Objective: To determine, even during postoperative period, the confiability of the cardiac index correlate with the data data given by a central atrial venous blood gasometry in patients who underwent cardiac surgery. Methods: From the sample of arterial and venous blood of right atrium gathered in postoperative of cardiac surgery, it was determinated the hemoglobin concentration and the gasometric study through what was observed of the venous oxygen saturation (SvO2) and the partial pressure of oxygen from venous blood gathered in right atrium (PvO2), add to the calculation of artery-venous difference of the oxygen content - radial artery/right atrium (C(a-v)O2). Afterwards, these parameters were compared with the cardiac index determined by thermodilution. Results: There was good correlation between SvO2, C(a-v)O2 of the venous right atrial blood and cardiac index meansured by termodiluition method, with sensibility and especificity good and high positive predict value and negative predict value. The PvO2 demonstrated poor sensibility in the estimative of low output. Conclusion: In cardiac surgery postoperative, the SvO2 and the C(a-v)O2 were safe parameters correlated with low cardiac output. The PvO2 demonstrated poor sensibility in the estimative of low output in postoperative cardiac surgery.
Objetivo: Determinar a confiabilidade em se correlacionar o índice cardíaco com os dados fornecidos pela gasometria do sangue venoso atrial direito em pacientes submetidos à cirurgia cardíaca, durante o período pós-operatório. Métodos: A partir das amostras de sangue arterial e venoso do átrio direito, colhidas no pós-operatório de cirurgia cardíaca, foram determinados os parâmetros de oxigênio do sangue venoso do átrio direito. Estes parâmetros foram então comparados com o índice cardíaco determinado pela termodiluição. Resultados: Houve boa correlação entre a saturação de oxigênio do sangue venoso do átrio direito (SvO2), diferença artério-venosa do conteúdo de oxigênio do sangue colhido no átrio direito e o índice cardíaco aferido pela termodiluição, com boa sensibilidade e especificidade e alto valor preditivo positivo e negativo. A pressão do sangue do átrio direito (PvO2) apresentou baixa sensibilidade na estimativa de baixo débito cardíaco. Conclusão: No pós-operatório de cirurgia cardíaca, a SvO2 e a diferença artério-venosa do conteúdo de oxigênio (C(a-v)O2) apresentaram-se como parâmetros confiáveis correlacionados a baixo débito cardíaco. A PvO2 foi pouco sensível no diagnóstico de baixo débito no pós-operatório de cirurgia cardíaca.
INTRODUCTION
The cardiac output monitoring has been incorporated into clinical practice, from studies by Swan et al.[1] in 1970, with the idealization of a pulmonary artery catheter, which allowed the measurement of cardiac output by thermodilution after improvement in their structure, described by Forrester et al.[2] in 1972. However, many criticisms have arisen about the risks and complications of using this apparatus, and that its use would increase the morbidity and mortality for patients[3]. But according to some recently published trials, effective studies are needed to determine the correct protocols to be followed and the groups of patients who may benefit from the use of Swan-Ganz® catheter[4-6].
New parameters have emerged as alternatives to cardiac function monitoring, such as the oxygen saturation of mixed venous blood, which according to studies by Krauss et al.[7] and Perner et al.[8] are well correlated with the values of cardiac output. Because of the greater difficulty in obtaining the blood samples from the pulmonary artery, the blood collected from the right atrium has been used with good correlation with mixed venous blood[9].
OBJECTIVE
This study aims to determine the reliability to correlate low cardiac output with the data provided by gasometry of venous blood collected from the right atrium in patients undergoing cardiac surgery during the postoperative period.
METHODS
Ten patients with heart valve disease referred for heart surgery were selected for the study, six males and four females, age ranging from 30 and 70 years (mean=50.4 years). On echocardiography, these patients presented signs of both heart failure and ejection fraction lower than 40% (mean = 36.2%±4.2).
Individuals who had other concurrent diseases, such as chronic obstructive pulmonary disease, hematological disorders, and liver and kidney diseases have been excluded. The existence of anatomical abnormalities that would provide a mixture of intracardiac blood and moderate and/or severe tricuspid insufficiency was also an exclusion criterion.
