ABSTRACT
INTRODUCTION: The present report describes the technique for "inverted L" upper ministernotomy with central canulation for the treatment of simple congenital cardiopathies and presents the initial results. METHODS: Ten patients (mean age: 7 ± 4.2 years; mean weight 29.1 ± 13.5 kg) were operated on between January 2006 and July 2007. RESULTS: All defects were corrected. No death was observed and no complication that required reintervention occurred. CONCLUSION: The described technique showed to be feasible and safe for the correction of certain congenital cardiopathies, with less surgical trauma, besides the aesthetic benefit and an expectation of diminished thoracic deformity in the future.
RESUMO
INTRODUÇÃO: Descreveremos a técnica com a miniesternotomia superior em "L invertido" com canulação central para o tratamento de cardiopatias congênitas simples e apresenta os resultados iniciais. MÉTODOS: Foram operados 10 pacientes (idade média: 7 ± 4,2 anos; peso médio: 29,1 ± 13,5 kg), entre janeiro de 2006 e julho de 2007. RESULTADOS: Todos os defeitos foram corrigidos sem a necessidade de conversão para esternotomia total. Não ocorreu nenhum óbito ou complicação que necessitasse de reintervenção. CONCLUSÃO: A referida técnica demonstrou ser aplicável e segura na correção de determinadas cardiopatias congênitas com benefício estético e expectativa de menor deformidade torácica no futuro.
INTRODUCTION
The upper mini-sternotomy technique is commonly used in adults as an access route for the treatment of various diseases, especially heart valve. Other access routes are described in the minimally invasive treatment of congenital heart diseases, such as right lateral minithoracotomy[1], transxifoide approach[2] and lower mini-sternotomy[3]. However, the details of the cannulation performed in each of these approaches and is never performed, but merely the authors report only on the central or peripheral cannulation.
The aim of this study is to describe the technique of "inverted L" upper mini-sternotomy with the tactics of central cannulation, which varies according to the defect to be corrected for congenital heart disease.
METHODS
Patients over 18kg, with simple cardiac diseases were selected to perform the first 10 cases of correction of congenital heart diseases by "L" upper ministernotomy with central cannulation during the period of January 2006 to July 2007 at Hospital Pró-Cardíaco. Patient's characteristics, procedures performed and initial results were collected from medical records. The mean age was 7 ± 4.2 years and mean weight of 29.1 ± 13.5kg. The surgeries performed were: five closures of IAC, three closures of IVC, one aortic valve replacement and resection of a subaortic membrane. Three surgeries had combined procedures (Table 1).
Surgical technique
We performed an incision in the skin of 4cm (1cm above the angle of Louis and 3cm below). The sternum was opened longitudinally in "L", using a surgical saw with straight blade. Thus, all the manubrium was opened and the sternum was divided in "L" up to the level of the 4th left intercostal space. After opening the sternum, the thymus was resected.
The arterial cannula was installed in the ascending aorta. The venous cannulation varied with the defect to be corrected. In cases of surgery in which the right atrium needed not to be opened, cannulation was performed with a single triple-stage cannula, installed via the superior vena cava into the inferior vena cava (Figure 1).
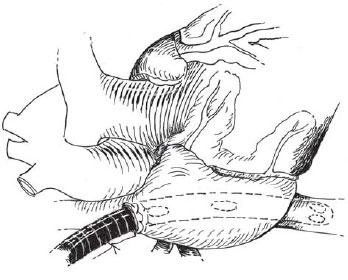
Fig 1. Use of triple stage cannula inserted through the superior vena cava reaching the inferior vena cava
In cases where transtricuspid access was necessary, cannulation of the superior and inferior vena cava were performed through the superior vena cava, so that the cannula for the inferior vena cava did not obstructed the view of the tricuspid valve (Figure 2). This tactic was used in two cases of closure of IVC, one with concomitant tricuspid valve surgery. Finally, in patients who had to open the right atrium, but without the need to transtricuspid approach (patients who underwent IAC), was performed cannulation of the inferior vena cava through the right atrium and cannulation of the superior vena cava through such vein (Figure 3). When necessary lacing the inferior vena cava, this was performed only after starting of CPB.

