André Mauricio Souza FernandesI; Gustavo Maltez de AndradeII; Rafael Marcelino OliveiraII; Gabriela Tanajura BiscaiaII; Francisco Farias Borges dos ReisIII; Cristiano Ricardo MacedoIV; André Rodrigues DurãesV; Roque Aras JúniorV
DOI: 10.5935/1678-9741.20140044
RESUMO
OBJETIVO: Descrever a mortalidade hospitalar em pacientes reumáticos submetidos à cirurgia de dupla troca valvar e sua relação com variáveis clínicas e ecocardiográficas.
MÉTODOS: Trata-se de um estudo de corte transversal. Foram estudados pacientes maiores que 18 anos, com valvopatia reumática que foram submetidos à cirurgia de DTV do período de janeiro de 2007 a dezembro de 2011 no Hospital Ana Nery - Salvador - Bahia. A coleta de dados se deu por meio de consulta aos prontuários dos pacientes.
RESULTADOS: Foram estudados 104 pacientes, 60 (57,7%) eram do sexo masculino. A média de idade da população estudada foi de 38,04±14,45 anos. Foram utilizadas 65 próteses biológicas e 38 próteses metálicas. Houve diferença estatisticamente significante entre os grupos comparados, pacientes que obtiveram alta versus pacientes que foram a óbito, em relação às seguintes variáveis: média de idade dos pacientes que receberam alta para casa e foram a óbito, respectivamente (36,30±13,03 vs. 45,35±17,8, P=0,011); média de hemoglobina, (11,10±2,19 vs. 9,22±2,26 g/dL, P=0,002); média do hematócrito, (34,22±5,86 vs. 28,44±6,62%, P<0,001). As classes funcionais III e IV (New York Heart Association) estiveram associadas estatisticamente com a mortalidade (P=0.022).
CONCLUSÃO: Os dados encontrados no estudo apresentam uma população pouco estudada na qual os principais achados foram a média do nível de hemoglobina/hematócrito e classe funcional NYHA. Deve se levar em conta esses dados para a escolha do melhor momento de cirurgia para essa população.
ABSTRACT
OBJECTIVE: To describe the hospital mortality and associated clinical and echocardiographic variables in patients with rheumatic disease who underwent double valve replacement surgery.
METHODS: This is a cross sectional descriptive study of mortality, performed in a referral hospital in Salvador, Bahia. Records from patients with rheumatic disease who underwent double valve replacement surgery during the years 2007-2011 were analyzed.
RESULTS: The studied sample comprises 104 patients and 60 (57.7%) were male. The mean age was 38.04±14.45. Sixty five bioprostheses and 38 mechanical prostheses were used in these patients at the time of surgery. There were statistically significant differences between the two groups, when we analyzed the following variables: the mean age (36.30±13.03 vs. 45.35±17.8 years-old, P=0.011), mean hemoglobin (11.10±2.19 vs. 9.22±2.26 g/dL, P=0.002), mean hematocrit (34.22±5.86 vs. 28.44±6.62%, P<0.001). New York Heart Association functional class III and IV (NYHA) (P=0.022) was statistically associated with mortality.
CONCLUSION: We concluded that the mean hemoglobin/hematocrit level and the NYHA functional class was the major variables associated to the mortality among these patients. Based on these data one may concern about the patient best moment for surgery and the patient hemoglobin level.
AR: Aortic regurgitation
CPB: Cardiopulmonary bypass
MR: Mitral regurgitation
NYHA: New York Heart Association
RF: Rheumatic fever
INTRODUCTION
Rheumatic fever (RF) is a major public health problem, especially in developing countries[1]. Valvular heart disease accounts for a significant portion of cardiovascular hospital admissions in Brazil. Unlike most developed countries, its main cause is RF, responsible for 70% of the cases[2]. During the acute phase of the disease, mitral regurgitation (MR) is the most frequent impairment, followed by aortic regurgitation (AR). Obstructive valve lesions usually do not occur in the early stages of the RF. Recurrence of the acute phase of rheumatic heart disease increases the long term risk of permanent heart injuries and may cause multiple valves lesions[3]. Therefore, patients with rheumatic valve disease tend to have multiple valve lesions: either due to rheumatic valve involvement (stenosis and/or regurgitation) or secondary to ventricle dilation, leading to mitral or tricuspid insufficiency.
