Objective: Acute renal failure following heart surgery is a major complication. The aim of this study was to evaluate if duration of cardiopulmonary bypass (CPB) is an important factor that influences kidney dysfunction.
Methods: One hundred and sixteen patients from a single center referred for heart surgery were evaluated. Demographic factors, clinical data, operative and postoperative variables were evaluated. Serum creatinine and creatinine clearance were calculated until the fifth postoperative day. Acute renal failure was defined as the requirement of dialysis therapy. Patients were divided into two groups, the CPB £70min Group, patients with CPB duration equal to or less than 70 minutes and the CPB³ 90min Group, patients with CPB duration equal to or more than 90 minutes.
Results: The median increases in serum creatinine were 0.18 + 0.41(CPB£70min) and 0.42 + 0.44 (CPB³ 90min - p=0.005). Dialysis was indicated in 1.3% (CPB£70min) and 12.5% (CPB³ 90min - p = 0.018). The odds ratio for dialysis was 1.12 (95% CI; 1.00-1.20) for CPB³ 90min. There was no significant difference in mortality (5.2 versus 7.5%, p = 0.631).
Conclusion: The greatest likelihood of developing kidney failure after heart surgery is observed when CPB is at least 90 minutes, although creatinine clearance was not significantly altered between the groups studied.
Objetivo: A insuficiência renal aguda (IRA) no pós-operatório (PO) de cirurgia cardíaca é complicação grave. O objetivo deste trabalho é avaliar o tempo de circulação extracorpórea (CEC) como fator de risco para IRA.
Método: Foram avaliados 116 pacientes de um único centro, submetidos a cirurgia cardíaca com CEC. Foram avaliados os dados demográficos, características clínicas, variáveis intra e pós-operatórias. A creatinina sérica e o clearance de creatinina foram avaliados até o 5ºPO. IRA foi definida como necessidade de diálise. Os pacientes foram estratificados em dois grupos: grupo CEC£ 70 min e grupo CEC³90min.
Resultados: O aumento médio da creatinina sérica no PO foi 0,18+0,41 no grupo CEC£70min e 0,42+0,44 no grupo CEC³90min (p=0,005). Diálise foi necessária em 1,3% dos pacientes do grupo CEC£70min, e em 12,5% do grupo CEC³90min (p=0,018). O risco relativo para diálise foi 1,12 (IC 95%, 1,00-1,20) para CEC³90min. Não houve diferença para mortalidade (5,2 versus 7,5%, p=0,631).
Conclusão: O desenvolvimento de IRA no pós-operatório de cirurgia cardíaca foi observado em pacientes com tempo de CEC superior a 90 minutos, embora o clearance de creatinina não tenha demonstrado alteração entre os grupos.
INTRODUCTION
Renal dysfunction in the postoperative period of heart surgery is a risk factor for hospital mortality [1,2]. It is a frequent complication in the postoperative period of heart surgery, with a reported incidence of between 1% and 31% [3-7]. The causes for renal dysfunction are multifactorial, with cardiopulmonary bypass (CPB) [8] producing harmful effects for renal function [9]. The non-physiological state of CPB triggers inflammatory cascades and coagulation disorders that change renal function. Patients with renal dysfunction before being submitted to heart surgery present an aggravation of the renal injury which affects long-term survival [10,11].
The aim of the current study is to evaluate the influence of the duration of CPB as a risk factor for renal function alterations.
METHOD
The patients, submitted to heart surgery between January and August 2003 in Hospital de Base, Bauru, Brazil were prospectively and consecutively assessed. The local Ethics Research Committee approved the study. Exclusion criteria were patients with ages less than 18 years old and preoperative renal failure requiring dialysis.
Anesthesia
Induction and maintenance of anesthesia were achieved with sufentanil (0.5 to 0.9µg/kg followed by 0.4 to 0.8µg/kg/h) and midazolam (0.05 to 0.1mg/kg followed by 0.1mg/kg/h). Supplementary isoflurane (0.5 to 1.0%) was used by inhalation and pancuronium bromide (0.1mg/kg) was used as a muscle relaxant.
