may identify pain earlier [23]. As pain is a common symptom in the postoperative period of heart surgery, the rehabilitation team should also receive training on this subject aiming at early recognition and treatment of pain.
CONCLUSION
The current study observed a significant impairment in the pulmonary function, which did not completely recover by the 5
th postoperative day. This alteration may be better perceived with the association between pain and pulmonary function parameters. The pain was located in the region of the sternotomy, and was a complaint that persisted during all the period of the study. The pulmonary function was negatively correlated with the length of mechanical ventilation and the length of hospitalization, which may have been determined by the association of the preoperative pulmonary function with the surgical injury. Significant differences were observed between the combined surgery, pulmonary function parameters and pain which are explained by the greater amount of surgical procedures that escalated these alterations in the postoperative period. There was no correlation between pain and the characteristics of the individuals, the type of surgical procedure or the length of hospital stay.
ACKNOWLEDGEMENTS
The authors would like to thank the teams of the Cardiology Unit of the Santa Clara Polyclinic and of the Surgical Intensive Care Unit of Hospital São Francisco of the Santa Casa Hospital Complex of Porto Alegre, Brazil for their effort and collaboration during this study.
1. Mueller XM, Tinguely F, Tevaearai HT, Revelly JP, Chioléro R, von Segesser LK. Pain location, distribution, and intensity after cardiac surgery. Chest. 2000;118(2):391-6. [MedLine]
2. Magnano D, Montalbano R, Lamarra M, Ferri F, Lorini L, Clarizia S, et al. Ineffectiveness of local wound anesthesia to reduce postoperative pain after median sternotomy. J Card Surg. 2005;20(4):314-8. [MedLine]
3. Cimen S, Ozkul V, Ketenci B, Yurtseven N, Günay R, Ketenci B, et al. Daily comparison of respiratory functions between on-pump and off-pump patients undergoing CABG. Eur J Cardiothorac Surg. 2003;23(4):589-94. [MedLine]
4. Lichtenberg A, Hagl C, Harringer W, Klima U, Haverich A. Effects of minimal invasive coronary artery bypass on pulmonary function and postoperative pain. Ann Thorac Surg. 2000;70(2):461-5. [MedLine]
5. Mueller XM, Tinguely F, Tevaearai HT, Ravussin P, Stumpe F, von Segesser LK. Impact of duration of chest tube drainage on pain after cardiac surgery. Eur J Cardiothorac Surg. 2000;18(5):570-4. [MedLine]
6. Westerdahl E, Lindmark B, Bryngelsson I, Tenling A. Pulmonary function 4 months after coronary artery bypass graft surgery. Respir Med. 2003;97(4):317-22. [MedLine]
7. Taggart DP. Respiratory dysfunction after cardiac surgery: effects of avoiding cardiopulmonary bypass and the use of bilateral internal mammary arteries. Eur J Cardiothorac Surg. 2000;18(1):31-7. [MedLine]
8. Erb J, Orr E, Mercer CD, Gilron I. Interactions between pulmonary performance and movement-evoked pain in the immediate postsurgical period: implications for perioperative research and treatment. Reg Anesth Pain Med. 2008;33(4):312-9. [MedLine]
9. Bonnet F, Marret E. Postoperative pain management and outcome after surgery. Best Pract Res Clin Anaesthesiol. 2007;21(1):99-107. [MedLine]
10. Almeida PLBM. Impacto da reabilitação cardiopulmonar intrahospitalar pré e pós-operatória em ex-tabagistas submetidos à cirurgia de revascularização miocárdica - um ensaio clínico randomizado [Dissertação de Mestrado]. Porto Alegre: Universidade Federal do Rio Grande do Sul;2007. [citado 2008 Set 26]. Disponível em: URI: http://hdl.handle.net/10183/14035.
11. Watt-Watson J, Stevens B, Katz J, Costello J, Reid GJ, David T. Impact of preoperative education on pain outcomes after coronary artery bypass graft surgery. Pain. 2004;109(1-2):73-85. [MedLine]
12. Romanini W, Muller AP, Carvalho KAT, Olandoski M, Faria-Neto JR, Mendes FL, et al. Os efeitos da pressão positiva intermitente e do incentivador respiratório no pós-operatório de revascularização miocárdica. Arq Bras Cardiol. 2007;89(2):105-10.
13. Müller AP, Olandoski M, Macedo R, Costantini C, Guarita-Souza LC. Comparative study between intermittent (Müller Reanimator) and continuous positive airway pressure in the postoperative period of coronary artery bypass grafting. Arq Bras Cardiol. 2006;86(3):232-9. [MedLine]
14. Pereira CAC, Jansen JM, Barreto SSM, Marinho J, Sulmonett N, Dias RM. Espirometria. In: Diretrizes para testes de função pulmonar. J Pneumol. 2002;28:S1-S82.
15. Morsch KT, Leguisamo CP, Camargo MD, Coronel CC, Mattos W, Ortiz LDN, et al. Perfil ventilatório dos pacientes submetidos a cirurgia de revascularização do miocárdio. Rev Bras Cir Cardiovasc. 2009;24(2):180-7. [MedLine] View article
16. Renault JA, Costa-Val R, Rossetti MB, Houri Neto M. Comparação entre exercícios de respiração profunda e espirometria de incentivo no pós-operatório de cirurgia de revascularização do miocárdio. Rev Bras Cir Cardiovasc. 2009;24(2):165-72 [MedLine] View article
17. Silva AMRP, Campagnucci VP, Pereira WL, Rosa RF, Franken RA, Gandra SMA, et al. Revascularização do miocárdio sem circulação extracorpórea em idosos: análise da morbidade e mortalidade. Rev Bras Cir Cardiovasc. 2008;23(1):40-5. [MedLine] View article
18. Renault JA, Costa-Val R, Rossetti MB. Fisioterapia respiratória na disfunção pulmonar pós-cirurgia cardíaca. Rev Bras Cir Cardiovasc. 2008;23(4):562-9. [MedLine] View article
19. Guizilini S, Gomes WJ, Faresin SM, Carvalho ACC, Jaramillo JI, Alves FA, et al. Efeitos do local de inserção do dreno pleural na função pulmonar no pós-operatório de cirurgia de revascularização do miocárdio. Rev Bras Cir Cardiovasc. 2004;19(1):47-54. View article
20. Giacomazzi CM, Lagni VB, Monteiro MB. A dor pósoperatória como contribuinte do prejuízo na função pulmonar em pacientes submetidos à cirurgia cardíaca. Rev Bras Cir Cardiovasc. 2006;21(4):386-92.
21. Mueller XM, Tinguely F, Tevaearai HT, Revelly JP, Chioléro R, von Segesser LK. Pain pattern and left internal mammary artery grafting. Ann Thorac Surg. 2000;70(6):2045-9. [MedLine]
22. Wrigge H, Uhlig U, Baumgarten G, Menzenbach J, Zinserling J, Ernst M, et al. Mechanical ventilation strategies and inflammatory responses to cardiac surgery: a prospective randomized clinical trial. Intensive Care Med. 2005;31(10):1379-87. [MedLine]
23. Wrigge H, Uhlig U, Zinserling J, Behrends-Callsen E, Ottersbach G, Fischer M, et al. The effects of different ventilatory settings on pulmonary and systemic inflammatory responses during major surgery. Anesth Analg. 2004;98(3):775-81.

 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license