ABSTRACT
BACKGROUND: It has been well documented that women have higher morbidity and mortality rates than men following coronary artery bypass graft (CABG) surgery. In view of this evidence, it is necessary to know if there is benefit to off-pump CABG surgery in women in comparison to on-pump CABG. OBJECTIVES: Compare outcomes between off-pump CABG and on-pump CABG in women. METHODS: Retrospective study. Our investigation analyzes comparatively clinical profile, thirteen procedure complications and mortality of a population of 941 consecutive women undergoing CABG surgery (549 off-pump and 392 on-pump) at two hospitals for the period January 2000 to December 2005. RESULTS: Mortality rate for women undergoing off-pump CABG surgery is lower than for women undergoing on-pump surgery, however, not statistically significant (3.1% vs 5.3%; P=0.134). The complication rates analyzed (hemorrhagic shock, neurologic, respiratory, acute renal failure, adult respiratory distress syndrome, septicemia, pneumonia, atrial fibrillation) were lower (significant statistically difference) for women off-pump than women on-pump, with the exception of low cardiac output and wound infection. CONCLUSIONS: Evidence suggests that off-pump CABG surgery may be better for women than on-pump CABG surgery because it appears to reduce morbimortality rates. Ten of 13 complications investigated demonstrated an advantage for women undergoing off-pump surgery relative to those receiving on-pump surgery.
RESUMO
INTRODUÇÃO: Tem sido bem documentado que mulheres têm taxas de morbimortalidade mais altas que homens submetidos à cirurgia de revascularização miocárdica (CRM). Em vista desta evidência, é necessário saber se há benefício da CRM sem circulação extracorpórea (CEC) em comparação à CRM com CEC. OBJETIVOS: Comparar desfechos de morbimortalidade entre CRM sem CEC e CRM com CEC. MÉTODOS: Estudo retrospectivo. Nossa investigação analisa comparativamente o perfil clínico, 13 complicações relativas ao procedimento e mortalidade de uma população de 941 mulheres submetidas à CRM (549 sem CEC e 392 com CEC) em dois hospitais, no período de janeiro de 2000 a dezembro de 2005. RESULTADOS: A taxa de mortalidade em mulheres submetidas à CRM sem CEC é menor que mulheres submetidas à CRM com CEC, entretanto, a diferença não é estatisticamente significativa (3,1% vs. 5,3%; P=0,134). As taxas de complicações analisadas (choque hemorrágico, neurológicas, respiratórias, insuficiência renal aguda, síndrome da angústia respiratória do adulto, septicemia, pneumonia, fibrilação atrial) foram menores (diferença estatisticamente significativa) em mulheres do grupo CRM sem CEC em comparação ao grupo CRM com CEC, com exceção das complicações baixo débito cardíaco e infecção de ferida operatória. CONCLUSÕES: As evidências sugerem que CRM sem CEC pode beneficiar as mulheres em comparação com CRM com CEC, pois parece reduzir as taxas de morbimortalidade. Dez das 13 complicações investigadas demonstraram uma significativa vantagem das mulheres submetidas à CRM sem CEC em relação àquelas submetidas à CRM com CEC.
INTRODUCTION
It has been established that women, compared to men, have higher morbidity and higher mortality related to coronary artery bypass grafting (CABG)[1]. In view of these higher rates in women, studies are needed to examine whether women who undergo surgery without cardiopulmonary bypass (CPB) receive any benefits compared to those who undergo surgery with CPB.
Although OPCAB has been widely performed in recent years, few data are available about the way women behave in each type of surgery (off-pump versus on-pump). Studies suggest that female gender is an independent risk factor for higher rates of mortality and morbidity after CABG, but long-term survival and functional recovery are similar to those in men who underwent CABG[2-4].
Other studies have suggested that, on average, women have a clinical preoperative disadvantage that can influence, by far, this difference found. These findings are not universal, taking into consideration that there are significant differences in clinical practice compared to different institutions[5].
It is essential that short- and long term safety, benefits and efficacy of OPCAB are assessed (as seen in other studies[6]), so that we can, indeed, know whether this new approach to surgical treatment of arterial disease coronary artery is higher or at least not inferior to the technique that is already established as the gold standard (on-pump CABG) in the world literature, in female patients.
