Hayley MauldonI; Gudrun DiebergII; Neil SmartII; Nicola KingI
DOI: 10.21470/1678-9741-2018-0388
ABSTRACT
Objective: There is currently much debate about which patients would benefit more after on- or off-pump coronary artery bypass grafting (CABG). The aim of this meta-analysis and meta-regression is to investigate the effect of age on short-term clinical outcomes after these approaches.ARDS = Acute respiratory distress syndrome
CABG = Coronary artery bypass grafting
CENTRAL = Cochrane Central Register of Controlled Trials
CI = Confidence intervals
CK-MB = Creatine kinase-muscle/brain
CMA = Comprehensive Meta-Analysis
CPB = Cardiopulmonary bypass
cTnI = Cardiac troponin I
EMBASE = Excerpta Medica dataBASE
GOPCABE = German Off-Pump Coronary Artery Bypass Grafting in Elderly Patients
hs-CRP = High-sensitivity creatine phosphate
ICU = Intensive care unit
MDA = Malondialdehyde
MI = Myocardial infarction
MRI = Magnetic resonance imaging
N/A = Not available.
NR = Not reported
NT-proBNP = N-terminal pro b-type natriuretic peptide
OR = Odds ratio
PRISMA = Preferred Reporting Items for Systematic Reviewsand Meta-analyses
RCT = Randomised controlled trials
UK = United Kingdom
USA = United States of America
INTRODUCTION
Coronary artery bypass grafting (CABG) is the gold standard treatment for patients with complex coronary artery disease. Originally in the 1950s, this surgery was carried out on-pump with cardiopulmonary bypass (CPB); however, this approach can be associated with aortic damage, myocardial ischaemic injury, renal damage, coagulation disorders, and systemic pro-inflammatory responses[1]. In addition, the use of side biting clamps can cause the embolization of atherosclerotic material leading to neurological events. To overcome these problems, off-pump CABG was introduced in the early 1960s, which reduces the amount of aortic manipulation. This approach has problems, the surgery is more technically challenging and there can be limitations associated with graft patency, completeness of revascularisation, and repeat revascularisation requirement[1]. The controversy as to which approach is superior has not been resolved by recent meta-analyses[2-4].
Recently, a meta-analysis was published investigating the long-term outcomes of on- vs. off-pump CABG[5]. The accompanying editorial comment suggested that the discussion should be refocused from comparing each approach overall to investigating precisely which groups of patients would benefit more from which technique[6]. In this respect, one group of interest is elderly people. The age of patients undergoing CABG is continually rising as a result of an increasingly aged population and improved survival rates following diagnoses[7]. For example, Ozen et al.[8] found out that octogenarians continue to have a higher morbidity and mortality rate following CABG than younger populations. Thus, highlighting the need for investigation into the most beneficial techniques within older generations.
Yuksel et al.[9] studied patients with age of >70 years and concluded that there was no significant benefit of either technique in terms of postoperative complications and mortality. However, they did find out that off-pump CABG required significantly less transfused blood products. One of the largest studies to date that included 2,539 participants with 75 years or older was the German Off-Pump Coronary Artery Bypass Grafting in Elderly Patients (GOPCABE) trial[10]. Again, this study found no difference between off-pump and on-pump CABG in elderly patients in terms of mortality, stroke, or MI as well as repeat revascularisation or new renal-replacement therapy after surgery. There have also been three meta-analyses investigating the effects of on- vs. off-pump CABG in patients with age of >70 or >80 years. The results are contradictory, e.g., Altarabsheh et al.[11] found higher rates of stroke following on-pump surgery, whilst Panesar et al.[12] and Zhu et al.[13] found comparable rates. Although elderly people represent an important subset of patients, there is a much broader age range of patients undergoing on- or off-pump CABG. Therefore, the aim of this novel meta-analysis is to investigate the effect of on- vs. off-pump CABG on short-term clinical outcomes across the full age range of patients using both meta-analysis and meta-regression.
METHODS
This analysis was planned in accordance with the current guidelines for performing comprehensive systematic reviews and meta-analysis with meta-regression, including the Preferred Reporting Items for Systematic Reviews and Meta-analyses (PRISMA) guidelines[14].
Search Strategy
To identify potential studies, systematic searches were carried out using the following databases: Excerpta Medica dataBASE (EMBASE), PubMed, Web of Science, and Cochrane Central Register of Controlled Trials (CENTRAL). The search was supplemented by scanning the reference lists of eligible studies. The search strategy included the key concepts of “cardiopulmonary bypass” AND “coronary artery bypass grafting” AND “off pump” OR “on pump” (Supplementary Figure 1). All identified papers were assessed independently by two reviewers (authors HM and NK). A third reviewer (author NS) was consulted to resolve disputes. Searches of published papers were conducted up until July 2018.
Types of Studies Included
This meta-analysis and meta-regression only included randomised controlled trials (RCT) comparing patients undergoing on- vs. off-pump CABG. There were no language restrictions. Animal studies, review papers, and non-randomised controlled trials were excluded. Studies that did not have any of the desired outcome measures or participants who were treated by other modalities, such as percutaneous coronary intervention, were excluded. Incomplete data or data from an already included study were excluded. Studies that included interventions other than off-pump vs. on-pump CABG were excluded. Studies where the mean ages of patients in each group were in different age bands were excluded. Studies where there were no mortality, strokes, or myocardial infarctions (MI) rates, leading to an incalculable odds ratio (OR), were excluded.
Participants/Population
This meta-analysis analysed RCTs of both male and female adult (≥18 years old) patients with coronary artery disease who were undergoing either off- or on-pump CABG. Other treatment modalities and interventions for coronary artery disease, such as percutaneous coronary intervention, were excluded.
Intervention(S), Exposure(S)
This meta-analysis considered all RCTs where patients with stable angina or acute coronary syndrome were treated with either on-pump or off-pump CABG. More specifically, all RCTs where the intervention of carrying out CABG without the use of CPB were performed.
Comparator(S)/Control
The studies in this analysis compared off-pump CABG with a usual care control group receiving on-pump CABG.
Search Results
Our initial search found 2,161 articles. Of these, 2,074 studies were excluded based on title and abstract and 36 studies were excluded as they were not RCTs. Of the RCTs, we excluded 14 studies, because either they had not reported the age of the patients or the mean age of the patients crossed two age bands (Figure 1). Thirty-seven studies were included in our analysis [S1-S37].
Outcome(S)
The primary outcomes analysed were short-term (<30 days) incidences of stroke, mortality, and MI.
Risk of Bias (Quality) Assessment
Risk of bias was assessed using a modification of the Jadad scale[15].
