ABSTRACT
Objective: Atrial fibrillation (AF) is a common complication following cardiac surgery and is associated with an increased patient morbidity and mortality. The objective of this study was to develop a risk index proposal to predict AF after cardiac surgery. Methods: A prospective observational study in that 452 patients were selected to assess the incidence and risk factors associated with postoperative AF. Only patients following cardiac surgery were selected. Continuous cardiac monitor and daily electrocardiogram were assessed. The most associated in a multivariable logistic model were selected for the risk index. Results: The average incidence of AF was 22.1%. The most associated factors with AF were: patients older than 75 years of age, mitral valve disease, no use of a beta blocker, withdrawal of a beta-blocker and a positive fluid balance. The absence risk factor determined 4.6% chance to postoperative AF, and for one, two and three or more risk factors, the chance was 16.6%, 25.9% and 46.3%, respectively. Conclusion: In a multivariable logistic model was possible to develop a risk index proposal to predict postoperative AF with a major risk of 46.3% in the presence of three or more risk factors.
RESUMO
OBJETIVO: A fibrilação atrial (FA) é uma complicação frequente após cirurgia cardíaca e está associada ao aumento na morbidade e mortalidade dos pacientes. O objetivo deste estudo foi desenvolver uma proposta de escore de risco para FA após cirurgia cardíaca. MÉTODOS: Estudo prospectivo observacional, no qual 452 pacientes foram selecionados para avaliação da incidência e fatores de risco associados com FA pós-operatória. Foram selecionados somente pacientes submetidos à cirurgia cardíaca. A avaliação utilizou monitoramento cardíaco contínuo e eletrocardiograma diário. Os fatores com maior associação em modelo de regressão logística multivariável foram selecionados para o escore de risco. RESULTADOS: A incidência média de FA foi de 22,1%. Os fatores mais associados com FA foram: pacientes com mais de 75 anos de idade, doença valvar mitral, não utilização de betabloqueador, interrupção do uso de betabloqueador e balanço hídrico positivo. A ausência fator de risco determinou 4,6% de chance de FA pós-operatória e para um, dois e três ou mais fatores de risco a chance foi, respectivamente, de 16,6%, 25,9% e 46,3%. CONCLUSÃO: Em modelo de regressão logística multivariada foi possível estabelecer uma proposta para escore de risco para predição de FA pós-operatória, com um risco máximo de 46,3% na presença de três ou mais fatores de risco.
INTRODUCTION
Atrial fibrillation (AF) is the most common arrhythmia in adults. This disease is initiated by a rapid electrical activity localized in an outbreak of the atrial myocardium and sustained by reentrant circuits. These circuits appear and disappear at different times and places in the atrium, leading to an arrhythmic contraction and thus decreasing the atrial contractility, which predisposes the atrium to new reentrant circuits[1-3]. Foci of rapid ectopic activity, often located in the region extending from the left atrium to the pulmonary veins are related to the onset of AF episodes in humans[4,5]. The proposed mechanisms are: increased automaticity, trigger activity, micro-reentry and changes in sympathetic tone[4]. The atria of patients with AF show structural abnormalities[6,7]. Histologic examination shows areas of fibrosis with juxtaposition of normal and diseased atrial fibers, which contribute to the heterogeneity of atrial refractoriness[8]. Fibrosis is an important component of the pathophysiology of AF, particularly when this arrhythmia is associated with heart failure or atrial dilatation[4].
The postoperative arrhythmias have a multifactorial etiology, but originate mainly from an incomplete myocardial protection. Oxygen-derived free radicals and calcium overload resulting from ischemia reperfusion are important arrhythmogenesis mechanisms that lead to transmural reentry[9].
The postoperative period of cardiac surgery is a period of high predisposition to develop AF, reaching an incidence of 10% to 50% of the patients[10-13]. The incidence of postoperative AF has its peak in the second and third postoperative days[3].
Several prophylactic measures for the onset of postoperative AF are reported in the literature, including the use of magnesium, amiodarone, digoxin, steroids and beta blockers, the latter being of greater viability and effectiveness[14].
Advanced age is the risk factor most frequently associated with postoperative AF. Other risk factors associated with AF in the postoperative period of cardiac surgery are: male gender, previous history of AF, hypertension, valvular disease, left ventricular hypertrophy, left heart failure, chronic obstructive pulmonary disease, suspension of beta-blockers, coronary stenosis,
systemic inflammatory response syndrome, sepsis and need for mechanical ventilation support[2,12-16].