The aim of this study was to investigate the differences in outcomes in female patients undergoing on-pump CABG compared with those undergoing OPCAB, tracing the preoperative clinical profile and analyzing the differences in rates of complications and possible differences in mortality rates.
METHODS
We studied 941 female patients undergoing CABG with two centers: Service of Cardiovascular Surgery at University Hospital Osvaldo Cruz (HUOC) and Cardiothoracic Surgery Unit (UNITÓRAX) of the Real Hospital Português, from January 2000 to December 2005.
Retrospective review was performed from the database of medical and surgical records from the previously mentioned centers and, initially, two groups were created: on-pump CABG (392 patients) and OPCAB (549 patients).
From then on, in a comparable manner, the following variables were assessed:
Preoperative clinical characteristics: average age, age > 70 years, smoking, diabetes mellitus, type of surgery (urgent or elective), acute renal failure, chronic renal failure, chronic obstructive pulmonary disease (COPD), preoperative cardiogenic shock, systemic arterial hypertension, previous infarction, presence of acute infarction, cardiomyopathy, heart failure, prior percutaneous treatment, reoperation, mitral valve disease, myocardial electrical conduction disturbance, peripheral vascular disease, prior cerebrovascular accident (CVA), unstable angina; Characteristics of the procedure: number of vessels treated (use of only saphenous vein graft, only mammary, use of both); Major complications related to the procedure: hemorrhagic shock, neurological damage (stroke or transient ischemic attack - TIA), low cardiac output, acute renal failure requiring hemodialysis; Minor complications related to the procedure: respiratory, acute respiratory distress syndrome (ARDS), wound infection, pneumonia, sepsis, peripheral vascular disease, postoperative atrial fibrillation, need for transfusion in the postoperative period;
Mortality rate
After data collection, the variables studied were stored in 6.0 EPI.INFO software for statistical analysis. Student's t test was used only in comparisons of mean age and number of vessels treated (quantitative variables). For all other variables (qualitative) it was used chi-square test. Results were considered statistically significant when P value was less than 0.05.
This study was approved by the Research Ethics Committee of the Hospital Complex of the University Hospital Oswaldo Cruz/Cardiac Emergency of Pernambuco - HUOC/PROCAPE, No. 115/2009.
RESULTS
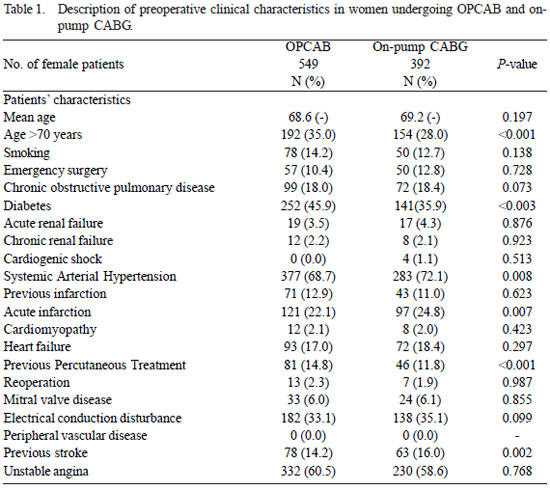
Characteristics of patients (Table 1)
Patients undergoing OPCAB had a mean age of 68.6 years and those undergoing on-pump CABG had a mean age of 69.2 years (P=0.197). Thirty-five percent of the OPCAB group were aged > 70 years versus 28.0% with on-pump CABG (P<0.001). The on-pump CABG group was more likely to produce hypertension (P=0.008), acute myocardial infarction (P=0.007) and previous stroke (P=0.002). In OPCAB group, there were more patients with diabetes (P<0.003) and higher percentage of women who have undergone previous percutaneous coronary treatment (P<0.001). The other variables showed no statistically significant differences between groups.
