Objective: This is an experimental study which aims at developing and evaluating the feasibility of experimental techniques of vascularized and cutaneous abdominal heterotopic heart transplant in mice, creating an instrument of investigation for the effectiveness of prservation solutions, new immunosuppressive drugs, biological agents, genetic therapy and induction of immunological tolerance.
Method: The techniques used in this work were previously described by Corry et al. and Billingham et al.
Results: The total surgical time to perform the cardiac transplants (n=20) was on average 60.3+6.3 minutes and the time of cutaneous transplants (n= 20) 17.75+0.71 minutes. The average survival of the cutaneous allografts (n=34) and cardiac (n=24) allografts was 7 and 11 days, respectively, while the syngeneic grafts survived more than 100 days.
Conclusions: Both techniques are characterized by the easy reproducibility of the experimental models. The differences between the techniques were not limited either by the methodological peculiarities or by the length of survival and vascularization, but mainly by the immunogenicity and susceptibility of rejection.
Objetivo: Estudo experimental com o objetivo de desenvolver e avaliar a viabilidade das técnicas de transplante experimental cardíaco heterotópico abdominal vascularizado e cutâneo em camundongos, criando um instrumento para investigação da eficácia de soluções de preservação, novas drogas imunossupressoras, agentes biológicos, terapia gênica e indução de tolerância imunológica.
Método: Para este estudo, as técnicas utilizadas foram descritas previamente por Corry et al. e Billingham et al.
Resultados: O tempo cirúrgico total para a realização dos transplantes cardíacos (n=20) foi, em média, 60,3±6,3 minutos e para os transplantes cutâneos (n=20), 17,75±0,71 minutos. A média de sobrevida dos aloenxertos cutâneos (n=34) e cardíacos (n=24) foi, respectivamente, 7 e 11 dias, enquanto que os isoenxertos sobreviveram por mais de 100 dias.
Conclusões: Ambas as técnicas se caracterizaram pela fácil reprodutibilidade dos modelos experimentais. As diferenças entre as técnicas não se limitaram às peculiaridades metodológicas ou ao tempo de sobrevida e vascularização, mas principalmente à sua imunogenicidade e suscetibilidade à rejeição.
INTRODUCTION
Nowadays organ transplantation is the most efficient therapy for patients with end organ failure. The success rate of renal transplantation at the end of the first year is such that, survival of patients and grafts is greater than 90% and 80%, respectively, in the majority of the most important transplantation centers worldwide [1]. These rates represent a great advance when compared with those obtained at the start of the modern era of organ transplantation from the 1950s until the start of the 1980s [2].
However, this therapeutic option continues to be a clinical and surgical challenge as many pertinent questions still remain without solutions. Maintenance of allografts require the permanent use of immunosuppressant drugs, which increase the incidence of tumors and opportunist infections, but even so the drugs do not totally impede the rejection process which continues to be the main cause of long-term graft loss. A more attractive alternative would be a method of specific immunosuppression that makes the recipient tolerant to the antigens of the donor without the necessity of continued immunosuppression.
Organ transplantations started in animals more than a century ago [3]. Using original techniques, Carrel [4] in 1908 achieved brilliant results in the transplantation of blood vessels, organs and limbs, when he developed the technique of vascular anastomosis, enabling the transplantation of vascularized solid organs such as the kidneys and the heart.
Although transplantation techniques of different organs and tissues are very well established, the great challenge continues to be the immunological obstacle, encouraging scientists to look for new options in the fields of xenotransplantations, transgenics and pharmacology and to develop methods of inducing immunological tolerance.
In order to understand and to get around the rejection processes, investigations performed from the 1950s have demonstrated the importance of isogenic mice in basic immunology, transplantation immunopathology and immunosuppression studies [4,5]. These animals allow the control and prediction of immunological events in experimental allotransplants and the study of antigenic stimuli during the rejection process, as well as surgical techniques and physiology in transplantation and the induction of immunological tolerance [5]. An important aspect was the evaluation of the role of individual loci products of the major histocompatibility complex in allorecognition, as well as their tolerogenic potential.