Strategy for Data Synthesis
Data was collected by two authors and independently verified by a third author using pre-established tables. Patients were divided into 5-year age groups beginning at 51-55 and ending at 76-80 and investigated in their individual groups using subgroup analysis. All meta-analysis data was dichotomous and calculated as OR. An OR is a measure of association between an exposure and an outcome. The OR represents the odds that an outcome will occur given a particular exposure, compared to the odds of the outcome occurring in the absence of that exposure. Heterogeneity was quantified using the Cochrane Q test[16], where I2=0% represents no heterogeneity and I2=100% represents considerable heterogeneity. A random-effects inverse variance model was used throughout. All meta-regression data was plotted as the log OR vs. the mean age of the patients in the off-pump group. In these graphs, a negative log OR favours off-pump and a positive log OR favours on-pump. We used a 5% level of significance and 95% confidence intervals (CI). All analyses were carried out in and all figures were produced in Comprehensive Meta-Analysis (CMA) V3.
RESULTS
The 37 studies included in the analysis had an aggregate of 15,324 participants, 7,661 of which had on-pump CABG and 7,663 had off-pump CABG. Table 1 summarises the characteristics of the included studies. Supplementary Table 1 lists the excluded RCTs and reasons for exclusion.
| Age range (years) | Study | N on CPB (off CPB) | Age on CPB (off CPB) | Male % on CPB (off CPB) | All outcome measures |
|---|---|---|---|---|---|
| 51-55 | Iqbal et al.[23], 2014 Pakistan |
100 (100) | 53.5 ± 10 (51.6 ± 10.3) |
NR | Encephalopathy Hospital stay ICU stay MI Mortality Renal failure Stroke Ventilation time |
| 56-60 | Bicer et al.[24], 2014 Turkey |
25 (25) | 56.9 ± 10.7 (57.7 ± 8.4) |
88 (88) | Mortality MDA hs-CRP M30 M65 |
| Gerola et al.[25], 2004 Brazil |
80 (80) | 58.9 ± 8.9 (59.1 ± 9.7) |
68 (64) | Atrial fibrillation CK-MB Hospital stay ICU stay MI Mortality Stroke |
|
| Kobayashi et al.[26] (JOCRI), 2005 Japan |
86 (81) | 59 ± 10 (60 ± 7) |
86 (87) | Atrial fibrillation CK-MB Graft patency ICU stay MI Mortality Neuron specific enolase S-100 protein Stroke Ventilation time |
|
| Penttila et al.[27], 2001 Finland |
11 (11) | 59.2 59.5 |
NR | MI Myocardial markers Myocardial metabolism |
|
| 61-65 | Al-Ruzzeh et al.[28], 2006 UK |
84 (84) | 63.1 ± 9.6 (63.1 ± 11) |
84 (83) | Atrial fibrillation Blood transfusions Graft patency Health-related quality of life Hospital stay ICU stay Mortality Neurocognitive function Stroke Ventilation time |
| Angelini et al.[29], 2002 UK |
BHACAS 1 100 (100) BHACAS 2 101 (100) |
BHACAS 1 61.7 ± 8.6 (62.2 ± 9.6) BHACAS 2 61.2 ± 9.2 (63.8 ± 8.5) |
BHACAS 1 79 (82) BHACAS 2 85 (82) |
Atrial fibrillation MI Mortality Stroke |
|
| Ascione et al.[30], 2000 UK |
100 (100) | 63 (63) | 79 (82) | Atrial fibrillation Hospital stay ICU stay MI Mortality Stroke Ventilation time |
|
| Fattouch et al.[31], 2009 Italy |
65 (63) | 61 ± 18 (63 ± 16) |
77 (61) | cTnI Cardiac contractile function Hospital stay ICU stay Mortality Ventilation time |
|
| Jongman et al.[32], 2014 The Netherlands |
29 (30) | 63 (63) |
90 (90) | Cardiac failure Inflammatory markers Major bleeding Pulmonary embolism Renal failure Stroke |
|
| Khan et al.[33], 2004 UK |
50 (54) | 64.7 | 82 (93) | Blood loss Extubation time Hospital stay ICU stay Infection Low cardiac output MI Mortality Repeat surgery |
|
| Kok et al.[34], 2014 The Netherlands |
29 (30) | 62.6 ± 9.9 (63 ± 9) |
90 (90) | Cerebral oxygenation Cognitive dysfunction Hospital stay ICU stay Stroke |
|
| Légaré et al.[35], 2004 Canada |
150 (150) | 63.7 ± 10 (62.1 ± 10.1) |
79 (81) | Atrial fibrillation Hospital stay ICU stay MI Mortality Stroke Transfusion requirement Ventilation time Wound infection |
|
| Lingaas et al.[36], 2004 Norway |
60 (60) | 65 ± 8.3 64 ± 7.8 |
72 (85) | CPB time Ventilation time Reintubation Bleeding Blood transfusions Atrial fibrillation CK-MB Aspartate aminotransferase Stroke Mortality Mediastinitis Graft patency |
|
| Lund et al.[37], 2003 Norway |
22 (29) | 64 (62) | 73.9 (89.7) | Cerebral blood flow Cerebral MRI Neuropsychologic tests Stroke |
|
| Michaux et al.[38], 2011 Switzerland |
25 (25) | 65 ± 8 (61 ± 9) |
84 (84) | Atrial fibrillation cTnI Hospital stay ICU stay MI Mortality Right ventricular function Ventilation time >12 hours |
|
| Motallebzdah et al.[39], 2004 UK |
20 (15) | 63 (65) | 90 (93) | Cerebral blood flow S100 protein Stroke |
|
| Motallebzdah et al.[40], 2007 UK |
104 (108) | 65.1 ± 0.9 (63.9 ± 0.9) |
91 (87) | Cerebral emboli Mortality Neurocognitive function Stroke |
|
| Nathoe et al.[41] (Octopus), 2003 USA |
139 (142) | 60.8 ± 8.8 61.7 ± 9.2 |
71 (66) | Cost MI Mortality Quality of life Repeat revascularisation Stroke |
|
| Puskas et al.[42] (SMART), 2003 USA |
99 (98) | 62.5 ± 9.5 (62.2 ± 11.1) |
77 (78) | Atrial fibrillation Coagulopathy and transfusion Hospital stay ICU stay MI Mortality Stroke |