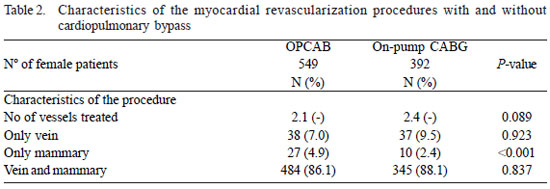
Characteristic of the procedure (Table 2)
There was no statistically significant difference compared to the total number of vessels treated (mean 2.1 vs. 2.4, P=0.089). The vast majority of both groups received mammary and saphenous vein graft. On average, women undergoing OPCAB received more single graft of the left mammary (4.9% vs. 2.4%, P<0.001).
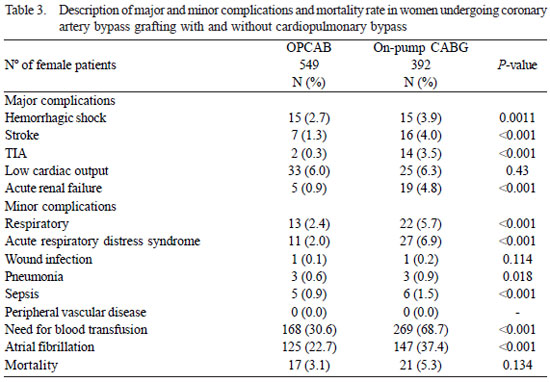
Major complications (Table 3)
Rates of hemorrhagic shock (2.7% vs. 3.9%, P=0.0011), stroke (1.3% vs. 4.0%, P<0.001), TIA (0.3% vs. 3.5%, P=0.0011), low cardiac output (6.0% vs. 6.3%, P=0.43) and acute renal failure requiring hemodialysis (0.9% vs. 4.8%, P<0.001) were lower in OPCAB group.
Minor complications (Table 3)
The rates of respiratory complications (2.4% vs. 5.7%, P<0.001), ARDS (2.0% vs. 6.9%, P<0.001), wound infection (0.1% vs . 0.2%, P=0.114), pneumonia (0.6% vs. 0.9%, P=0.018), sepsis (0.9% vs. 1.5%, P<0.001), need for blood transfusion (30.6% vs. 68.7%, P<0.001) and atrial fibrillation (22.7% vs. 37.4%, P<0.001) were lower in the group without CPB.
Mortality (table 3)
The mortality rate was lower in OPCAB when compared to on-pump CABG group (3.1% vs. 5.3%), however, this difference was not statistically significant (P=0.134).
DISCUSSION
It is unclear whether the female gender is an independent predictor of risk for adverse complications in coronary artery bypass surgery or if there are other variables occurring more often in women, which increase the risk. The Bypass Angioplasty Revascularization Investigation (BARI) showed that, after adjusting of risk factors in women, females showed an independent predictor of survival at 5 years[7]. Other possible reasons include the fact that women have a higher incidence of diabetes, which leads to increased postoperative complications, especially in the insulin-dependent group[8]. Late presentation in a state of emergency and/or emergency is also a variable that occurs more often in women, which leads to higher rates of complications.[9] It has been demonstrated a higher incidence of left ventricular hypertrophy and hypertensive heart disease in women, which has been proposed as causes of major complications[5].
In an attempt to reduce morbidity and mortality for conventional CABG, the OPCAB procedure was reintroduced in the 80s and widespread throughout the world in 90s. The elimination of cardiopulmonary bypass and systemic inflammatory response associated with this, it was expected that early adverse outcomes could be reduced without compromising outcomes in the long term. Retrospective analysis of databases have shown statistically significant benefit in operative mortality with the use of OPCAB[10,11]. However, all these tests are subject to selection biases that can not be accounted for in retrospective series.
On-pump CABG activates the complement and fibrinolytic cascade, contributing to postoperative bleeding[12]. In our study, we observed lower rates of hemorrhagic shock and also decrease in the need for blood transfusions in the OPCAB group compared to on-pump CABG group. This removal of blood transfusion reduces the risk of infections[13]. In our study, women undergoing OPCAB had less pneumonia and sepsis compared to patients undergoing on-pump CABG, however, we can not say that this decrease was necessarily due to decrease in blood product transfusions, since we have not performed that analysis.