This study aims at developing experimental techniques of skin and vascularized abdominal heterotopic heart transplantations in mice, with the objective of utilizing them as an instrument of study of the immunological mechanisms involved in allorecognition, in the evaluation of new immunosuppressant drugs or biological agents and in the induction of tolerance.
METHOD
Animals
To develop this work, C3H/HeJ (H2K), C57BL/6N (H2b) and BALB/c (H2d) isogenic mice were utilized. These animals were bred and kept in conditions of a conventional animal house, in the Production and Animal Experimentation Coordination (PAEC) of the Scientific and Technological Development Center (STDC) of the State Heath Production and Research Foundation (SHPRF).
All animals were male with ages of between 8 to 10 months. Before and during the experimental period, these animals were fed with standard feed for rodents, received water ad libitum and were maintained in individual cages, duly identified and with a photo-period of 12 hours of light and 12 hours of dark (06:00 a.m./18:00 p.m.).
All the procedures employed involving the animals complied with the Brazilian Code on Animal Experimentation, in respect to the State Constitution Law [6]. The research project was approved by the Ethics Commission and the Scientific Commission of the Research Group in Post Graduation of the Hospital das Clínicas in Porto Alegre, Brazil.
Heterotopic heart transplantation
To develop the experimental model of vascularized heterotopic heart transplantation in mice, the technique previously described by Corry et al. [7] was employed. For this, a microsurgical microscope (Nikon ® Stereomicroscope teaching system, model SMZ-U) was utilized, as well as previously sterilized compatible instruments (as described below).
Ninety-two animals were used among donors and recipients to perform a total of 22 isografts and 24 allografts.
All animals in this study, after weighting in an analytical balance (Marte ®, AM220) were anesthetized using a final solution of 2% xylazine hydrochloride (Rompun ®, Bayer Animal Heath) and 10% Ketamine hydrochloride (Dopalen®, Agribrands Brasil Ltda.) diluted in 2 mg/mL and l0 mg/mL in 0.9% saline solution (Alcon®, Alcon Labs. do Brasil Ltda.), respectively. One only dose of 0.l mL for each 10 g of body weight was used intraperitoneally.
After anesthetization and preparation for surgery, donor and recipient, were fixed by the paws, in the dorsal decubitus position, using adhesive tape (Cremer ®, on a plaque heated at a temperature of 37ºC.
Preparation of the recipient
Under a microscope with an amplification of 16 x, using straight thin scissors and teethed dissection tweezers, an abdominal xiphopubic laparotomy was made and using a 70-mm Alm retractor (Downs® Downs Surgical Ltd, UK) a 4 cm opening in the abdominal was maintained.
A gauze dampened with 0.9% saline solution was placed over the abdominal opening where, with the help of flexible ear swabs (Cotonetes ®, Johnson & Johnson), the viscera were removed up and to the right through the cut and were carefully wrapped in gauze, thereby exposing the aorta and the inferior vena cava (IVC). The lumbar veins were delicately dissected with the help of nº 5 iris tweezers, which were then ligated using 7-0 thread (Pearsalls Suture ®, Somerset, UK), causing definitive hemostasis in three of the vessels, thus providing a good surgical field.
The aorta and IVC were maintained in contiguity, as, not only did they not interfere in the achieving of the anastomosis, but dissection of the intervascular plan would unnecessarily increase the surgical time, as well as making the wall of the IVC fragile and cause bleeding.
Five-mm vascular clamps (Scoville Lewis ®, Downs Surgical Ltd., UK) were positioned immediately under the renal veins and arteries and close to the emergence of the ileac veins. Finally, aortotomy and venotomy were performed, next to each other, respecting the position of the pulmonary artery (PA) and of the aorta, using a thin 24G needle and stretched with straight 85 mm microscissors. At this moment, with the vessels repaired, the incision was covered with a damp gauze and the recipient was put to one side while the heart of the donor was isolated.