In addition to expanding costs, readmissions and prolongation of hospital stay, AF leads to a worsened prognosis of the patient, resulting in increased morbidity and mortality [10-13]. The high incidence of AF in the postoperative of cardiac surgery points to the importance of identifying patients at high risk for developing this arrhythmia. The benefit of preventive and therapeutic measures have been proposed for the study of the genesis of AF in the postoperative period. Thus, this study aimed to develop a proposal for a risk score for the incidence of AF after cardiac surgery.
METHODS
The present study consists of a prospective, observational analysis, in which 448 patients were enrolled at the Institute of Cardiology/University Foundation of Cardiology of Rio Grande do Sul (IC-FUC).
We selected adult patients undergoing CABG or valve surgery with or without cardiopulmonary bypass. Patients with AF or with history of paroxysmal or permanent AF preoperatively were excluded. Patients were selected during the immediate postoperative period in the Postoperative Unit Number I (POU I) of the IC-FUC. This study included analysis of a sample of patients obtained in two separate years.
Patients were selected systematically. The sample included all patients undergoing cardiac surgery on a given weekday, and in each week the day of selection was different, consecutively, from Monday to Friday. All patients enrolled in the study were followed until the day of hospital discharge.
Assessment of each patient was divided into four phases: immediate postoperative phase, intensive care unit (ICU) postoperative (POU I and II), post-ICU (nursing beds) and day of discharge from hospital. In each of the four phases, we used a protocol previously approved by the Research Ethics Committee of the IC-FUC in which there were the data to be searched.
All patients who met the inclusion criteria signed a written informed consent approved by the Research Ethics Committee of the IC-FUC. Failure to sign the informed consent resulted in the exclusion of the patient. In the selection phase, the demographics and preoperative data have been chosen for survey.
All patients were examined personally by the researchers. Surveys were also analyzed pre-and postoperatively. In the phase of ICU - postoperative and in the phase of discharge from ICU, patients were assessed daily, from the clinical and laboratory point of view.
Cardiac rhythm was assessed by continuous cardiac monitoring in all patients for a minimum of 72 hours (postoperative ICU) and by daily electrocardiographic examinations until hospital discharge.
Additional electrocardiographic exams were performed when the patients reported palpitations, tachycardia or angina
pectoris.
It was considered AF any episode of supraventricular arrhythmia whose electrocardiographic tracing showed "f" waves of variable morphology and amplitude, with irregular ventricular rhythm. There were considered for the study episodes of AF lasting at least 15 minutes or requiring treatment due to symptoms or hemodynamic instability.
Statistical analysis
During the selection and analysis of the patients, there was the implementation of a protocol for prevention of AF after cardiac surgery. This protocol was implemented by the establishment of an independent and not linked manner to this study. Thus, it became necessary to compare clinical and demographic data between patients by Student's t test for independent samples.
Through a derivation cohort, risk factors were associated with postoperative AF. Among these factors it was developed a score of chances on which were selected the risk factors independently associated with postoperative AF in multivariate logistic regression model with backward selection (P < 0.05).
Data analysis was performed using the Statistical Package for Social Sciences (SPSS) version 12.0 (Chicago, Illinois, USA).
RESULTS
This study included the screening of 448 patients over a period of two years. Patients selected before and after implementation of routines for prevention of AF were, respectively, 145 and 303 individuals. Faced with the comparison of clinical and demographic characteristics, no statistically significant differences at baseline were found. So, as a single sample, the average age was 61 years (sd+12), being 25% over 70 years. Males constituted 64% of the sample.
In all patients, we obtained an incidence of 22.1% (n=99) of postoperative AF.
Univariate analysis of the derivation cohort showed that significant risk factors for AP were: age over 70 years, diabetes, mitral and aortic valve disease, dyspnea, dyslipidemia, left heart failure (LHF), beta-blockers discontinued and increased total fluid balance. These variables were defined by clinical, laboratory and radiographic findings, according to the literature. Only the use of beta-blockers or not was considered (Table 1).
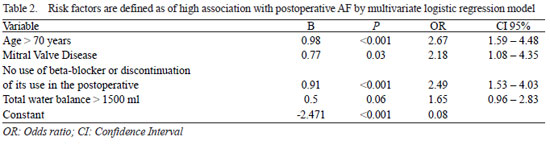
Among all risk factors mentioned above, which showed strong association in multivariate logistic regression with postoperative AF, according to their clinical relevance were: age over 70 years, mitral valve disease, the use or discontinuation of beta-blockers and fluid balance above 1500 ml. These factors were used for composition of the risk score for prediction of AF (Table 2).