Studies have suggested higher rates of stroke in patients undergoing on-pump CABG when compared to those undergoing OPCAB[14]. CPB can potentially contribute to neurological injury by loss of autoregulation of cerebral flow at low temperatures or by low perfusion pressure, micro and macroemboli, and alteration of the blood-brain barrier by the systemic inflammatory response, resulting in cerebral edema[15]. Randomized studies[16,17] on on-pump CABG versus off-pump CABG in multivessel disease patients clearly demonstrate significant radiological and biochemical evidence of greater brain injury, as well as greater numbers of cerebral emboli detectable[18] in patients undergoing on-pump CABG. This information is consistent with our findings, in which women undergoing OPCAB had significantly reduced rates of stroke and TIA postoperatively compared to those undergoing on-pump CABG.
Assessing the early postoperative outcomes, we have demonstrated reduced incidence of low cardiac output in OPCAB group (difference not statistically significant). This finding suggests a lower degree of myocardial injury in OPCAB. Some studies[19] show lower release of enzymes from myocardial injury in the postoperative (CK, CK-MB, troponin T, parameters of myocardial injury) in patients undergoing OPCAB. The regional normothermic ischemia in OPCAB, the temporary interruption of coronary flow approached, seems to cause less myocardial injury compared to hypothermic global ischemia induced by cardioplegic arrest[20].
The BHACAS-1 study (Beating Heart versus Cardioplegic Arrest Studies)[21] as well as other non-randomized prospective study[22] showed significant reduction in glomerular function (using the creatinine clearance) and tubular function (through fractional excretion of sodium and free water clearance) when comparing the use of off-pump CABG with OPCAB. The etiology of renal dysfunction after cardiac surgery is multifactorial[23] and in patients with multiple comorbidities that are associated with postoperative renal dysfunction (elderly, diabetics, previous renal failure), the CPB is associated with increased risk of developing renal failure requiring dialysis[24]. In our series, women undergoing OPCAB had a significant reduction of acute renal failure requiring dialysis postoperatively compared to those undergoing on-pump CABG.
Inflammatory response induced by CPB seems to impair lung function,[24]. In our study, women undergoing OPCAB demonstrated significant reduction in respiratory complications, indicating less pulmonary injury.
In studies BHACAS 1 and 2[21], it was found that on-pump CABG was associated with a higher rate of postoperative arrhythmias compared with OPCAB. Another study[25] showed that the CPB associated with cardioplegic arrest was an independent predictor of atrial fibrillation postoperatively. Again, our findings agree with these studies, with an incidence of atrial fibrillation in the postoperative of OPCAB significantly lower than the group that underwent on-pump CABG.
The mortality rate was lower in OPCAB compared to on-pump CABG group (3.1% versus 5.3%, 17 and 21 patients respectively), however, this difference was not statistically significant. Although this difference may seem low, if we translate these data in terms of relative risk, the OPCAB showed decrease of 41.5% in mortality when compared to on-pump CABG. One should take into account the fact that in the OPCAB group there was a higher percentage of diabetic women (P<0.003) and that, despite the difference in average age in the groups was not statistically significant, this group showed a higher percentage of women with over 70 years (P<0.001).
Recently, Shroyer et al.[26] published controversial study (ROOBY Trial) about the subject OPCAB versus on-pump CABG. The study started in 2002 and completed in 2008, randomizing 1099 patients to on-pump CABG group and 1104 patients to the OPCAB group (all elective surgery, no emergency). In the short-term analysis, the study's primary outcome included a composite of death or postoperative complications, for example, reoperation, new mechanical support or cardiac arrest within the first 30 days postoperatively.
The researchers did not observe any differences in outcomes between groups On-pump CABG and OPCAB. However, we should emphasize several factors that limit the conclusions of this study: it was not double-blind, low average number of procedures performed by surgeon, more than half of surgeries performed by residents, 99% men; analysis of patency with catheterization only in the postoperative period, without confirmation of patency of the grafts equivalent between groups in intraoperative period at the end of the procedure (which leaves the results at the mercy of possible technical failures at the time of closure of the chest). Such a study should be read and interpreted carefully to avoid harming the use of OPCAB - surgical procedure already established and that has demonstrated many benefits to patients.