Preparation of the donor
With the anesthetized animal in the dorsal decubitus position, the abdominal was approached similar to the recipient. A solution of sodium heparin (Liquemine (®, Roche Brasil) was injected into the IVC at 10 IU/10g of body weight diluted in saline solution. After the removal of the needle (24G), exsanguination occurred through the orifice left by the needle.
To better expose the thoracic cavity, an opening using scissors and resection of the anterior wall by bilateral parasternal sectioning were made, followed by manual luxation of the costovertebral joints and a bilateral diaphragmatic incision.
Individually, the distal IVC, the proximal superior vena cava and the azygous vein were ligated using 7-0 thread and sectioned using straight microscissors. The aorta was sectioned anterior to the brachiocephalic artery and the pulmonary artery was sectioned anterior to the bifurcation.
To complete the harvesting of the heart, the pulmonary veins were carefully brought together with 7-0 thread (Prolene, Ethicon ®), being careful to leave the aorta and PA free, leaving a thread of repair to help in its handling. The heart was gently removed from the thorax of the donor and put in a Beaker (50 mL) with 0.9% saline solution at 4ºC. To maintain the temperature constant, while the recipient was being prepared again, the Beaker was maintained in dry ice.
Implantation of the heart graft
The heart of the donor was removed from the saline solution and adjusted in the abdomen of the recipient, in a way that the ligature in blocks were maintained, during the operation. During the implantation of the heart graft, saline solution (4ºC) was continuously dripped on it to protect it.
First the end-to-side anastomosis of the aorta of the donor with the aorta of the recipient was performed (Figure 1). A suture was made in the proximal end of the aortotomy and another in the distal end, from which a continuous simple suture was began from a side of the ellipse formed, finishing at the proximal end. The same procedure was repeated for the other side of the ellipse. The same technique was employed with the anastomoses of the PA with the IVC. Both vascular anastomoses were made using 7-0 suture thread with a 0.07-mm needle (Ethilon ®, Surgicon Ltd., UK).
After finishing the anastomoses, they were wrapped in a hemostatic sponge (Gelfoam ®, Pharmacy & Upjohn Co., USA) and the clamps were removed, first the proximal end and after the distal end. Perfusion was performed with blood from the abdominal aorta of the recipient which entered in a retrograde manner through the aorta of the recipient. Due to the anti-reflux competency of the aortic valve, the blood which entered in the coronary arteries of the graft, passed by the myocardium and returned to the right atrium and ventricle inside the coronary arteries and then to the pulmonary artery, still in the donor heart, passing to the abdominal vena cava of the recipient. This is, however, a non-functional transplantation, as not all the heart cavities received blood.
After finishing the anastomoses, the viscera were replaced around the graft in the abdominal cavity using ear swabs. The muscle and skin planes were sutured with 7-0 thread (Prolene, Ethicon ®), the adhesive tapes which were holding the paws were removed and the animal was maintained on the heated plaque for an extra 2 hours. Finally, the recipient was put in an individual cage, maintaining the routine management of the animal house of PCAE.
The functioning of the heart graft was controlled day by day for 100 days after transplantation, by means of direct palpitation of the abdomen by two or more investigators.
Skin transplantation
To develop the experimental method of skin transplantation, the procedure described by Billingham & Medawar [8,9] was employed. For this 21 donors and 64 recipients among the different strains were utilized, performing a total of 30 isografts and 34 allografts.
Preparation of the recipient
After anesthesia, dorsum-lateral trichotomy was performed (4 cm2) using a shaver (Oster ®, USA), followed of anti-sepsis using 70% ethylic alcohol and the animal was placed in the dorsal decubitus position.
Preparation of the donor
With the donor, euthanasia was performed by cervical dislocation according to the Law 714 from 20th June 2002, which regulates procedures and methods of euthanasia in animals published by the Federal Council on Veterinary Medicine and by the Brazilian College of Animal Experimentation (COBEA) [10,11].
The skin of the base of the tail of the animal was transversally sectioned using a nº 24 scalpel blade (Solidor ®) and after lengthwise. With the help of dissection tweezers, this was distally pulled (base-point), removed from the animal and immersed in 0.9% saline solution at 4ºC.
