ABSTRACT
Introduction: The incidence of intravascular embolization of venous catheters reported in the world medical literature corresponds to 1% of all the described complications. However, its mortality rate may vary between 24 to 60%. Catheter malfunction is the most likely signal of embolization, since patients are usually asymptomatic. Objective: To report the method of removing intravascular foreign bodies, catheters with the use of various endovascular techniques and procedures. Methods: This is a two-year retrospective study of 12 patients: seven women and five men. The average age was 29 years (ranging from two months to 65 years). Results: Technical performance was 100% successful. Ten port-a-caths, one intra-cath and one PICC were extracted. The most common sites for the lodging of one of the ends of the intravascular foreign bodies were the right atrium (41.6%) and the right ventricle (33.3%). In 100% of the cases, only one venous access was used for extraction of foreign bodies, and in 91.6% of the cases (11 catheters) the femoral access was used. The loop-snare was used in 10 cases (83.3%). The most common cause of intravascular foreign body insertion was a catheter fracture, which occurred in 66.6% of the cases (eight cases). One major complication, the atrial fibrillation, occurred (8.3%), which was related to the intravascular foreign body extraction. The mortality rate in 30 days was zero. Conclusion: Percutaneous retrieval of intravascular foreign bodies is considered gold standard treatment because it is a minimally invasive, relatively simple, safe procedure, with low complication rates compared to conventional surgical treatment.
RESUMO
Introdução: A incidência da embolização de cateteres intravenosos, na literatura mundial, é de 1% dentre todas as complicações descritas. Porém, possui taxa de mortalidade podendo variar de 24 a 60%. O não funcionamento do cateter é a suspeita diagnóstica principal da embolização, visto que, habitualmente, os pacientes são assintomáticos. Objetivo: Relatar o manejo na extração de corpos estranhos intravenosos, com o uso de táticas e técnicas endovasculares diversas. Métodos: Estudo retrospectivo com 12 pacientes, no período de dois anos. Sete pacientes eram do sexo feminino e cinco do sexo masculino, com média de idade de 29 anos (dois meses a 65 anos). Resultados: Sucesso técnico foi obtido em 100% dos casos. Foram extraídos 10 port-a-caths, um intra-cath e um PICC. Os locais mais frequentes de alojamento de uma das extremidades dos corpos estranhos intravenosos foram o átrio direito (41,6%) e o ventrículo direito (33,3%). Em 100% dos casos se utilizou um único acesso venoso. O acesso femoral foi o mais utilizado, em 91,6% dos casos (11 cateteres). Utilizou-se o laço (loop-snare) em 10 (83,3%) casos. O motivo mais frequente da presença do corpo estranho intravascular foi a fratura do cateter, que ocorreu em 66,6% dos casos (oito pacientes). Houve uma complicação, fibrilação atrial (8,3%), relacionada à extração de corpo estranho intravenoso. A taxa de mortalidade em 30 dias foi igual a zero. Conclusão: A retirada de corpos estranhos intravenosos por via percutânea é considerada tratamento padrão ouro, por se tratar de procedimento minimamente invasivo, relativamente simples, seguro e com baixas taxas de complicações quando comparada ao tratamento cirúrgico convencional.
INTRODUCTION
The use of central venous access in medical practice has become more and more common. The applications of this technique include drug administration, chemotherapies, or parenteral nutrition; hemodynamic monitoring; implantation of defibrillators and/or pacemakers, or else, as an access for endovascular treatments.
Several types of catheter are used in this practice:
intra-cath, Double lumen and PICC (peripheral inserted central catheter),
perm-cath and
Hickman (semi-implantable) and Port-a-cath (totally implantable). The main catheter-related complications include venous or catheter thrombosis and infection. Embolization of a catheter or a fragment from the catheter is rare and occurs in around 1% of patients[1-4]. Despite its low incidence, embolization may cause severe and potentially fatal complications such as: thromboembolia[5,6], bacterial endocarditis[7], sepsis, myocardial lesions, and cardiac arrhythmias[8]. The mortality rate may vary from 24 to 60%[9]. Therefore, the removal of foreign bodies is always recommended. Before the development of endovascular techniques for the removal of foreign bodies, the removal of these objects was made by conventional surgery. In some cases, the professionals adopted an attitude of mere expectation. The use of endovascular techniques was found to be safe and effective, and has become the most common treatment in the referred situations, besides having a low complication rate[1,2,3,4,9].
