Female neonate diagnosed with ectopia cordis and onphalocele was submitted to an operation at 6 hours of age to reconstruct the abdominal wall and place the heart in the left pleural space. After initial hemodinamic instability the patient was reoperated to open the sternum; with progressive recovery, extubation ocurred on 15th postoperative day and she was discharged in 40th day. With 8 months of life a new operation was successfully performed to close the sternum and reconstruct the abdominal wall. After four years, the child is asymptomatic with no necessity of medications or physical restrictions.
Recém-nascido, sexo feminino, com diagnóstico de ectopia cordis e onfalocele; realizada cesariana e com 6 horas correção da parede abdominal e da ectopia cordis. Evoluiu com grave instabilidade hemodinâmica, sendo reoperada para liberação dos pontos do esterno. Apresentou melhora progressiva, extubação no 15º e alta no 40º dia. Aos oito meses foi reinternada para fechamento do esterno e reconstrução abdominal (neoonfaloplastia). Houve boa evolução, com alta no 5º dia. Com 4 anos de evolução, encontra-se assintomática, sem medicações ou restrições físicas.
INTRODUCTION
Prenatal diagnosis of heart and thoracic-abdominal wall defects are becoming an important weapon in the programming of delivery and of perinatal therapy. Among these, Cantrell syndrome (ectopia cordis and malformation of abdominal wall) is one example. In spite of its low prevalence, this is a challenge for the surgeon due to the variety and severity of the cardiac and abdominal malformations and high mortality rate [1-3].
Here we describe the case of a child with a satisfactory evolution whose diagnosis was made intrauterine and the malformations corrected early.
CASE REPORT
A Caucasian, female infant was born from the third pregnancy of a 34-year-old mother. At 26 weeks the infant was diagnosed with ectopia cordis, muscular interventricular communication and omphalocele. At 38 weeks a c-section was performed and the baby was born with 3095g and 1 and 5-minute Apgar scores of 8 and 10.
The physical examination revealed an exposed cardiac area, with the ventricles totally outside of the thoracic cavity without pericardium protection, which would serve as the cavity lining and the existence of omphalocele. In the sixth postnatal hour the infant was submitted to abdominal wall reconstruction using polypropylene netting and peritoneal and cutaneous patches. The ectopia cordis was then corrected and agenesis of two thirds of the distal sternum was observed with the herniated portion in contact with the peritoneum and little constriction in the basal portion of the ventricles. The surgeon opted to resect the pericardium to the left and to release the heart, positioning it in the left hemithorax; the anterior portion of the diaphragm was repaired with separate sutures, the sternum was fixed with steel wire and closure of the skin of the thoracic and abdominal regions was achieved.
The infant evolved with severe hemodynamic instability, bad peripheral perfusion and hypotension, requiring dopamine, dobutamine and adrenaline but she did not show improvement. An echocardiogram was performed which revealed preserved biventricular systolic performance and signs of diastolic restriction. The baby was again submitted to surgery 12 hours after, with release of the sternal fixation sutures. The decision was to maintain the heart in the left hemithorax and close the subcutaneous layers and skin.
She remained hemodynamically unstable, on high doses of inotropic agents which were suspended on the seventh day of life. Extubation occurred on the 15th postoperative day, she was released from the intensive care unit at 33 days and discharged at 40 days, using oxygen, which was suspended when she was three months of age.
When the infant was eight months old she was again hospitalized for the correction of residual defects. She presented with sternal instability due to mechanic dehiscence, with the right sternal portion riding over the left and abdominal arching (Figure 1).
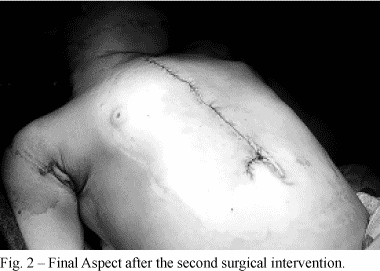
During the operation, dehiscence of the anchoring of the polypropylene prosthesis was observed; sternum closure was achieved using substernal reinforcement and diaphragmatic plicature and the reconstruction of the abdominal wall using thoracic-abdominal cutaneous patches; the excessive skin was removed (Figure 2). The child presented a good evolution, she was extubated on the first postoperative day; and was released from hospital on the fifth postoperative day. An echocardiogram showed occlusion of the intraventricular communication and an ostium secundum-type interatrial communication, without clinical repercussions.
She has been followed-up for four years and remains asymptomatic without taking medications and without physical restrictions. She has no gastrointestinal, neurologic development or psychomotor disorders and her school performance and learning abilities are normal for her age. She persists with an 8-mm interatrial communication observed during a routine follow-up echocardiogram examination.