Surgical treatment is usually focused at the most severe valve lesion. However, double valve replacement surgery is being performed more frequently nowadays as an attempt to achieve better quality of life and to improve cardiovascular hemodynamics, reducing mortality among these patients[2,4].
Present literature lacks data on clinical or echocardiographic variables associated to in-hospital mortality in rheumatic patients undergoing double valve replacement surgery. Thus, this study aims to assess which of these determinants has impact in this population.
METHODS
This is a cross-sectional retrospective study including all rheumatic patients admitted to the Ana Neri Hospital, Salvador, BA, Brazil, older than 18 years old, that underwent double valve replacement surgery from January 2007 to December 2011. Medical records were reviewed and evaluated for data collection.
The surgical procedure was performed with the patient in the dorsal decubitus position, with a central arterial line to monitor the mean arterial pressure and a central venous line. Median sternotomy and systemic heparinization (0.4 mg/Kg) were performed, followed by cannulation of the ascending aorta for cardioplegia, using hypothermia (32ºC) as a protective strategy, followed by cardiopulmonary bypass (CPB). In the presence of AR, the Aorta was opened and then injected the cardioplegic solution into the coronary ostium. For those patients without AR, the cardioplegic solution was injected directly into the aortic root. Afterwards, the left atrium was opened to perform the mitral and aortic valve replacement, in this respective order, with mechanical or biological prostheses as indicated.
Statistical analysis was performed with SPSS (Version 17.0). Variables were tested for normality using the One Sample Test Kolmogorov-Smirnov and the appropriate statistical test was applied according to its distribution. Continuous variables were described as mean ± standard deviation. Continuous variables with normal distribution were compared using Student's t-test. Asymmetrical distribution variables were analyzed by the Mann-Whitnney test, and their depiction was done by their median, maximum and minimum values. Categorical variables were described by their frequencies and analyzed with the Chi-square test. The level of statistical significance in this study was 5% (P<0.05).
This study was approved by the institutional review board of the Ana Nery Hospital (protocol 59/10).
RESULTS
This study sample was composed by 104 patients who underwent double valve replacement surgery between January 2007 and December 2011. The mean age±standard deviation was 38.04±14.45 years. Clinical and epidemiological characteristics of the study population are shown in Table 1.
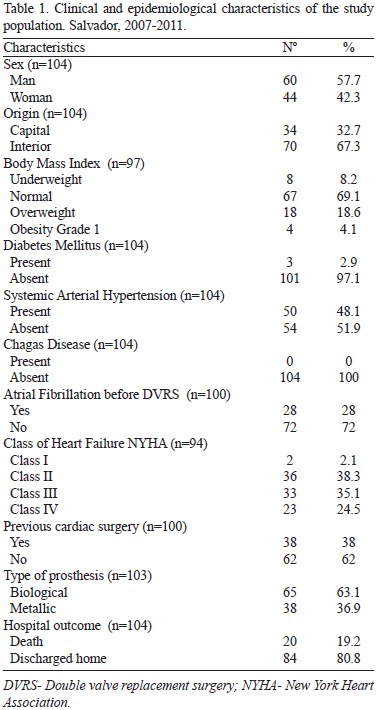
In the study population, 100% of the patients underwent mitral and aortic valve replacement. This surgery was associated with another surgical procedure in only 30.8% of cases. The postoperative hospitalization period ranged from one day to a maximum of 56 days (median 13 days).
The aortic and mitral valves were the most affected in this study population, but the tricuspid and pulmonary valves were also impaired, as follows. Three patients presented mild tricuspid stenosis and one patient had moderate tricuspid stenosis. Two patients presented with mild pulmonary regurgitation and one patient presented with severe insufficiency. No patients presented pulmonary stenosis (Figure 1).

The left atrium was analyzed through echocardiography in 96 patients, ranging from a minimum of 33 mm until 129 mm (median 53 mm). The left atrium size was not associated with hospital mortality (P=0.785). The left ventricle diameters and left ventricular systolic function were also not associated with mortality (Table 2), as well as the degree of valve lesion.
