Moises Teixeira SobrinhoI; Gabriel Negretti GuiradoI; Marcos Augusto de Moraes SilvaII
DOI: 10.5935/1678-9741.20140021
RESUMO
INTRODUÇÃO: Procedimentos cirúrgicos aumentaram progressivamente nas últimas décadas, inclusive a revascularização do miocárdio(RM).
OBJETIVOS: Demonstrar a importância da fisioterapia no préoperatório de cirurgia cardíaca, em relação à redução do tempo de internação hospitalar, alteração de volumes pulmonares e força muscular respiratória.
MÉTODOS: Foi realizado estudo clínico prospectivo, com pacientes submetidos à revascularização do miocárdio, no Hospital das Clínicas da Universidade Estadual PaulistaUNESP / Botucatu - SP. Foram avaliados 70 pacientes de ambos os gêneros, com faixa etária entre 40 a 75 anos, randomizados por meio programa computadorizado em dois grupos: Grupo I - 35 pacientes de ambos os sexos, que receberam um protocolo de orientação por escrito, exercícios respiratórios e treinamento muscular respiratório no pré-operatório e Grupo II - 35 pacientes de ambos os gêneros, que receberam apenas orientação de rotina da enfermaria no dia da cirurgia. Trabalho foi aprovado pelo Comitê de Ética da Universidade Estadual PaulistaUNESP / Botucatu - SP.
RESULTADOS: A avaliação das pressões inspiratórias máximas evidenciou aumento significativo no terceiro dia pós-operatório e quinto dia pós-operatório para o grupo de intervenção e análise das pressões expiratórias máximas apresentou valores significativos apenas no quinto dia pós-operatório para o grupo intervenção em relação ao grupo controle, observando-se ainda que o grupo submetido ao protocolo de tratamento fisioterapêutico pré-operatório apresentou menor tempo de internação hospitalar.
CONCLUSÃO: A fisioterapia possui papel importante no préoperatório, de modo que indivíduos do grupo intervenção restauraram com maior presteza os parâmetros avaliados antes da cirurgia, além disso, houve diminuição no tempo de internação pós-operatório.
ABSTRACT
INTRODUCTION: The frequency of surgical procedures has increased steadily in recent decades, including the myocardial revascularization.
OBJECTIVES: To demonstrate the importance of physiotherapy in the preoperative period of cardiac surgery in relation to the reduction of hospital stay, changes in lung volumes and respiratory muscle strength.
METHODS: We conducted a prospective study with patients undergoing myocardial revascularization, the Hospital das Clínicas da Universidade Estadual Paulista (UNESP)/Botucatu - SP. We evaluated 70 patients of both genders, aged between 40 and 75 years, subdivided into two groups: group I - 35 patients of both genders, who received a written protocol guidance, breathing exercises and respiratory muscle training in the preoperative period and group II - 35 patients of both genders, who received only orientation of the ward on the day of surgery. This study was approved by the Ethics Committee of UNESP / Botucatu - SP.
RESULTS: Maximal inspiratory pressure in third postoperative day and fifth postoperative day and significant difference between groups, being better for the intervention group. Expiratory pressure was significant in fifth postoperative day in the intervention group compared to controls. The difference of length of hospital stay in the postoperative was found between the groups with shorter hospital stay in the group receiving preoperative therapy.
CONCLUSION: Physical therapy plays an important role in the preoperative period, so that individuals in the intervention group more readily restored the parameters evaluated before surgery, in addition, there was a decrease in the time of the postoperative hospital stay. Thus, it is thought the cost-effectiveness of a program of preoperative physiotherapy.
BMI: Body mass index
CABG: Coronary artery bypass graft surgery
CPB: Cardiopulmonary bypass
Cpm: Cycles per minute
FRC: Functional residual capacity
HDL-cholesterol: High-density lipoprotein cholesterol
ICU: Intensive care unit
LDL-cholesterol: Low-density lipoprotein cholesterol
MEP: Maximal voluntary expiratory
MIP: Measurement of inspiratory pressure
Ml: Milliliters
MR: Myocardium revascularization
PRE: Preoperative period
RV: Residual volume
INTRODUCTION
The cardiac surgery was always clothed with great interest, curiosity, and in some moments, mysticism, and fact understandable when we analyzed the noble importance of this component for the proper functioning of the human body[1].