COMMENTS
Pentalogy of Cantrell is a congenital syndrome, which was initially described by CANTRELL et al. [1] in 1958. It is characterized by two principal defects: ectopia cordis and malformations of the abdominal wall associated with defects of three interposed structures - the distal third of the sternum, anterior portion of the diaphragm and the diaphragmatic pericardium.
Ectopia cordis can be classified as a rare congenital defect, related to the malformation of the anterior wall of the thorax, with an extrathoracic location of the heart. Depending on the position of where the heart is found, it can be categorized as one of four types; cervical, thoracic, thoracic-abdominal and abdominal [2,3], but omphalocele is a malformation of the abdominal wall and is the most common finding. The formation of the thoracic and abdominal walls is complete in the ninth week of pregnancy and of the heart in the eighth week [1]. Any problem in this process can result in the appearance of the Cantrell syndrome [4]. The associated anomalies, as already described in the literature, are principally anomalies of the cardiovascular, respiratory and central nervous systems and of the gastrointestinal and genitourinary tracts [1,4].
The prevalence of this disease is low (it is thought to be about one in every 65,000 live births), and there have been, approximately nine hundred cases described in the international literature [5]. The infant in this report is female with two normal brothers.
The prognosis depends on the degree of the intracardiac involvement and associated malformations, as well as the degree to which the heart is exposed. The majority of neonates die within the first hours of birth. Attempts at surgical correction are already widely performed, with immediate covering of the heart and exposed abdominal contents using silastic prosthesis being recommended. Additionally a complete evaluation and correction of the intracardiac defects should be performed before closing the abdominal wall [6]. This procedure sometimes causes distortion of the great vessels and compression of the heart resulting in low cardiac output [6].
The obstetrician's conduct, if there is suspicion of Pentalogy of Cantrell, must included a cautious investigation of associated anomalies, especially intracardiac anomalies and a request for a fetal karyotype examination. Interruption of the pregnancy in the first few months and programming of the c-section in the last three months of pregnancy must also be considered and discussed with the parents.
The child in this case had all the signs of Cantrell syndrome: ectopia cordis, omphalocele, agenesis of the sternum, malformation of the diaphragmatic pericardium and of the anterior portion of the diaphragm and intraventricular communication. Surgical treatment included the correction of the position of the heart and correction of abdominal and thoracic defects. The muscular intraventricular communication diagnosed at birth was considered small, which did not justify its correction. The spontaneous closing of the intraventricular communication confirmed this to be the correct decision.
Another intracardiac defect which was not corrected in the reoperation was the interatrial communication, because of the same reasons. After four years of follow-up, the child is asymptomatic, without clinic repercussions caused by the presence of the interatrial communication and its future approach must be decided according to the child's clinical evolution.
An aspect which we consider important was the prenatal diagnosis, with details of the defects, making programming of the delivery in a well prepared hospital structure, with a pediatric intensive care unit and early surgery possible.
There are controversies in the literature as to the best surgical technique and generally the option is to correct all existent defects early taking into consideration the severity of the anomalies. In those patients in which these defects are not so serious, surgical planning must take priority the correction of omphalocele and of the diaphragmatic alterations because these corrections when performed early on, are technically easier and this may avoid the potential risk of compression of the heart by the sternum and pulmonary hypoplasia.
BIBLIOGRAPHIC REFERENCES
1. Cantrell JR, Haller JA, Ravitch MM. A syndrome of congenital defects involving the abdominal wall, sternum, diaphragm, pericadium and heart. Surg Gynecol Obstet 1958; 107:602-14.
2. Blatt ML, Zeldes M. Ectopia cordis: report of a case and review of the literature. Am J Dis Child 1942; 63:515.
3. Byron F. Ectopia cordis: report of a case with attempted operative correction. J Thorac Surg 1949;17:717-22.
4. Shah HR, Patwa PC, Shah BP. Case report: antenatal ultrasound diagnosis of a case of "Pentalogy of Cantrell" with common cardiac chambers. Ind J Radiol Imag 2000; 10:99-101.
5. Cullinan JA, Nyberg DA. Fetal abdominal wall defects. In: Rumack CM, Wilson Sr, Charboneau JW, editors. Diagnostic ultrasound. 2nd ed. Vol. 2. New York: C.V. Mosby; 1996. p.1167-9.
6. Harrison MR, Filly RA, Stanger P, De Lorimier AA. Prenatal diagnosis and management of omphalocele and ectopia cordis. J Pediatr Surg 1982;17:64-6.
[ Medline ]


 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license