Monitoring was achieved by continuous electrocardiography of the DII and V5 derivations (MPC-10, TEB, São Paulo, Brazil), with oximetry and capnography (DX-7100, Dixtal, São Paulo, Brazil) in the surgical center. The mean arterial pressure (MAP) obtained by dissection of the radial artery was also monitored (UM62009, Braile Biomédica, São José do Rio Preto, Brazil). Central venous access was provided by venous dissection of the cubital vein or puncture of the right subclavian vein. A digital thermometer (UM62009, Braile Biomédica, São José do Rio Preto, Brazil) was utilized to assess the nasopharyngeal temperature.
Cardiopulmonary bypass
Anticoagulation was achieved by sodium heparin to maintain the activated coagulation time greater than 480 seconds. The CPB circuit was filled with l.8 L lactate Ringers solution, 50 mL 20% mannitol, 10 mL 10% calcium gluconate, 10 mL 10% magnesium sulfate, 500 mg hydrocortisone, 750 mg cefuroxime and 5000 IU of heparin.
Hypothermia at 32ºC was employed during CPB with non-pulsatile arterial blood flow at 2.4 L/min/m2 and a perfusion pressure between 60 and 80 mmHg. Myocardial protection was by intermittent anterograde hyperkalemic blood cardioplegia. Blood transfusions were made during CPB to maintain the hematocrit concentration greater than 17%. The MAP was greater than 65 mmHg during the process to interrupt CPB. The heart was supported by an external pacemaker when the heart frequency dropped to less than 70 bpm. Dobutamine was routinely used at an initial dose of 3 µg/kg/min. When the MAP fell to under 65 mmHg, noradrenalin was administrated. Protamine was utilized (1mg for each 100 IU of heparin). Prophylactic antibiotic therapy was performed using cefuroxime in the first 48 postoperative hours.
Analysed variables and definitions
The variables analysed were age, weight, height, body surface, gender, perfusion duration, anoxia time, type of surgery, lowest hematocrit level during CPB and systemic arterial hypertension, diabetes mellitus, peripheral vascular disease or early acute myocardial infarction.
The serum creatinine (PreCr) was determined before surgery and the postoperative serum creatinine was evaluated in the 1st, 2nd and 5th postoperative days. The highest postoperative creatinine level (PosCr) was defined as the greatest value of serum creatinine determined in the postoperative period. The difference in percentage of creatinine (%"Cr) is defined as the difference between the PreCr and PosCr represented as a percentage of the PreCr.
The estimated creatinine clearance was calculated using the Cockroft-Gault formula: creatinine clearance = (140-age) x weight (kg)/(serum creatinine x 72 [x0.85 for women]).
The creatinine clearance was calculated in the preoperative period and on the 1st, 2nd and 5th postoperative days.
Hemodialysis was performed to treat hyperpotassemia, hypervolaemia, uremia or metabolic acidosis due to acute renal failure (ARF) when necessary.
Stratification of the groups
The patients were divided into two groups using the criteria of Boldt et al. [12]. The CPB£70 Group composed of patients whose CPB duration was less than or equal to 70 minutes and CPBe"90 Group whose CPB duration was equal to or more than 90 minutes.
Statistical analysis
The continuous variables are presented as means ± standard deviation. Ordinal variables are presented as frequencies (%).The chi-squared test or Fishers exact test were utilized to analyze ordinal variables. The groups were compared using the Student t-test for non-matched samples. The two-tailed variance analysis for repeated measurements and post-hoc Bonferroni analysis was used for creatinine clearance analysis within each group. The significance level was established at 5%. The statistical analysis computer program SPSS® version 11.0 (SPSS, Chicago, IL, EUA) was utilized.
RESULTS
One hundred and sixteen patients submitted to on-pump heart surgery in the study period were analyzed with 28 individuals being excluded because the CPB duration was between 70 and 90 minutes.