When considering two distinct groups, those who were discharged after surgery and those who died during hospital stay, some statistically significant differences can be noticed: their mean age, respectively (36.30±13.03 vs. 45.35±17.8 years old, P=0.011), mean hemoglobin (11.10±2.19 vs. 9.22±2.26 g/dL, P=0.002); and mean hematocrit (34.22±5.86 vs. 28.44±6.62 %, P<0.001).
Comparisons of gender, city of origin, body mass index, diabetes mellitus, hypertension, atrial fibrillation, class of heart failure, urea, creatinine, previous cardiac surgery and kind of prosthesis between the groups and outcomes are presented in Table 3.
The anoxia time was 129±30 minutes, CPB time was 163±40 minutes, and the total time of surgery was 305±66 minutes. The comparison between the mean anoxia time, CPB time, and total surgical time in both hospital outcomes (death x discharge) were, respectively, 149.17±40.99 and 123.99±24.125 (P=0.001), 185.53±54.597 and 157.34±34.623 (P=0.006), 350.29 and 295.23±56.692±63.983 (P=0.002).
DISCUSSION
Five clinical variables were associated with mortality during the hospitalization of rheumatic patients who underwent double valve replacement surgery: age, hemoglobin, hematocrit, diabetes mellitus and NYHA functional class (New York Heart Association (NYHA) functional classification of heart failure).
The double valve replacement surgery is a risk factor for death independent of preoperative data[5], mainly due to longer duration of surgery, CPB and aortic clamping[2,6,7].
The mortality rate in the study population was 19.2%. Despite elevated when compared to other referral centers in developed countries, different socioeconomic profiles and different access to health between developed and developing countries lead to a comparison limitation[8,9].
In this study population, 59.6% of patients had functional New York Heart Association (NYHA) class III or IV, and 24.5% were in NYHA functional class IV. No other study has a number of patients in a so severe functional class. Studies with low mortality rates show a maximum of 8% of the population with NYHA functional class IV[8,10]. The lowest mortality rate was 0.7% presented by a study which had only 0.5% of patients in NYHA functional class IV[11] and NYHA functional class IV has been presented as an independent risk factor for operative mortality in double valve replacement surgery. Possibly, this is due to an increased release of proinflammatory vasodepressive cytokines in NYHA functional class IV[12]. Patient with advanced heart failure presents a state of chronic inflammation, especially in episodes of decompensation, generating greater degree of difficulty and complications during the surgical technique performing[12].
Preoperative anemia is associated with increased morbidity and mortality among patients undergoing cardiac surgery[13]. Patients with lower hemoglobin levels and preoperative hematocrit are more likely to be transfused, and the use of blood derivates bags is an independent risk factor for mortality and clinical complications such kidney failure, infections, and cardiac complications, pulmonary and neurological in the first thirty postoperative days[14,15]. Studies evaluating mortality in patients undergoing double valve replacement not present data on hemoglobin and hematocrit preoperatively patients[9-11]. This prevents a proper comparison of the results of this study which showed hemoglobin and hematocrit significantly lower in patients who had hospital death. The magnitude of the effect of anemia in the preoperative surgical double valve replacement as well as the optimal management of these patients lack of data in literature.
The mean age of patients who died was 45.35±17.8 years. Age as a mortality predictor in cardiac surgery is described in the literature as one of the main risk factors in most scores[15-22]. However, it should be noted that each score has its own cut-off point from which the surgical risk is established. The EuroSCORE indicates that there is an increased risk of death above 60 years old and one point is given for every 5 additional years[16,17].
A previous study states that patients who were at least 50 years old had higher in-hospital mortality, regardless of the valve surgery performed: aortic or mitral valve replacement, double valve replacement, with or without coronary bypass revascularization[23]. This study shows a higher surgical risk among those with a lower mean age when compared to previously published data, since it is a more complex surgery in critically ill patients. Therefore, existing scores in the literature may not be suitable for predicting the actual risk for this specified population. It is possible that the relative risk with age is established at a lower age range for this group of patients.