The proposed risk score is shown in Figure 1 in graph form, where it can be observed the increasing line of risk in relation to the increased number of associated factors (Figure 1).

Fig. 1 - Increased risk (expressed in%) for the occurrence of postoperative AF in accordance with the number of risk factors present. The bars represent the confidence interval of 95% (P < 0.001)
DISCUSSION
During the development of this proposal of risk score, this study examined patients in the postoperative period of cardiac surgery. Some studies have sought to establish the main factors associated with postoperative AF.
This study showed that age above 70 years is strongly associated with AF in the postoperative period of cardiac surgery (P < 0.001). Among the patients over 70 years, 33.1% developed AF during the hospital stay. The model of Zaman et al.[17] sought to highlight the preoperative risk of AF after CABG. This study used age above 60 years, enlarged P wave (greater than 155ms, suggesting atrial overload) and male gender as risk factors. Patients with three risk factors were considered at high risk for developing postoperative AF. Mathew et al.[18] in a prospective and multicenter study, also developed an index for risk of atrial fibrillation after cardiac surgery, in which factors considered independently associated with postoperative AF were age, previous history of AF, valve surgery, chronic obstructive pulmonary disease and discontinuation of beta blockers or angiotensin converting enzyme 1.
Literature reports any patient over 70 years as high-risk patient for developing AF. In addition, it is also known that every 10 years of patient's age, the risk of postoperative AF increased 75%[17,19]. Advanced age is associated with changes in connective tissue and atrial dilatation, and may cause changes in electrical conduction and thereby also increasing the chance of FA. Most of these patients suffer from hypertension and left ventricular hypertrophy, which further predispose the atrium to the development of AF[19]. However, it is not possible to relate the high association of AF in elderly patients only with cardiac surgery, and some authors have shown that the incidence of AF in elderly patients is also high in postoperative of non-cardiac surgery in populations not undergoing surgery[20,21]. Previous studies, in agreement with the study presented herein, demonstrate the advanced age as a factor of extreme importance for the development of postoperative AF.
Our study has shown that among all patients who discontinued use of beta-blockers, 32.1% had AF, which is a significant risk factor (P=0.008). Although it is considered a multifactorial etiology, the postoperative AF can be initiated after an exaggerated response to adrenergic stimulation due to incomplete myocardial protection, without the use of beta-blockers in the immediate postoperative period.
Mathew et al.[21] showed that discontinuation of beta-blockers in the immediate postoperative period resulted in 91% increase in the occurrence of postoperative AF[18]. It is observed that inadequate myocardial protection without the use or the discontinuation of a beta-blocker, increases the incidence of postoperative AF as demonstrated in this study.
Concerning the fluid balance, this study indicates that this represents a risk factor with a strong association in multivariate logistic regression (P=0.026). Silva et al.[22] found total positive fluid balance in the first 24 hours after surgery as a risk factor for AF. This study demonstrated that there is a 1% risk of developing AF for each 1ml above the average of total fluid balance. In line with these findings, a study by Kallus et al.[23] showed that positive fluid balance and excess of administration of volume on the second postoperative day were higher in patients who developed postoperative AF. In this study, the positive fluid balance on the second postoperative day was an independent predictor of postoperative AF among patients who did not receive pharmacological prophylaxis. It is suggested therefore that the arrhythmia can be triggered by atrial distension caused by fluid retention[24].
Another risk factor used in preparing this proposed risk score was the mitral valve disease, significant in multivariate logistic regression (P=0.022). In a cross-sectional study and in accordance with the findings of this study, Almassi et al.[10] observed that the surgical repair (OR 1.42 and P < 0.0001) and replacement (OR 2.33 and P < 0.001) of the mitral valve had a higher association with AF after cardiac surgery between variables intraoperatively[11]. These surgeries generally require bicaval cannulation and a long duration of cardiopulmonary bypass and aortic clamping. Although the ischemic time and cardiopulmonary bypass did not contribute significantly to the occurrence of AF in this study, other studies have shown that bicaval cannulation and cardiopulmonary bypass time increase the risk of postoperative AF[25,26]. These factors may create a bias and interfering with the role of surgery as an isolated factor in the development of postoperative AF.
The sum of factors for AF in the multivariate analysis of this study does not cover all risk factors for postoperative AF. Probably this is because the sample was insufficient and because other risk factors that are demonstrably linked to the incidence of postoperative atrial fibrillation, such as inflammation and activation of the renin-angiotensin-aldosterone system, male gender, hypertension, chronic obstructive pulmonary disease, coronary stenosis and need for mechanical ventilation support, had not been analyzed in the derivation cohort[14,27-29]. We believe that this was a major limitation of this study, but this does not prevent its validation in another population undergoing cardiac surgery.