In recent decades the frequency of surgical procedures has progressively increased, among them the myocardial revascularization (MR). Cardiovascular diseases are a serious public health problem in Brazil[2].
In individuals over 70 years old it is estimated an incidence of 70% of coronary artery disease. As the age is a determinant of coronary atherosclerosis, a growing number of elderly people will be subjected to MR and/or other therapeutic methods[3,4].
The main risk factors that contribute to cardiac diseases are: smoking, high levels of low-density lipoprotein cholesterol (LDL-cholesterol), low level of high-density lipoprotein cholesterol (HDL-cholesterol), diabetes mellitus, systemic hypertension, family history, lifestyle, obesity, sedentary lifestyle and alcohol intake as factors related to atherosclerosis and its clinical manifestations[4,5].
The coronary artery bypass graft surgery (CABG) procedure is indicated for the treatment of ischemic heart disease that is manifested clinically by angina and acute myocardial infarction. The CABG surgery creates a new route for the blood flow and, is used for making a diversion of blood to the portions of the coronary artery distal to the obstructive atherosclerotic involvement[1,5].
With the advancements in care of physical therapy in the preoperative period, surgical techniques, cardiopulmonary bypass (CPB), techniques for myocardial protection, anesthesia and intensive care in the post-operative period, there was a decrease in morbidity and mortality of MR which caused the surgical indication in groups of patients increasingly complex[6,7].
Observing the fact that they are common pulmonary complications of CABG with CPB was justified to carry out this research, there is great importance in properly carrying out evaluations, guidelines and breathing exercises in the period before surgery, and addition, observe the influence and duration of physical therapy assistance in the preoperative period and also its behavior in the postoperative period.
Objective
To demonstrate the importance of the role of physical therapy in the preoperative period of cardiac surgery with extracorporeal circulation, in relation to the respiratory muscle strength, pulmonary volumes and duration of hospital stay after surgery.
METHODS
We performed a prospective clinical study, simple blind, in the period from July 2009 to September 2011 in the ward of cardiac and thoracic surgery at Hospital das Clínicas da Universidade Estadual Paulista (UNESP), Botucatu-SP. We evaluated 70 patients of both gender, age ranging from 40 to 75 years, undergoing CABG with use of CPB, randomized by means of a computerized software (STATTREK) and delivered in a sealed envelope to the physical therapist responsible for primary health care, subdividing into two groups:
- Group I (GI) - Thirty-five patients, undergoing physiotherapeutic intervention, performed under supervision, once a day, during the period that preceded the surgery. The protocol consisted of breathing exercises (breathing in time, deep breathing followed by prolonged expiration, sustained maximal inspiration with apnea of 6 seconds, and diaphragmatic breathing associated with the mobilization of the upper limbs) and breathing exercises with threshold - IMT® (Threshold - IMT® Inspiratory Muscle Trainer, HealthscanProducts Inc.) at an intensity of 40% of the initial MIP with three sets of ten repetitions, respecting two-minute intervals between each series.
- Group II (GII) - thirty-five patients who did not undergo the physical therapy protocol during the preoperative period, receiving only guidelines ward routine.
We included patients of both sexes, aged 40-75 years with coronary artery disease admitted for cardiac surgery with cardiopulmonary bypass (CPB) MR, who agreed to participate in the study. We excluded patients who require the use of intra-aortic balloon, carrying pulmonary pathology, musculoskeletal impairment and severe neurological surgery performed without CPB, emergency surgery, homodynamic instability, and any event that threatens the integrity of patient or the fidelity of the measures analyzed.
Delimitation
All patients were evaluated by the same evaluator (preoperative period - PRE), third postoperative (3PO) and fifth postoperative days (5PO), as well as received physiotherapeutical treatment, according to their needs in the postoperative period by physical therapy team in the hospital and only Group I received physiotherapy in the preoperative period.
The variables evaluated were: body mass index (BMI) - criterion for obesity was a BMI > 30 kg/m2, smoking (patients who smoke or have smoked up to 30 days before surgery and for former smokers those with a prior history, 30 days ago) as well as the time of surgery, CPB, anoxia, IOT (defined by the sum between the anesthesia time and the time that the patient remained with the endotracheal tube in the intensive care unit - ICU), VM (IOT time defined by the time of ventilator disconnection (when the patient was placed in spontaneous ventilation in the T-tube), ICU stay (when the patient arrived in the intensive care unit until discharged to the ward bed) and length of stay in the OP (obtained from the time that the patient arrived in the ICU of the Cardio chest until the time of discharge.) All these data were obtained by means of the daily developments of medical and nursing staff.