|
| Rastan et al.[43], 2005 Germany |
20 (20) | 65.3 ± 3.9 (63 ± 6) |
80 (80) | CK-MB C-reactive protein cTnI Intraoperative myocardial ischaemia MI Mortality NT-proBNP Oxidative stress Stroke |
|
| Sahlman et al.[44], 2003 Finland |
26 (24) | 61.5 ± 8.1 (64 ± 9) |
77 (88) | Extubation time Bleeding CK-MB ICU stay Hospital stay Weight gain Complement C3 C4 Protein carbonyls Wound infection Low cardiac output syndrome Cerebral infarction Oxidative stress markers |
|
| Shroyer et al.[45] (ROOBY), 2009 USA |
1099 (1104) | 62.5 ± 8.5 (63 ± 8.5) |
99 (99) | Cardiac arrest Coma Hospital stay ICU stay Mediastinitis Mortality New mechanical support Renal failure Reoperation Stroke Tracheostomy Ventilation time |
|
| Straka et al. [46] (PRAGUE-4), 2004 Czech Republic |
184 (204) | 62 (63) | 86 (77) | Atrial fibrillation Hospital stay ICU stay MI Mortality Renal failure Stroke Ventilation time |
|
| Vedin et al.[47], 2006 [47] Sweden |
37 (33) | 65 (65) | 84 (78) | Anxiety Cognitive function Depression MI Stroke |
|
| 66-70 | Carrier et al.[48], 2003 Canada |
37 (28) | 70 ± 6 (70 ± 8) |
84 (68) | Mortality MI Stroke Renal insufficiency Respiratory failure/infection Bleeding Blood transfusions ICU stay Hospital stay |
| Lamy et al [49] (CORONARY), 2012 Canada |
2377 (2375) | 67.5 ± 6.9 (67.6 ± 6.7) |
82 (80) | Atrial fibrillation MI Mortality New renal failure Stroke |
|
| Lee et al [50], 2003Hawaii | 30 (30) | 66 ± 11.2 (65.5 ± 9.6) |
73 (80) | Cerebral microemboli Cerebral perfusion Cost Hospital stay Mortality Neurological function Stroke |
|
| Muneretto et al.[51], 2003 Italy |
88 (88) | 66 ± 9 (67 ± 8) |
59 (63) | Abdominal infarction Atrial fibrillation Hospital stay ICU stay MI Mortality Stroke Ventilation time |
|
| Nesher et al.[52], 2006 Israel |
60 (60) | 68 ± 5 (67 ± 1) |
77 (73) | CK-MB cTnI Cytokines Hospital stay Stroke Ventilation time |
|
| Niranjan et al.[53], 2006 UK |
40 (40) | Atrial fibrillation Blood transfusion requirements Clotting tests Hospital stay ICU stay Mortality Postoperative blood loss Stroke Ventilation time |
|||
| 71-75 | Hlavicka et al.[54] (PRAGUE-6), 2016 Czech Republic |
108 (98) | 73.6 ± 7.4 74.7 ± 6.5 |
57.4 (59.2) | MI Mortality Renal failure Stroke |
| Houlind et al.[55] (DOORS), 2012 Denmark |
450 (450) | 75 (75) | 78 (76) | Hospital stay ICU stay MI Mortality Quality of life Stroke |
|
| Lemma et al.[56] (ON-OFF), 2012 Italy |
203 (208) | 73 (74) | 69 (70) | MI Mortality Renal failure Stroke Reoperation for bleeding ARDS |
|
| 76-80 | Diegeler et al. [10] (GOPCABE), 2013 Germany |
1207 (1187) | 78.4 ± 2.9 (78.6 ± 3.0) |
68 (69) | Hospital stay ICU stay MI Mortality New renal-replacement therapy Repeat revascularisation Stroke Ventilation time |
| Møller et al. [57] (BBS), 2010 Denmark |
163 (176) | 75.6 ± 4.9 (76.1 ± 5.2) |
64 (65) | Cardiac arrest with successful resuscitation Coronary reintervention Low cardiac output syndrome MI Mortality Stroke |
|
| Rogers et al.[58] (CRISP), 2014 UK |
53 (53) | 75.7 ± 7.7 (76.4 ± 5.8) |
76 (78) | MI Mortality Prolonged initial ventilation Renal failure Sternal wound dehiscence Stroke |
ARDS=acute respiratory distress syndrome; CK-MB=creatine kinase-muscle/brain; CPB=cardiopulmonary bypass; cTnI=cardiac troponin I; hs-CRP=high-sensitivity creatine phosphate; ICU=intensive care unit; MDA=malondialdehyde; MI=myocardial infarction; MRI=magnetic resonance imaging; NR=not reported; NT-proBNP=N-terminal pro b-type natriuretic peptide; UK=United Kingdom; USA=United States of America
Stroke Incidence
A total of 31 studies investigated the incidence of stroke. The overall OR was 0.770 (95% CI 0.594, 0.998, I2=0%, P=0.048). When the patients were grouped according to age, there were no significant differences in the odds of a stroke occurring in the off-pump group compared to the on-pump group. Fifty-one to 55 years old OR 0.32 (95% CI 0.063, 1.624, I2=0%, P=0.169); 56-60 OR 0.203 (95% CI 0.023, 1.834, I2=0%, P=0.156); 61-65 OR 0.884 (95% CI 0.522, 1.497, I2=0%, P=0.647); 66-70 OR 0.801 (95% CI 0.486, 1.321, I2=0%, P=0.385); 71-75 OR 0.555 (95% CI 0.275, 1.120, I2=0%, P=0.100); and 76-80 OR 0.879 (95% CI 0.552, 1.399, I2=0, P=0.586). See Figure 2 for the forest plot.
Mortality Incidence
A total of 27 studies investigated the mortality incidence. The overall OR was 0.876 (95% CI 0.703, 1.093, I2=0%, P=0.241). There was no significant difference in the odds of mortality occurring in the off-pump group compared to the on-pump group. This was also true when mortality was calculated according to different age groups. Fifty-one to 55 years old OR 0.660 (95% CI 0.108, 4.036, I2=0%, P=0.653); 56-60 OR 0.323 (95% CI 0.050, 2.096, I2=0%, P=0.236); 61-65 OR 1.192 (95% CI 0.717, 1.980, I2=0%, P=0.499); 66-70 OR 0.889 (95% CI 0.634, 1.247, I2=0%, P=0.495); 71-75 OR 0.722 (95% CI 0.368, 1.417, I2=0%, P=0.344); and 76-80 OR 0.793 (95% CI 0.511, 1.231, I2=0%, P=0.301). See Figure 3 for the forest plot.