The aim of the present study is to demonstrate the method of removal of intravascular foreign bodies, catheters, with the use of various endovascular techniques and procedures.
METHODS
This is a retrospective study based on data collected from the medical records of 12 consecutive patients (seven women and five men) treated from July 2007 to July 2009. The average age was 29 years (from two months to 65 years) (Table 1). The catheters were implanted by a heterogeneous group of professionals composed of vascular, thoracic and pediatric surgeons, for
port-a-caths catheters, and doctors and nurses, for the implantation of catheters for a short period of time. All patients with x-ray diagnosis of catheter migration or fracture were referred for an interventional radiology suite and they had the catheters removed. All patients were asymptomatic. Using hemodynamic monitoring, all the procedures were followed-up by anesthesiologists.
Technique
Through percutaneous venous access, preferably the right common femoral vein, the implantation of the 8-French sheath is performed, which made it possible to handle the materials. One 5-French guiding catheter, with a curved configuration to locate the foreign body, is passed over 0.035" 260 cm hydrophilic guide wire and placed next to one of the catheter ends. After positioning the guide wire, the 5-French catheter is removed, and the extraction device, preferably the
loop-snare, is introduced on the same guide wire, until it is placed at the anterior end of the catheter. At this moment, the intravascular foreign body, a catheter, is grasped by the device and taken to the 8-F sheath to be removed.
RESULTS
The most commonly used site for catheter insertion was the internal jugular vein - the right side in four patients and left side in two patients - totalizing six accesses. Ten
port-a-caths, one
intra-cath and one PICC were extracted. All catheters or fragments of catheters were removed in one piece, without fragmentation. The successful retrieval process rate was as high as 100%. The most common sites for the lodging of one of the ends of the intravascular foreign bodies were the right atrium (41.6%) and the right ventricle (33.3%)(Table 1).
In 100% of the cases, only one venous access was used for extraction of foreign bodies, and in 91.6% of the cases (11 catheters) the femoral access was used, with the right femoral vein being the most commonly used access - 83.3% (10 catheters)(Table 01). In case 9, the left common femoral access was used, since the proximal end of the catheter was in the left external iliac vein. The patient was a 2-month-old baby and, thus, a 4-French sheath was used (Figure 1). In case 10, the only venous access available, the right subclavian vein was used (8.3%)(Figure 2).
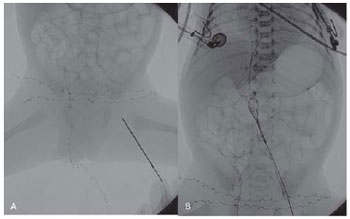
Fig. 1 - A - Puncture of the left common femoral vein. Use of 4-French materials. Distal end of the catheter located in the left external iliac vein. B - Retrieval of PICC type catheter with loopsnare

Fig. 2 - A - Puncture of the right subclavian vein. B - Retrieval of the distal end of the catheter with the loop-snare. Hydrophilic guide wire parallel to the loop-snare with its distal end located in the inferior vena cava. C - Removal of the whole set with the hydrophilic guide wire in the inferior vena cava (maintenance of subclavian venous access)
The most used extraction device was the
loop-snare in 10 cases (83.3%). It was also the device preferred by the expert team. The
Basket was used in one case (8.3%). In the absence of these materials, in case 8, a long micro-guide wire (300 cm) was folded and introduced into one 5-French guiding catheter with a cobra II curved configuration making a loop (8.3%). Then, the distal end of the catheter located in the inferior vena cava was captured, and the whole catheter was grasped (Figure 3).

Fig. 3 - A - Catheter proximal end located in the right innominate vein and the distal end located in the inferior vena cava. B - Retrieval of the distal end of catheter with an improvised loop-snare (cobra II 5-French catheter and 300 cm folded micro-guide wire). C - Removal of the intravascular foreign body through the right femoral vein
The most common cause of intravascular foreign body insertion was the catheter fracture, which occurred in 66.6% of the cases (8 cases). Diagnosis of catheter fracture occurred in 87.5% of the cases (7 out of 8 cases) after an attempt to use
port-a-caths, that is, for those patients who still used the access. Only in one case (12.5%) a catheter fracture occurred during the surgery for its removal (case 12). It was also found that the fracture of
port-a-cath type catheters were the predominant cause (100% of the cases) of catheter embolization related to subclavian venous access ports (cases 4,10,11 and 12). Another cause of intravascular foreign body insertion was catheter migration, which occurred in four patients (33.3%). In case 2, the migration occurred during the intra-cath implantation in the right subclavian vein. In case 6, a disconnection between the catheter and the port occurred. In case 8, catheter migration followed an attempt to exchange a
port-a-cath for a
permcath. In case 9, migration occurred during the implantation of the PICC in the left vena saphena magna (Table 1).