Some studies have shown the effectiveness in the implementation of pharmacological measures to prevent AF after cardiac surgery[22,30,31]. It is believed that a risk score for the incidence of AF may guide the conduct of clinical and surgical approaches, indicating the best candidate to receive these measures.
As presented herein, we can conclude that, through a multivariate logistic regression model, it was possible to develop a propose of risk score for AF after cardiac surgery, thus enabling the identification of risk patients and the development of conduct and protocols for prophylaxis of AF in these situations. It is believed that this model can also provide an appropriate scientific basis if it is demonstrated in the validation cohort.
REFERENCES
1. Markides V, Schilling RJ. Atrial fibrillation: classification, pathophysiology, mechanisms and drug treatment. Heart. 2003;89(8):939-43. [MedLine]
2. Nattel S. Atrial electrophysiology and mechanisms of atrial fibrillation. J Cardiovasc Pharmacol Ther. 2003;8(Suppl 1):S5-11. [MedLine]
3. Maisel WH, Rawn JD, Stevenson WG. Atrial fibrillation after cardiac surgery. Ann Intern Med. 2001;135(12):1061-73. [MedLine]
4. Bharti S, Lev M. Histology of the normal and diseased atrium. In: Falk RH, Podrid PJ eds. Fibrillation: mechanisms and management. New York:Raven Press;1992. p.15-39.
5. Lip GY, Lip PL, Zarifis J, Watson RD, Bareford D, Lowe GD, et al. Fibrin D-dimer and beta-thromboglobulin as markers of thrombogenesis and platelet activation in atrial fibrillation. Effects of introducing ultra-low-dose warfarin and aspirin. Circulation. 1999;94(3):425-31.
6. Narayan SM, Cain ME, Smith JM. Atrial fibrillation. Lancet. 1997;350(9082):943-50. [MedLine]
7. Hohnloser SH. Can we predict atrial fibrillation after coronary surgery and why should we? Eur Heart J. 1998;19(5):684-5. [MedLine]
8. Siebert J, Rogowski J, Jagielak D, Anisimowicz L, Lango R, Narkiewicz M. Atrial fibrillation after coronary artery bypass grafting without cardiopulmonary bypass. Eur J Cardiothorac Surg. 2000;17(5):520-3. [MedLine]
9. Balser JR. Pro: all patients should receive pharmacologic prophylaxis for atrial fibrillation after cardiac surgery. J Cardiothorac Vasc Anesth. 1999;13(1):98-100. [MedLine]
10. Almassi GH, Schowalter T, Nicolosi AC, Aggarwal A, Moritz TE, Henderson WG, et al. Atrial fibrillation after cardiac surgery: a major morbid event? Ann Surg. 1997;226(4):501-11.
11. Hougue CW Jr, Creswell LL, Gutterman DD, Fleisher LA; American College of Chest Physicians. Epidemiology, mechanisms, and risks. American College of Chest Physicians guidelines for the prevention and management of postoperative atrial fibrillation after cardiac surgery. Chest. 2005;128(2 Suppl):9S-16S. [MedLine]
12. European Heart Rhythm Association; Heart Rhythm Society, Fuster V, Rydén LE, Cannom DS, Crijns HJ, Curtis AB, Ellenbogen KA; American College of Cardiology; American Heart Association Task Force on Practice Guidelines; European Society of Cardiology Committee for Practice Guidelines; Writing Committee to Revise the 2001 Guidelines for the Management of Patients with Atrial Fibrillation, et al. ACC/ AHA/ESC 2006 guidelines for the management of patients with atrial fibrillation -executive summary: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines and the European Society of Cardiology Committee for Practice Guidelines (Writing Committee to Revise the 2001 Guidelines for the Management of Patients With Atrial Fibrillation). J Am Coll Cardiol. 2006;48(4):854-906. [MedLine]
13. Silva RG. Resultado da implantação de rotinas para fibrilação atrial pós-operatória em hospital terciário [Tese de Doutorado]. Porto Alegre:Instituto de Cardiologia, Fundação Universitária de Cardiologia;2007.