Myocardial Infarction Incidence
A total of 28 studies investigated the MI incidence. The overall OR was 0.937 (95% CI 0.795, 1.105, I2=0%, P=0.439). There was no difference in the odds of a MI happening in the off-pump group compared to the on-pump group. There was one significant result when patients were grouped according to age band. Fifty-one to 55 years old OR 6.056 (95% CI 1.307, 28.073, I2=0%, P=0.021); 56-60 OR 0.670 (95% CI 0.229, 1.962, I2=0%, P=0.465); 61-65 OR 0.937 (95% CI 0.627, 1.401, I2=0%, P=0.753); 66-70 OR 0.921 (95% CI 0.737, 1.151, I2=0%, P=0.469); 71-75 OR 1.078 (95% CI 0.689, 1.688, I2=70%, P=0.742); and 76-80 OR 0.763 (95% CI 0.467, 1.245, I2=0%, P=0.279). See Figure 4 for the forest plot.
Risk of Bias
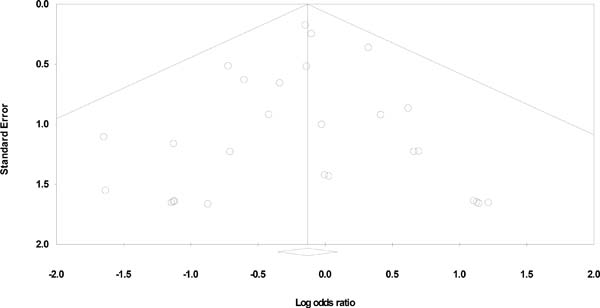
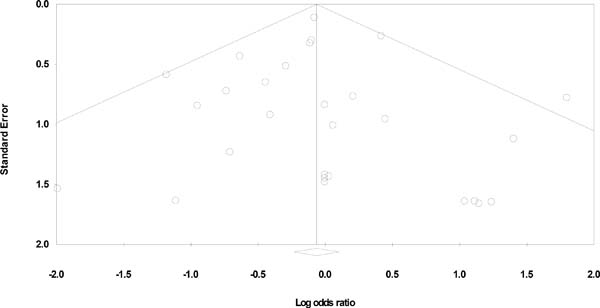
Risk of bias was assessed using a modified Jadad scale with a maximum score of six (Supplementary Table 2). The median score was three. Publication bias was investigated using funnel plots, all of which were symmetrical. The funnel plots with their respective Begg and Mazumdar’s test and Egger’s test statistics can be found in Supplementary Figures 2 to 4.
Meta-Regression Analyses
Figure 5 shows the meta-regression plot graphing the log of the OR for stroke occurrence against the mean age of the patients in the off-pump group. The regression line lies slightly on the side favouring off-pump, although the upper 95% CI lies on the side favouring on-pump. There is no difference in the modality favoured across the different ages measured and no relationship between age and the log OR (Q=0.200, P=0.652).

Figure 6 shows the meta-regression plot graphing the log of the OR for mortality occurrence against the mean age of the patients in the off-pump group. The meta-regression line begins on the side favouring on-pump and then moves to the side favouring off-pump as age increases; however, the 95% CI are equally dispersed either the side of the line of no effect across all the ages. Therefore, there is no difference in the modality favoured across the different ages measured and no relationship between age and the log OR (Q=0.360, P=0.548).
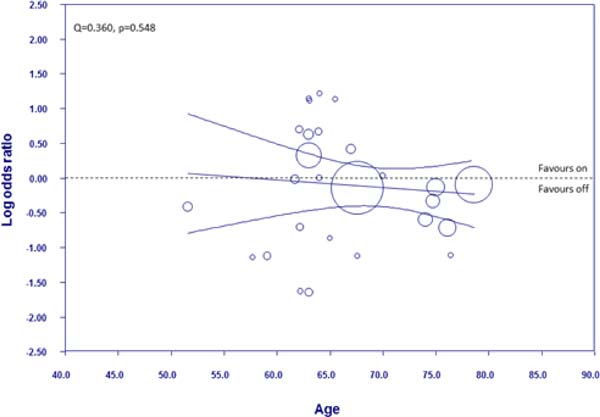
Figure 7 shows the meta-regression plot graphing log OR for myocardial infarction occurrence against the mean age of the patients in the off-pump group. The meta-regression line throughout the graph is close to the line of no effect and the 95% CI are equally dispersed about the line of no effect. Therefore, there is no difference in the modality favoured across the different ages measured and no relationship between age and the log OR (Q=0.540, P=0.464).

DISCUSSION
A recent editorial comment[6] suggests that it is important to investigate which category of patient would benefit more from either off- or on-pump CABG. One of the ways in which patients can be categorised is according to age, with patient vulnerability increasing with increasing age. In this novel meta-analysis and meta-regression, we have investigated the effect of age on short-term clinical outcomes following off- or on-pump surgery. Most of the results showed that when patients were classified according to 5-year age bands there was no difference in the OR for stroke, mortality, or MI occurring in the off-pump group compared to the on-pump group. There was a small significant difference in the odds of stroke incidence overall. This was replicated in the meta-regression plots with off-pump favoured for stroke incidence but no differences in the modality favoured according to the different ages measured.
There was no significant difference in the incidence of mortality or MI between on-pump and off-pump CABG overall, mirroring the results of the four largest trials to date[10,17-19] and the three most recent meta-analyses[2-4]. This has been the general trend in many studies to date. In addition to this, there was no evidence from this meta-analysis to suggest that the increasing age influences the occurrence of these outcomes as no significant difference in the meta-regression was found. The single exception to this is the MI incidence in the 51-55-year age band; however, it should be noted that this result was based on a single trial and clearly more trials investigating this age group are required.
This meta-analysis found a significantly higher occurrence of stroke in the on-pump group overall but no differences in the different age groupings. The overall result concurs with the results of Deppe et al.[3] and Kowalewski et al.[2]. However, they contrast with the four largest trials to date[10,17-19] and the meta-analysis by Dieberg et al.[4]. These findings suggest that if there is a difference in the occurrence of stroke between the off-pump and on-pump groups, then age is not the determining factor. In contrast, other retrospective trials, e.g. Ricci et al.[19] and the meta-analysis by Altarabsheh et al.[11], examined patients older than 80 years and found lower stroke rates in the off-pump CABG patients. There are no RCTs in patients >80 years old.
It is often hypothesised that off-pump CABG should produce a lower incidence rate of stroke as it does not involve aortic manipulation and cross-clamping[1]. But performing the proximal anastomoses during cross-clamping is one possible solution to reduce the aortic manipulation involved in on-pump CABG, thus weakening this hypothesis. There have been many contradictory results as to whether off-pump CABG reduces the risk of stroke and therefore, a definitive answer has not been reached. This could be due to the occurrence of perioperative stroke during CABG being a relatively rare event, meaning that even large trials and meta-analyses lack the weight to support their results. Nevertheless, it is important to continue this evaluation as stroke is a devastating complication of CABG that can lead to a decreased quality of life and increased mortality rate[20]. It is important to link potential preoperative risk factors to the incidence of perioperative stroke in order to improve techniques to reduce its occurrence; however, this meta-analysis suggests that age is not one of them. Another potential risk factor that could be associated with an increased risk of stroke is gender. Puskas et al.[21] found that there is a higher incidence of post-operative stroke within the female population, along with a higher mortality and MI rate. They also found that females are more likely to benefit from off-pump CABG than males. Hence, there are many factors that need to be considered and researched further when comparing off-pump and on-pump CABG.