The assessment of respiratory muscle strength was obtained by measurement of inspiratory pressure (MIP) and maximal voluntary expiratory (MEP) in the preoperative period (PRE), 3PO and 5PO using analog manometer Commercial Medical® brand spread over -120 to 120 cmH2O equipped with adapter buccal and nasal forceps according to the technique described by Nephew et al. (2008). The MIP measurement was performed from residual volume, and MEP was obtained from total lung capacity. Three measurements were taken technically satisfactory, and if there were more than 20% difference between the measurements, a fourth and even fifth measurement would be performed, being always considered the highest value obtained. The MIP was performed for evaluation of inspiratory muscle strength in three different stages of the study (Pre, 3PO and 5PO), as well as to adjust the training load (40% MIP) using the Threshold - IMT® (Threshold - IMT® inspiratory Muscle Trainer, HealthscanProducts Inc.). A small hole about one millimeter (mm) was performed to prevent occlusion of the glottis and influence of the buccinator muscles during MIP maneuver[9].
Mark Wright 8 display with 35 mm (FERRARIS) in PRE moments, 3PO and 5PO were used to prevent lung volumes. The minute volume was obtained with the patient breathing for a minute for a mouth connected to the spirometer. Tidal volume was obtained indirectly by the relationship between the respiratory rate and minute volume (MV/FR), the two volumes measured in milliliters (ml) and respiratory rate was measured in cycles per minute (cpm) and obtained by direct observation of respiratory cycles during the evaluation of the minute volume[7].
Procedures/treatment
Patients allocated to the GI protocol underwent preoperative physiotherapy consisting of breathing exercises (breathing in time, deep breath and then exhaling long, sustained maximal inspiration with a 6-second apnea, diaphragmatic breathing associated with mobilization of the upper limb, with three series out of ten for each breathing exercise) and breathing exercises with the device Threshold - IMT®. We conducted three sets of ten repetitions with an interval of two minutes each repetition, once a day for every day of hospitalization in the PRE, with a load of 40% of the initial MIP, obtained by manovacuometry[8-10].
The GII patients received only guidelines ward routine before surgery, but postoperatively, both groups performed physical therapy as needed by staff physiotherapy service.
Statistical Analysis
The sample should be made with at least 26 patients who were randomly divided into two study groups (with physical therapy preoperatively and control patients who did not receive preoperative physiotherapy). We considered the level of significance of 5% and a test power in the order of 80% for a minimum difference in the order of two.
The comparison between the groups for age and body mass index (BMI) was performed by Wilcoxon test for independent samples. The smoking variable was analyzed using Goldman to compare proportions within and among multinomial populations. The perfusion, anoxia, mechanical ventilation, anesthesia, surgery, ICU and postoperative hospital stay were obtained in minutes and analyzed by Student's t test or the nonparametric Mann-Whitney test. MIP, MEP, TV, MV and FR were assessed by Friedman tests for comparison of the moments in each group and Mann Whitney test to compare groups at each time, adopting a significance level of 5% probability of rejecting null hypothesis.
This study was approved by the Research Ethics Committee of Universidade Estadual Paulista (UNESP)/Faculty of Medicine of Botucatu (registration number 236/2009, protocol 3223) and all patients signed an informed consent form.
RESULTS
Seventy patients were divided into two groups, Group I composed of 35 patients (12 female and 23 male) and Group II, with 35 patients (six female and 29 male), as illustrated in Figure 1.
No significant difference was noticed between groups for the variables age (GI 58.9±9.53 years and GII 61.4±8.43 years; P=0.26) and body mass index (GI 26.8±3.96 kg/m2 and G II 26±3.86 kg/m2) (Table 1).
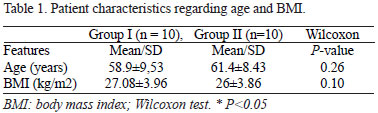
The groups were homogenous concerning presence of active smoking, ex-smokers and nonsmokers, as illustrated in Table 2.
Between the GI and GII, no significant difference regarding the proportion of ex-smokers, smokers and nonsmokers, in other words, the groups were homogeneous as demonstrated below (Table 2).