There are some important limitations in this study that require caution in interpretation: 1) The data presented herein are not adjusted for specific risk attributed to clinical characteristics, and it is possible that the choice of surgical procedure is based on these clinical differences, a fact that is not captured by the analysis of the database; 2) The groups are not matched with respect to preoperative clinical characteristics, which compromises in some degree the findings; 3) An intention to treat can not be identified because the database only identifies the use or not use of CPB, so that conversions from OPCAB to on-pump CABG intraoperatively can not be analyzed, a fact that may bias the adverse outcomes in on-pump CABG, 4) the study population was assessed retrospectively. In order to these limitations are overcome, we need more prospective randomized studies.
CONCLUSION
The OPCAB in women decreased the rate of complications compared with on-pump CABG. Although we found lower mortality rate in the group without CPB, this study was not powered to demonstrate robustly that difference.
REFERENCES
1. Edwards FH, Carey JS, Grover FL, Bero JW, Hartz RS. Impact of gender on coronary bypass operation mortality. Am Thorac Surg. 1998;66(1):125-31.
2. Brandup-Wognsen G, Berggren H, Hartford M, Hjalmarson A, Karlsson T, Herlitz J. Female sex is associated with increased mortality and morbidity early, but not late, after coronary artery bypass grafting. Eur Heart J. 1996;17(9):1426-31. [MedLine]
3. Risum O, Abdelnoor M, Nitter-Hauge S, Levorstad K, Svennevig JL. Coronary artery bypass surgery in women and in men; early and long-term results. A study of the Norwegian population adjusted by age and sex. Eur J Cardiothorac Surg. 1997;11(3):539-46. [MedLine]
4. Hochman JS, McCabe CH, Stone PH, Becker RC, Cannon CP, DeFeo-Fraulini T, et al. Outcome and profile of women and men presenting with acute coronary syndromes: a report from TIMI IIIB: TIMI Investigators. Thrombolysis in Myocardial Infarction. J Am Coll Cardiol. 1997;30(1):141-8. [MedLine]
5. King KB, Clark PC, Hicks GL Jr. Patterns of referral and recovery in women and men undergoing coronary artery bypass grafting. Am J Cardiol. 1992;69(3):179-82. [MedLine]
6. Lima RC, Escobar MAS, Lobo Filho JG, Diniz R, Saraiva A, Césio A, et al. Resultados cirúrgicos na revascularização do miocárdio sem circulação extracorpórea: análise de 3.410 pacientes. Rev Bras Cir Cardiovasc. 2003;18(3):261-7. View article
7. Jacobs AK, Kelsey SF, Brooks MM, Faxon DP, Chaitman BR, Bittner V, et al. Better outcome for women compared with men undergoing coronary revascularization: a report from the bypass angioplasty revascularization investigation (BARI). Circulation. 1998;98(13):1279-85. [MedLine]
8. Szabó Z, Hakanson E, Svedjeholm R. Early postoperative outcome and medium-term survival in 540 diabetic and 2239 nondiabetic patients undergoing coronary artery bypass grafting. Ann Thorac Surg. 2002;74(3):712-9. [MedLine]
9. O'Rourke DJ, Malenka DJ, Olmstead EM, Quinton HB, Sanders JH Jr, Lahey SJ, et al. Improved in-hospital mortality in women undergoing coronary artery bypass grafting. Northern New England Cardiovascular Disease Study Group. Improved in-hospital mortality in women undergoing coronary artery bypass grafting. Ann Thorac Surg. 2001;71(2):507-11. [MedLine]
10. Wenger NK. Is what's good for the gander good for the goose? J Thorac Cardiovasc Surg. 2003;126(4):929-31. [MedLine]
11. Mack MJ, Brown PP, Kugelmass AD, Battaglia SL, Tarkington LG, Simon AW, et al. Current status and outcomes of coronary revascularization 1999 to 2002: 148,396 surgical and percutaneous procedures. Ann Thorac Surg. 2004;77(3):761-8.