Study Limitations
Studies scored between two and four out of six on the modified Jadad scale indicating that the median study quality score was moderate (Table 2). There was also some evidence of heterogeneity in many of the studies. Linked to this, not all studies recorded the method of randomisation and there was great variation of methods used between studies. There were also many studies that did not describe dropouts or withdrawals. It is worth noting that it is impossible to use blinding methods within this analysis as surgeons cannot be blinded as to what surgery they are to perform.
One of the most obvious limitations of this study, as in many of the meta-analyses to date that have compared on-pump and off-pump CABG, is the relatively small size of most of the included studies. Only three of the RCTs included more than 1,000 patients[10,17-18] and the next biggest trial included 900 patients[19-22]. Many had less than 100 patients (e.g., S4) and some as little as <20 patients (e.g., S6) within their studies. Removing all studies with <100 patients did not change the overall results, except for the stroke incidence, where the overall significance disappeared. Moreover, the included studies often reported a low occurrence of events in terms of their clinical endpoints, as previously described. This means that most of the included trials were underpowered and endpoints were underestimated, thus the reliability of their results are affected.
In addition, there are many differences in the methods used in each of the included studies. There is variation in the experience of the surgeons and some studies do not state this. For example, one of the larger studies included in this meta-analysis[17] has been criticised for the use of trainee surgeons in their trial who were inexperienced in the off-pump CABG procedure. The CABG procedure itself also varied between studies as some surgeons used hypothermic CPB (e.g., S6) whilst others used normothermic CPB (e.g., S7). Similarly, there were some variations in the method of cardioplegic arrest used for on-pump CABG; some trials used cold blood cardioplegia (e.g., S13) and some used warm blood cardioplegia (e.g., S9).
Another big limitation of this study is the small number of trials with a mean age between 51-55 years or >66 years, meaning that these age groups were underpowered compared to the others. On top of this, there were no trials with a mean age of over 80 years, meaning that this age group was completely omitted from the analysis. In order to gain a better analysis of the effect that age has on the outcomes of on-pump and off-pump CABG, more trials need to be completed, including patients within these age groups.
CONCLUSION
There is continuing debate as to which approach on- or off-pump CABG is superior. There are many ways in which patients could be subdivided to discover which selected groups would benefit most from one approach or another, including age. This meta-analysis and meta-regression has shown that separating patients according to their age up to the age of 80 years does not affect whether off-pump or on-pump should be favoured in these patients.
| Study | Reason |
|---|---|
| Chowdhury et al., 2008 | Mean age crossed over two age groups |
| Covino et al., 2001 | Did not record mean age |
| Formica et al., 2013 | Mean age crossed over two age groups |
| Gulielmos et al., 2000 | Mean age crossed over two age groups |
| Hernandez et al., 2007 | Did not record mean age |
| Hoel et al., 2007 | Did not record mean age |
| Kobayashi et al., 2005 | Mean age crossed over two age groups |
| Kochamba et al., 2000 | Mean age crossed over two age groups |
| Kunes et al., 2007 | Mean age crossed over two age groups |
| Medved et al., 2008 | Mean age crossed over two age groups |
| Paparella et al., 2006 | Did not record mean age |
| Rachwalik et al., 2006 | Mean age crossed over two age groups |
| Rainio et al., 2007 | Mean age crossed over two age groups |
| Raja et al., 2003 | Did not record mean age |

| Study | Randomisation | Methods of randomisation | Methods of blinding described | Method of blinding appropriate | Withdrawals/dropouts described | Other potential bias | Score (out of 6) |
|---|---|---|---|---|---|---|---|
| Al-Ruzzeh et al.[28], 2006 | Yes | Yes | No | N/A | No | No | 3 |
| Angelini et al.[29], 2002 | Yes | Yes | No | N/A | No | Yes | 2 |
| Ascione et al.[30], 2000 | Yes | Yes | No | N/A | No | No | 3 |
| Bicer et al.[24], 2014 | Yes | No | No | N/A | No | No | 2 |
| Carrier et al.[48], 2003 | Yes | No | No | N/A | No | No | 2 |
| Diegeler et al.[10], 2013 | Yes | Yes | No | N/A | Yes | No | 4 |
| Fattouch et al.[31], 2009 | Yes | Yes | No | N/A | No | No | 3 |
| Gerola et al.[25], 2004 | Yes | No | No | N/A | No | No | 2 |
| Hlavicka et al.[54], 2013 | Yes | Yes | No | N/A | Yes | No | 4 |
| Houlind et al. [22], 2012 | Yes | Yes | No | N/A | Yes | No | 4 |
| Iqbal et al.[23], 2014 | Yes | No | No | N/A | No | No | 2 |
| Jongman et al.[32], 2014 | Yes | No | No | N/A | No | No | 2 |
| Khan et al.[33], 2004 | Yes | No | No | N/A | No | No | 2 |
| Kobayashi et al.[26], 2005 | Yes | Yes | No | N/A | No | No | 3 |
| Kok et al.[34], 2014 | Yes | No | No | N/A | Yes | No | 3 |
| Lamy et al.[49], 2012 | Yes | Yes | No | N/A | No | No | 3 |
| Lee et al.[50], 2003 | Yes | Yes | No | N/A | No | No | 3 |
| Légaré et al.[35], 2004 | Yes | Yes | No | N/A | No | Yes | 2 |
| Lemma et al.[56], 2012 | Yes | Yes | No | N/A | Yes | No | 4 |
| Lingaas et al.[36], 2004 | Yes | No | No | N/A | No | No | 2 |
| Lund et al.[37], 2003 | Yes | No | No | N/A | Yes | No | 3 |
| Michaux et al.[38], 2011 | Yes | Yes | No | N/A | No | Yes | 2 |
| Moller et al.[57], 2010 | Yes | Yes | No | N/A | No | Yes | 2 |
| Motallebzadeh et al.[39], 2004 | Yes | Yes | No | N/A | No | No | 3 |
| Motallebzadeh et al.[40], 2007 | Yes | Yes | No | N/A | No | No | 3 |
| Munereto et al.[51], 2003 | Yes | No | No | N/A | No | No | 2 |
| Nathoe et al.[41], 2003 | Yes | Yes | No | N/A | No | No | 3 |
| Nesher et al.[52], 2006 | Yes | Yes | No | N/A | Yes | No | 4 |
| Niranjan et al.[53], 2006 | Yes | Yes | No | N/A | No | No | 3 |
| Penttila et al.[27], 2001 | Yes | No | No | N/A | No | No | 2 |
| Puskas et al.[42], 2003 | Yes | Yes | No | N/A | Yes | Yes | 3 |
| Rastan et al.[43], 2005 | Yes | Yes | No | N/A | No | No | 3 |
| Rogers et al.[58], 2014 | Yes | Yes | No | N/A | Yes | Yes | 3 |
| Sahlman et al.[44], 2003 | Yes | No | No | N/A | No | No | 2 |
| Shroyer et al.[45], 2009 | Yes | Yes | No | N/A | Yes | Yes | 3 |
| Straka et al.[46], 2004 | Yes | Yes | No | N/A | Yes | No | 4 |
| Vedin et al.[47], 2006 | Yes | No | No | N/A | Yes | No | 3 |
REFERENCES
1. Apostolakis A, Papakonstantinou NA, Koniari I. Myocardial revascularization without extracorporeal circulation; why hasn't it convinced yet? Ann Card Anaesth. 2017;20(2):219-55. doi:10.4103/aca.ACA_39_16.