Atrial fibrillation was a major complication and occurred in 8.3% of the cases, which were related to intravascular foreign body extraction. The mortality rate in 30 days was equal to zero.
DISCUSSION
Intravascular or catheter embolization of a foreign body, either by fracture or migration, is a rare condition, occurring in approximately 1%[1-4], but if left untreated, it may cause serious complications and even death, leading to a high mortality rate[9]. Due to this high mortality rate, extraction of foreign bodies is strongly recommended even in asymptomatic patients.
Percutaneous intervention for removal of intravascular foreign bodies is currently the best treatment option for patients. It is a minimally invasive, relatively simple, safe procedure, with low complication rates compared to conventional surgical treatment[1-4,9-15].
In the present study, most catheters extracted were totally implantable
port-a-cath type catheters, maybe due to the fact that these catheters must be in place for a long time, which may cause them to wear out more quickly. Of the 10
port-a-caths retrieved, eight were fractured, and four were implanted in subclavian veins (100%). These fractures were caused by a chronic compression of the catheter between the clavicle and the first rib, known as a
pinch-off syndrome. This syndrome may be prevented by using the jugular access, or else by the implantation of the catheter in the most lateral part of the subclavian vein[16-18]. One catheter was disconnected from the reservoir (port) and was removed intact. This may have been caused by incorrect fixation of the safety lock or a manufacture defect in the
port-a-cath [19]. The incidence of disconnection between the catheter and the reservoir was 0.2%[20]. A technical error occurred during the implantation of another
port-a-cath, in the
intra-cath and in the PICC (25%).
There are some devices for extraction of intravascular foreign bodies in the market which have proven to be very effective in some situations. However, the most versatile, more used and preferred by the expert team was the loop-snare. It is a loop at a right angle to the handle, of various sizes and amplitudes (5 to 35mm), and arrangements (one or three loops). These characteristics facilitate the removal of foreign bodies[21-23].
The venous access recommended for the removal of intravascular foreign bodies is the common femoral vein [11], preferably the right one. The advantages of this approach include: easier handling; the patient feels more comfortable; puncture is facilitated by the blood vessel diameter and because the vessel is situated close to the surface of the skin; presence of posterior bone protection that allows its fixation during puncture and safety in the effective compression following the removal of the objects; Access to the main sites of migration of intravascular foreign bodies, and a vessel diameter that allows for the insertion of materials of various sizes. Depending on the degree of difficulty of the procedure, one femoral vein can be used, or both simultaneously, although it is always preferable to use only one access. In the present series, the referred access was used in 91.6% of the cases. However, there are cases in which this approach is not available. In case 10, the patient had a history of deep venous thrombosis (DVT) of the lower limbs and an inferior vena cava filter, which made the access through the femoral veins impossible. Attempt to access the site through the right and left internal jugular veins were unsuccessful due to thrombosis. The removal of the foreign body and the implantation of a new
port-a-cath were requested. So, we chose to puncture the right subclavian vein (previous access of the fractured
port-a-cath), implantation of the 8-French sheath, passing the guide wire into the distal end of the catheter located in the right ventricle and the placement of the
loop-snare guiding catheter. Parallel to the guide wire, the hydrophilic guide wire was simultaneously introduced through the 8-French sheath, and this one was placed in the inferior vena cava, ensuring subclavian venous access.