One hour prior to the surgical procedure, a Swan-Ganz® catheter was inserted in each patient in the right pulmonary artery, at Wedge zone II, and a central venous catheter was inserted in the right atrium, both positioned with the assistance of radioscopy. A plastic catheter was also introduced in the radial artery in order to obtain continuous monitoring of mean arterial pressure and arterial blood samples for arterial blood gasometry study. All patients underwent cardiac surgery (four mitral valve repairs, one implantation of aortic valve prosthesis, and five implants of mitral valve protheses) performed by the same team of the Cardiovascular Surgery Service from the University Hospital at Federal University of Mato Grosso do Sul. Cardiopulmonary bypass support with similar technique and apparatus was used in all the cases.
In the postoperative period, the patients were initially kept under mechanical ventilation with a multiprocessor pressure-controlled respirator. They were also monitored by pulse oximetry, capnography, and ECG. Bedside chest radiography confirmed the correct placement of catheters.
Arterial and right atrium blood samples were collected simultaneously from each patient, according to the need of hemodynamic and blood gasometry assessment. A total of ten samples from each patient were collected. The following parameters were determined: plasma hemoglobin (Hb) concentration, arterial oxygen saturation (SaO2), right atrium mixed venous oxygen saturation (SvO2), partial pressure of arterial oxygen (PaO2), and partial pressure of right atrium venous oxygen (PvO2 ).
Concurrently, with the collection of blood samples, the cardiac index was measured by thermodilution method, using Swan-Ganz® catheter, and considering as the final value, the average of three consecutive measurements, since there were no differences greater than 10% between them. The measurement of this parameter during the period of mechanical ventilation was performed in the final phase of expiration.
Data provided by the analysis of the collected blood samples allowed the calculation of the arteriovenous difference of oxygen content (C(a-v)O2), according to the equations represented as follows:
CaO
2 = SaO
2 x Hb x 1.39 + 0.0031 x PaO
2
CvO
2 = SvO
2 x Hb x 1.39 + 0.0031 x PvO
2
C(a-v)O
2 = CaO
2 - CvO
2
Where: CaO
2 represents the oxygen content of the arterial blood, and CvO
2 the oxygen content of venous blood of the right atrium. The value 1.39 represents the amount of oxygen in milliliters that can be delivered by one gram of hemoglobin, and 0.0031 is the solubility of oxygen in the plasma.
The results were statistically analyzed using the linear correlation coefficient (r) and the Student's t test, and p equal to 5% was considered significant. Diagnostic tests in relation to the gold standard (thermodilution) were applied to assess the capacity of a given parameter to estimate the cardiac index (CI). It was assumed that SvO
2 < 60%, PvO
2 < 28mmHg, C(a-v)O
2 = 7.0mL/%, and CI < 2.0L/min/m
2 represented a low cardiac output clinic al situation.
The study was approved by the Ethical Committee of the UFMS University Hospital, and the free informed consent was obtained from each patient.
RESULTS
The SvO
2, PvO
2 and C(a-v)O
2 showed a linear correlation (r) with the CI of 0.80, 0.79, and -0.84, respectively, all values of P < 0.05.
Table 1 shows the comparison between SvO2, PvO2 and C(a-v)O
2 with CI, considering the linear correlation (r) and Student's
t test.
Figures 1, 2, and 3 represent graphically these correlations.
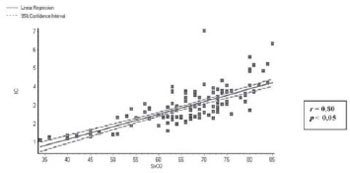
Fig. 1 - Correlation between oxygen saturation of blood from the right atrium (SvO2) and cardiac index (CI)
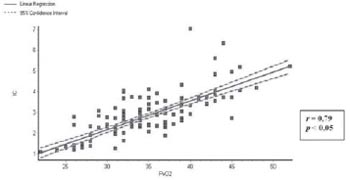
Fig. 2 - Correlation between partial pressure of oxygen in the blood of the right atrium (PvO2) and cardiac index (CI)
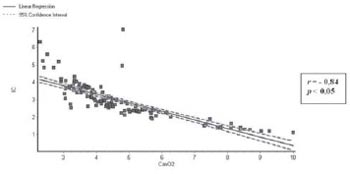
Fig. 3 - Correlation between the difference in arteriovenous content of oxygen (CavO2) and cardiac index (CI)
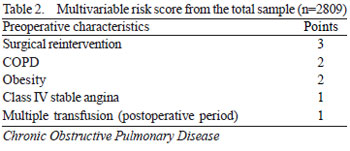
Table 2 shows the results of diagnostic tests performed for each parameter studied in relation to the thermodilution method, considered the gold standard for determination of cardiac index.