2. Kowalewski M, Pawliszak W, Malvindi PG, Bokszanski MP, Perlinski D, Raffa GM, et al. Off-pump coronary artery bypass grafting improves short-term outcomes in high-risk patients compared with on-pump coronary artery bypass grafting: meta-analysis. J Thorac Cardiovasc Surg. 2016;151(1):60-77. doi:10.1016/j.jtcvs.2015.08.042.
3. Deppe AC, Arbash W, Kuhn EW, Slottosch I, Scherner M, Liakopoulos OJ, et al. Current evidence of coronary artery bypass grafting off-pump versus on-pump: a systematic review with meta-analysis of over 16,900 patients investigated in randomized controlled trials. Eur J Cardiothorac Surg. 2016;49(4):1031-41. discussion 1041. doi:10.1093/ejcts/ezv268.
4. Dieberg G, Smart NA, King N. On- vs. off-pump coronary artery bypass grafting: a systematic review and meta-analysis. Int J Cardiol. 2016;223:201-11. doi:10.1016/j.ijcard.2016.08.250. [MedLine]
5. Smart NA, Dieberg G, King N. Long-term outcomes of on- versus off-pump coronary artery bypass grafting. J Am Coll Cardiol. 2018;71(9):983-91. doi:10.1016/j.jacc.2017.12.049. [MedLine]
6. Adams DH, Chikwe J. On-pump CABG in 2018: still the gold standard. J Am Coll Cardiol. 2018;71(9):992-3. doi:10.1016/j.jacc.2018.01.026. [MedLine]
7. Flather M, Rhee JW, Boothroyd DB, Boersma E, Brooks MM, Carrié D, et al. The effect of age on outcomes of coronary artery bypass surgery compared with balloon angioplasty or bare-metal stent implantation among patients with multivessel coronary disease: a collaborative analysis of individual patient data from 10 randomized trials. J Am Coll Cardiol. 2012;60(21):2150-7. doi:10.1016/j.jacc.2012.08.982.
8. Ozen A, Unal EU, Songur M, Kocabeyoglu SS, Hanedan O, Yilmaz M, et al. Coronary artery bypass grafting in the octogenarians: should we intervene, or leave them be? J Geriatr Cardiol. 2015;12(2):147-52. doi:10.11909/j.issn.1671-5411.2015.02.005.
9. Yuksel A, Yolgosteren A, Kan II, Cayir MC, Velioglu Y, Yalcin M, et al. A comparison of early clinical outcomes of off-pump and on-pump coronary artery bypass grafting surgery in elderly patients. Acta Chir Belg. 2018;118(2):99-104. doi:10.1080/00015458.2017.1383087. [MedLine]
10. Diegeler A, Börgermann J, Kappert U, Breuer M, Böning A, Ursulescu A, et al. Off-pump versus on-pump coronary-artery bypass grafting in elderly patients. N Engl J Med. 2013;368(13):1189-98. doi:10.1056/NEJMoa1211666.
11. Altarabsheh SE, Deo SV, Rababa’h AM, Lim JY, Cho YH, Sharma V, et al. Off-pump coronary artery bypass reduces early stroke in octogenarians: a meta-analysis of 18,000 patients. Ann Thorac Surg. 2015;99(5):1568-75. doi:10.1016/j.athoracsur.2014.12.057.
12. Panesar SS, Athanasiou T, Nair S, Rao C, Jones C, Nicolaou M, et al. Early outcomes in the elderly: a meta-analysis of 4921 patients undergoing coronary artery bypass grafting - comparison between off-pump and on-pump techniques. Heart. 2006;92(12):1808-16. doi:10.1136/hrt.2006.088450.
13. Zhu ZG, Xiong X, Ding JL, Chen J, Li Y, Zhou JL, et al. Comparison of outcomes between off-pump versus on-pump coronary artery bypass surgery in elderly patients: a meta-analysis. Braz J Med Biol Res. 2017;50(3):e5711. doi:10.1590/1414-431X20165711. [MedLine]
14. Moher D, Liberati A, Tetzlaff J, Altman DG. Preferred reporting items for systematic reviews and meta-analyses: the PRISMA statement. Ann Intern Med. 2009;151(4):264-9. doi:10.7326/0003-4819-151-4-200908180-00135.
15. Jadad AR, Moore RA, Carroll D, Jenkinson C, Reynolds DJ, Gavaghan DJ, et al. Assessing the quality of reports of randomized clinical trials: is blinding necessary? Control Clin Trials. 1996;17(1):1-12. doi:10.1016/0197-2456(95)00134-4. [MedLine]
16. Higgins JP, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD,et al. The Cochrane collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928. doi:10.1136/bmj.d5928.
17. Shroyer AL, Grover FL, Hattler B, Collins JF, McDonald GO, Kozora E, et al. On-pump versus off-pump coronary-artery bypass surgery. N Engl J Med. 2009;361(19):1827-37. doi:10.1056/NEJMoa0902905.
18. Lamy A, Devereaux PJ, Prabhakaran D, Taggart DP, Hu S, Paolasso E, et al. Off-pump or on-pump coronary-artery bypass grafting at 30 days. N Engl J Med. 2012;366(16):1489-97. doi:10.1056/NEJMoa1200388.
19. Ricci M, Karamanoukian HL, Abraham R, Von Fricken K, D’Ancona G, Choi S, et al. Stroke in octogenarians undergoing coronary artery surgery with and without cardiopulmonary bypass. Ann Thorac Surg. 2000;69(5):1471-5. doi:10.1016/s0003-4975(00)01238-8.