Implantation of the skin graft
In the region of the trichotomy of the recipient, using nº 3 tweezers and straight thin iris scissors, 1 cm2 of skin tissue was removed. Using the scalpel blade, 1 cm2 of the total skin of the tail of the donor was sectioned. Using tweezers, the fragment of the tail skin was placed into the receptor region and held with a simple transfixing suture on the four sides of the grafted skin square (Figure 2). The recipients were placed in individual cages, maintaining the routine control for animal houses of the CPEA.
The animals were observed daily for 100 days after the transplantation and rejection was identified as a combination of some characteristics: cyanoses, erythema, erosion and finally, total loss of the skin graft.
Statistical analysis
The survival curve by the Kaplan-Meier method was utilized for statistical analysis.
RESULTS
Vascularized abdominal heterotopic heart transplantation
Analyzing a sample of animals (n=20) which was randomly chosen, it was observed that the total surgical time to perform transplantations was, on average, 60.3 ± 6.3 minutes with the time to prepare the recipient being 22.9 ± 3.1 minutes, liberation of the donor heart 11.1 ± 1.5 minutes and to perform the anastomoses 26.3 ± 3.6 minutes.
From a total of 22 heart isotransplantations performed using direct palpitation, it was observed that four hours after the transplantation, the graft of one (4%) of the animals was not beating and the animal died 5 hours after. After the anesthetic effect passed another was seen to be paraplegic. Although there was evidence that the graft was beating, euthanasia is recommended in these cases because of the paralysis and the suffering, which was performed 48 hours after the transplantation. The other mice (20) and their grafts (91%) survived for more than 100 days after the surgery.
However, from the 24 allo-transplantations performed, absence of a beating graft was noted in eight animals on the 10th day after transplantation, in twelve animals on the 11th day and in four animals on the 12th day (Figure 3).
Skin transplantation
For the preparation of recipients of the skin grafts, the mean time necessary, observed in a random sample (n=20) was 7.0 ± 0.9 minutes; for euthanasia and removal of the skin from the donor tail the time was 5.00 ± 0.8 minutes and for the implantation of the skin graft the time was 5.75 ± 0.71 minutes, with a total mean surgery time of 17.75 ± 0.71 minutes.
In the 30 skin isotransplantations performed, there were no cases of rejection. However, from the 34 allo-transplantations, nine grafts (27%) were rejected on the 6th day, twelve grafts (35%) on the 7th day and thirteen (38%) rejected skin grafts on the 8th day (Figure 4).
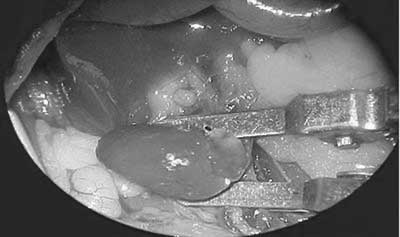
Fig. 1 - Heart transplantation: implantation of the cardiac graft - end-to-side anastomosis of the donor and recipient aortas and end-to-side anastomosis of the donor pulmonary artery with the inferior vena cava of the recipient (amplification 16 x)
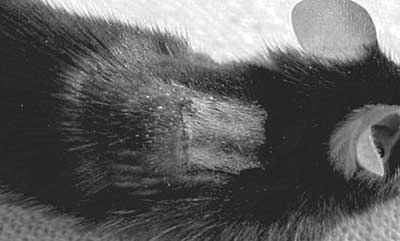
Fig. 2 - Skin transplantation: isograft in a mouse of the C57BL/6N strain, six days after transplantation

Fig. 3 - Graft showing cardiac graft survival: 22 isotransplantations and 24 allotransplantations

Fig . 4 - Graft showing skin graft survival: 30 isotransplantations and 34 allotransplantations
COMMENTS
Mice are the experimental animal chosen in several areas because they are easy to breed and manipulate, they have fast reproduction, sweet behavior, resistance against infections and surgical traumas, great genetic diversity and great similarity of the biological structures and anatomic position of the internal structures when compared to humans. Additionally, it is estimated that the homology of the DNA codifier, between these two strains is understood in between 70% and 90% [5].