SvO
2 < 60% presented 8% of the false positive results and 2% of the false negative results, and consequently, lower specificity; however, SvO
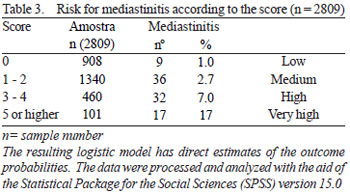
2 < 55% as an indicator of low cardiac output presented a better diagnosis profile, as shown in Table 3, with only 2.6% and 2% of false positive and false negative results, respectively.
DISCUSSION
The use of oxygen saturation in the blood of the right atrium (SvO2
RA) as a substitute for mixed venous blood (SvO2
PA) has been used to estimate the tissue oxygenation in the cardiac output due to the greater facility to obtain it.
Martin et al.[10] studying patients in septic shock, reported that the values of oxygen saturation of venous blood collected in the central superior vena cava (SvO2
svc) and SvO2
PA were not overlapped. According to Stone et al.[11] and Smith et al.[12], the redistribution of blood flow in favor of cerebral perfusion under conditions of low cardiac output would be responsible for the difference found among the values of SvO2
cs and SvO2
AD, and the estimate of SvO2
AP. Thus, the oxygen saturation of blood from the superior vena cava would have become greater than the blood of the inferior vena cava due to the reduced perfusion of splanchnic organs; therefore, the values of SvO2
AD would better represent the values of SvO2
AP compared with the data provided by SvO2
cs.
These data explain the findings by Scheinman et al.[13] in 1969, studying patients with acute myocardial infarction, who reported a greater difference between the mean values of SvO2cs and SvO2
AP for patients with clinical evidence of left ventricular failure or shock, different from that observed in patients clinically stable.
Martin et al.[14] suggested the maintenance of SvO2
AP values greater than 60% would be an important parameter to guide therapy in critically ill patients from the hemodynamic standpoint.
In relation to the cardiac index, which in the final analysis, could express the hemodynamic status of the patient, the literature shows large discrepancies in the correlations between this parameter and the oxygen saturation of central venous blood.
Krauss et al.[7] reported a good correlation (r=0.78) between mixed venous oxygen saturation and cardiac index in patients undergoing cardiac or pulmonary surgery. Waller et al.[15], studying patients undergoing coronary artery bypass grafting, through continuous monitoring of SvO2AP using fiber optic catheters, reported good correlation between changes in values of SvO2
AP and CI, with r=0.69, when there was a variation increase or decrease of 5% or more in SvO2
AP value.
Jamieson et al.[16], studying patients undergoing cardiac surgery, showed a good correlation between the CI and SvO2
AP, with r=0.95, and SvO2
AP values greater than 65% corresponded to a satisfactory cardiac index. Other authors have presented different results, in which they had obtained little correlation between the extent of SvO2
AP and CI[17-19].
Jain et al.[20] attributed the high variability of results reported in the literature to different metabolic and hemodynamic profile of the patients studied. As these authors described, the correlation between SvO2
AP and cardiac output does not occur linearly as suggested by the authors mentioned above. These authors showed that in the group of patients with CI < 2L/min/m2 and SvO2
AP < 55%, the correlation was good (r=0.87), differing from the lowest correlation (r=0.42) found in the most hemodynamically stable group of patients with CI > 2L/min/m2 and SvO2AP > 55%. These authors also considered the homogeneity of the group of patients, considering the concentration of hemoglobin (Hb) and oxygen consumption (VO2), as an important factor responsible for the variability of the correlation between CI and SvO2
AP.
The results obtained by this study corroborate the above statements, once in the patients with greater hemodynamic instability the correlation between the CI and SvO
2 was higher. However, the threshold value of 60% of SVO
2 determined almost 8% of false positive results, which was reduced to only 2.6% when considering SvO
2 less than 55% as indicative of low output, promoting improvement in sensitivity and especially in specificity, with greater positive predictive value. This diagnostic profile of SVO
2 certifies its routine use in the postoperative period as an additional and important parameter in the hemodynamic analysis of patients, and it may guide procedures, such as drug weaning process and infusion volumes, slowing, or even preventing in some cases, the use of Swan-Ganz® catheter.