20. Nicolini F. Stroke after coronary artery bypass grafting: where do we stand? J Heart Stroke. 2017;2(1):1105.
21. Puskas JD, Kilgo PD, Kutner M, Pusca SV, Lattouf O, Guyton RA. Off-pump techniques disproportionately benefit women and narrow the gender disparity in outcomes after coronary artery bypass surgery. Circulation. 2007;116(11 Suppl):I192-9. doi:10.1161/CIRCULATIONAHA.106.678979.
22. Houlind K, Kjeldsen BJ, Madsen SN, Rasmussen BS, Holme SJ, Nielsen PH, et al. On-pump versus off-pump coronary artery bypass surgery in elderly patients: results from the Danish on-pump versus off-pump randomization study. Circulation. 2012;125(20):2431-9. doi:10.1161/CIRCULATIONAHA.111.052571.
23. Iqbal J, Ghaffar A, Shahbaz A, Abid AR. Stroke after coronary artery bypass surgery with and without cardiopulmonary bypass. J Ayub Med Coll Abbottabad. 2014;26(2):123-8.
24. Bicer M, Senturk T, Yanar M, Tutuncu A, Oral AY, Ulukaya E, et al. Effects of off-pump versus on-pump coronary artery bypass grafting: apoptosis, inflammation, and oxidative stress. Heart Surg Forum. 2014;17(5):E271-6. doi:10.1532/HSF98.2014326.
25. Gerola LR, Buffolo E, Jasbik W, Botelho B, Bosco J, Brasil LA, et al. Off-pump versus on-pump myocardial revascularization in low-risk patients with one or two vessel disease: perioperative results in a multicenter randomized controlled trial. Ann Thorac Surg. 2004;77(2):569-73. doi:10.1016/S0003-4975(03)01353-5.
26. Kobayashi J, Tashiro T, Ochi M, Yaku H, Watanabe G, Satoh T, et al. Early outcome of a randomized comparison of off-pump and on-pump multiple arterial coronary revascularisation. Circulation. 2005;112(9 Suppl):I338-43. doi:10.1161/CIRCULATIONAHA.104.524504.
27. Penttilä HJ, Lepojärvi MV, Kiviluoma KT, Kaukoranta PK, Hassinen IE, Peuhkurinen KJ. Myocardial preservation during coronary surgery with and without cardiopulmonary bypass. Ann Thorac Surg. 2001;71(2):565-71. doi:10.1016/s0003-4975(00)02002-6.
28. Al-Ruzzeh S, George S, Bustami M, Wray J, Ilsley C, Athanasiou T, et al. Effect of off-pump coronary artery bypass surgery on clinical, angiographic, neurocognitive, and quality of life outcomes: randomised controlled trial. BMJ. 2006;332(7554):1365. doi:10.1136/bmj.38852.479907.7C.
29. Angelini GD, Taylor FC, Reeves BC, Ascione R. Early and midterm outcome after off-pump and on-pump surgery in beating heart against cardioplegic arrest studies (BHACAS 1 and 2): a pooled analysis of two randomised controlled trials. Lancet 2002;359(9313):1194-9. doi:10.1016/S0140-6736(02)08216-8.
30. Ascione R, Caputo M, Calori G, Lloyd CT, Underwood MJ, Angelini GD. Predictors of atrial fibrillation after conventional and beating heart coronary surgery: a prospective, randomized study. Circulation. 2000;102(13):1530-5. doi:10.1161/01.cir.102.13.1530.
31. Fattouch K, Guccione F, Dioguardi P, Sampognaro R, Corrado E, Caruso M, et al. Off-pump versus on-pump myocardial revascularization in patients with ST-segment elevation myocardial infarction: a randomized trial. J Thorac Cardiovasc Surg. 2009;137(3):650-6; discussion 656-7. doi:10.1016/j.jtcvs.2008.11.033.
32. Jongman RM, Zijlstra JG, Kok WF, van Harten AE, Mariani MA, Moser J, et al. Off-pump CABG surgery reduces systemic inflammation compared with on-pump surgery but does not change systemic endothelial responses: a prospective randomized study. Shock. 2014;42(2):121-8. doi:10.1097/SHK.0000000000000190.
33. Khan NE, De Souza A, Mister R, Flather M, Clague J, Davies S, et al. A randomized comparison of off-pump and on-pump multivessel coronary- artery bypass surgery. N Engl J Med. 2004;350(1):21-8. doi:10.1056/NEJMoa031282.
34. Kok WF, van Harten AE, Koene BM, Mariani MA, Koerts J, Tucha O, et al. A pilot study of cerebral tissue oxygenation and postoperative cognitive dysfunction among patients undergoing coronary artery bypass grafting randomised to surgery with or without cardiopulmonary bypass. Anaesthesia. 2014;69(6):613-22. doi:10.1111/anae.12634.
35. Légaré JF, Buth KJ, King S, Wood J, Sullivan JA, Hancock Friesen C, et al. Coronary bypass surgery performed off pump does not result in lower in-hospital morbidity than coronary artery bypass grafting performed on pump. Circulation. 2004;109(7):887-92. doi:10.1161/01.CIR.0000115943.41814.7D.
36. Lingaas PS, Hol PK, Lundblad R, Rein KA, Tønnesen TI, Svennevig JL, et al. Clinical and angiographic outcome of coronary surgery with and without cardiopulmonary bypass: a prospective randomized trial. Heart Surg Forum. 2004;7(1):37-41. [MedLine]
37. Lund C, Hol PK, Lundblad R, Fosse E, Sundet K, Tennøe B, et al. Comparison of cerebral embolization during off-pump and on-pump coronary artery bypass surgery. Ann Thorac Surg. 2003;76(3):765-70; discussion 770. doi:10.1016/s0003-4975(03)00679-9.
38. Michaux I, Filipovic M, Skarvan K, Bolliger D, Schumann R, Bernet F, et al. A randomized comparison of right ventricular function after on-pump versus off-pump coronary artery bypass graft surgery. J Thorac Cardiovasc Surg. 2011;141(2):361-7. Erratum in: J Thorac Cardiovasc Surg. 2011;142(3):726. doi:10.1016/j.jtcvs.2010.02.023.
39. Motallebzadeh R, Kanagasabay R, Bland JM, Kaski JC, Jahangiri M. S100 protein and its relation to cerebral microemboli in on-pump and off-pump coronary artery bypass surgery. Eur J Cardiothorac Surg. 2004;25(3):409-14. doi:10.1016/j.ejcts.2003.12.018.