Isogenic strains, by breeding among siblings for at least 20 generations giving a genetically identical mouse population constitutes one of the greatest advantages in the use of this model for the study of immunological mechanisms [5].
Thus, laboratory animals, especially mice, are exponentially utilized in the development of experimental transplantation techniques, in particular heart, renal and pancreatic islet transplantation.
The researchers Robert Corry, Henry Winn and Paul Russel [7], in 1973, recognizing the importance of the use of isogenic strains for the understanding of immunologic events, developed a murine experimental heart technique similar to the experimental protocol for heart allografts in rats, by Ono & Lindsey, in 1969 [12]. Thus, as in skin transplantation, currently, this is the most utilized experimental technique in biomedical research [13-15].
The experimental technique of vascularized heterotopic heart transplantation in mice, described by Corry et al. [7] and developed in this study, although it can be performed by just one surgeon, requires previous microsurgery training of at least four months, in order to acquire manual ability, as dealing with small animals (about 35g), it was necessary, apart from using a microscope, to use specific microsurgical instruments. Technical mistakes are responsible for the deaths of animals in the first 72 hours after the transplantation [5]. However, as reported by Corry et al. [7], the success of the technique is approximately 90%.
Another limiting factor of transplantation in mice is the anesthesia. Small animals such as rats, mice and hamsters have a relatively high metabolism and need a higher dose of anesthesia, when compared to larger species. There is also a difference in the use of anesthesia between different lines of the same species. Thus, there are two factors that make anesthesia in mice difficult: the low body weight increasing the risk of overdoses causing hypothermia and frequently death; and different strains that metabolize the anesthetic agents differently. Thus, standardization and administration of doses among distinct isogenic mice strains, for a surgical time on average of one hour (61.14 ± 7.31 minutes), must be very flexible [16].
Vessels (1-3 mm of diameter) and other structures are very small and are extremely delicate [17]. Even cotton ear swabs, if rubbed against the wall of the IVC or abdominal aorta, can make them fragile and cause bleeding. It is necessary that extra care is taken during the dissection of the lumbar veins for definitive hemostasis. This procedure is performed using straight iris tweezers as these vessels are extremely sensitive, any contact with the tweezers can be sufficient to rupture and cause bleeding. The same care must be taken during the ligation of the veins and arteries during the harvesting of the donor heart. Any contact of the tweezers with the atria or ventricles may cause perforations that are unnoticeable until the moment that the graft is perfused after anatomization, causing failure of the technique and consequently the death of the animal.
The incidence of paralysis (n=1) was associated with an ischemia time of approximately 60 minutes. This complication is generally solved with an increase in the ability of the surgeon performing the technique and a reduction in the surgical time.
This experimental transplantation method has the advantage of allowing the instantaneous evaluation of the functioning of the graft by immediate visualization of the beating heart, thus showing, the success of the technique [5]. However, occasionally, there is the necessity of making massage to the cardiac graft so that it returns to the normal rhythm [7]. The graft is perfused with oxygenated blood originating from the abdominal aorta of the recipient, which enters the coronary artery of the graft and returns to the right atrium and ventricle and then, to the pulmonary artery, draining to the IVC of the recipient.
Although this perfusion is maintained during the survival of the graft, the left ventricular is not filled, which results in hypotrophy of the isolated heart muscle [13].
Control of the heart contraction of the graft, by means of direct palpitation of the abdomen performed daily, sometimes can be confused with the transmission of the pulse of the aorta of the donor [18]. Very strong beats of the artery can mean obstruction, similar to the ingurgitation of the vein [19].
Thus, similar to the murine heart experimental model, the skin transplantation is widely utilized in research which aims at improving understanding of the immunology of transplantations, mainly the mechanisms involved in rejection and its prevention and treatment [5,9].
The skin transplantation technique developed in this study was established and standardized by Billingham & Medawar [8] in 1951, an important step in the study of immunological basis of allograft rejections [19].
Skin grafts are an excellent way of identifying the histocompatibility between donor and recipient, a technique widely utilized in animal houses to evaluate the isogenicity in colonies of inbred animals [17].