Fig. 2 - Cannulation of both vena cava through the superior vena cava, allowing transtricuspid procedures

Fig. 3 - Cannulation of the superior vena cava through itself and cannulation of the inferior vena cava through the right atrium
CPB was normothermic with crystalloid perfusate and anterograde hypothermic blood cardioplegia every 20 minutes. Patients weighing over 40 kg were received venous drainage. In all patients CO
2 was used in the field to facilitate the removal of air cavities at the end of CPB.
RESULTS
In all patients it was possible to obtain the total correction of their heart diseases using CPB. The mean CPB time was 36 ± 20 min.
The patient who had undergone aortic valve replacement was directly approached by the ascending aorta. The patient who had undergone ventriculoseptoplasty and resection of subaortic membrane was approached by the pulmonary artery trunk and the ascending aorta. The other patients had the right transatrial approach in the correction of their heart diseases.
There were no surgical complications or need for conversion to full sternotomy. No patient was transfused during hospital stay. The mean hospital stay was 5.5 ± 1.2 days. There were no postoperative complications that required immediate reoperation and no patients had residual shunts. All patients are alive and under outpatient follow-up.
DISCUSSION
Minimally invasive cardiac surgery in adults has gained popularity in recent years and the application of these approaches and tactics in the pediatric population occurred with some restraint. The safety and feasibility of upper ministernotomy have been demonstrated[4,5], and despite increased surgical time, there is no increase in complications[6]. In our country, Rocha e Silva et al.[5] demonstrated the safety of upper ministernotomy to surgically correct the IAC of 20 children and Sampaio et al.[7] reported the aesthetic benefit without deleterious effects in adults also operated to correct the IAC.
The minimally invasive approach should allow the surgeon adequate exposure to the structures to be repaired, safe installation of cardiopulmonary bypass, effective removal of air from the open cavities and control of bleeding sites. However, the descriptions of the various approaches previously published did not include details of the tactic of cannulation, the aim of our study.
This study proposes that the three different surgical tactics exposed are chosen according to the defect to be repaired so as to enable adequate visualization of the structures in question, while allowing ready access to the sites of the purses and their sutures in the case of bleeding. The latter appears to be of paramount importance in the restricted environment such as the mini-incisions. Often, the greatest constraint to cannulation of the inferior vena cava is a right atrium enlarged, besides the risk of bleeding with difficult access at the time of decannulation.
The drainage of the mediastinum should be performed also with the patient still under CPB, therefore, as the outlet site of the drain remains in the subxiphoid region, the uncompressed cavities facilitate the passage of forceps and drain underneath the body below the mediastinum that is intact. With respect to the difficulty of maneuvers to remove air from the cavities, we used the CO
2 bath in the operative field, which displaces the environmental air and replaces it by this gas that is more diffusible in the blood, reducing the risk of gas embolism[8].
CONCLUSION
The technique of cannulation indicated to the type of congenital heart defect to be repaired has shown to be safe and effective in approaches through upper mini-sternotomy, for its comfort and practicability, without compromising the surgical field.
REFERENCES
1. Palma G, Giordano R, Russolillo V, Cioffi S, Palumbo S, Mucerino M, et al. Anterolateral minithoracotomies for the radical correction of congenital heart diseases. Tex Heart Inst J. 2009;36(6):575-9. [MedLine]
2. Barbero-Marcial M, Tanamati C, Jatene MB, Atik E, Jatene AD. Transxiphoid approach without median sternotomy for the repair of atrial septal defects. Ann Thorac Surg. 1998;65(3):771-4. [MedLine]
3. Luo W, Chang C, Chen S. Ministernotomy versus full sternotomy in congenital heart defects: a prospective randomized study. Ann Thorac Surg. 2001;71(2):473-5. [MedLine]
4. Gundry SR, Shattuck OH, Razzouk AJ, del Rio MJ, Sardari FF, Bailey LL. Facile minimally invasive cardiac surgery via ministernotomy. Ann Thorac Surg. 1998;65(4):1100-4. [MedLine]
5. Rocha-e-Silva R, Canêo LF, Lourenço Filho DD, Franchi SM, Afiune CMC, Rodrigues Sobrinho CRM, et al. Correção de comunicação interatrial com cirurgia minimamente invasiva em pacientes pediátricos. Rev Bras Cir Cardiovasc. 1999;14(1):46-50. View article
6. Laussen PC, Bichell DP, McGowan FX, Zurakowski D, DeMaso DR, del Nido PJ. Postoperative recovery in children after minimum versus full-length sternotomy. Ann Thorac Surg. 2000;69(2):591-6. [MedLine]
7. Sampaio LCN, Carvalho JL, Alves CAP, Guedes MAV, Rabelo JR A. Estudo comparativo entre a miniesternotomia em "L" invertido e esternotomia longitudinal total na correção cirúrgica da comunicação interatrial. Rev Bras Cir Cardiovasc. 2005;20(1):46-51. View article
8. Martens S, Neumann K, Sodemann C, Deschka H, Wimmer-Greinecker G, Moritz A. Carbon dioxide field flooding reduces neurologic impairment after open heart surgery. Ann Thorac Surg. 2008;85(2):543-7. [MedLine]
Article receive on Monday, February 22, 2010




 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license