Maximum Inspiratory Pressure (MIP)
The mean values the for maximum inspiratory pressures evaluated in the preoperative period and 3PO showed no significant difference between groups (P=0.276 and 0.065; respectively), however, we observed greater inspiratory muscle strength for GI in relation to GII in 5PO (P=0.001) (Figure 2).

Maximum Expiratory Pressure (MEP)
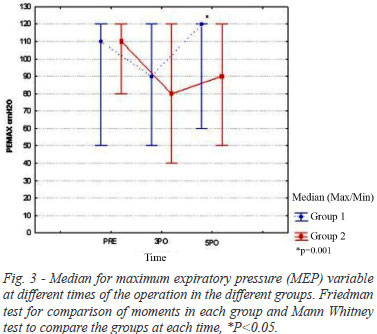
The mean value for the maximum expiratory pressure obtained in the preoperative period for GI was 110 (120/50 cmH2O) and 110 cmH2O (120/80 cmH2O) for GII, not presenting significant difference between groups (P=0.704). However, the values referring MEP measured in the 5PO showed significant difference between groups (P=0.001), as illustrated in Figure 3.
Minute Volume (MV)
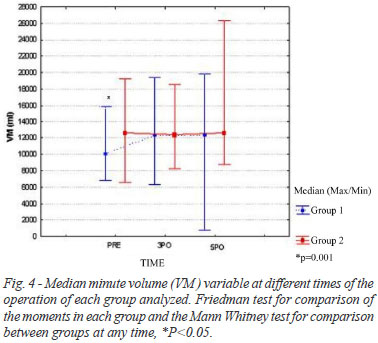
The analysis of the minute volume variable is presented in Figure 4. The values the MV obtained in the preoperative period presented significant difference between groups (GI: 10,110 ml and GII: 12,660 ml; P=0.001). However, these values have not showed significative difference in the 3PO and 5PO (P=0.585 and P=0.329; respectively).
Tidal Volume
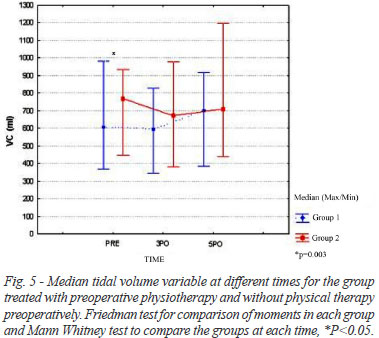
Figure 5 illustrates the analysis of variable volume obtained in the PRE, 3PO and 5PO. Upon PRE, a significant difference between groups was detected (GI: 607 ml and GII: 769 ml, P=0.003), but these values were not significantly different for the 3PO and 5 PO (P=0.059 and P=0.549; respectively).
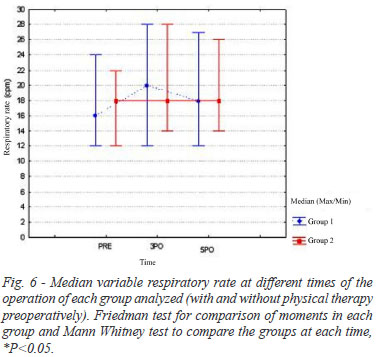
Respiratory rate (RR)
The median refers to the respiratory rate obtained preoperatively for GI and GII showed no significant difference (16 cpm and 18 cpm, respectively, P=0.602). Likewise, the measurements were made in the 5PO 3PO and showed no significant difference between groups (P=0.090 and P=0.886, respectively), as shown in Figure 6.
Infusion time, anoxia, mechanical ventilation, anesthesia, surgery, ICU stay and hospital stay after surgery.
Variables infusion time, anoxia, mechanical ventilation, anesthesia, surgery and ICU stay did not significantly differ between groups, however, significant difference was observed for the length of stay variable in the postoperative period (P=0.001), as shown in Table 3.
DISCUSSION
Studies by Feltrim et al.[10] show that performing preoperative physiotherapy is more effective in reducing respiratory complications in patients with moderate or higher risk than those whose risk was low.
In the present study, we observed no significant difference between the subjects of Group I and Group II as the characteristics (age, BMI, smoking and number of co morbidities), which suggests that the study subjects in both groups were homogeneous.
In the study by Leguisamo et al.[9], with 86 patients undergoing CABG, divided into two groups: the intervention group (44 patients) who were assessed and received physiotherapeutic guidance at least 15 days before surgery. The control group received routine care on the day of hospitalization.