The most common site of lodging of The loop-snare was introduced through the guiding catheter until the distal end, the catheter was grasped and the whole set was removed, including the 8-French sheath, but maintaining the access to the right subclavian vein through the guide wire located in the inferior vena cava[24]. Then, a new port-a-cath was implanted (Figure 02). One of the tips of catheters in this series was the right atrium (41.6%) followed by the right ventricle (33.3%)(Table 1). The right atrium and the trunk of pulmonary artery are common sites of lodging of these foreign bodies described in the literature. However, the right ventricle is not a common site[1-4,9,13]. The site of lodging of post-embolization catheter depends on the vein used as access for the implantation, on the length and flexibility of the catheter, on the blood flow in the vessel or in the cardiac chamber, and on patient positioning at the moment of the incident[25]. In case 11, the two tips of the catheter were in the right ventricle. The previous mobilization of one of the tips was necessary in order to make the retrieval. During the mobilization of the foreign body with a curved catheter and a guide wire, the patient showed cardiac arrhythmia and atrial fibrillation without hemodynamic instability which could only be reversed with Amioradona in the interventional suite. One of the tips of the catheter was dislocated to the trunk of a pulmonary artery and could be retrieved. The patient remained in the intensive care unit for 24 hours under hemodynamic monitoring, and no alterations in the electrocardiogram were noted, so he was discharged (Fig. 4). Transitory cardiac arrhythmias may occur during the foreign body retrieval, which are related to the manipulation of cardiac chambers[4]. However, persistent arrhythmias that can only be reversed with drugs have been described[8,14]. We believe that the longer the time required and the manipulation of cardiac chambers for the removal of the catheter, the greater the chance of occurring persistent cardiac arrhythmia - with these conditions being directly related to the positioning of the intravascular foreign body. The foreign body with its two ends inside the right ventricle does not favor its removal, requiring greater manipulation of the cardiac chamber, thus increasing the risk of arrhythmias. Besides cardiac arrhythmia, as an early complication, the presence of hematoma in the puncture site is another possible and more common complication. No hematoma and no late complications (a 30 day-period after the extraction) were found. The mortality rate was zero.
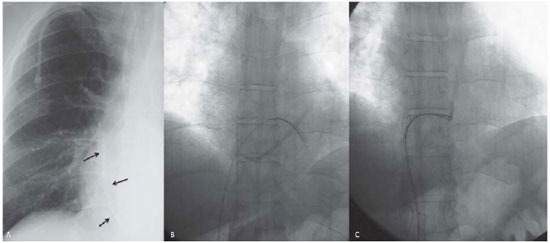
Fig. 4 - A - Simple chest x-ray showing a catheter fragment inside the right ventricle. B - Catheter entirely located in the right ventricle. Position not favorable to retrieval. C - Retrieval of catheter with the loop-snare previously mobilized to the trunk of pulmonary artery
The incidence of intravascular embolization of venous catheters reported in the world medical literature corresponds to 1% of all the described complications. The most likely diagnosis of catheter embolization is device malfunction, since patients are usually asymptomatic. This diagnosis can be confirmed by chest x-ray. Previous extraction of all diagnosed foreign bodies is recommended to avoid potentially serious and fatal complications. Percutaneous retrieval of intravascular foreign bodies is considered a gold standard treatment because it is a minimally invasive, relatively simple, safe procedure, with low complication rates compared to conventional surgical treatment.
REFERENCES
1. Smouse HB, Fox PF, Brady TM, Swischuk JL, Castañeda F, Pham MT. Intravascular foreign body removal. Semin Intervent Radiol. 2000;17:201-12.
2. Andrews RE, Tulloh RM, Rigby ML. Percutaneous retrieval of central venous catheter fragments. Arch Dis Child. 2002;87(2):149-50. [MedLine]
3. Uflacker R, Lima S, Melichar AC. Intravascular foreign bodies: percutaneous retrieval. Radiology. 1986;160(3):731-5. [MedLine]
4. Andrade G, Marques R, Brito N, Bomfim A, Cavalcanti D, Abath C. Cateteres intravenosos fraturados: retirada por técnicas endovasculares. Radiol Bras. 2006;39(3):199-202.