Some clinical variables assessed in this study showed no influence on in-hospital mortality. Some are part of major risk scores for mortality risk in heart surgery, such as: female gender, previous cardiac surgery and serum creatinine[16,19]. However, most studies evaluated these variables in all types of cardiac surgeries, not specifically double valve replacement. Otherwise, one study that presented independent risk factors for double valve replacement surgery, also found no influence of the variables mentioned above. It is noteworthy that most of these studies were conducted in major medical centers of the United States and Europe. This demonstrates the need to develop scores of preoperative risk in populations with different socioeconomic characteristics.
Echocardiography's measurements of the left ventricle compared between the two groups of patients (who were discharged home and who died) were not statistically significant, in agreement with previously published data[7]. Because they are variables characteristic of chronic disease, it seems possible that a certain degree of adaptation to the hemodynamic status may occur, with no impact on in-hospital mortality. However, it is necessary to investigate the influence of these variables on morbidity and mortality in a long term way.
The study has quite few limitations. It was a single center study, which may cause bias due to the restricted population size, limiting extrapolation of data to other populations.
CONCLUSION
This study is remarkable for highlighting the value of age, hemoglobin, hematocrit, diabetes mellitus and NYHA functional class as possible variables associated to in-hospital mortality of rheumatic patients undergoing double valve replacement surgery.
A precise cut off point in the hemoglobin value to determine and predict mortality risk should be studied in order to improve the therapeutic management of patients who will undergo double valve replacement. Furthermore, early indication of heart valve surgeries may avoid a delayed procedure at an advanced stage of the disease.
Therefore, new prospective studies in national territory are needed to compare mortality rates between different Brazilian centers, enabling an advance in the management of this disease that still represents a serious public health problem.
REFERÊNCIAS
1. Barbosa PJB, Müller RE, Latado AL, Achutti AC, Ramos AIO, Weksler C, et al. Diretrizes Brasileiras para Diagnóstico, Tratamento e Prevenção da Febre Reumática da Sociedade Brasileira de Cardiologia, da Sociedade Brasileira de Pediatria e da Sociedade Brasileira de Reumatologia. Arq Bras Cardiol. 2009;93(3 supl.4):1-18.
2. Tarasoutchi F, Montera MW, Grinberg M, Barbosa MR, Piñeiro DJ, Sánchez CRM, et al. Diretriz Brasileira de Valvopatias - SBC 2011 / I Diretriz Interamericana de Valvopatias - SIAC 2011. Arq Bras Cardiol. 2011;97(5 supl.3):1-67. [MedLine]
3. Peixoto A, Linhares L, Scherr P, Xavier R, Siqueira SL, Pacheco TJ, et al. Febre reumática: revisão sistemática. Rev Soc Bras Clin Med. 2011;9(3):234-8.
4. Okuyama H, Hashimoto K, Kurosawa H, Tanaka K, Sakamoto Y, Shiratori K. Midterm results of the Manouguian double valve replacement: comparison with standard double valve replacement. J Thorac Cardiovasc Surg. 2005;129(4):869-74. [MedLine]
5. Edwards MB, Taylor KM. Is 30-day mortality an adequate outcome statistic for patients considering heart valve replacement? Ann Thorac Surg. 2003;76(2):482-5.