This technique has the advantage of being simple and fast and can be performed in series as the time between the harvesting of the graft and its transplantation does not exceed 20 minutes. Another advantage is the possibility of performing up to five transplantations with the tail skin of only one donor. Apart from the short-time of anesthesia required, a smaller dose of anesthesia is necessary without increased risks for the animals [9,16].
The survival or rejection of the graft is easily controlled (visual evaluation), based on the aspect of the skin, showing well-defined characteristics of acute and chronic rejection [19]. Acute rejection occurs normally within the first week after transplantation and the graft presents with dilated vessels and cyanoses, followed by skin erosion. Chronic rejection can take weeks or even months, depending on the histocompatibility between donor and recipient [8,19].
Thus, the technique has limitations. It is well established that avascularized grafts are subject to ischemic degeneration which can result in inflammation and necrosis, even when syngeneic [20]. However, it is being demonstrated that non-vascularized heart allografts are rejected more gradually (and, sometimes, not even rejected) than skin grafts with the same combination of strains [15]. Thus, the difference in the type of vascularization does not seem to be the only difference in the survival of skin grafts (7th post-operative day) and heart graft (11th post-operative day).
The difference between the techniques is not limited by the complexities of the method or vascularization, but more to the effector mechanisms, susceptibility to rejection or resistance to immunological tolerance induction. [21-23].
The existence of a hierarchy in the susceptibility to rejection of different allografts (skin, pancreatic islets and heart) is well defined, however, the mechanisms responsible are unknown. Although the heart graft stimulates the activation of a greater number of alloreactive T-cells than skin grafts, the skin presents more susceptibility to rejection and is more resistant to immunological tolerance induction [15]. On the other hand, Sun et al. [24] demonstrated that the greater the allografted mass the greater is its survival. Just one transplanted heart or kidney, among different strains of rats, gives an acute rejection in a short time however, simultaneous transplantation of two hearts or kidneys in just one recipient results in better survival of these allografts.
Studies suggest that the microenvironment and the antigenic load of grafts can play an important role in the determination of the susceptibility to rejection of an allograft and resistance to immunologic tolerance induction [25]. Additionally, another explanation for the greater susceptibility of the skin to rejection (and less tolerance induction) is the presence of tissue-specific antigens, for which the central tolerance (thymic) was not developed by the recipient [25].
It is exactly this greater difficulty in immunologic tolerance induction of skin grafts, together with the simplicity to perform the procedure, that makes this an interesting experimental model and with greater clinical relevance when compared with vascularized methods.
Unfortunately, there are no safe and reproducible manners of inducing immunologic tolerance, in human transplantation. Although the murine experimental models developed in this study present limitations, they are an important instrument to improve the knowledge of immunologic mechanisms involved in allorecognition and the creation of tolerance.
Acknowledgements
This work received financial support from the Foundation for Research of the State of Rio Grande do Sul (FAPERGS). Also the authors wish to thank the collaboration of the Medical Foundation of the Hospital de Clínicas of Porto Alegre (HCPA) and the State Foundation for Production and Research in Health.
BIBLIOGRAPHIC REFERENCES
1 Morris PJ. Results of renal transplantation. In: Kidney transplantation: principles and practice. Philadelphia:W.B. Saunders;1994. p.504.
2 Danovitch GM. Immunosuppressive medications and protocols for kidney transplantation. In: Handbook of kidney transplantation. Boston: Brown and Company;1996. p.55.
3 Küss R, Bourget P. An illustrated history of organ transplantation. Rueil-Malmaison, France:Laboratories Sandoz;1992. p.1-35.
4 Carrel A. Results of transplantation of blood vessels, organs and limbs. JAMA1908;51:1662-7.
5 Bueno V, Pestana JOM. Modelos experimentais de transplante de órgãos. São Paulo:UPM;2000. Disponível em:
. Acesso em: 18 jul. 2000.
6 Constituição do Estado do Rio Grande do Sul. Código Estadual de Proteção aos Animais. Lei 11.915, art.82 inc IV (29 mai. 2003).