Fifty-six of the patients were women. For all the patients, the mean age was 56.74 ± 15.37 years and the mean CPB duration was 74.70 ± 29.44 minutes. Ninety-one coronary artery bypass grafting surgeries and 25 valve surgeries were performed.
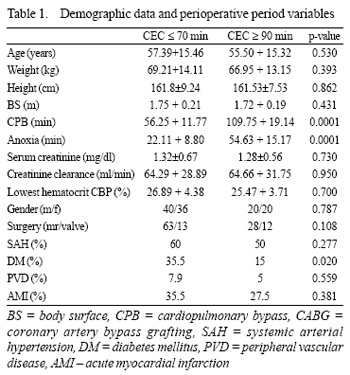
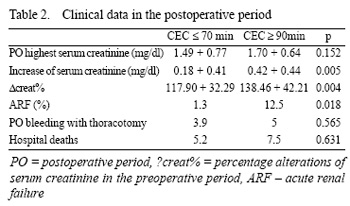
The demographic characteristics and intraoperative variables for both groups are illustrated in Table 1. The postoperative data, shown in Table 2, demonstrate that there was an increase of the serum creatinine of 0.18 ± 0.41 for the CPB£70 Group and 0.42 ± 0.44 for the CPBe"90 Group (p=0.005). The "creat% were 117.90 ± 32.39% and 138.46 ± 42.21% for the CPB£70 and CPBe"90 Groups, respectively (p=0.004).
Figure 1 demonstrates the creatinine clearance according to the day of the surgery for the two groups. There was no statistical difference between the basal creatinine clearance and the postoperative creatinine clearance (p>0.05) for the two groups.
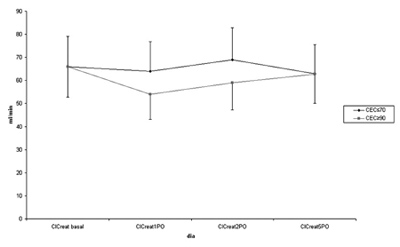
Fig. 1 - Changes in creatinine clearance - ClCreatbasal = preoperative creatinine clearance, ClCrea1PO = creatinine clearance on the first postoperative day, ClCreat2PO = creatinine clearance on the second postoperative day, ClCreat5PO = creatinine clearance on the fifth postoperative day
There was a statistical difference (p=0.018) for ARF between the two groups. The CPBe"90 Group presented an incidence of 12.5% versus 1.3% for the CPB£70 Group. The odds ratio for dialysis was 10.71 (95% CI, 1.20-95.18).
DISCUSSION
This observational study evaluated the influence of the CPB duration on postoperative renal function and in the development of ARF. It was observed that the CPB duration was correlated to postoperative renal dysfunction and to an increase in the need of dialysis.
Advanced age, diabetes mellitus, preoperative renal dysfunction, peripheral vascular disease and body weight are known preoperative risk factors for the development of ARF [6,13-15]. In spite of the widespread use of off-pump heart surgery and of new equipment and drugs to prevent postoperative renal dysfunction, the incidence of renal failure is high and ARF is a challenging problem in heart surgery [16,17].
CPB triggers a significant inflammatory response in heart surgery [18,19], with significantly fewer consequences when the CPB duration is less than 70 minutes [20]. Renal dysfunction in heart surgery evaluated by CPB durations of less than 70 minutes or greater than 90 minutes was assessed for patients with serum creatinine levels of up to 200 mmol/dL (1.7mg/dL) in the preoperative period. In this study, 100 patients were evaluated up to the 2nd postoperative day with changes in renal tubular enzymes being reported, including beta N-acetylgalactosaminidase and glutathione transferases [12]. The evolution of serum creatinine and creatinine clearance in our study was performed until the 5th postoperative day and dialysis was utilized as the criterion for ARF. It is important to note that 12.9% of our patients presented with serum creatine greater than l.7mg/dL.