Sommers et al.[21], studying patients undergoing coronary artery bypass grafting, most specifically the first eight hours postoperatively, reported better correlation between PvO2
AP and CI, with a mean value of r=0.6502, compared to the SvO2
AP and CI with r=0.424. These results were attributed to the instability of the patients during the immediate postoperative period and the likely variability of oxygen consumption (VO2) by the patient during this period.
Kandel et al.[22] reported that it would be preferable to use SvO2
AP instead of PvO2
AP to monitor tissue oxygenation, once changes in SvO2
AP can be used to identify disturbances in oxygen transport in an earlier stage, thus allowing a better response to disso, a SvO2
AP seria determinada apenas pelos componentes do sistema de transporte de oxigênio, ou seja, DC, Hb, SaO
2 e VO
2, enquanto a PvO2
AP pode ser alterada na presença de qualquer fator que cause desvios na curva de dissociação da hemoglobina sem necessariamente existir distúrbios no transporte de oxigênio.the treatment. In addition, SvO2
AP would be determined only by the system components of oxygen transport, i.e., CO, Hb, SaO
2 and VO
2, while PvO2
AP can be altered by any factor that causes deviations in the dissociation curve of hemoglobin without having necessarily disturbances in oxygen transport.
In our study, despite the good correlation found between the PvO2 and CI (r=0.79), this parameter was less sensitive (sensitivity of 65.7% ± 15.7) in diagnosing low cardiac output compared to SvO2, agreeing with the results of Kandel et al.[22].
Theoretically, the arteriovenous oxygen content difference (C(a-v)O2) has a better performance when correlated to the cardiac output, compared to SvO2, because to its calculation it is used a measure of two other determinant factors (SaO2 and Hb) of the oxygen transport. This argumentation was corroborated by the studies of Buheitel et al.[23]. When examining children in the postoperative period of congenital cardiac surgery, they found a better correlation between cardiac index and CaO2/C(a-v)O2 ratio, in comparison to SvO2AP.
Valentine et al.[24], studying patients suffering from acute myocardial infarction, showed that the average C(a-v)O2 was higher, 7.2mL/100mL in patients who had radiological signs of pulmonary edema when compared with the 6.6mL/100mL in the group that did not present these radiological changes. Of the 19 patients studied by these authors, five died, and of these, only one did not have C(a-v)O2 greater than 7.5mL/100 mL.
Tahvanainen et al.[25] described a good relationship between the oxygen arteriovenous difference, considering the blood from the right atrium and pulmonary artery, as r=0.89 and p < 0.001, as well as Furqan et al.[26], but in a group of postoperative pediatric patients for congenital heart disease repair.
The arteriovenous oxygen content difference (C(a-v)O2) showed the best diagnostic profile among the parameters studied, showing a correlation of -0.84 with the cardiac index, specificity of 100%, sensitivity of 94.1% ± 7.9, and accuracy of 98.7 ± 1.9%. The positive predictive value was 100% and the negative predictive value of 95.9% ± 4.0%, showing no false positive results and only 1.33% of false negative results, thus consisting in the most efficient blood gasometry parameters correlated to low cardiac output.
CONCLUSIONS
The blood gasometry from the right atrium can be useful in evaluating the hemodynamic status of patients in the postoperative period of cardiac surgery. SvO2 < 55% and C(a-v)O2 > 7.0mL/100mL reflect a state of low cardiac output and due to a good sensitivity, specificity, and accuracy its use can be widely applied without establishing further risks to the patients. This is a simple method to be applied in the postoperative cardiac surgery routine and together with the clinical examination may safely guide therapeutic procedures, such as weaning of inotropic drugs and fluid replacement, especially in those patients with hemodynamic instability.
1. Swan HJ, Ganz W, Forrester J, Marcus H, Diamond G, Chonette D. Catheterization of the heart in man with use of a flow-directed balloon-tipped catheter. N Eng J Med. 1970;283(9):447-51.