The average MIP between groups showed neither significant difference in the preoperative period nor in the 1PO and 6PO.
In the present study it was observed that there was no significant difference between groups to measure MIP in the preoperative period, but now in times of 3PO and 5PO significant difference between groups was found. Similarly, no significant difference in the amount of MEP preoperatively in the 3PO and between groups. However in 5PO, there was significant difference between the groups with the best values of the group that performed physical therapy before surgery.
Barros et al.[11] evaluated the MIP and MEP in the preoperative period, the first day after surgery and in 38 patients undergoing CABG with CPB who were divided into two groups: 23 patients in group I (respiratory muscle training) and 15 in group II (control). Group I received conventional physiotherapy over respiratory muscle training and Group II the conventional physiotherapy. The authors found that the values obtained for MIP and MEP in hospital discharge were higher in group I.
There was no decrease in maximal respiratory pressures, transdiaphragmatic pressure and diaphragm pressure, indicating weakness of respiratory muscle strength[12,13].
Agreeing with the authors cited above, we observed in the present study, after cardiac surgery, MIP values in GI and GII which decreased in 3PO, however the value of MIP in 5PO increase was observed for GI values compared to those in PRE and 3PO since the GII values remained stable in 3PO. The authors noted the drop in MEP in 3PO in both groups, however, in 5PO MEP has increased in GI. Regarding PRE and 3PO in GII no return value was observed in PRE.
Arcêncio et al.[12] conducted a study with 30 patients, aged 50 years-old and candidates for CABG and / or heart valve, dividing into two groups. Intervention group comprised 15 patients who underwent at least a two weeks inspiratory muscle training using incentive spirometry ("Threshold - IMT®) with 40% charge of the MIP and control group with 15 patients who received only general guidelines. The authors compared the spirometric values before and after training and showed no significant difference in the values of MIP and MEP[14].
Elias et al.[15] studied 42 patients aged 18 to 75 years-old with coronary artery disease, in the pre-and postoperative period, divided into two groups. Intervention group received TMR with Threshold - IMT® and control group received only guidelines. The TMR both pre and post-operative period consisted of three sets of 10 inspiratory exercises once a day for three consecutive days. It was observed that after cardiac surgery there was a significant reduction in MIP and MEP in both groups.
Morsch et al.[13] conducted a study to evaluate 108 patients undergoing elective CABG surgery from April 2006 to February 2007 (preoperatively and postoperatively).
The average values of MIP in the preoperative period were significantly decreased compared to 6 days after the surgery (P<0.001). The authors also observed a significant decrease in the values of MEP obtained on the 6th postoperative day compared to the preoperative period (P<0.001).
Patients with respiratory muscle weakness have higher risk of postoperative pulmonary complications. The respiratory muscle training in the pre-operative may prevent pulmonary complications in patients undergoing thoracic surgery[16]. There may be a reduction of all lung volumes resulting from factors such as diaphragmatic dysfunction, pain, absence of deep breaths, pulmonary changes and ribcage. The functional residual capacity (FRC) decreases because of the reduction of both the residual volume (RV) and expiratory reserve volume. The ventilation is affected by VC reduction by approximately 20%, and the increase in FR[22-24]. The sum of these factors cause changes in the mechanics of respiration, which leads to a shallow breathing pattern of decreased lung volume[13].
Patients undergoing CABG develop mostly PO pulmonary dysfunction with a significant reduction in lung volumes, impairments in respiratory function, decreased lung compliance and increased work of breathing. The reduction in lung volumes and capacities contributes to changes in gas exchange, resulting in hypoxemia[17].
In this study, the VM showed significant difference regarding the groups I and II in the preoperative period but not significant between groups in 3PO. Likewise, the mean value of the VM for the GI 5PO, there was no significant difference in the GII. The mean value of VC in PRE in GI was significant, as the mean value of the VC in GII patients, however in GI and GII we observed in 5PO and 3PO that there was no significant difference. It was observed in GI at different times that the increase of VM will be very likely due to increased FR, since the current VC remained without many changes between different times.
Barros et al.[11] demonstrated a significant decrease in lung volumes in patients undergoing cardiac surgery in the postoperative period.
Carvalho et al.[18] observed a decrease in the values of minute volume and tidal volume measured on the 2nd postoperative day, however, these values showed gradual improvement returning to the values obtained at baseline (preoperative period) at the time of hospital discharge.