The deleterious influence of the CPB duration on renal function was observed by the increases in serum creatinine, the variations in serum creatinine and the elevated incidence of dialysis in patients with CPB duration of greater than 90 minutes. The odds ratio was greater than 10 times higher for dialysis between the groups, which is similar to reports published in a multicentric study of more than 2400 patients, which excluded patients with preoperative serum creatinine of more than 2.0 mg/dL. This study reported that, when the CPB duration was more than 3 hours, the risk for ARF is 4 times greater than with a cutoff limit of 2 hours [3].
The longer CPB duration may provoke the increased risk for arterial hypotension with local renal hypoxemia [3,13-14]. Additionally, the longer CPB duration is associated to an increase in proinflammatory cytokines such as TNF-a, IL-1, IL-6 and endotoxins, which may explain tubular injury and the deterioration of the renal function [12,20].
During the CPB, episodes of embolia must be considered as a potential risk factor for renal infarctions and subsequent reductions in renal function [21,22]. Recently it has been discussed whether not using CPB during coronary artery bypass grafting may protect renal function [23]. Sensitive markers of renal tubular injury, such as N-acetyl-ß-D-glucosaminidase, are elevated in patients after CPB [24]. A recent metanalysis demonstrated that dialysis is less common in patients submitted to off-pump coronary artery bypass grafting [16].
There are several limitations in the current study. First, it is an observational study in just one center. Second, the variability of results may lead to errors that did not demonstrate correlation, in spite of being significant. Third, the data presented do not allow the evaluation of the CPB duration, of blood flow and of the perfusion pressure independently. And finally, dialysis may have started after the 5th postoperative day.
CONCLUSION
The development of ARF after postoperative heart surgery is commoner in patients with CPB duration longer than 90 minutes compared to the group with duration shorter than 70 minutes.
REFERENCES
1. Hirose H, Amano A, Yoshida S, Takahashi A, Nagano N, Kohmoto T. Coronary artery bypass grafting in the elderly. Chest. 2000;117(5):1262-70. [
MedLine]
2. Herlitz J, Brandrup-Wognsen G, Karlsson T, Karlson B, Haglid M, Sjoland H. Predictors of death and other cardiac events within 2 years after coronary artery bypass grafting. Cardiology. 1998;90(2):110-4. [
MedLine]
3. Mangano CM, Diamondstone LS, Ramsay JG, Aggarwal A, Herskowitz A, Mangano DT. Renal dysfunction after myocardial revascularization: risk factors, adverse outcomes, and hospital resource utilization. The Multicenter Study of Perioperative Ischemia Research Group. Ann Intern Med. 1998;128(3):194-203. [
MedLine]
4. Provenchere S, Plantefeve G, Hufnagel G, Vicaut E, De Vaumas C, Lecharny JB, et al. Renal dysfunction after cardiac surgery with normothermic cardiopulmonary bypass: incidence, risk factors, and effect on clinical outcome. Anesth Analg. 2003;96(5):1258-64.
5. Chertow GM, Levy EM, Hammermeister KE, Grover F, Daley J. Independent association between acute renal failure and mortality following cardiac surgery. Am J Med. 1998;104(4):343-8. [
MedLine]
6. Chertow GM, Lazarus JM, Christiansen CL, Cook EF, Hammermeister KE, Grover F, et al. Preoperative renal risk stratification. Circulation. 1997;95(4):878-84. [
MedLine]
7. Sear JW. Kidney dysfunction in the postoperative period. Br J Anaesth. 2005;95(1):20-32. [
MedLine]
8. Mangos GJ, Brown MA, Chan WY, Horton D, Trew P, Whitworth JA. Acute renal failure following cardiac surgery: incidence, outcomes and risk factors. Aust N Z J Med. 1995;25(4):284-9. [
MedLine]