5. Suárez-Peñaranda JM, Guitian-Barreiro, Concheiro-Carro L. Longstanding intracardiac catheter embolism. An unusual autopsy finding. Am J Forensic Med Pathol. 1995;16(2):124-6. [MedLine]
6. Knutson H, Stenberg K. Pulmonary embolism after catheter break. Nord Med. 1959;62:1491. [MedLine]
7. Balbi M, Bertero G, Bellotti S, Rolandelli ML, Caponnetto S. Right-sided valvular endocarditis supported by an unexpected intracardiac foreign body. Chest. 1990;97(6):1486-8. [MedLine]
8. Denny MA, Frank LR. Ventricular tachycardia secondary to Port-a-Cath fracture and embolization. J Emerg Med. 2003;24(1):29-34. [MedLine]
9. Gabelmann A, Kramer S, Gorich J. Percutaneous retrieval of lost or misplaced intravascular objects. AJR Am J Roentgenol. 2001;176(6):1509-13. [MedLine]
10. Yang FS, Ohta I, Chiang HJ, Lin JC, Shih SL, Ma YC. Nonsurgical retrieval of intravascular foreign body: experience of 12 cases. Eur J Radiol. 1994;18(1):1-5. [MedLine]
11. Egglin TK, Dickey KW, Rosenblatt M, Pollak JS. Retrieval of intravascular foreign bodies: experience in 32 cases. AJR Am J Roentgenol. 1995;164(5):1259-64. [MedLine]
12. Liu JC, Tseng HS, Chen CY, Chern MS, Ko SC, Chiang JH, et al. Percutaneous retrieval or intravascular foreign bodies: experience with 19 cases. Kaohsiung J Med Sci. 2002;18(10):492-9. [MedLine]
13. Surov A, Jordan K, Buerke M, Persing M, Wollschlaeger B, Behrmann C. Atypical pulmonary embolism of port catheter fragments in oncology patients. Support Care Cancer. 2006;14(5):479-83. [MedLine]
14. Cheng CC, Tsai TN, Yang CC, Han CL. Percutaneous retrieval of dislodged totally implantable central venous access system in 92 cases: experience in a single hospital. Eur J Radiol. 2009;69(2):346-50. [MedLine]
15. Chow LM, Friedman JN, Macarthur C, Restrepo R, Temple M, Chait PG, et al. Peripherally inserted central catheter (PICC) fracture and embolization in the pediatric population. J Pediatr. 2003;142(2):141-4. [MedLine]
16. Hinke DH, Zandt-Stastny DA, Goodman LR, Quebbeman EJ, Krzywda EA, Andris DA. Pinch-off syndrome: a complication of implantable subclavian venous access devices. Radiology. 1990;177(2):353-6. [MedLine]
17. Schlangen JT, Debets JM, Wils JA. The "pinch-off phenomenon": a radiological symptom for potential fracture of an implanted permanent subclavian catheter system. Eur J Radiol. 1995;20(2):112-3. [MedLine]
18. Kim OK, Kim SH, Kim JB, Jeon WS, Jo SH, Lee JH, et al. Transluminal removal of a fractured and embolized indwelling central venous catheter in the pulmonary artery. Korean J Intern Med. 2006;21(3):187-90. [MedLine]
19. Ballarini C, Intra M, Pisani Ceretti A, Cordovana A, Pagani M, Farina G, et al. Complications of subcutaneous infusion port in the general oncology population. Oncology. 1999;56(2):97-102. [MedLine]
20. Kock HJ, Pietsch M, Krause U, Wilke H, Eigler FW. Implantable vascular access systems: experience in 1500 patients with totally implanted central venous port systems. World J Surg. 1998;22(1):12-6. [MedLine]
21. Yedlicka JW Jr, Carlson JE, Hunter DW, Castañeda-Zúñiga WR, Amplatz K. Nitinol gooseneck snare for removal of foreign bodies: experimental study and clinical evaluation. Radiology. 1991;178(3):691-3. [MedLine]
22. Cekirge S, Weiss JP, Foster RG, Neiman HL, McLean GK. Percutaneous retrieval of foreign bodies: experience with the nitinol Goose Neck snare. J Vasc Interv Radiol. 1993;4(6):805-10. [MedLine]
23. Ventura LM, Affonso BB, Carnevale FC. Retirada de corpos estranhos intravasculares. In: Carnevale FC, editor. Radiologia intervencionista e cirurgia endovascular. 1ª Ed. São Paulo:Revinter;2006. p351-6.
24. Motta-Leal-Filho JM, Carnevale FC, Cerri GG. Subclavian vein an unusual access for the removal of intravascular foreign bodies. Ann Vasc Surg.2010, in press. DOI 10.1016/j.avsg.2010.02.031 [MedLine]
25. Bloomfield DA. Techniques of nonsurgical retrieval of iatrogenic foreign bodies from the heart. Am J Cardiol. 1971;27(5):538-45. [MedLine]
Article receive on Sunday, January 17, 2010




 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license