14. Tineli RA, Rosa e Silva Jr. J, Luciano PM, Rodrigues AJ,Vicente WVA, Évora PRB. Fibrilação atrial e cirurgia cardíaca: uma história sem fim e sempre controversa. Rev Bras Cir Cardiovasc. 2005;20(3):323-31. View article
15. Svedjeholm R, Hakanson E. Predictors of atrial fibrillation in patients undergoing surgery for ischemic heart disease. Scand Cardiovasc J. 2000;34(5):516-21. [MedLine]
16. Shingu Y, Aoki H, Oba J, Takigami K, Eya K, Ebuoka N. Atrial fibrillation after isolated coronary bypass surgery. Kyobu Geka. 2005;58(9):807-11. [MedLine]
17. Zaman AG, Archbold RA, Helft G, Paul EA, Curzen NP, Mills PG. Atrial fibrillation after coronary artery bypass surgery: a model for preoperative risk stratification. Circulation. 2000;101(12):1403-8. [MedLine]
18. Mathew JP, Fontes ML, Tudor IC, Ramsay J, Duke P, Mazer CD, et al. A multicenter risk index of atrial fibrillation after cardiac surgery. JAMA. 2004;291(14):1720-9. [MedLine]
19. Aranki SF, Shaw DP, Adams DH, Rizzo RJ, Couper GS, VanderVliet M, et al. Predictors of atrial fibrillation after coronary artery surgery. Current trends and impact on hospital resources. Circulation. 1996;94(3):390-7. [MedLine]
20. Amar D, Zhang H, Leung DH, Roistacher N, Kadish AH. Older age is the strongest predictor of postoperative atrial fibrillation. Anesthesiology. 2002;96(2):352-6. [MedLine]
21. Benjamin EJ, Levy D, Vaziri SM, D'Agostino RB, Belanger AJ, Wolf PA. Independent risk factors for atrial fibrillation in a population-based cohort. The Framingham Heart Study. JAMA. 1994;271(11):840-4. [MedLine]
22. Silva RG, Lima GG, Laranjeira A, Costa AR, Pereira E, Rodrigues R. Fatores de risco e morbimortalidade associados à fibrilação atrial no pós-operatório de cirurgia cardíaca. Arq Bras Cardiol. 2004;83(2):99-104.
23. Kalus JS, Caron MF, White CM, Mather JF, Gallagher R, Boden WE, et al. Impact of fluid balance on incidence of atrial fibrillation after cardiothoracic surgery. Am J Cardiol. 2004;94(11):1423-5. [MedLine]
24. Moreira DAR. Arritmias no pós-operatório de cirurgia cardíaca. Rev Soc Cardiol Estado de São Paulo. 2001;11(5):941-55.
25. Mathew JP, Parks R, Savino JS, Friedman AS, Koch C, Mangano DT, et al. Atrial fibrillation following coronary artery bypass graft surgery: predictors, outcomes, and resource utilization. MultiCenter Study of Perioperative Ischemia Research Group. JAMA. 1996;276(4):300-6. [MedLine]
27. Fontes ML, Mathew JP, Rinder HM, Zelterman D, Smith BR, Rinder CS; Multicenter Study of Perioperative Ischemia (McSPI) Research Group. Atrial fibrillation after cardiac surgery/cardiopulmonary bypass is associated with monocyte activation. Anesth Analg. 2005;101(1):17-23. [MedLine]
28. Frustaci A, Chimenti C, Belloci F, Morgante E, Russo MA, Maseri A. Histological substrate of atrial biopsies in patients with lone atrial fibrillation. Circulation. 1997;96(4):1180-4. [MedLine]
29. Dilaveris P, Giannopoulos G, Synetos A, Stefanadis C. The role of renin angiotensin system blockade in the treatment of atrial fibrillation. Curr Drug Targets Cardiovasc Haematol Disord. 2005;5(5):387-403. [MedLine]
30. Chen MC, Chang JP, Liu WH, Yang CH, Chen YL, Tsai TH, et al. Increased inflammatory cell infiltration in the atrial myocardium of patients with atrial fibrillation. Am J Cardiol. 2008;102(7):861-5. [MedLine]
31. Bradley D, Creswell LL, Hogue CW Jr, Epstein AE, Prystowsky EN, Daoud EG; American College of Chest Physicians. Pharmacologic prophylaxis: American College of Chest Physicians guidelines for the prevention and management of postoperative atrial fibrillation after cardiac surgery. Chest. 2005 Aug;128(2 Suppl):39S-47S.
32. Wanderley JF, Lamprea D, Moraes CR, Moraes F, Tenório E, Gomes CA, et al. Profilaxia da fibrilação atrial no pós-operatório imediato de cirurgia coronária: comparação entre propranolol e sotalol utilizados em baixas doses. Rev Bras Cir Cardiovasc 2001;16(4):350-3. View article
Article receive on Tuesday, October 13, 2009


 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license