7 Corry RJ, Winn HJ, Russell PS. Primarily vascularized allografts of hearts in mice: the role of H-2D, H-2K and Non- H-2 antigens in rejection. Transplantation. 1973;16(4):343-50.
8 Billingham RE, Medawar PB. The technique of free skin grafting in mammals. J Exp Biol. 1951;28(3):385-402.
9 Green MK, Mandel TE. Skin grafting in mice: indicators of cell-mediated and humoral immunitty. In: Loveland BE, Henning MM, editors. Experimental transplantation models in small animals. London: Dunitz Martin Ltda;1995. p.95-114.
10 Conselho Federal de Medicina Veterinária. Procedimentos e métodos de eutanásia em animais. Brasil. Lei 714, art. 16 (20 jun. 2002).
11 COBEA. Colégio Brasileiro de Experimentação Animal: Legislação e Ética. São Paulo. Disponível em: Acesso em: 20 mar. 2002.
12 Ono K, Lindsey ES. Improved technique of heart transplantation in rats. J Thorac Cardiovasc Surg. 1969;57(2):225-9.
13 Abbott CP, Dewitt CW, Creech Jr. O. The transplanted rat heart: histologic and electrocardiographic changes. Transplantation. 1965;85:432-45.
14 Rosz CG, Wakely ME, Bumgardner GL, Weringer EJ. Experimental models in transplantation. In: Parnham MJ, editor. Progress in inflammation research. Switzerland: Birkhäuser Verlag;1998.
15 Jones ND, Turvey SE, Van Maurik A, Hara M, Kingsley CI, Smith CH et al. Differential susceptibility of heart, skin and islet allografts to t cell-mediated rejection. J Immunol. 2001;166(4):2824-30.
16 Svendsen P. Laboratory anesthesia. In: Svendsen P, Hau J, editors. Handbook of laboratory animal science: selection and handling of animals in biomedical research. Florida:CRC Press, Inc.;1994. cap.19. p. 311-37.
17 Steinbrüchel DA. Laboratory anesthesia. In: Svendsen P, Hau J, editors. Handbook of laboratory animal science: selection and handling of animals in biomedical research. Florida:CRC Press, Inc.;1994. cap. 22. p.371-82.
18 Saitovitch D. Transplantation tolerance: an experimental model exploring mechanisms of its induction and maintenance after pre-treatment with donor antigen and anti-CD4 antibodies. Oxford:University of Oxford;1995. p.207.
19 Klein J. Biology of the mouse histocompatibility-2 complex: principles of immunogenetics applied to a single system. New York:Springer-Verlag;1975. p.620.
20 Medawar PB. The behaviour and fate of skin autografts and skin homografts in rabbits. J Anat. 1944;78:176.
21 Phillips NE, Markees TG, Mordes JP, Greiner DL, Rossini AA. Blockade of CD40- mediated signalling is sufficient for inducing islet but not skin transplantation tolerance. J Immunol. 2003;170(6):3015-23.
22 Goddard S, Youster J, Morgan E, Adams DH. Interleukin-10 secretion differentiates dendritic cells from human liver and skin. Am J Pathol. 2004;164(2):511-9.
23 Hasegawa S, Becker G, Nagano H, Libby P, Mitchell RN. Pattern of graft- and host-Specific MHC class II expression in long-term murine cardiac allografts: origin of inflammatory and vascular wall cells. Am J Pathol. 1998;153(1):69-79.
24 Sun J, McCaughan GW, Gallagher ND, Sheil AG, Bishop GA. Deletion of spontaneous rat liver allograft acceptance by donor irradiation. Transplantation. 1995;60(3):233-6.
25 Youssef AR, Otley C, Mathieson PW, Smith RM. Effector mechanisms in murine allograft rejection: comparison of skin and heart grafts in fully allogeneic and minor histocompatibility antigen-mismatched strain combinations. Transpl Int. 2002;15(6):302-9.




 All scientific articles published at rbccv.org.br are licensed under a Creative Commons license
All scientific articles published at rbccv.org.br are licensed under a Creative Commons license