12. Mack MJ, Pfister A, Bachand D, Emery R, Magee MJ, Connolly M, et al. Comparison of coronary bypass surgery with and without cardiopulmonary bypass in patients with multivessel disease. J Thorac Cardiovasc Surg. 2004;127(1):167-73. [MedLine]
13. Cartier R, Brann S, Dagenais F, Martineau R, Couturier A. Systematic off-pump coronary artery revascularization in multivessel disease: experience of three hundred cases. J Thorac Cardiovasc Surg. 2000;119(2):221-9. [MedLine]
14. Lund C, Hol PK, Lundblad R, Fosse E, Sundet K, Tennoe B, et al. Comparison of cerebral embolization during off-pump and on-pump coronary artery bypass surgery. Ann Thorac Surg. 2003;76(3):765-70.
15. Taylor KM. Central nervous system effects of cardiopulmonary bypass. Ann Thorac Surg. 1998;66(5 Suppl):S20-4.
16. Lloyd CT, Ascione R, Underwood MJ, Gardner F, Black A, Angelini GD. Serum S-100 protein release and neuropsychologic outcome during coronary revascularization on the beating heart: a prospective randomized study. J Thorac Cardiovasc Surg. 2000;119(1):148-54. [MedLine]
17. Wandschneider W, Thalmann M, Trampitsch E, Ziervogel G, Kobinia G. Off-pump coronary bypass operations significantly reduce S100 release: an indicator for less cerebral damage? Ann Thorac Surg. 2000;70(5):1577-9. [MedLine]
18. Bowles BJ, Lee JD, Dang CR, Taoka SN, Johnson EW, Lau EM, et al. Coronary artery bypass performed without the use of cardiopulmonary bypass is associated with reduced cerebral microemboli and improved clinical results. Chest. 2001;119(1):25-30. [MedLine]
19. Koh TW, Carr-White GS, DeSouza AC, Ferdinand FD, Hooper J, Kemp M, et al. Intraoperative cardiac troponin T release and lactate metabolism during coronary artery surgery: comparison of beating heart with conventional coronary artery surgery with cardiopulmonary bypass. Heart. 1999;81(5):495-500. [MedLine]
20. Czerny M, Baumer H, Kilo J, Lassnigg A, Hamwi A, Vukovich T, et al. Inflammatory response and myocardial injury following coronary artery bypass grafting with or without cardiopulmonary bypass. Eur J Cardiothorac Surg. 2000;17(6):737-42. [MedLine]
21. Angelini GD, Taylor FC, Reeves BC, Ascione R. Early and midterm outcome after off-pump and on-pump surgery in Beating Heart Against Cardioplegic Arrest Studies (BHACAS 1 and 2): a pooled analysis of two randomised controlled trials. Lancet. 2002;359(9313):1194-9. [MedLine]
22. Loef BG, Epema AH, Navis G, Ebels T, van Oeveren W, Henning RH. Off-pump coronary revascularization attenuates transient renal damage compared with on-pump coronary revascularization. Chest. 2002;121(4):1190-4. [MedLine]
23. Conlon PJ, Stafford-Smith M, White WD, Newman MF, King S, Winn MP, et al. Acute renal failure following cardiac surgery. Nephrol Dial Transplant. 1999;14(5):1158-62. [MedLine]
24. Yokoyama T, Baumgartner FJ, Gheissari A, Capouya ER, Panagiotides GP, Declusin RJ. Off-pump versus on-pump coronary bypass in high-risk subgroups. Ann Thorac Surg. 2000;70(5):1546-50. [MedLine]
25. Ascione R, Caputo M, Calori G, Lloyd CT, Underwood MJ, Angelini GD. Predictors of atrial fibrillation after conventional and beating heart coronary surgery: Aprospective, randomized study. Circulation. 2000;102(13):1530-5. [MedLine]
26. Shroyer AL, Grover FL, Hattler B, Collins JF, McDonald GO, Kozora E, et al. On-pump versus off-pump coronary-artery bypass surgery. N Engl J Med. 2009;361(19):1827-37. [MedLine]
Article receive on Wednesday, November 11, 2009
 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license