2. Forrester JS, Ganz W, Diamond G, McHugh T, Chonette DW, Swan HJ. Thermodilution cardiac output determination with a single flow-directed catheter. Am Heart J. 1972;83(3):306-11. [MedLine]
3. Gore JM, Goldberg RJ, Spodick DH, Alpert JS, Dalen JE. A community-wide assessment of the use of pulmonary artery catheters in patients with acute myocardial infarction. Chest. 1987;92(4):721-7. [MedLine]
4. Ivanov RI, Allen J, Sandham JD, Calvin JE. Pulmonary artery catheterization: a narrative and systematic critique of randomized controlled trials and recommendations for the future. New Horiz. 1997;5(3):268-76. [MedLine]
5. Harvey S, Young D, Brampton W, Cooper AB, Doig G, Sibbald W, et al. Pulmonary artery catheters for adult patients in intensive care. Cochrane Database Syst Rev. 2006;3:CD003408. [MedLine]
6. Shah MR, Hasselblad V, Stevenson LW, Binanay C, O'Connor CM, Sopko G, et al. Impact of the pulmonary artery catheter in critically ill patients: meta-analysis of randomized clinical trials. JAMA. 2005;294(13):1664-70. [MedLine]
7. Krauss XH, Verdouw PD, Hughenholtz PG, Nauta J. On-line monitoring of mixed venous oxygen saturation after cardiothoracic surgery. Thorax. 1975;30(6):636-43. [MedLine]
8. Perner A, Haase N, Wiis J, White JO, Delaney A. Central venous oxygen saturation for the diagnosis of low cardiac output in septic shock patients. Acta Anaesthesiol Scand. 2010;54(1):98-102. [MedLine]
9. Lee J, Wright F, Barber R, Stanley L. Central venous oxygen saturation in shock: a study in man. Anesthesiology. 1972;36(5):472-8. [MedLine]
10. Martin C, Auffray JP, Badetti C, Perrin G, Papazian L, Gouin F. Monitoring of central venous oxygen saturation versus mixed venous oxygen saturation in critically ill patients. Intensive Care Med. 1992;18(2):101-4. [MedLine]
11. Stone HH, MacKrell TN, Brandstater BJ, Haidak GL, Nemir P Jr. The effect of induced hemorrhagic shock on the cerebral circulation and metabolism of man. Surg Forum. 1955;5:789-94. [MedLine]
12. Smith LL, Reeves CD, Hinshaw DB. Hemodynamic alterations and regional blood flow in hemorrhagic shock. In: Mills LC, Moyer JH, eds. Shock and hypotension. New York:Grune & Stratton;1965. p.373.
13. Scheinman MM, Brown MA, Rapaport E. Critical assessment of use of central venous oxygen saturation as a mirror of mixed venous oxygen in severely ill cardiac patients. Circulation. 1969;40(2):165-72. [MedLine]
14. Martin WE, Cheung PW, Johnson CC, Wong KC. Continuous monitoring of mixed venous oxygen saturation in man. Anesth Analg. 1973;52(5):784-93. [MedLine]
15. Waller JL, Kaplan JA, Bauman DI, Craver JM. Clinical evaluation of a new fiberoptic catheter oximeter during cardiac surgery. Anesth Analg. 1982;61(8):676-9. [MedLine]
16. Jamieson WR, Turnbull KW, Larrieu AJ, Dodds WA, Allison JC, Tyers GF. Continuous monitoring of mixed venous oxygen saturation in cardiac surgery. Can J Surg. 1982; 25(5):538-43. [MedLine]
17. Schmidt CR, Frank LP, Forsythe SB, Estafanous FG. Continuous S-vO2 measurement and oxygen transport patterns in cardiac surgery patients. Crit Care Med. 1984;12(6):523-7. [MedLine]
18. Richard C, Thuillez C, Pezzano M, Bottineau G, Giudicelli JF, Auzepy P. Relationship between mixed venous oxygen saturation and cardiac index in patients with chronic congestive heart failure. Chest. 1989;95(6):1289-94. [MedLine]
19. Shenaq SA, Casar G, Chelly JE, Ott H, Crawford ES. Continuous monitoring of mixed venous oxygen saturation during aortic surgery. Chest. 1987;92(5):796-9. [MedLine]
20. Jain A, Shroff SG, Janicki JS, Reddy HK, Weber KT. Relation between mixed venous oxygen saturation and cardiac index. Nonlinearity and normalization for oxygen uptake and hemoglobin. Chest. 1991;99(6):1403-9. [MedLine]
21. Sommers MS, Stevenson JS, Hamlin RL, Ivey TD, Russell AC. Mixed venous oxygen saturation and oxygen partial pressure as predictors of cardiac index after coronary artery bypass grafting. Heart Lung. 1993;22(2):112-20. [MedLine]



 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license