In a study, Guizilini et al.[19] evaluated 30 patients with a mean age of 56 years and divided into two groups, group A (n=15) without CPB and group B (n=15) with CPB. All patients underwent pulmonary function. In both groups, there was a decrease in FVC until the fifth postoperative day (P<0.05).
Regarding the respiratory rate in the present study, we can verify that there was an increase in both groups, with a higher peak on the 3rd postoperative day and decreased on the 6th postoperative day, but the respiratory rate did not return to the preoperative values, Carvalho et al.[18] already mentioned above that they concluded in their studies that the mean respiratory frequency had a significant increase between pre and 2nd PO, 3rd PO, decreasing on the 4th postoperative day and increased again on the 5th postoperative day and decreased in hospital discharge, but patients did not return to the preoperative values.
According to the results obtained in this study, we can affirm that there was no significant difference between the groups regarding the time variables: anesthesia, surgery, perfusion, anoxia, mechanical ventilation, intubation. This suggests that the groups were quite homogeneous. As for the time of postoperative hospital stay, there was a decrease of approximately 25 hours, comparing patients who underwent physical therapy before surgery with patients who did not.
In contrast to the findings of this study, Patman et al.[20] performed a randomized study of 236 patients to evaluate the effects of physical therapy interventions performed early versus only started after extubation in patients undergoing cardiac surgery and no significant differences were found in the time of intubation, ICU stay and length of hospital stay between the groups.
However, Celli et al.[21] conducted a study with 172 patients and showed a decrease in length of hospital stay in the group that had received guidelines breathing exercises (9.6±3.2 days) compared to the control group (13±5 days).
Corroborating these findings, as well as those obtained in the present study, Leguisamo et al.[9] performed a prospective study to evaluate the effectiveness of a physiotherapy program start in the preoperative period in reducing the length of hospital stay and showed a significant reduction in length of hospital stay for the intervention group compared to the control group (P<0.05).
These data suggest that physical therapy initiated before surgery can improve conditions of patients, reestablishing early respiratory pressures, reducing the length of stay and decreased hospital costs for the period of hospitalization.
Limitation of the study
The major limitation was the short period of time that patients received preoperative physiotherapy; however, we understand that physiotherapeutic treatment had a relevance even in a short period, so the study may add knowledge of response to therapy performed during intraoperative CABG surgery.
Not performing spirometry can be mentioned as a limitation on the analysis of ventilation parameters, however, due to the conditions offered by our service, we could not perform this evaluation.
On the other hand, the results showed that even with limited time monitoring in the preoperative period and respiratory variables obtained only by respirometry and manometry in physical therapy in the preoperative period, proved to be beneficial for patients undergoing surgery CABG.
We understand that the results may open up new avenues of future research related to the role of physiotherapy in preoperative myocardial revascularization, in addition, further studies should be conducted using tools such as spirometry, to assess and quantify the volume and lung capacity more accurately.
CONCLUSIONS
The physical therapy has an important role in the preoperative period, restoring greater readiness ventilatory parameters of patients undergoing coronary artery bypass grafting with cardiopulmonary bypass, resulting in a decrease in length of hospital stay after surgery.
REFERÊNCIAS
1. Pires AC, Breda JB. Cirurgia cardíaca em adultos. In: Sarmento GJV. Fisioterapia respiratória nos pacientes críticos. Rotinas clínicas. São Paulo: Manole; 2007. p.339-48.
2. Vilas Boas AG, Perondini GB, Sperandio PCA, Kawauchi TS. Fisioterapia e fatores de risco da doença cardiovascular. In: Umeda IIK. Manual de fisioterapia na reabilitação cardiovascular. São Paulo: Manole; 2006. p.1-40.
3. Silva LHF, Nascimento CS, Viotti Jr AP. Revascularização do miocárdio em idosos. Rev Bras Cir Cardiovasc.1997;12(2):132-40. Visualizar artigo
4. Blattner C, Saadi EK. O papel da fisioterapia respiratória precoce na evolução de pacientes submetidos à cirurgia cardíaca com circulação extracorpórea. Fisioter Bras. 2007;8(1):53-6.
5. Polanczyk CA. Fatores de risco cardiovascular no Brasil: os próximos 50 anos. Arq Bras Cardiol. 2005;84(3):199-201. [MedLine]
6. Cavalheiro LV, Chiavegato LD. Avaliação pré-operatória do paciente cardiopata. In: Regenga MM. Fisioterapia em cardiologia. Da Unidade de Terapia Intensiva à reabilitação. São Paulo: Roca; 2000. p.21-9.