6. Laffey JG, Boylan JF, Cheng DC. The systemic inflammatory response to cardiac surgery: implications for the anesthesiologist. Anesthesiology. 2002;97(1):215-52. [MedLine]
7. Brandão CMA, Pomerantzeff PMA, Souza LR, Tarasoutchi F, Grimberg M, Oliveira SA. Fatores de risco para mortalidade hospitalar nas reoperações valvares. Rev Bras Cir Cardiovasc. 2002;17(3):236-41. Visualizar artigo
8. Talwar S, Mathur A, Choudhary SK, Singh R, Kumar AS. Aortic valve replacement with mitral valve repair compared with combined aortic and mitral valve replacement. Ann Thorac Surg. 2007;84(4):1219-25. [MedLine]
9. McGonigle N, Jones JM, Sidhu P, Macgowan S. Concomitant mitral valve surgery with aortic valve replacement: a 21-year experience with a single mechanical prosthesis. J Cardiothorac Surg. 2007;2:24. [MedLine]
10. Gillinov AM, Blackstone EH, Cosgrove DM 3rd, White J, Kerr P, Marullo A, et al. Mitral valve repair with aortic valve replacement is superior to double valve replacement. J Thorac Cardiovasc Surg. 2003;125(6):1372-87. [MedLine]
11. Ho HQ, Nguyen VP, Phan KP, Pham NV. Mitral valve repair with aortic valve replacement in rheumatic heart disease. Asian Cardiovasc Thorac Ann. 2004;12(4):341-5. [MedLine]
12. Grossman GB, Rohde LE, Clausell N. Evidence for peripheral production of tumor necrosis factor-α in advanced congestive heart failure. Am J Cardiol. 2001;88(5):578-81. [MedLine]
13. LaPar DJ, Crosby IK, Ailawadi G, Ad N, Choi E, Spiess BD, et al.; Investigators for the Virginia Cardiac Surgery Quality Initiative. Blood product conservation is associated with improved outcomes and reduced costs after cardiac surgery. J Thorac Cardiovasc Surg. 2013;145(3):796-803. [MedLine]
14. Hajjar LA, Vincent JL, Galas FR, Nakamura RE, Silva CM, Santos MH, et al. Transfusion requirements after cardiac surgery: the TRACS randomized controlled trial. JAMA. 2010:304(14);1559-67. [MedLine]
15. Bhaskar B, Dulhunty J, Mullany DV, Fraser JF. Impact of blood product transfusion on short and long-term survival after cardiac surgery: more evidence. Ann Thorac Surg. 2012;94(2):460-7. [MedLine]
16. Roques F, Nashef SA, Michel P, Gauducheau E, de Vincentiis C, Baudet E, et al. Risk factors and outcome in European cardiac surgery: analysis of the EuroSCORE multinational database of 19030 patients. Eur J Cardiothorac Surg. 1999;15(6):816-22.
17. Nashef SA, Roques F, Michel P, Gauducheau E, Lemeshow S, Salamon R. European system for cardiac operative risk evaluation (EuroSCORE). Eur J Cardiothorac Surg. 1999;16(1):9-13. [MedLine]
18. Roques F, Gabrielle F, Michel P, De Vincentiis C, David M, Baudet E. Quality of care in adult heart surgery: proposal for a self-assessment approach based on a French multicenter study. Eur J Cardiothorac Surg. 1995;9(8):433-9.
19. Pons JM, Granados A, Espinas JA, Borras JM, Martin I, Moreno V. Assessing open heart surgery mortality in Catalonia (Spain) through a predictive risk model. Eur J Cardiothorac Surg. 1997;11(3):415-23. [MedLine]
20. Tu JV, Jaglal SB, Naylor CD. Multicenter validation of a risk index for mortality, intensive care unit stay, and overall hospital length of stay after cardiac surgery. Steering Committee of the Provincial Adult Cardiac Care Network of Ontario. Circulation. 1995;91(3):677-84. [MedLine]
21. Parsonnet V, Dean D, Bernstein AD. A method of uniform stratification of risk for evaluating the results of surgery in acquired adult heart disease. Circulation. 1989;79(6 Pt 2):I3-I12. [MedLine]
22. Higgins TL, Estafanous FG, Loop FD, Beck GJ, Blum JM, Paranandi L. Stratification of morbidity and mortality outcome by preoperative risk factors in coronary artery bypass patients. JAMA. 1992;267(17):2344-8. [MedLine]
23. Hannan EL, Racz MJ, Jones RH, Gold JP, Ryan TJ, Hafner JP, et al. Predictors of mortality for patients undergoing cardiac valve replacements in New York State. Ann Thorac Surg. 2000;70(4):1212-8. [MedLine]
No financial support.
Authors’ roles & responsibilities
AMSF: Planning and writing of the manuscript
GMA:Collection and analysis of data and writing of the manuscript; statistical analysis; conception and design of the study; completion of the operations and/or experiments
RMO: Collection and analysis of data
GTB: Collection and analysis of data
FFBR: Interpretation and review of the manuscript
CRM: Interpretation and review of the manuscript
ARD: Review of the manuscript and approval of final version
RAJ: Review of the manuscript and approval of final version
Article receive on domingo, 22 de setembro de 2013
 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license