9. Byers J, Sladen RN. Renal function and dysfunction. Curr Opin Anesthesiol. 2001;14(6):699-706.
10. Van der Wal RM, van Brussel BL, VoorsAA, Smilde TD, Kelder JC, van Swieten HA, et al. Mild preoperative renal dysfunction as a predictor of long-term clinical outcome after coronary bypass surgery. J Thorac Cardiovasc Surg. 2005,129(2):330-5. [
MedLine]
11. Zakeri R, Freemantle N, Barnett V, Lipkin GW, Bonser RS, Graham TR, et al. Relation between mild renal dysfunction and outcomes after coronary artery bypass grafting. Circulation. 2005;112(9 suppl.):I270-5. [
MedLine]
12. Boldt J, Brenner T, Lehmann A, Suttner SW, Kumle B, Isgro F. Is kidney function altered by the duration of cardiopulmonary bypass? Ann Thorac Surg. 2003;75(3):906-12. [
MedLine]
13. Ostermann ME, Taube D, Morgan CJ, Evans TW. Acute renal failure following cardiopulmonary bypass: a changing picture. Intensive Care Med. 2000;26(5):565-71. [
MedLine]
14. Conlon PJ, Sttaford-Smith M, White WD, Newman MF, King S,Winn MP, et al. Acute renal failure following cardiac surgery. Nephrol Dial Transplant. 1999;14(5):1158-62. [
MedLine]
15. Hammermeister KE, Burchfiel C, Johnson R, Grover FL. Identification of patients at greatest risk for developing major complications at cardiac surgery. Circulation. 1990;82( 5 suppl):IV380-9. [
MedLine]
16. Reston JT, Tregear SJ, Tukelson CM. Meta-analysis of short-term and mid-term outcomes following off-pump coronary artery bypass grafting. Ann Thorac Surg. 2003;76(5):1510-5. [
MedLine]
17. Morgera S, Woydt R, Kern H, Schmutzler M, DeJonge K, Lun A, et al. Low-dose prostacyclin preserves renal function in high-risk patients after coronany bypass surgery. Crit Care Med. 2002;30(1):107-12. [
MedLine]
18. Hall RI, Smith MS, Rocker G. The systemic inflammatory response to cardiopulmonary bypass: pathophysiological, therapeutic and pharmacological considerations. Anesth Analg. 1997;85(4):766-82. [
MedLine]
19. de Vroege R, van Oeveren W, van Klarenbosch J, Stooker W, Huybregts MA, Hack CE, et al. The impact of heparin-coated cardiopulmonary bypass circuits on pulmonary function and the release of inflammatory mediators. Anesth Analg. 2004;98(6):1586-94.
20. Whitten CW, Hill GE, Ivy R, Greilich PE, Lipton JM. Does the duration of cardiopulmonary bypass or aortic cross-clamp, in the absence of blood and/or blood product administration, influence the IL-6 response to cardiac surgery? Anesth Analg. 1998;86(1):28-33. [
MedLine]
21. Bronden B, Dencker M, Allers M, Plaza I, Jonsson H. Differential distribution of lipid microemboli after cardiac surgery. Ann Thorac Surg. 2006;81(2):643-8. [
MedLine]
22. Abu-Omar Y, Balacumaraswami L, Pigott DW, Matthews PM, Taggart DP. Solid and gaseous cerebral microembolization during off-pump, on-pump, and open cardiac surgery procedures. J Thorac Cardiovasc Surg. 2004;127(6):1759-65. [
MedLine]
23. Bucerius J, Gummert JF, Walther T, Schmitt DV, Doll N, Falk V, et al. On-pump versus off-pump coronary artery bypass grafting: impact on postoperative renal failure requiring renal replacement therapy. Ann Thorac Surg. 2004;77(4):1250-6. [
MedLine]
24. Ascione R, Lloyd CT, Underwood MJ, Gomes WJ, Angelini GD. On-pump versus off-pump coronary revascularization: evaluation of renal function. Ann Thorac Surg. 1999;68(2):493-8. [
MedLine]

 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license