7. Hulzebos EH, Helders PJ, Favié NJ, De Bie RA, Brutel de la Riviere A, Van Meeteren NL. Preoperative intensive inspiratory muscle training to prevent postoperative pulmonary complications in high-risk patients undergoing CABG surgery: a randomized clinical trial. JAMA. 2006;296(15):1851-7. [MedLine]
8. Sobrinho MT, Fonseca L, Alves DLM, Silva MAM. Atuação da fisioterapia no pré-operatório de cirurgia cardíaca. Fisioter Especial. 2008;3(2):16-22.
9. Leguisamo CP, KaliI RAK, Furlani AP. A efetividade de uma proposta fisioterapêutica pré-operatória para cirurgia de revascularização do miocárdio. Ver Bras Cir Cardiovasc. 2005;20(2):134-41. Visualizar artigo
10. Feltrim MIZ, Jatene FB, Bernardo WM. Em pacientes de alto risco, submetidos à revascularização do miocárdio, a fisioterapia respiratória pré-operatória previne as complicações pulmonares? Rev. Assoc. Med. Bras. 2007;53(1):8-9. [MedLine]
11. Barros GF, Santos CS, Granado FB, Costa PT, Límaco RP, Gardenghi G. Treinamento muscular respiratório na revascularização do miocárdio. Rev Bras Cir Cardiovasc. 2010;25(4):483-90. [MedLine] Visualizar artigo
12. Arcencio L, Souza MD, Bortolin BS, Fernandes ACM, Rodrigues AJ, Evora PRB. Cuidados pré e pós-operatórios em cirurgia cardiotorácica: uma abordagem fisioterapêutica. Rev Bras Cir Cardiovasc. 2008;23(3):400-10. [MedLine] Visualizar artigo
13. Morsch KT, Leguisamo CP, Camargo MD, Coronel CC, Mattos W, Ortiz LDN, et al. Perfil ventilatório dos pacientes submetidos à cirurgia de revascularização do miocárdio. Rev Bras Cir Cardiovasc 2009;24(2):180-7. [MedLine] Visualizar artigo
14. Siafakas NM, Mitrouska I, Bouros D, Georgopoulos D. Surgery and the respiratory muscles. Thorax. 1999;54(5):458-65. [MedLine]
15. Elias DA, Costa D, Oishi J, Pires VA, Silva MAM. Efeitos do treinamento muscular respiratório no pré e pós-operatório de cirurgia cardíaca. Rev Bras Ter. Intensiva. 2000;12(1):9-18.
16. Barisione G, Rovida S, Gazzaniga GM, Fontana L. Upper abdominal surgery: does a lung function test exist to predict early severe postoperatory respiratory complications? Eur Respir J. 1997;10(6):1301-8. [MedLine]
17. Renault JA, Costa-Val R, Rossetti MR. Fisioterapia respiratória na disfunção pulmonar pós-cirurgia cardíaca. Rev Bras Cir Cardiovasc 2008;23(4):562-9. [MedLine]
18. Carvalho JBR, Ferreira DLMP, Antunes LCO, Carvalho SM, Silva MAM. Evolução das pressões e volumes pulmonares na cirurgia cardíaca. Salusvita. 2003;22(1):85-111.
19. Guizilini S, Gomes WJ, Faresin SM, Bolzan DW, Alves FA, Catani R, et al. Avaliação da função pulmonar em pacientes submetidos à cirurgia de revascularização do miocárdio com e sem circulação extracorpórea. Rev Bras Cir Cardiovasc. 2005;20(3):310-6. Visualizar artigo
20. Patman S, Sanderson D, Blackmore M. Physiotherapy following cardiac surgery: is it necessary during the intubation period? Aust J Physiother. 2001;47(1):7-16. [MedLine]
21. Celli BR, Rodriguez KS, Snider GL. A controlled trial of intermittent positive pressure breathing, incentive spirometry, and deep breathing exercises in preventing pulmonary complications after abdominal surgery. Am Rev Respir Dis. 1984;130(1):12-5. [MedLine]
No financial support.
Authors' roles & responsibilities
MTS: Main author
GNG: Co-author
MAMS: Co-author
Article receive on terça-feira, 2 de abril de 2013
 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license