40. Motallebzadeh R, Bland JM, Markus HS, Kaski JC, Jahangiri M. Neurocognitive function and cerebral emboli: randomized study of on-pump versus off-pump coronary artery bypass surgery. Ann Thorac Surg. 2007;83(2):475-82. doi:10.1016/j.athoracsur.2006.09.024.
41. Nathoe HM, van Dijk D, Jansen EW, Suyker WJ, Diephuis JC, van Boven WJ, et al. A comparison of on-pump and off-pump coronary bypass surgery in low-risk patients. N Engl J Med. 2003;348(5):394-402. doi:10.1056/NEJMoa021775. [MedLine]
42. Puskas JD, Williams WH, Duke PG, Staples JR, Glas KE, Marshall JJ, et al. Off-pump coronary artery bypass grafting provides complete revascularization with reduced myocardial injury, transfusion requirements, and length of stay: a prospective randomized comparison of two hundred unselected patients undergoing off-pump versus conventional coronary artery bypass grafting. J Thorac Cardiovasc Surg. 2003;125(4):797-808. doi:10.1067/mtc.2003.324. [MedLine]
43. Rastan AJ, Bittner HB, Gummert JF, Walther T, Schewick CV, Girdauskas E, et al. On-pump beating heart versus off-pump coronary artery bypass surgery-evidence of pump-induced myocardial injury. Eur J Cardiothorac Surg. 2005;27(6):1057-64. doi:10.1016/j.ejcts.2005.03.007.
44. Sahlman A, Ahonen J, Nemlander A, Salmenperä M, Eriksson H, Rämö J, et al. Myocardial metabolism on off-pump surgery; a randomized study of 50 cases. Scand Cardiovasc J. 2003;37(4):211-5. doi:10.1080/14017430310001726.
45. Shroyer AL, Grover FL, Hattler B, Collins JF, McDonald GO, Kozora E, et al. On-pump versus off-pump coronary-artery bypass surgery. N Engl J Med. 2009;361(19):1827-37. doi:10.1056/NEJMoa0902905.
46. Straka Z, Widimsky P, Jirasek K, Stros P, Votava J, Vanek T, et al. Off-pump versus on-pump coronary surgery: final results from a prospective randomized study PRAGUE-4. Ann Thorac Surg. 2004;77(3):789-93. doi:10.1016/j.athoracsur.2003.08.039.
47. Vedin J, Nyman H, Ericsson A, Hylander S, Vaage J. Cognitive function after on or off pump coronary artery bypass grafting. Eur J Cardiothorac Surg. 2006;30(2):305-10. doi:10.1016/j.ejcts.2006.03.037.
48. Carrier M, Perault LP, Jeanmart H, Martineau R, Cartier R, Page P. Randomized trial comparing off-pump to on-pump coronary artery bypass grafting in high risk patients. Heart Surg Forum. 2003;6(6):E89-92.
49. Lamy A, Devereaux PJ, Prabhakaran D, Taggart DP, Hu S, Paolasso E, et al. Off-pump or on-pump coronary-artery bypass grafting at 30 days. N Engl J Med. 2012;366(16):1489-97. doi:10.1056/NEJMoa1200388.
50. Lee JD, Lee SJ, Tsushima WT, Yamauchi H, Lau WT, Popper J, et al. Benefits of off-pump bypass on neurologic and clinical morbidity: a prospective randomized trial. Ann Thorac Surg. 2003;76(1):18-25; discussion 25-6. doi:10.1016/s0003-4975(03)00342-4.
51. Muneretto C, Bisleri G, Negri A, Manfredi J, Metra M, Nodari S, et al. Off-pump coronary artery bypass surgery technique for total arterial myocardial revascularization: a prospective randomized study. Ann Thorac Surg. 2003;76(3):778-82; discussion 783. doi:10.1016/s0003-4975(03)00564-2.
52. Nesher N, Frolkis I, Vardi M, Sheinberg N, Bakir I, Caselman F, et al. Higher levels of serum cytokines and myocardial tissue markers during on-pump versus off-pump coronary artery bypass surgery. J Card Surg. 2006;21(4):395-402. doi:10.1111/j.1540-8191.2006.00272.x. [MedLine]
53. Niranjan G, Asimakopoulos G, Karagounis A, Cockerill G, Thompson M, Chandrasekaran V. Effects of cell saver autologous blood transfusion on blood loss and homologous blood transfusion requirements in patients undergoing cardiac surgery on- versus off-cardiopulmonary bypass: a randomised trial. Eur J Cardiothorac Surg. 2006;30(2):271-7. doi:10.1016/j.ejcts.2006.04.042.
54. Hlavicka J, Straka Z, Jelinek S, et al. PPRAGUE-6 trial: off-pump versus on-pump coronary artery bypass graft surgery in patients with EuroSCORE 6. Prague: Third Faculty of Medicine, Charles University Prague; 2013 . Available from:
55. Houlind K, Kjeldsen BJ, Madsen SN, Rasmussen BS, Holme SJ, Nielsen PH, et al. On-pump versus off-pump coronary artery bypass surgery in elderly patients: results from the Danish on-pump versus off-pump randomization study. Circulation. 2012;125(20):2431-9. doi:10.1161/CIRCULATIONAHA.111.052571.
56. Lemma MG, Coscioni E, Tritto FP, Centofanti P, Fondacone C, Salica A, et al. On-pump versus off-pump coronary artery bypass surgery in high-risk patients: operative results of a prospective randomized trial (on-off study). J Thorac Cardiovasc Surg. 2012;143(3):625-31. doi:10.1016/j.jtcvs.2011.11.011.
57. Møller CH, Perko MJ, Lund JT, Andersen LW, Kelbaek H, Madsen JK, et al. No major differences in 30-day outcomes in high-risk patients randomized to off-pump versus on-pump coronary bypass surgery: the best bypass surgery trial. Circulation. 2010;121(4):498-504. doi:10.1161/CIRCULATIONAHA.109.880443. [MedLine]
58. Rogers CA, Pike K, Campbell H, Reeves BC, Angelini GD, Gray A, et al. Coronary artery bypass grafting in high-RISk patients randomised to off- or on-pump surgery: a randomised controlled trial (the CRISP trial). Health Technol Assess. 2014;18(44):v-xx,1-157. doi:10.3310/hta18440.
Authors' roles & responsibilities
HM Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work; final approval of the version to be published.
GD Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work; final approval of the version to be published.
NS Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work; final approval of the version to be published.
NK Substantial contributions to the conception or design of the work; or the acquisition, analysis, or interpretation of data for the work; final approval of the version to be published.
Article receive on Tuesday, November 27, 2018
Article accepted on Thursday, December 27, 2018
 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license